Abstract
Purpose
The purpose of this study was to examine the effects of a daily life-based physical activity enhancement program performed by middle-aged women at risk for cardiovascular disease.
Methods
This study used a randomized control group pretest-posttest design. Middle-aged women aged 45 to 64 were recruited from two outpatient cardiology departments, and randomly assigned to an experimental group (n=28) and a control group (n=30). For the experimental group, after providing one-on-one counseling and education, we provided customized text messages to motivate them in daily life. To monitor the practice of physical activity, they also used an exercise diary and mobile pedometer for 12 weeks. Subjects' physical activities (MET-min/week) were measured using the International Physical Activity Questionnaire (IPAQ). Their physiological data were obtained by blood tests using a portable analyzer, and the data were analyzed using the SPSS 21.0/WIN program.
Results
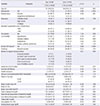
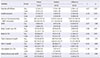
There were significant differences in exercise self-efficacy, health behavior, IPAQ score, body fat, body muscle, and fasting blood sugar between the two groups. However, there were no significant differences in total cholesterol, hemoglobin A1c, high-density lipoprotein cholesterol, and waist-to-hip ratio.
Figures and Tables
 | Figure 2Flow diagram of the progress through the phases of a randomized trial (based on CONSORT statement). |
Notes
References
1. Statistics Korea. 2015 Annual report on the causes of death statistics [Internet]. Daejeon: Statistics Korea;c2016. cited 2016 Sep 27. Available from: http://www.kostat.go.kr/portal/korea/kor_nw/2/1/index.board.
2. Appelman Y, van Rijn BB, ten Haaf ME, Boersma E, Peters SA. Sex differences in cardiovascular risk factors and disease prevention. Atherosclerosis. 2015; 241(1):211–218. DOI: 10.1016/j.atherosclerosis.2015.01.027.


3. Bassuk SS, Manson JE. Physical activity and cardiovascular disease prevention in women: A review of the epidemiologic evidence. Nutrition, Metabolism and Cardiovascular Diseases. 2010; 20(6):467–473. DOI: 10.1016/j.numecd.2009.12.015.

4. Kling JM, Miller VM, Mankad R, Wilansky S, Wu Q, Zais TG, et al. Go red for women cardiovascular health-screening evaluation: The dichotomy between awareness and perception of cardiovascular risk in the community. Journal of Women's Health. 2013; 22(3):210–218. DOI: 10.1089/jwh.2012.3744.


5. Kim MH, Chung EW, Lee DH. Cardiovascular diseases prevention and control campaign, 2015. Public Health Weekly Report. 2015; 8(39):925–928.
6. Korea Centers for Disease Control and Prevention. Chronic disease current status and issues 2017, chronic illness factbook [internet]. Cheongju: Korea Centers for Disease Control and Prevention;c2018. cited 2018 Jan 5. Available from: http://www.cdc.go.kr/CDC/intro/CdcKrIntro0504.jsp?menuIds=HOME006-MNU2804-MNU2942-MNU2944&cid=136662.
7. Mosca L, Benjamin EJ, Berra K, Bezanson JL, Dolor RJ, Lloyd-Jones DM, et al. Effectiveness-based guidelines for the prevention of cardiovascular disease in women—2011 update: A guideline from the American Heart Association. Journal of the American College of Cardiology. 2011; 57(12):1404–1423. DOI: 10.1016/j.jacc.2011.02.005.


8. Luke A, Dugas LR, Durazo-Arvizu RA, Cao G, Cooper RS. Assessing physical activity and its relationship to cardiovascular risk factors: NHANES 2003–2006. BMC Public Health. 2011; 11(1):387. DOI: 10.1186/1471-2458-11-387.



9. Haidinger T, Zweimüller M, Stütz L, Demir D, Kaider A, Strametz-Juranek J. Effect of gender on awareness of cardiovascular risk factors, preventive action taken, and barriers to cardiovascular health in a group of Austrian subjects. Gender Medicine. 2012; 9(2):94–102. DOI: 10.1016/j.genm.2012.02.001.


10. Cho SH, Choi MK, Lee JH, Cho HW. Relationship between expectations regarding aging and physical activity among middle aged adults in urban areas: Based on the Pender's health promotion model. Journal of Korean Academy of Nursing. 2015; 45(1):14–24. DOI: 10.4040/jkan.2015.45.1.14.


11. Saber F, Shanazi H, Sharifirad G, Hasanzadeh A. Checking the determinants of physical activity based on the theory of planned behavior in the housewives. Journal of Education and Health Promotion. 2014; 3:94.


12. Burke LE, Ma J, Azar KM, Bennett GG, Peterson ED, Zheng Y, et al. Current science on consumer use of mobile health for cardiovascular disease prevention: A scientific statement from the American Heart Association. Circulation. 2015; 132(12):1157–1213. DOI: 10.1161/cir.0000000000000232.


13. Morton K, Sutton S, Hardeman W, Troughton J, Yates T, Griffin S, et al. A text-messaging and pedometer program to promote physical activity in people at high risk of type 2 diabetes: The development of the PROPELS follow-on support program. JMIR mHealth and uHealth. 2015; 3(4):e105. DOI: 10.2196/mhealth.5026.

14. Pilch WB, Mucha DM, Pałka TA, Suder AE, Piotrowska AM, Tyka AK, et al. The influence of a 12-week program of physical activity on changes in body composition and lipid and carbohydrate status in postmenopausal women. Przegląd menopauzalny = Menopause review. 2015; 14(4):231–237. DOI: 10.5114/pm.2015.56311.


15. Song MS, Yoo YK, Kim NC. Effects of walking and resistance exercise on body composition and lipid profile of obese women in their 30~40s. Korean Journal of Adult Nursing. 2011; 23(4):412–419.
16. Ajzen I, Fishbein M. The influence of attitudes on behavior. In : Albarracin D, Johnson BT, Zanna MP, editors. The Handbook of Attitudes. Mahwah (NJ): Lawrence Erlbaum Associates;2005. p. 173–221.
17. Carver CS, Scheier MF. Origins and functions of positive and negative affect: A control-process view. Psychological Review. 1990; 97(1):19–35. DOI: 10.1037/0033-295X.97.1.19.

18. Powers SK, Dodd SL, jackson EM. Total Fitness and Wellness. 6th ed. Boston (MA): Pearson;2014. p. 1–420.
19. Artinian NT, Fletcher GF, Mozaffarian D, Kris-Etherton P, Van Horn L, Lichtenstein AH, et al. Interventions to promote physical activity and dietary lifestyle changes for cardiovascular risk factor reduction in adults: A scientific statement from the American Heart Association. Circulation. 2010; 122(4):406–441. DOI: 10.1161/cir.0b013e3181e8edf1.


20. Lin CH, Chiang SL, Yates P, Lee MS, Hung YJ, Tzeng WC, et al. Moderate physical activity level as a protective factor against metabolic syndrome in middle-aged and older women. Journal of Clinical Nursing. 2015; 24(9-10):1234–1245. DOI: 10.1111/jocn.12683.


21. Bang KS, Lee IS, Kim SJ, Song MK, Park SE. The effects of urban forest-walking program on health promotion behavior, physical health, depression, and quality of life: A randomized controlled trial of office-workers. Journal of Korean Academy of Nursing. 2016; 46(1):140–148. DOI: 10.4040/jkan.2016.46.1.140.


22. Shin Y, Jang HJ, Pender NJ. Psychometric evaluation of the exercise self-efficacy scale among Korean adults with chronic diseases. Research in Nursing & Health. 2001; 24(1):68–76. DOI: 10.1002/1098-240x(200102)24:1<68::aidnur1008>3.0.co;2-c.


23. Kang SW. The validity and reliability of a lifestyle evaluation tool for patients with metabolic syndrome. Journal of Korean Academy of Fundamentals of Nursing. 2010; 17(4):487–497.
24. Choi SK, Kim IS. Effects of a cardiocerebrovascular disease prevention education program for postmenopausal middle-aged women. Journal of Korean Academy of Nursing. 2015; 45(1):25–34. DOI: 10.4040/jkan.2015.45.1.25.


25. Park MK, Kim JH. Effects of a comprehensive lifestyle improvement program for middle-aged women with cardio-cerebrovascular disease-related risk factors. Journal of Korean Academy of Community Health Nursing. 2013; 24(2):111–122. DOI: 10.12799/jkachn.2013.24.2.111.

26. Després JP. Obesity and cardiovascular disease: Weight loss is not the only target. Canadian Journal of Cardiology. 2015; 31(2):216–222. DOI: 10.1016/j.cjca.2014.12.009.

27. Pattyn N, Cornelissen VA, Eshghi SRT, Vanhees L. The effect of exercise on the cardiovascular risk factors constituting the metabolic syndrome. Sports Medicine. 2013; 43(2):121–133. DOI: 10.1007/s40279-012-0003-z.


28. Park SY, Kim CS, Nam SH. Effects of elastic band resistance exercise program on body functions and HbA1c of the elderly with type 2 diabetes. The Journal of Korean Physical Therapy. 2012; 24(5):362–369.
29. Chun KH. Evidence-based management and treatment of high-risk individuals with pre-diabetes. Journal of the Korean Medical Association. 2011; 54(10):1020–1027. DOI: 10.5124/jkma.2011.54.10.1020.

30. Wang J, Wu Y, Ning F, Zhang C, Zhang D. The association between leisure-time physical activity and risk of undetected prediabetes. Journal of Diabetes Research. 2017; 2017:4845108. DOI: 10.1155/2017/4845108.





 PDF
PDF ePub
ePub Citation
Citation Print
Print






 XML Download
XML Download