Journal List > Dement Neurocogn Disord > v.18(1) > 1121658
Echolalia is a language disorder of repeating the same words and coping what others speak. It can appear as a language impairment after cerebral infarction and there are few other treatments besides language rehabilitation.1 Post stroke emotional incontinence (PSEI), which shows emotional changes of pathologic laughing or crying is effective to serotonin reuptake inhibitor (SSRI).2 Although PSEI does not include language disorder, they have a common feature in that they both occur after cerebral infarction and have a serotonin related mechanism. This study reports a case of symptomatic improvement using SSRI in echolalia after cerebral infarction.
An 85-year-old man was unable to speak suddenly, three days after undergoing radiofrequency catheterization with atrial fibrillation. The patient was trying to speak but could not make a sound. According to neurological examination, the patient had a tendency of being drowsy and responded to the stimulation. There was slight motor weakness on the right side with no pathological reflex. At first it was thought to be Broca's aphasia.
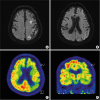
Brain diffusion-weighted image showed multifocal ischemic lesion in the left frontal lobe, parietal lobe and cerebellum. Brain MR angiography showed focal stenosis in M1 segment of right middle cerebral artery and proximal internal carotid artery (Fig. 1A and B). The patient was taking rivaroxaban but switched taking to dabigatran. Three days after the treatment, the patient began to speak simple words intermittently. In the language test, the patient had no spontaneous speech; however, he tended to repeat the words that he could hear. He could understand simple sentences, and it was therefore thought to be a transcortical motor aphasia. The patient's verbal symptoms improved during the treatment, but he began to feel depressed. A week after treatment, serotonin administration was initiated, considering the patient's condition, and taking into account both depressive mood caused by language disorder and PSEI. 10 days after admission, the Korean version of the Western aphasia test was conducted to accurately evaluate language disorders. The patient was cooperative in the test but his ability to pay attention was poor. He could answer only one out of the 6 questions asked. Fluency decreased and there were only automatic spoken expressions in repetition. The recognition of auditory sentences was somewhat possible but he repeated the last 4 words of the sentences of the question. Based on the results, the aphasia of the patient was classified as transcortical motor aphasia according to the Kertesz classification table. However, the echolalia was prominent. Thus, FDG-PET was conducted and it showed hypo-metabolism in left frontal, parietal and temporal lobe (Fig. 1C and D). A month after serotonin therapy, his depressive mood and echolalia symptom improved.
Echolalia is a disorder of repeating other's words. It happens in autism spectrum disorder, but can also appear in neurodegenerative dementia and post stroke aphasia.3 Echolalia after stroke is mainly accompanied by transcortical motor aphasia and represents about 4%–20% cases of aphasia.4
Although the exact mechanism of the disease has not been identified, it can be seen in medial frontal, anterior cingulate cortex and subcortical lesions. As in above case, it resulted in the dysfunction in ability to learn, remember and control language of left frontal lobe lesion.5
There is also a hypothesis from a neurochemical aspect, that it could be caused by immunoexcitotoxicity in the brain damage because of serotonin concentration change, resulting in dysregulation of language or memory.6 In this case, the patient was diagnosed with cerebral infarction in the left hemisphere, and at first, he was marked by echolalia. In the case of echolalia continuum, the patient had poor communication and showed automatic echolalia, which is moderate.3 Afterwards, he was scheduled to have language rehabilitation, but was given SSRI considering his depressive mood due to the possibility of PSEI. Although follow up FDG-PET showed aggravation of frontotemporal lobe uptake, language symptoms were recovered after about a month of SSRI administration. PSEI appeared in both pathologic laughing and crying, in the form of emotional symptoms that occurred after cerebral infarction.2
Recently, there have been reports of various emotional incontinence related to serotonin, it can therefore be thought to be related to the mechanism of echolalia mentioned above.2 In fact, echolalia is not within the PSEI category. However, there are reports of echolalia after cerebral infarction, and symptoms of language can also be induced PSEI or related to similar mechanisms. Therefore, through the improvement of echolalia, which is effective by the use of SSRI, it can be concluded that echolalia is associated with PSEI and it can be consider as a language incontinence. Also, serotonin-related effects can be expected on other language disorder such as paralalia and perseveration, after cerebral infarction.
1. Geschwind N, Quadfasel FA, Segarra JM. Isolation of speech area. Neuropsychologia. 1968; 6:327–340.
2. Choi-Kwon S, Han SW, Kwon SU, Kang DW, Choi JM, Kim JS. Fluoxetine treatment in poststroke depression, emotional incontinence, and anger proneness: a double-blind, placebo-controlled study. Stroke. 2006; 37:156–161.


3. Berthier ML, Torres-Prioris MJ, López-Barroso D. Thinking on treating echolalia in aphasia: recommendations and caveats for future research directions. Front Hum Neurosci. 2017; 11:164.



4. Berthier ML. Echophenomena, Automatic Speech and Prosody, in Transcortical Aphasias. East Sussex: Psychology Press;1999. p. 151–186.
- TOOLS
- ORCID iDs
-
Heewon Bae

https://orcid.org/0000-0002-2266-9288JaeYoung Park

https://orcid.org/0000-0001-8641-3786YoungSoon Yang

https://orcid.org/0000-0002-2448-2599 - Similar articles




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download