This article has been
cited by other articles in ScienceCentral.
Abstract
Thoracic outlet syndrome is a relatively well known disease. Other than trauma, this disease is mostly caused by anatomical structures that cause vascular or neural compression. The cause of thoracic outlet syndrome is diverse; however, there are only few reports of thoracic outlet syndrome caused by lipoma in the pectoralis minor space. We report a case of compression of the lower trunk of brachial plexus in which a large lipoma that developed in the pectoral minor space grew into the subclavicular space, along with a review of literature.
Keywords: Lipoma, Nerve compression syndrome, Thoracic outlet syndrome
INTRODUCTION
Thoracic outlet syndrome (TOS) occurs when the neurovascular bundle is structurally compressed at the thoracic outlet area. The pathology, symptoms, and treatment of this condition are well defined.
6) In particular, neurogenic TOS, compared with vascular TOS, is the most common type of TOS, and accounts for 95% of the cases.
6) Neurogenic TOS is mostly extrinsic compression of the neural structure due to bony or muscular structures, but abnormalities of these anatomical structures also cause the occurrence of arterial TOS.
46) Apart from these causes, there have been reports of TOS due to tumors in the thoracic outlet region.
235)
The anatomical space that can induce TOS can be divided into the interscalene triangle, costoclavicular space, and pectoralis minor space (
FIGURE 1).
14) Most cases of TOS occur in the interscalene triangle or in the costoclavicular space.
146) However, the pectoralis minor space is relatively wide, and the incidence of TOS here is low.
14) We report the anatomical features of TOS caused by a lipoma in the pectoralis minor space, with a review of the literature.
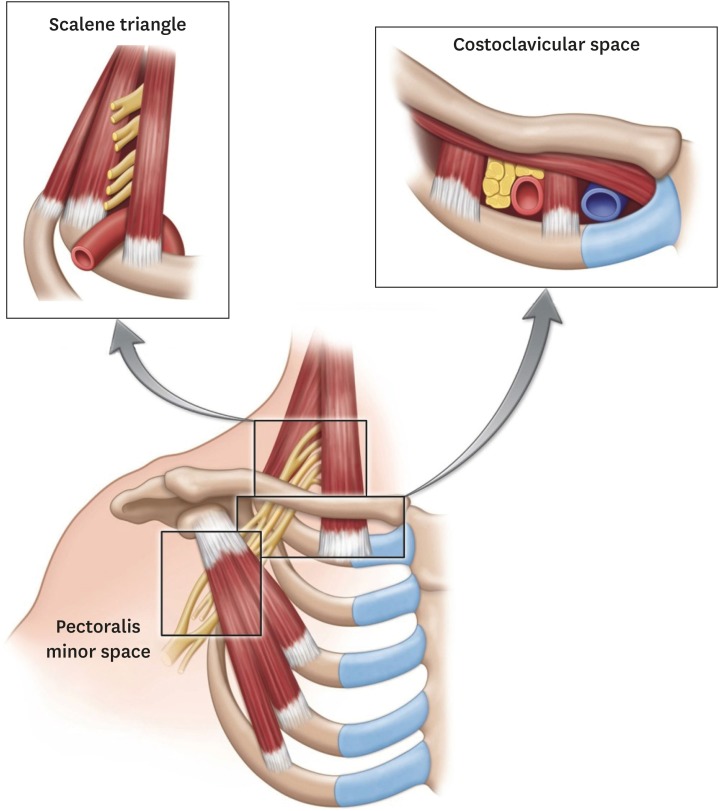
FIGURE 1
Illustration of the thoracic outlet region where thoracic outlet syndrome can occur. Permission was obtained from Wiley Online Library for reprinting this image.
CASE REPORT
We obtained informed consent from the patient.
A 45-year-old man was admitted to our hospital with paresthesia and tingling sensation in the left arm that started 3 months prior. He had an unevaluated asymptomatic mass at the left side anterior wall. Physical examination at admission revealed a palpable mass of about 0.1 meter in the right subclavicular area. Neurological examination showed paresthesia and tingling sensation with right ulnar nerve deviated dermatome, and there was no weakening of muscle strength. His symptoms worsened in a shoulder abduction test. Chest simple radiography showed a slight radiopaque round mass around the left side clavicle (
FIGURE 2A). Chest computed tomography (CT) showed a mass of well capsulated, low density mass that was growing from the pectoralis minor space to the costoclavicular space, and the subclavian vascular bundle was deviated (
FIGURE 2B & C). Coronal fat suppression T2 weight images of magnetic resonance images (MRI) revealed well capsulated, 0.05×0.06×0.13 meter of mass in pectoralis minor space, mass extended to costoclavicular space (
FIGURE 2D). Electrophysiological examination revealed conduction disturbance of the inferior trunk of the brachial plexus.
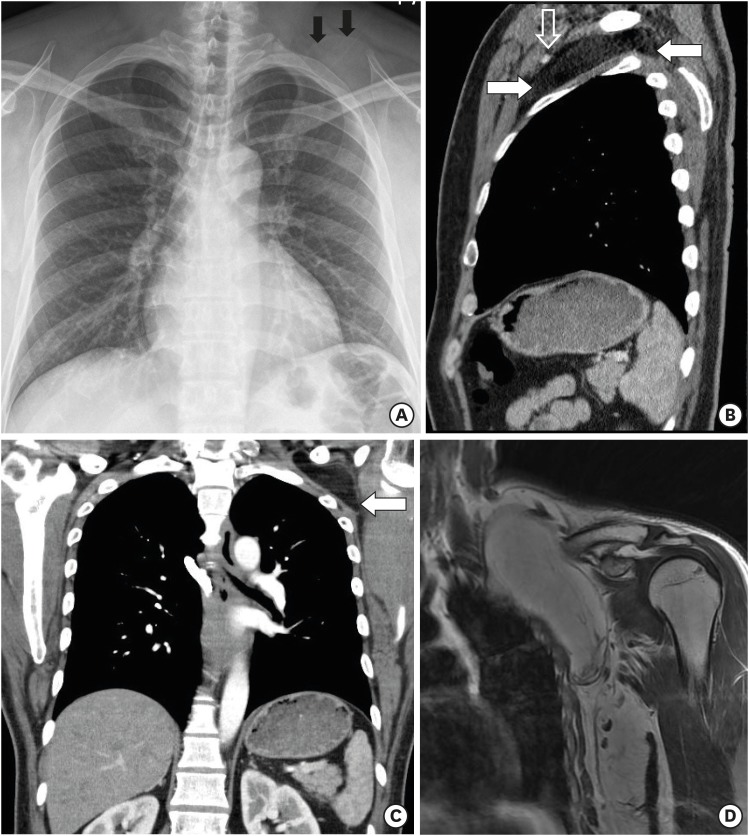
FIGURE 2
(A) Simple chest radiography showing a round mass (black arrow) in the left side upper thorax area. (B, C) Chest computed tomography showing a low density of mass between pectoralis minor space and costoclavicular space, deviated upward direction of vascular bundle (white arrow: mass, open white arrow: neurovascular bundle). (D) Magnetic resonance images of the shoulder showing a huge lipoma in the pectoralis minor space and costoclavicular space.
We performed a skin incision parallel to the clavicle under general anesthesia and retracted the pectoralis major, split the pectoralis minor, and observed a well capsulated, yellowish mass. The mass was relatively easily dissected and removed entirely by dissecting to the costoclavicular space. The mass compressed the neurovascular bundle forward in the pectoralis minor space and was adjacent to the cervical roots in the costoclavicular space. Gross photography showed well capsulated, yellowish and about 0.14 m-sized mass (
FIGURE 3A). Postoperative chest CT showed complete removal (
FIGURE 3B). All neurologic abnormalities before surgery were eliminated. There was no abnormal finding in a follow up after 1 year.
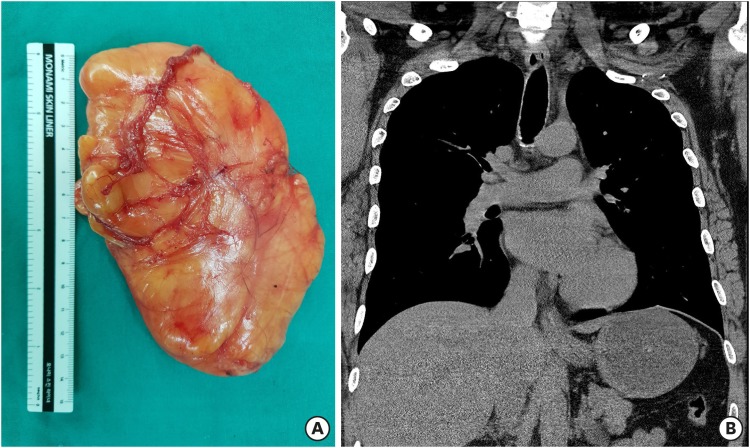
FIGURE 3
(A) Gross photography of the yellowish mass, which was about 0.14 meter. (B) The mass is absent in postoperative chest computed tomography.
DISCUSSION
TOS is a clinical syndrome caused by neurogenic or vascular compromise due to bone or musculature at the thoracic outlet area. It is caused by structural abnormalities such as clavicular deformity, cervical rib, anomalous fibromuscular band, or hypertrophic change of scalene musculature, or by occupational or repetitive strain injury.
146) However, some cases of TOS have been reported to be caused by tumors around the thoracic outlet.
235) TOS can be divided into neurogenic, arterial, and venous TOS depending on the structure entrapped, and can occur in combination. Neurogenic TOS is the most common type, and the incidence increases in the presence of structural abnormalities, especially in the case of arterial TOS.
4)
Anatomically, there are three areas where TOS can occur (
FIGURE 1).
14) First, the scalene triangle bound by the scalene muscle and clavicle: This triangle contains the 5th–8th cervical roots, 1st thoracic nerve root, and subclavian artery. Second, the costoclavicular space bound by the clavicle, scalene muscle, and first rib: This space contains three trunks of the brachial plexus, subclavian artery, and vein. At these two sites, TOS occurs due to the scalene muscle, cervical rib, and other bony prominence. The occurrence of TOS in these two sites in relatively well known. Third, the pectoralis minor space, which is the space between the ribs and pectoralis minor. This site includes three trunks and cords of the brachial plexus and an axillary vascular bundle. This space is relatively wide and less structurally abnormal than other sites, and incidence of TOS is low.
47) Most cases of TOS due to a mass have been reported in this space.
235) Demondion et al.
1) reported that the costoclavicular space and pectoralis minor space were narrowed by a symptom provoking test, but not the scalene triangle. Thus, TOS is caused by structural abnormalities in the scalene triangle, but it may occur in the other two spaces due to other reasons other than structural abnormalities.
The physical examination for TOS, such as Adson's maneuver, Halsted maneuver, Roo examination, and hyperabduction test, is a provocating test that induces symptoms by narrowing the space of the thoracic outlet.
6) The diagnosis of a mass in the pectoralis minor space is made easily by ultrasound, CT, and MRI. Kuyumdzhiev et al.
5) reported that clinical symptoms may develop if the mass is larger than 0.05 meter. In our case, the mass was 0.14 meter and was enlarged into the costoclavicular space. We believe that the brachial plexus was entrapped at the costoclavicular space and pectoralis minor space, and the patient's clinical symptoms seemed to be caused by compression of the lower trunk of the brachial plexus in the costoclavicular space as indicated by electrophysiological findings. An electrophysiological examination is not of diagnostic value in all types of TOS, but is a good method to diagnose neurogenic TOS.
6)
The primary treatment of TOS is conservative treatment.
6) However, surgical treatment is needed when there is extrinsic compression of the neurovascular bundle at the thoracic outlet area.
6) In order to predict the surgical effect, blocking the scalene muscle or pectoralis minor can be attempted to observe for improvement in the clinical symptoms.
67) In our case, because of neuropathy due to lipoma, surgical treatment was performed.
CONCLUSION
Neurogenic TOS is a rare neurologic disorder. In particular, neurogenic TOS caused by a mass in the pectoralis minor space is very rare. Here, we investigated the anatomical location and characteristics of TOS and reported this rare case with a review of the literature.





 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download