Abstract
Background
With the ageing population, number of dementia patients is on the rise, as well as the public interest. The population who would visit memory disorder clinic will also grow. The diagnostic significance of brain MRI in dementia lies in idetifying hippocampal atrophy or ischemic lesions. However, patients visiting memory disorder clinic are mostly old-aged with multiple vascular risk factors, raising the risk of cerebrovascular abnormalities. The authors set out to evaluate the need for cerebrevascular imaging in patients who visited memory disorder clinic.
Methods
The study recruited patients who visited the memory clinic in Seoul medical center between July 2011 and June 2012. Among those, patients who had taken the neuropsychiatric test and had both brain MRI and MRA taken were included for analysis. In brain MRI, severities of white matter hyperintensities and presence of cerebral infarction were assessed. In brain MRA, intra- and extra-cranial arterial stenosis and presence of aneurysm were noted.
Results
A total of 173 patients was included, and 64 were men. The mean age was 71±9.4 years, and the mean education period was 7±5.2 years. In brain MRI, white matter hyperintensities were observed in 113 patients (65.3%), and cerebral infarction was present in 57 patients (32.9%). In brain MRA, 88 (50.9%) patients showed more than one stenotic segment in intracranial vessel or proximal ICA and 6 patients (3.5%) were diagnosed with unruptured aneurysm.
Conclusions
The incidence of white matter hyperintensities or stenosis of cerebral vessels on magnetic resonance imaging is very high. Therefore, brain MRI and MRA should be included in diagnostic work up for dementia in patients who are old aged and have multiple vascular risk factors. It would provide clinicians with valuable information in making treatment decisions and prevention of future cerebrovascular accident.
Figures and Tables
Fig. 1
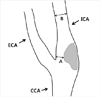
Diagram demonstrating the measurement of ICA stenosis using the NASCET criteria: NASCET (%)=(B-A)/B×100% (adapted from U-King-Im JM, et al. [11]).
References
1. Korea National Statistical Office. Population projections for Korea. 2006. Seoul: Korean National Statistical office;1–56.
2. Heo JH, Kim HS, Bae HJ, Lee K, Bae MH, Lee JB. Trend in treatment of dementia by benefit cost status based on Health Insurance Review & Assessment Service (HIRA)'s data from 2003 to 2007. Dement Neurocogn Disord. 2010. 9:135–139.
3. McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM. Clinical diagnosis of Alzheimer's disease: report of the NINCDS-ADRDA Work Group under the auspices of Department of Health and Human Services Task Force on Alzheimer's Disease. Neurology. 1984. 34:939–944.

4. Katzman GL, Dagher AP, Patronas NJ. Incidental findings on brain magnetic resonance imaging from 1000 asymptomatic volunteers. JAMA. 1999. 282:36–39.

5. Merkle S, Kreil S, Suttner G, Doelken M, Dorfler A, Richter-Schmidinger T, et al. Retrospective analysis of routine-MRI and correlation with aetiology of dementia, severity and neuropsychology in a memory-clinic population. Fortschr Neurol Psychiatr. 2011. 79:642–646.

6. Tsushima Y, Taketomi-Takahashi A, Endo K. Prevalence of abnormal findings on brain magnetic resonance (MR) examinations in adult participants of brain docking. BMC Neurol. 2005. 5:18.

7. Roman GC, Tatemichi TK, Erkinjuntti T, Cummings JL, Masdeu JC, Garcia JH, et al. Vascular dementia: diagnostic criteria for research studies. Report of the NINDS-AIREN International Workshop. Neurology. 1993. 43:250–260.

8. Petersen RC, Smith GE, Waring SC, Ivnik RJ, Kokmen E, Tangelos EG. Aging, memory, and mild cognitive impairment. Int Psychogeriatr. 1997. 9:65–69.

9. Kang YW, Na DL. Seoul Neuropsychological Screening Battery. 2003. Seoul, Korea: Human Brain Research & Consulting Co..
10. Fazekas F, Chawluk JB, Alavi A, Hurtig HI, Zimmerman RA. MR signal abnormalities at 1.5T in Alzheimer's dementia and normal aging. AJR. 1987. 149:351–356.
11. Heo JH, Lee ST, Chu K, Park HJ, Shim JY, Kim M. White matter hyperintensities and cognitive dysfunction in Alzheimer disease. J Geriatr Psychiatry Neurol. 2009. 22:207–212.

12. Heiserman J, Drayer B, Keller P, Fram E. Intracranial vascular stenosis and occlusion: evaluation with three-dimentional time-of-flight MR angiography. Radiology. 1992. 185:667–673.

13. U-King-Im JM, Trivedi RA, Cross JJ, Higgins NJ, Hollingworth W, Graves M, et al. Measuring carotid stenosis on contrast-enhanced magnetic resonance angiography: diagnostic performance and reproducibility of 3 different methods. Stroke. 2004. 35:2083–2088.

14. Uehara T, Mori E, Tabuchi M, Ohsumi Y, Yamadari A. Detection of occlusive lesions in intracranial arteries by three-dementional time-of-flight magnetic resonance angiography. Cerebrovasc Dis. 1994. 4:365–370.

15. Seshadri S, Beiser A, Selhub J, Jacques PF, Rosenberg IH, D'Agostino RB, et al. Plasma homocysteine as a risk factor for dementia and Alzheimer's disease. N Engl J Med. 2002. 346:476–483.

16. Honig LS, Kukull W, Mayeux R. Atherosclerosis and AD: analysis of data from the US National Alzheimer's Coordinating Center. Neurology. 2005. 64:494–500.

17. de Groot JC, de Leeuw FE, Oudkerk M, van Gijn J, Hofman A, Jolles J, et al. Cerebral white matter lesions and cognitive function: The Rotterdam Scan Study. Ann Neurol. 2000. 47:145–151.

18. Sacco RL, Kargman DE, Gu Q, Zamanillo MC. Race-ethnicity and determinants of intracranial atherosclerotic cerebral infarction: the northern Manhattan stroke study. Stroke. 1995. 26:14–20.

19. Lee K, Kim H, Heo JH, Bae HJ, Koh IS, Chang S. Application of magnetic resonance imaging and magnetic resonance angiography as diagnostic measures for the first attack of suspected cerebrovascular disease in Korea. Yonsei Med J. 2011. 52:727–733.

20. Heo JH, Lee KM, Park TH, Ahn JY, Kim MK. Validation of the Korean Addenbrooke's Cognitive Examination for Diagnosing Alzheimer's Dementia and Mild Cognitive Impairment in the Korean Elderly. Appl Neuropsychol Adult. 2012. 19:127–131.

21. Kim SK, Lee SY, Kang MJ, Park KW. A case of hypoperfusion dementia recovered by carotid stenting. Dement Neurocogn Disord. 2008. 7:68–71.
22. Kang JY, Kim HS, Kang MJ, Kim DH, Cha JK, Huh JT, et al. Changes on cognitive function after carotid artery stenting in patients with severe carotid artery stenosis: a prospective, 3 months follow-up study. J Korean Geriatr Soc. 2012. 16:12–20.

23. Yu KH, Lee BC, Ma HI, Kim YJ, Jeong JH, Na DL, et al. Implication of cerebral steno-occlusive lesions in patients with subcortical vascular dementia: MR angiography and FDG-PET study. Dement Neurocogn Disord. 2004. 3:29–36.




 PDF
PDF ePub
ePub Citation
Citation Print
Print






 XML Download
XML Download