Abstract
Marchiafava-Bignami disease (MBD) is a rare disorder of demyelination or necrosis of the corpus callosum. Mainly, MBD is associated with alcohol and malnutrition. We report a 60-year-old woman with no history of alcohol consumption or malnutrition who had MBD as a possible complication of normal pressure hydrocephalus (NPH). The patient presented with a 2-month history of progressive gait unsteadiness, urinary incontinence, and forgetfulness, for which the patient underwent ventriculoperitoneal shunt surgery with remarkable improvement. Magnetic resonance imaging (MRI) demonstrated hyperintensity in the body and splenium of corpus callosum when she was brought to the hospital again with rapid deterioration of her mental ststus. It might be postulated that cerebrospinal fluid (CSF) tumor necrosis factor-alpha (TNF-α) might have contributed to the development of MBD although not measured in this patient, given that TNF-α, as a proinflammatory cytokine mediating demyelinating process have been found in be increased in the CSF of NPH.
Normal pressure hydrocephalus (NPH) is a leading element of the differential diagnosis for treatable dementias. The cardinal manifestations are gait disturbance, incontinence, and dementia caused by pressure on the corticospinal leg fibers descending lateral to the ventricles, the cortical center for bladder and bowel control in the paracentral lobes, and the frontal lobes and their interconnections, respectively [1, 2]. The main treatment for NPH is the ventriculoperitoneal (VP) shunt surgery.
Marchiafava-Bignami disease (MBD) is a rare disorder mostly associated with chronic alcoholism and is characterized by symmetric demyelination and necrosis of the corpus callosum [3]. Clinical features include neuropsychiatric features, impaired consciousness, and symptoms of interhemispheric disconnection. MBD may present with rapidly progressive dementia (RPD). Two subtypes of MBD were suggested according to the clinical and radiologic features [4]. Type A is characterized by marked impairment of consciousness, extensive involvement of the corpus callosum on magnetic resonance imaging (MRI), and a poor outcome. Type B shows a normal to slight impairment of consciousness, partial lesions, and a favorable outcome. A case of MBD with no history of alcoholism or malnutrition was reported in a patient with diabetes mellitus [5], although MBD has usually been reported in patients with alcoholism or malnutrition. We report a patient with MBD type A possibly superimposed on NPH in the absence of alcohol consumption or malnutrition and also in the setting of well controlled blood sugar level.
A 60-year-old right-handed diabetic woman presented with a 2-month history of progressive gait unsteadiness, urinary incontinence, and forgetfulness to the neurosurgery department. She also had difficulty in carrying out daily routine activities and needed some assistance. Her past medical history was remarkable for diabetes which was well controlled. A neurological examination revealed gait unsteadiness, memory impairment. Once NPH was suspected. MRI of the brain showed symmetric dilatation of all the ventricles without signal changes in the corpus callosum (Fig. 1A-C). The Evan index (the ratio of maximum diameter of the frontal horns to the maximum width of the cranial cavity at the same level) was 0.56. There were no significant white matter abnormalities. A diagnosis of NPH was made, a cerebrospinal fluid (CSF) tap test was performed, and 50 ml of CSF was drained. CSF study was unremarkable for the opening pressure, the cell counts, and the protein and sugar levels. The patient underwent ventriculoperitoneal (VP) shunt surgery and there was a remarkable improvement in gait disturbance, urinary incontinence, and cognitive disturbance. The patient was sent home approximately 4 week after the VP shunt.
Two months later, the patient was brought to the emergency room due to rapidly deteriorating level of consciousness preceded by progressive gait disturbance for a few days. The patient underwent VP shunt revision twice in the neurosurgery department under the possibility of shunt failure. Nonetheless, her changed consciousness did not recover, so the patient was refered to the neurology department for evaluation of RPD. On neurological examination, the patient was stuporous and had quadriparesis. Blood biochemistry, electrolytes, nutrition and endocrine functions were all within the normal limits. The Body mass index (BMI) was 23. The CSF studies showed no abnormal findings. Extensive work up with heavy metals, Human immunodeficiency virus, and autoimmune antibodies test was negative. Follow-up CT revealed hypodense lesions in the corpus callosum (Fig. 1D-F). MR imaging showed the lesions suggestive of demyelination in the body and splenium of corpus callosum (Fig. 1G-I) and was devoid of lesions typical of acute disseminated encephalomyelitis or multiple sclerosis. On follow-up neurological examination, the patient was able to open her eyes spontaneously, but did show voluntary limb movements.
She showed preserved saccadic eye movement to the direction of auditory sources to either side. She had blinking on visual threatening on bilateral visual fields.
The patient was diagnosed with MBD based on the clinical and typical MRI findings. It is nocitable that she developed MBD while her diabetes has been well controlled and she had neither history of alcohol consumption nor malnutrition. The patient has been treated conservatively with thiamine, fluoxetine, and dopamine agonist which did not make any significant changes in her clinical courses.
Marchiafava-Bignami disease is a rare disorder of demyelination or necrosis of the corpus callosum and adjacent subcortical white matter that occurs predominantly in the malnourished or the alcoholics. However, MBD in a diabetic patient was reported in the absence of malnutrition in Japan [5]. It was postulated that the untreated diabetes might have caused hyperosmolar state which induced central demyelination of MBD.
Interestingly, it is notable that the present case had no history of alcohol consumption, malnutrition and diabetes has been under good control. For this patient, it is not clear what condition have precipitated the development of MBD. It was reported that the levels of tumor necrosis factor-alpha (TNF-α), a proinflammatory cytokine mediating demyelinating process, were increased in the CSF of NPH patients and correlated with the levels of sulfatide, a marker for white matter changes [6].
It might be postulated that CSF TNF-α might have contributed to the development of MBD at least in part, although the CSF levels of TNF-α were not measured in this patient. We may include the possibility of MBD into the lists of differential diagnosis and complications of NPH when the patients show changes in the mental status as in this patient, although the causative relationship between two diseases remains elusive.
Figures and Tables
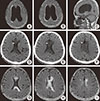 | Fig. 1The findings on the MRI and CT of the brain. The initial axial and saggital MR images reveal the enlarged ventricles (A-C). Brain CT images 2 months after the readmission show the hypointense lesions in the corpus callosum (D-F) and axial fluid-attenuated inversion recovery (FLAIR) MR images demenstrate the lesions with hyperintensity in the corpus callosum (G-I). |
References
1. Factora R, Luciano M. Normal pressure hydrocephalus: diagnosis and new approaches to treatment. Clin Geriatr Med. 2006; 22:645–657.

2. Hebb AO, Cusimano MD. Idiopathic normal pressure hydrocephalus: a systematic review of diagnosis and outcome. Neurosurgery. 2001; 49:1166–1184. discussion 1184-66.

3. Castaigne P, Buge A, Cambier J, Escourolle R, Rancurel G. [Marchiafava-Bignami disease: anatomoclinical study of 2 cases]. Rev Neurol (Paris). 1971; 125:179–196.
4. Heinrich A, Runge U, Khaw AV. Clinicoradiologic subtypes of Marchiafava-Bignami disease. J Neurol. 2004; 251:1050–1059.

5. Suzuki Y, Oishi M, Ogawa K, Kamei S. A patient with Marchiafava-Bignami disease as a complication of diabetes mellitus treated effectively with cortico steroid. J Clin Neurosci. 2012; 19:761–762.

6. Tarkowski E, Tullberg M, Fredman P, Wikkelsö C. Normal pressure hydrocephalus triggers intrathecal production of TNF-alpha. Neurobiol Aging. 2003; 24:707–714.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download