Abstract
Background
Alzheimer's disease is a chronic neurodegenerative condition, mostly affecting the medial temporal lobe and associated neocortical structures. In this report, we present a rare clinical manifestation of this disease.
Case Report
A 61-year-old female with word finding difficulty and memory disturbances was diagnosed with Alzheimer's disease. Two years later, she complained of right homonymous hemianopia without optic ataxia, ocular apraxia, and simultagnosia. No findings other than parenchymal disease were apparent in magnetic resonance imaging and laboratory tests.
Conclusions
In this case, in a patient initially diagnosed with Alzheimer's dementia with progressive disease, we found only homonymous hemianopia, without signs of Balint's syndrome or Gerstmann's syndrome. After careful investigation showing that Alzheimer's dementia with visual symptom was not associated with parenchymal disease, we concluded a case of atypical variant of Alzheimer's disease.
Alzheimer's disease is a chronic neurodegenerative condition, mostly affecting the medial temporal lobe and associated neocortical structures.1 Cognitive decline is the most common symptom. Other atypical symptoms include behavioral and personality changes, Balint's syndrome, and Gerstmann's syndrome.2
Here we report a case of Alzheimer's disease with homonymous hemianopsia without evidence of another parenchymal brain disease. Posterior cortical atrophy with hemianopsia was previously reported in Italy3 and Japan.4 However, to the authors' knowledge, this is the first report of Alzheimer's disease with homonymous hemianopsia in Korea.
In 2012, a 61-year-old female visited the clinic with word-finding difficulty and memory disturbances. Her family complained that she had trouble retrieving words and took longer to answer questions. She had no past medical history except for hypertension. We carried out neurologic and neuropsychological evaluation, including a Korean version of Mini-Mental State Examination (K-MMSE), brain magnetic resonance imaging (MRI), and further laboratory tests.
No abnormal findings were apparent in neurological and physical examination except impairment in delayed recall. However, the neuropsychological test revealed impairment in general neurocognitive function, especially in language, visual and verbal memory, and recognition (Table 1).
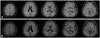
Electroencephalography and other laboratory findings were normal. Brain MRI showed mild cortical atrophy (Fig. 1). We diagnosed the patient with probable Alzheimer's disease, and she visited the clinic regularly.
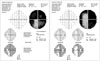
Two years later, she complained she could not detect objects on her right side. Ophthalmologic testing revealed right-side homonymous hemianopsia (Fig. 2). There were no abnormal findings associated with ophthalmic disease.
The patient visited the hospital for further investigations. Her vital signs were stable and MRI of her brain did not reveal any symptoms of parenchymal disease, such as cerebrovascular disease (Fig. 1). Her K-MMSE score declined to 13. Neurological examination did not show ocular apraxia, or simultagnosia. In addition, there was no sign of agraphia or finger agnosia. The patient diagnosis was posterior type of Alzheimer's disease.
Informed consent was obtained for the case report.
In 1988 Benson et al.5 reported patients with visual symptoms without ophthalmic problems, a syndrome later termed posterior cortical atrophy. The most common features of this condition involve visuospatial impairments, alexia, and features of Balint's and Gerstmann's syndrome.6 Executive and memory functions are intact in the early stages of this condition. Alzheimer's disease is the most common underlying cause of posterior cortical atrophy, which has been regarded as a variant of Alzheimer's dementia. However, currently pathological features such as Lewy bodies, prion disease, or corticobasal ganglionic syndrome are associated with posterior cortical atrophic syndrome.78
Compared with the cases reported in Italy and Japan, our patient showed a relatively early impairment in executive function and memory. In addition, considering the fact that posterior cortical atrophy or visual variant of Alzheimer's dementia usually affects the right hemisphere more severely, the right-side hemianopsia involving left hemisphere is an atypical presentation.910 Also, no signs of Balint's or Gerstmann's syndrome were observed, except for right-left disorientation. However, several reports suggest that hemianopsia is a rare first symptom of posterior cortical atrophy111213 and eventually affects the higher visual functions.6 We suggested a retrochiasmal deficit of the visual pathway as the pathology of Alzheimer's disease such as neurofibrillary tangles and senile plaques progressed and affected primary visual cortex and associated visual area.14 Although the patient's neurologic examination and perimetry showed homonymous hemianopsia, we cannot exclude unilateral right optic ataxia. To the best of our knowledge, no report of unilateral optic ataxia involving posterior cortical atrophy is available. However, it is known that unilateral optic ataxia can occur when contralateral parietal lobule is affected.1516 Therefore, unilateral optic ataxia may develop as Alzheimer's disease progressed in the left parietal lobule, masked by homonymous hemianopsia.
The primary symptoms of posterior cortical atrophy and visual variant of the Alzheimer's dementia are predominantly visual and patients often visit ophthalmology clinic initially.1718 However, with this case, we insist the importance of considering neurodegenerative disease in elderly patients with visual defects.
Figures and Tables
References
1. De-Paula VJ, Radanovic M, Diniz BS, Forlenza OV. Alzheimer's disease. Subcell Biochem. 2012; 65:329–352.

3. Pellegrini F, Lee AG, Zucchetta P. Homonymous hemianopsia due to posterior cortical atrophy. Neuroophthalmology. 2017; 41:154–158.

4. Ishiwata A, Kimura K. Homonymous hemianopsia associated with probable Alzheimer's disease. J Nippon Med Sch. 2016; 83:87–92.

6. Crutch SJ, Lehmann M, Schott JM, Rabinovici GD, Rossor MN, Fox NC. Posterior cortical atrophy. Lancet Neurol. 2012; 11:170–178.

7. Renner JA, Burns JM, Hou CE, McKeel DW Jr, Storandt M, Morris JC. Progressive posterior cortical dysfunction: a clinicopathologic series. Neurology. 2004; 63:1175–1180.

8. Tang-Wai DF, Graff-Radford NR, Boeve BF, Dickson DW, Parisi JE, Crook R, et al. Clinical, genetic, and neuropathologic characteristics of posterior cortical atrophy. Neurology. 2004; 63:1168–1174.

9. Snowden JS, Stopford CL, Julien CL, Thompson JC, Davidson Y, Gibbons L, et al. Cognitive phenotypes in Alzheimer's disease and genetic risk. Cortex. 2007; 43:835–845.

10. Mendez MF, Ghajarania M, Perryman KM. Posterior cortical atrophy: clinical characteristics and differences compared to Alzheimer's disease. Dement Geriatr Cogn Disord. 2002; 14:33–40.

11. Shea YF, Chu LW. Visual field defect as an uncommon presentation of posterior cortical atrophy. Geriatr Gerontol Int. 2014; 14:1003–1004.

12. Cordano C, Alessandria G, Leonardi A, Cellerino M, Nourbakhsh B, Nobili F, et al. Homonymous hemianopia as the first sign of posterior cortical atrophy. J Neurol Sci. 2017; 373:38–40.

13. Wan SL, Bukowska DM, Ford S, Chen FK. Posterior cortical atrophy presenting with superior arcuate field defect. Case Rep Ophthalmol Med. 2015; 2015:796381.

15. Auerbach SH, Alexander MP. Pure agraphia and unilateral optic ataxia associated with a left superior parietal lobule lesion. J Neurol Neurosurg Psychiatry. 1981; 44:430–432.

16. Perenin MT, Vighetto A. Optic ataxia: a specific disruption in visuomotor mechanisms. I. Different aspects of the deficit in reaching for objects. Brain. 1988; 111(Pt 3):643–674.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download