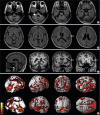
MRI showed atrophy of the cerebellum, insular cortex, fusiform gyrus, inferior orbito-frontal gyrus, superior temporal gyrus, and caudate nucleus in the MSA patient with cognitive impairment.
5 Impairment of frontal lobe-related functions was reported in 41% of MSA-C type.
6 Patient's initial manifestation appeared to be normal, however, explosive speech started after olanzapine therapy. There are two neural networks in the synthesis of human speech.
7 The first network is a motor pathway for primitive vocalizations, which passes through the anterior cingulate gyrus and the adjacent mesiofrontal regions and projects via midbrain, basal ganglia, and pons to cranial nerve motor nuclei in the lower brainstem responsible for the innervation of vocal tract musculature.
8 The second extensive network contributes to complex forms such as linguistically meaningful sounds. At the cortical level, this second pathway encompasses the lateral and medial premotor regions and the supplementary motor area (SMA) involving the anterior insula.
8 At the subcortical level, the basal ganglia and the cerebellum are critically involved in this network.
18 Drug-induced speech defects have been reported following treatment with neuroleptics including clozapine and phenothiazines, theophylline, tricyclic antidepressants, selective serotonin reuptake inhibitors and benzodiazepine.
9 The patient's explosive speech might be attributed to not only atrophy of the frontal operculum, especially dysfunctional left side affecting cerebellar-cortical circuit in the secondary pathway of premotor area and SMA but also by olanzapine therapy resulting in MSA-C. A few case reports suggested a possible relationship between olanzapine and speech defects including dysarthria, decreased speech speed, verbal output, and voice volume.
1011
The limitations of this study related to determination of the onset time of abnormal symptoms based on the patient's subjective reports and not based on the physician's close observations. In addition, due to ethical constraints, olanzapine re-administration to confirm the causal relationship was not carried out. Although it depends on the subtype of MSA, speech defect in MSA-C was characterized by progressive scanning dysarthria with gait ataxia and limb kinetic ataxia.
1213 This patient was clinically diagnosed based on olanzapine-related symptoms due to the speech defects occurring in the immediate aftermath of olanzapine treatment. We reported this MSA patient manifesting irreversible explosive speech following olanzapine therapy as an unusual finding.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download