Abstract
For a 67-year-old man with diabetes mellitus, a 9-cm liver mass was found on CT during the diagnostic work-up for weight loss and fever. Dynamic CT and MRI showed a layered pattern of contrast enhancement suggesting the imaging features of the solid inflammatory mass. After tissue diagnosis of immunoglobulin G4 (IgG4)-related disease by gun needle biopsy, steroid therapy induced partial shrinkage of the mass on the follow-up CT at 4 weeks. On the 5-month follow-up CT with the maintenance of low-dose oral steroid medication, disease progression with invasion to diaphragm brought surgical intervention of right hemihepatectomy considering the possibility of combined malignancy. In the area of diaphragmatic destruction, focal actinomycosis was complicated in the main mass of IgG4-related disease. We are the first to describe a rare case of IgG4-related inflammatory pseudotumor, complicated by actinomycosis, showing an invasive nature that mimicked malignancy during steroid therapy in a diabetic patient.
Hepatic involvement of immunoglobulin G4 (IgG4)-related diseases may reveal a broad spectrum of hepatopathies involving the liver parenchyma and bile ducts; among them, intrahepatic mass-formation has been rarely reported (1). For the treatment of histologically confirmed IgG4-related hepatic inflammatory pseudotumor, steroid therapy could be applied preferentially like other IgG4-related disease instead of surgical intervention (2,3). Meanwhile, there is a potential of secondary infection as a complication of long-term steroid use especially for the immunocompromised patients (4). In this report, we describe a rare case of mass-forming IgG4-related disease of the liver complicated by actinomycosis showing invasive nature mimicking malignancy during steroid therapy with emphasis on its imaging features and discuss their clinicopathological properties.
A 67-year-old man came to our tertiary referral hospital for further investigation of his liver abscess. He was suffering from fever and diagnosed to have liver abscess in abdomen-pelvis CT and treated with antibiotics in an external general hospital. He had a history of 5 kg weight loss over 3 months. For three years he was on oral medication for diabetes mellitus and hypertension. Upon admission, laboratory results showed elevated alkaline phosphatase (118 IU/L; normal range, 39–111 IU/L), elevated gamma-GT (76 IU/L, normal range: 8–46), elevated serum glucose (254 mg/dL, normal range: 80–118) and elevated C-reactive protein (67 mg/L, normal range: 0.1–6.0).
Initial dynamic abdomen-pelvis CT showed a large (8.5 × 7.8 × 8.9 cm) mass in the right hepatic lobe with gradual and delayed rind-like enhancement of the outer portion of the mass and hyperemic change of adjacent hepatic parenchyma with segmental portal vein obliteration favoring the impression of solid inflammatory mass rather than tumorous condition (Fig. 1A upper left and 1A upper middle). For further characterization, a liver MRI was performed and showed similar dynamic imaging features in addition to nonspecific T1-weighted hypointensity and T2-weighted hyperintensity (Fig. 1A upper right and 1A lower left). Diffusion-weighted imaging showed higher apparent diffusion coefficient for the outer component of delayed enhancement from the restricted diffusion in the central portion in the mass (Fig. 1A lower middle). Positron emission tomography-CT showed a nonspecific strong fludeoxyglucose uptake (standardized uptake value = 9) (Fig. 1A lower right).
For histopathologic confirmation, sonography-guided core needle biopsy was conducted uneventfully, and the pathologic report described that the tissue was consisted of an abscess with abundant fibrosis and increased IgG4-positive lymphoplasma cells (about 30/high-power field) compatible with IgG4-related disease. The immunohistochemical stain results showed cytokeratin (ALK)-19 positivity in biliary ducts and anaplastic lymphoma kinase negativity. The serum IgG4 quantitation level at that time was increased to 2215.8 mg/dL (normal range: 800–1800 mg/dL). Oral steroid therapy started, and the dose of prednisolone was 40 mg/day for the first two weeks, tapered by 5 mg per 2 weeks until the dose reached 5 mg/day.
In the 4-week follow-up CT after the start of steroid therapy, the inflammatory mass partially resolved to 8.1 × 5.8 × 6.0 cm (50% volume loss) (Fig. 1B upper left). Oral prednisolone medication continued with 25 mg/day for 2 weeks, 15 mg for the next 2 weeks and followed by 5 mg/day for maintenance. Second follow-up CT and MRI were performed after 4 months since the first follow-up CT, and revealed that the mass rather enlarged to 8.9 × 7.0 × 6.3 cm (139% in volume) since the last examination and expanded to the lower lobe of right lung with destruction of the right hemidiaphragm (Fig. 1B upper right, lower left, and lower right). Due to the failure of steroid therapy and the possibility of combined malignancy for the invasive nature, right hepatectomy and wedge resection of the right lung were performed (Fig. 1C upper left). The pathologic specimen showed dense lymphoplasmocytic infiltration with fibrosis and abscess formation containing actinomycotic colonies in the uppermost part of liver and lower lung parenchyma (Fig. 1C upper right, lower left, and lower right). Due to the eccentric and focal actinomycotic colonies, the histopathological features indicated a superimposed infection of actinomycosis over IgG4-related diseases. So far, there has been no evidence of recurrence or progression of the symptom for 10 months.
Shibata et al. (4) reported a case of IgG4-related hepatic inflammatory pseudotumor with a review of 11 cases of previously reported mass forming IgG4-related liver disease about the clinical findings of elevated serum IgG4 levels, combined IgG4-related disease in addition to the size and location of hepatic lesion. Five did not provide any information about the combined disease. Of the other seven patients, sclerosing cholangitis (n = 3), autoimmune pancreatitis (n = 1), tubulointerstitial nephritis (n = 1) or mass forming inflammatory lesion in the esophagus with a gastric ulcer (n = 1) while there was no combined disease in the Shibata et al.'s own case (4) like the present patient.
The imaging findings of IgG4-related hepatic inflammatory pseudotumor have not been specifically reported, and it is necessary to refer to broad-concept inflammatory pseudotumor. Considering that the liver involvement of IgG4-related disease is basically broad spectrum, mass-forming lesions may appear as nonspecific infiltrative masses with or without combined sclerosing cholangitis. The present patient showed the delayed enhancement of thick peripheral rind on the first dynamic cross-sectioning imaging mimicking solid organizing abscess or the majority features of various inflammatory pseudotumor in the liver (5,6). These findings have been also reported in inflammatory mass suggestive of infectious origin which were described as inflammatory myofibroblastic tumors depending on the positivity of immunochemical staining of smooth muscle actin (7). Contrast enhancement pattern of gradually enhancing thick and rather poorly-defined outer layer could be useful to exclude the possibility of neoplastic conditions like hepatocellular carcinomas which could have thin and smooth outer pseudocapsules or intrahepatic cholangiocarcinoma and many hepatic metastases showing a different layered pattern of early enhancing peripheral cellular portion and gradual centripetal diffusion into the inner noncellular component (8).
For management of the present patient, the lesion was not resolved in size even though the patient had received antibiotics based on the impression of abscess during the initial care in the other hospital. After histological diagnosis of IgG4-related inflammatory pseudotumor by percutaneous core needle biopsy, the treatment strategy changed according to the consensus statement for use of corticosteroids as the most appropriate treatment for IgG4-related disease including the hepatic mass forming lesions (2,3). Although it was the largest of the mass-forming lesions reported so far, the present patient was treated with tapering dose of prednisolone. About 50% of volume reduction at 1-month follow-up CT anticipated complete resolution of the lesion by the low-dose maintenance of the oral prednisolone; however, the lesion enlarged again with an invasive feature of extension to the lung through the right hemidiaphragm on the 5 months-follow-up imaging studies. In this situation, regardless of the tissue diagnosis of IgG4-related disease, surgical resection performed due to the failure of steroid therapy with a suspicion of combined malignancy (9).
Actinomycosis can be depicted as mass forming lesion in the liver and used to be confused from hepatic malignancy due to its invasive nature. The imaging finding of hepatic actinomycosis is rather nonspecific that most of the lesions are nonhypervascular with fuzzy margin (10). In the pathologic specimen actinomycotic colonies were focally found around the diaphragm in the present patient. Recently, Shibata et al. (4) reported a case that IgG4-related hepatic inflammatory pseudotumor was completely replaced by pyogenic abscess showing typical imaging feature containing the wide centrally necrotic area different from the present patient showing solid appearance during steroid treatment. The patient also suffered from diabetes mellitus like the present patient, and thus belongs to immune-compromised patient. Since the diabetes was not well controlled by oral medication before and after treatment, it was likely that secondary infection accompanied with steroid treatment in both cases by different pathogens. Although steroid therapy is known to be most suitable for IgG4-related, if immuno-compromised status is difficult to be controlled consistently, long-term use of steroids should be more carefully considered. Especially in the cases of large solitary mass-forming lesions, even if suggested to be benign, early surgical resection may be helpful to reduce their morbidity.
In summary, IgG4-related disease was identified by biopsy with imaging findings suggestive of inflammatory pseudotumor for the large mass with a gradually enhancing thick outer layer found in the patient with nonspecific symptom such as weight loss and fever. After the partial temporary resolution by steroid therapy, actinomycosis occurred as a complication of uncontrolled diabetes mellitus, therefore, the invasive nature of diaphragmatic destruction could not exclude the possibility of combined malignancy. In this report, we first describe the superimposed actinomycosis as the adverse effect of steroid treatment for a rare IgG4-related hepatic inflammatory pseudotumor. Recalling the knowledge of image findings, clinical background and the mechanism of the disease progression in this rare situation might be helpful in the future management of patients with related disease problems.
Figures and Tables
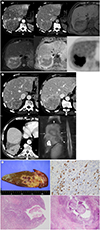 | Fig. 1IgG4-related hepatic inflammatory pseudotumor complicated by actinomycosis during steroid therapy in a 67-year-old man presenting with fever and abdominal pain.
A. Initial axial CT of arterial phase shows a large soft tissue mass consisted of internally inhomogeneous contrast enhancement surrounded by hypovascular rind (arrowheads) and adjacent parenchymal hyperemia in the right hepatic lobe (upper left). On the equilibrium phase of the same section of (upper left), contrast enhancement of the outer portion (arrowheads) looks stronger than the internal component and reflects fibrotic component in the peripheral portion of the lesion suggesting an inflammatory mass (upper middle). Axial T1-weighted (upper right) and T2-weighted (lower left) MRIs show roughly targetoid component of the same lesion, and apparent diffusion coefficient map (lower middle) shows peripheral area of high fluid contents (arrowheads) corresponding to the T1-weighted hypointensity and T2-weighted hyperintensity suggesting inflammation rather than solid tumor. Axial positron emission tomography-CT shows nonspecifically strong fludeoxyglucose uptake (lower right).
B. Four-week follow-up axial CT in portal venous phase since the start of steroid therapy shows shrinkage of the lesion (arrowheads) in about 50% in volume (upper left). Two axial images of 5-month follow-up CT in portal venous phase since the start of steroid therapy shows the enlargement of the mass (arrowheads) with superiorly extended to the lower lobe of right lung across the right hemidiaphragm (upper right, lower left). Five-month follow-up coronal T2-weighted MRI (lower right) shows the mass (arrowheads) extended across the right hemidiaphragm (arrows), and preexisting hepatic cyst (asterisk).
C. Gross photography and microscopic photographies of liver parenchyma and lung parenchyma after right hepatectomy and wedge resection from right lower lobe. Gross photography of the coronal section after mass excision (upper left) shows yellowish vaguely defined lesion, measuring 10 × 5 cm involving liver and lung parenchyma through the right hemidiaphragm. On the microscopy, lots of IgG4-positive plasma cells are scattered in the background of inflammatory cells (upper right; IgG4 staining, × 400). Focal actinomycotic colonies are also defined around the destructed right hemidiaphragm in the upper portion of the liver (lower left; H&E, × 40) and lower lung parenchyma (lower right; H&E, × 12.5).
H&E = hematoxylin and eosin stain, IgG4 = immunoglobulin G4
|
References
1. Hedgire SS, McDermott S, Borczuk D, Elmi A, Saini S, Harisinghani MG. The spectrum of IgG4-related disease in the abdomen and pelvis. AJR Am J Roentgenol. 2013; 201:14–22.


2. Deshpande V, Zen Y, Chan JK, Yi EE, Sato Y, Yoshino T, et al. Consensus statement on the pathology of IgG4-related disease. Mod Pathol. 2012; 25:1181–1192.

3. Umehara H, Okazaki K, Masaki Y, Kawano M, Yamamoto M, Saeki T, et al. A novel clinical entity, IgG4-related disease (IgG4RD): general concept and details. Mod Rheumatol. 2012; 22:1–14.


4. Shibata M, Matsubayashi H, Aramaki T, Uesaka K, Tsutsumi N, Sasaki K, et al. A case of IgG4-related hepatic inflammatory pseudotumor replaced by an abscess after steroid treatment. BMC Gastroenterol. 2016; 16:89.



5. Kim YK, Kim CS, Lee JM, Ko SW, Moon WS, Yu HC. Solid organizing hepatic abscesses mimic hepatic tumor: multiphasic computed tomography and magnetic resonance imaging findings with histopathologic correlation. J Comput Assist Tomogr. 2006; 30:189–196.

6. Ahn KS, Kang KJ, Kim YH, Lim TJ, Jung HR, Kang YN, et al. Inflammatory pseudotumors mimicking intrahepatic cholangiocarcinoma of the liver; IgG4-positivity and its clinical significance. J Hepatobiliary Pancreat Sci. 2012; 19:405–412.


7. Yu JS, Park C, Kim JH, Chung JJ, Kim KW. Inflammatory myofibroblastic tumors in the liver: MRI of two immunohistochemically-verified cases. J Magn Reson Imaging. 2007; 26:418–421.

8. Lamba R, Fananapazir G, Corwin MT, Khatri VP. Diagnostic imaging of hepatic lesions in adults. Surg Oncol Clin N Am. 2014; 23:789–820.






 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download