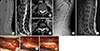
A 19-year-old male presented with the chief complaint of progressive back pain and bilateral buttocks pain. Computed tomography revealed a spinal canal widening and remodeling at the level of T11-L1 (Fig. 1A). Magnetic resonance imaging (MRI) revealed an extradural cystic lesion in the dorsal aspect of the thecal sac at the level of T11-L1. The cystic lesion had several septations and the cystic fluid showed a signal intensity similar to that of cerebrospinal fluid. (Fig. 1 B–D).
The patient underwent osteoplastic laminotomy at the levels of T12 and L1. The cystic wall was thin and transparent in the microscopic view (Fig. 1E). Dissection of a multilayered transparent membrane and partial removal of the ventral cystic wall revealed a communicating defect at the dural sleeve near the right T12 rootlet. Herniated rootlets were identified within the dural defect and the defect was closed with primary suturing without sacrifice or injury of the rootlets (Fig. 1F, G). Pathological examination demonstrated an arachnoid cyst mixed with a flattened epithelium. On the basis of these findings, the lesion was diagnosed as an extradural meningeal cyst. The six month follow-up plain radiography and MRI showed no recurrence and the patient was satisfied with the outcome and had no neurological complications. (Fig. 1H, I).
Spinal extradural meningeal cysts are rare. In the past, the entire cyst was removed for treatment, as the etiology was unclear.1 The cause of a meningeal cyst is now thought to be fluid accumulation due to a dural defect after trauma.2 The treatment goal has also changed to primary closure of the dural defect through hemilaminectomy or laminotomy, removing only part of the ventral cystic wall.23 With this approach, the cyst can be treated less invasively, and an excellent treatment outcome can be expected. Therefore, we suggest that disruption of the communicating tract through primary closure of the dural defect is the key to management of an extradural meningeal cyst.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download