Abstract
Purpose
The purpose of this study was to examine the effects of breathing exercises performed using panflutes in elderly patients undergoing spinal surgery.
Methods
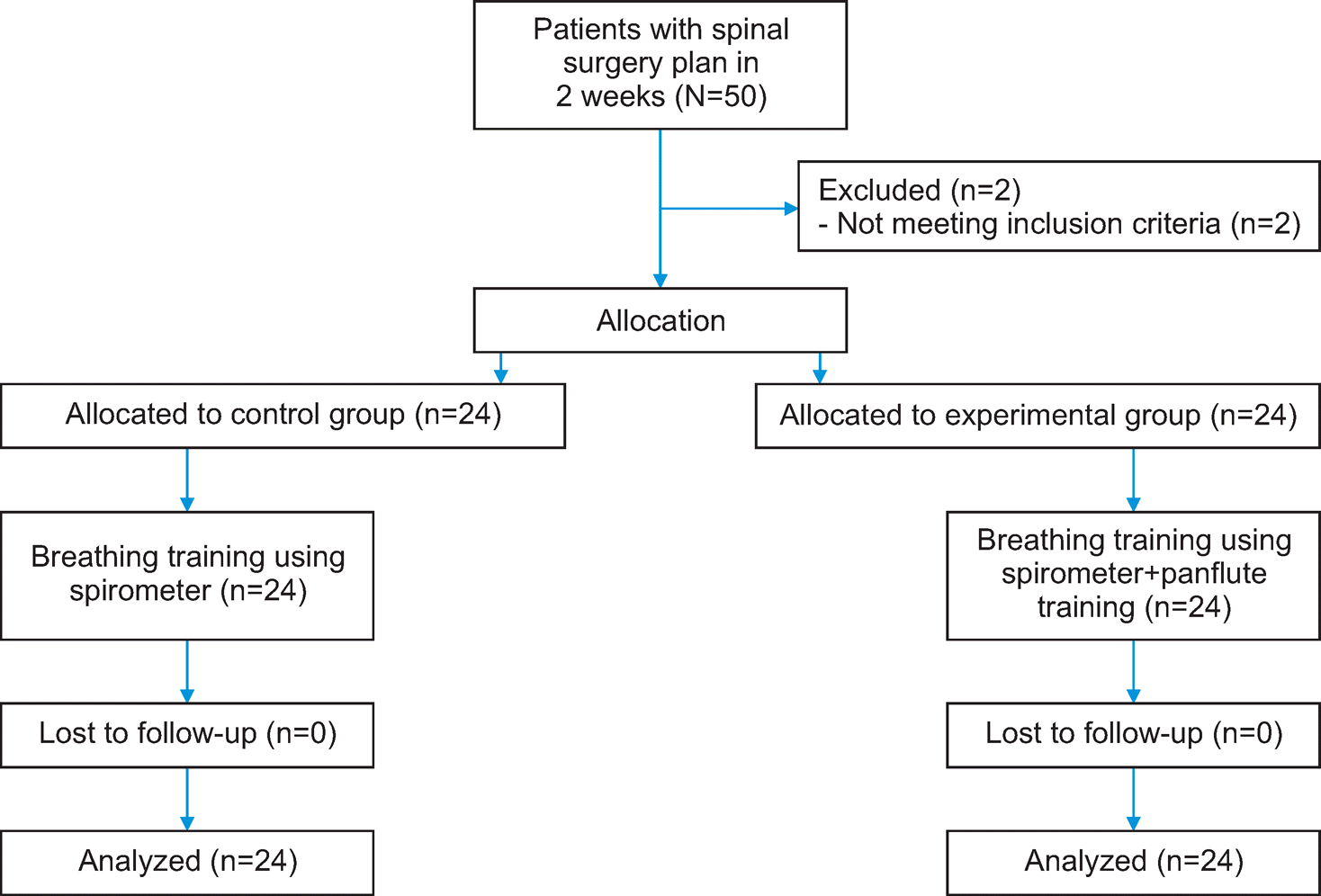
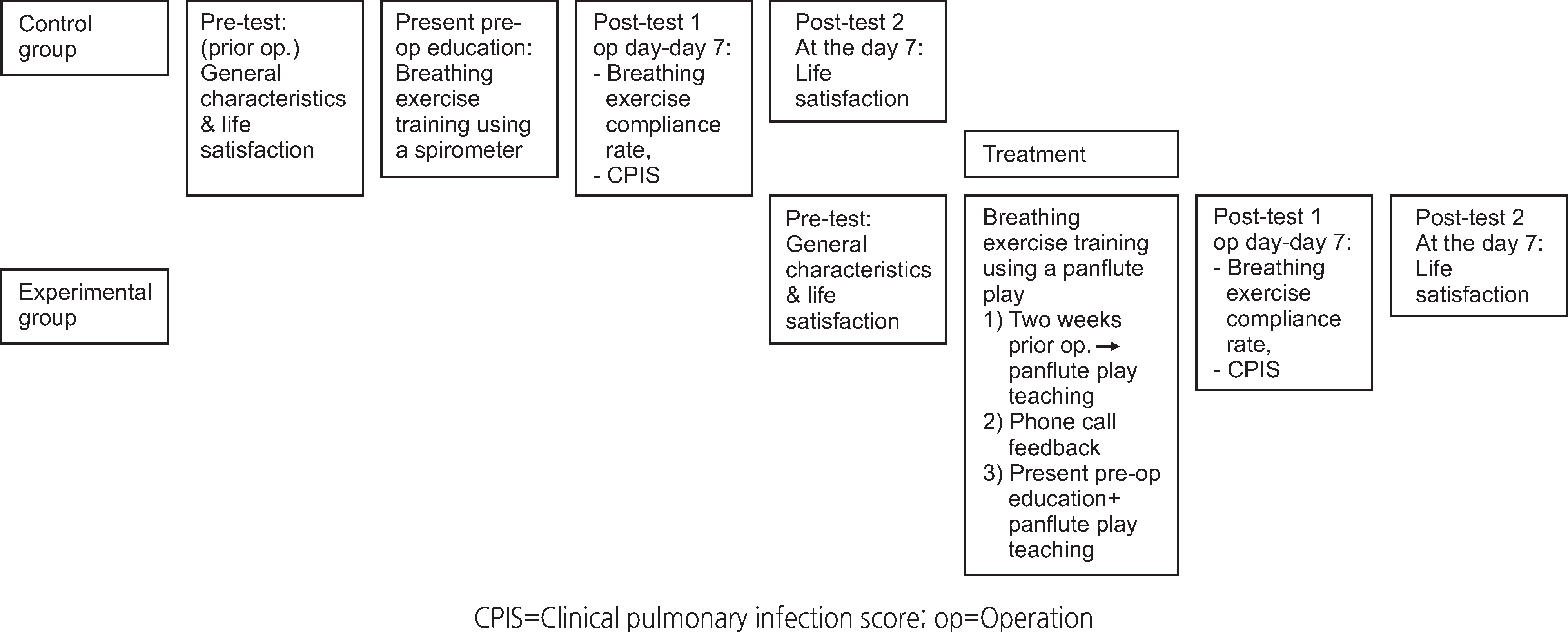
The study design was a nonequivalent control group non-synchronized pre-post test. The study included 24 patients in both the experimental group and the control group. The experimental group completed a daily breathing exercise regimen using panflutes for 30minutes after meals, whereas the control group was provided standard preoperative education, including breathing exercises using incentive spirometers. After the exercise regimen, breathing exercise compliance, pulmonary infections, and life satisfaction were measured in both groups, and the data were analyzed using the SPSS/WIN program.
Results
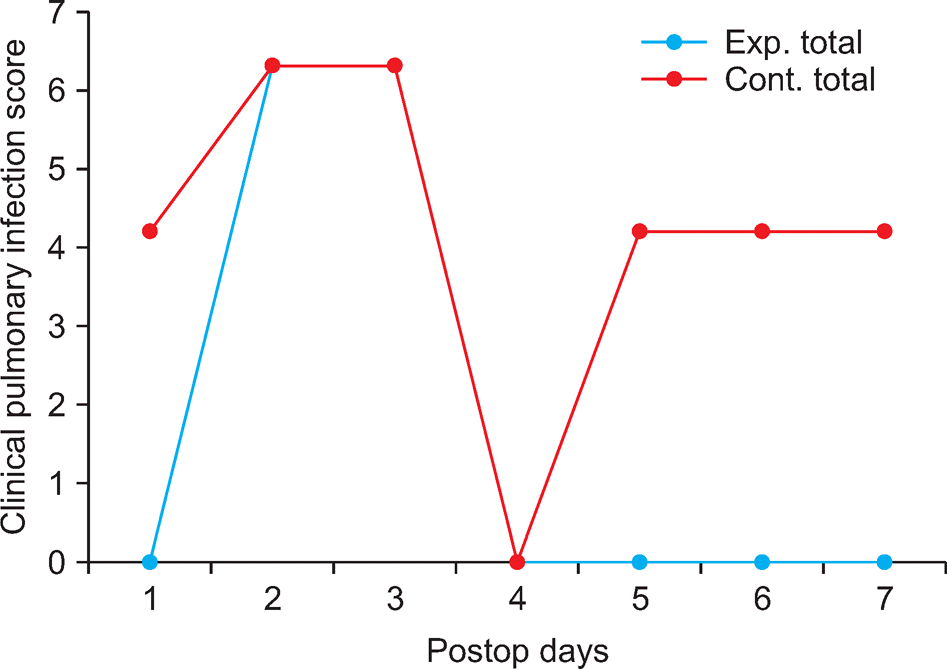
The compliance rate of breathing exercises was significantly higher in the experimental group. The experimental group presented no pulmonary infections in the later period, whereas the control group presented higher pulmonary infection rates in the same period. In addition, the life satisfaction score in the experimental group significantly increased.
Go to : 
References
1. Kim HJ, Kim MY. Effect of water drinking on the changes in blood pressure after spinal surgery in the elderly. Journal of Korean Clinical Nursing Research. 2014; 20(1):113–122.
2. National Health Insurance Service. 2015 Main surgery statistical yearbook. Statistics Bulletin. Seoul: National Health Insurance Service;2016. Nov. Report No.: 11-B550928-000034-10.
3. Kim HJ, Park SK, Jung WS, Choi YS. Prevalence and predictors of postoperative complications in patients older than 80 years. Journal of the Korean Geriatrics Society. 2015; 19(1):9–15. https://doi.org/10.4235/jkgs.2015.19.1.9.

4. Kääriäinen T, Leinonen V, Taimela S, Aalto T, Kröger H, Herno A, et al. Lumbar paraspinal and biceps brachii muscle function and movement perception in lumbar spinal stenosis. European Spine Journal. 2013; 22(4):788–793. https://doi.org/10.1007/s00586-012-2563-x.

5. Gao K, Yu PM, Su JH, He CQ, Liu LX, Zhou YB, et al. Cardiopulmonary exercise testing screening and pre-operative pulmonary rehabilitation reduce postoperative complications and improve fast-track recovery after lung cancer surgery: A study for 342 cases. Thoracic Cancer. 2015; 6(4):443–449. https://doi.org/10.1111/1759-7714.12199.

6. Shim YJ, Moon OK, Choi WS, Kim BK. Effects of the inspiratory muscle strengthening training on the respiratory functions and the quality of life in patients with cervical spinal cord injury patients. The Journal of the Korea Institute of Electronic Communication Sciences. 2013; 8(11):1785–1792. https://doi.org/10.13067/JKIECS.2013.8.11.1785.

7. Ki C, Heo M. Effects of feedback forced breathing exercise on the weight lifting and thoracic stabilization of chronic low back pain patients. Journal of Korea Entertainment Industry Association. 2014; 8(3):441–449. https://doi.org/10.21184/jkeia.2014.09.8.3.441.

8. Lee JH, Kim SY. Comparative effectiveness of Schroth therapeutic exercise versus sling therapeutic exercise in flexibility, balance, spine angle and chest expansion in patient with Scoliosis. Journal of the Korean Society of Physical Medicine. 2014; 9(1):11–23. https://doi.org/10.13066/kspm.2014.9.1.11.

9. Branson RD. The scientific basis for postoperative respiratory care. Respiratory Care. 2013; 58(11):1974–1984. https://doi.org/10.4187/respcare.02832.

10. Kim KS, Byun MK, Lee WH, Cynn HS, Kwon OY, Yi CH. Effects of breathing maneuver and sitting posture on muscle activity in inspiratory accessory muscles in patients with chronic obstructive pulmonary disease. Multidisciplinary Respiratory Medicine. 2012; 7:9. https://doi.org/10.1186/2049-6958-7-9.

11. Jin MH. A study about influence that have an effect of abdominal breathing on life satisfaction in elderly with dementia [dissertation]. Seoul: Dongkook University;2013. p. 1–155.
12. Jeong H. Effects of the respiration exercise program through the pan-flute on the physiological and psychological status of the elderly. Journal of Korean Academic Society of Adult Nursing. 2008; 20(4):588–599.
13. Ellis RJ, Thayer JF. Music and autonomic nervous system (dys) function. Music Perception: An Interdisciplinary Journal. 2010; 27(4):317–326. https://doi.org/10.1525/mp.2010.27.4.317.
14. Wang JZ, Li L, Pan LL, Chen JH. Hypnosis and music interventions (HMIs) inactivate HIF-1: A potential curative efficacy for cancers and hypertension. Medical Hypotheses. 2015; 85(5):551–557. https://doi.org/10.1016/j.mehy.2015.07.008.

15. Bradt J, Dileo C, Magill L, Teague A. Music interventions for improving psychological and physical outcomes in cancer patients. Cochrane Database of Systematic Reviews. 2016; (8). CD006911. https://doi.org/10.1002/14651858.CD006911.pub3.

16. Chen SL, Lin HC, Jane SW. Perceptions of group music therapy among elderly nursing home residents in Taiwan. Complementary Therapies in Medicine. 2009; 17(4):190–195. https://doi.org/10.1016/j.ctim.2009.03.002.

17. Kim E, Cho B. An experimental study of deep breathing exercise using phonation on effect of pulmonary ventilatory function, dyspnea, and duration of chest tube insertion in patients with pneumothorax. Chonnam Journal of Nursing Science. 2001; 6(1):17–37.
18. Min YM. The effect of regular practice for deep breathing on function of postoperative pulmonary ventilation in geriatric patients [master’s thesis]. Suwon: Ajou University;2007. p. 1–42.
19. Fartoukh M, Maitre B, Honoré S, Cerf C, Zahar JR, Brun-Buisson C. Diagnosing pneumonia during mechanical ventilation: The clinical pulmonary infection score revisited. American Journal of Respiratory and Critical Care Medicine. 2003; 168(2):173–179. https://doi.org/10.1164/rccm.200212-1449OC.
20. Shan J, Chen HL, Zhu JH. Diagnostic accuracy of clinical pulmonary infection score for ventilator-associated pneumonia: A meta-analysis. Respiratory Care. 2011; 56(8):1087–1094. https://doi.org/10.4187/respcare.01097.

21. Choi SJ. A study on the development of measuring scale of the concept of life satisfaction. Hangukmunhwayeonguwon Non-chong. 1986; 49:233–256.
22. Ji L, Bai JJ, Sun J, Ming Y, Chen LR. Effect of combining music media therapy with lower extremity exercise on elderly patients with diabetes mellitus. International Journal of Nursing Sciences. 2015; 2(3):243–247. https://doi.org/10.1016/j.ijnss.2015.07.008.

23. Kawagoshi A, Kiyokawa N, Sugawara K, Takahashi H, Saka-ta S, Satake M, et al. Effects of low-intensity exercise and home-based pulmonary rehabilitation with pedometer feedback on physical activity in elderly patients with chronic obstructive pulmonary disease. Respiratory Medicine. 2015; 109(3):364–371. https://doi.org/10.1016/j.rmed.2015.01.008.

24. Bhatt NR, Sheridan G, Connolly M, Kelly S, Gillis A, Conlon KC, et al. Postoperative exercise training is associated with reduced respiratory infection rates and early discharge: A case-control study. The Surgeon. 2017; 15(3):139–146. https://doi.org/10.1016/j.surge.2015.07.003.

25. Pettersson H, Faager G, Westerdahl E. Improved oxygenation during standing performance of deep breathing exercises with positive expiratory pressure after cardiac surgery: A randomized controlled trial. Journal of Rehabilitation Medicine. 2015; 47(8):748–752. https://doi.org/10.2340/16501977-1992.

26. Moon D, Kim KH, Lee S. Effects of deep breathing with incentive spirometer on pulmonary function and O2 saturation by time process in patients with rib fracture. The Journal of the Korea Contents Association. 2015; 15(3):174–183. https://doi.org/10.5392/JKCA.2015.15.03.174.

27. de Manincor M, Bensoussan A, Smith C, Fahey P, Bourchier S. Establishing key components of yoga interventions for reducing depression and anxiety, and improving well-being: A Delphi method study. BMC Complementary and Alternative Medicine. 2015; 15:85. https://doi.org/10.1186/s12906-015-0614-7.

28. Baek KH, Lee JY, Kim MY, Kim HJ, Yoon KR, Kang SJ. The effects of holistic breathing using biofeedback on Hemodialysis patients’ fatigue, depression, and sleep disorders. Journal of Korean Clinical Nursing Research. 2015; 21(1):21–30.
Go to : 
Table 1.
Homogeneity Test for General Characteristics and Outcome Variable between the Two Groups (N=48)
| Characteristics | Exp. (n=24) N (%)/(M±SD) | Cont. (n=24) N (%)/(M±SD) | Z/t | p | |
|---|---|---|---|---|---|
| Gender† | Male | 11 (45.8) | 5 (20.8) | 3.37 | .066 |
| Female | 13 (54.2) | 19 (79.2) | |||
| Occupation† | Employed | 20 (83.4) | 23 (95.8) | 6.37 | .272 |
| Unemployed | 4 (16.6) | 1 (4.2) | |||
| Education | Less than Elementary school | 12 (50.0) | 9 (37.6) | 5.03 | .412 |
| Middle school | 6 (25.0) | 5 (20.8) | |||
| More than high school | 6 (25.0) | 10 (41.6) | |||
| Religion† | Catholic | 6 (25.0) | 4 (16.6) | 3.35 | .340 |
| Christianity | 4 (16.6) | 9 (37.6) | |||
| Buddhism | 3 (12.4) | 4 (16.6) | |||
| None | 11 (46.0) | 7 (29.2) | |||
| Age†† | 70.04±3.96 | 71.13±5.85 | -0.75 | .456 | |
| Past history of illness | Present | 21 (87.6) | 19 (79.2) | 0.60 | .439 |
| None | 3 (12.4) | 5 (20.8) | |||
| BMI† kg/m2 | 25.48±4.60 | 24.54±3.16 | -0.83 | .413 | |
| Preoperative life satisfaction†† | 22.46±5.36 | 19.71±5.52 | -1.75 | .087 | |
Table 2.
Effects of Panflute Training on Compliance Rate and Life Satisfaction (N=48)
Table 3.
Effects of Panflute Training on Clinical Pulmonary Infection Rate (%) (N=48)




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download