Journal List > J Korean Med Sci > v.32(11) > 1108348
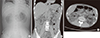
A 46-year-old man with poorly controlled type 2 diabetes mellitus and hepatocellular carcinoma with hepatitis B virus infection presented with general weakness and oliguria of 3-day duration. Serum creatinine was 6.6 mg/dL, blood urea nitrogen 112 mg/dL, leukocytes 37,600/μL, platelets 5,000/μL, and glycated hemoglobin 11.8%. He developed hypotension and metabolic acidosis. Continuous renal replacement therapy and inotropics were immediately initiated. Plain abdomen (Fig. 1A), and computer tomography (Fig. 1B and 1C, arrows) without contrast revealed extensive intraparenchymal and perinephric air collections in both enlarged kidneys that looked like wood charcoal, as well as air tracking in both proximal ureters. He was diagnosed with bilateral emphysematous pyelonephritis (EPN) and received intravenous meropenem, empirically. However, bilateral percutaneous drainage could not be performed due to hemodynamic instability. Escherichia coli was isolated in blood and urine cultures. He died of septic shock 3 days after admission.
EPN is a rare necrotizing infection of kidney predominantly seen in patients with diabetes. Although the left kidney is more frequently involved than the right, bilateral EPN is also reported to occur in up to 10% of patients. Although early nephrectomy has been considered the treatment of choice in EPN, bilateral nephrectomy is associated with high mortality rate and would necessitate lifelong renal replacement therapy in patients with bilateral EPN (1). Successful management with antibiotics and percutaneous drainage have been reported in bilateral EPN patients. Nevertheless, the mortality has been reported at up to 50% for bilateral EPN (2).
1. Kumar S, Ramachandran R, Mete U, Mittal T, Dutta P, Kumar V, Rathi M, Jha V, Gupta KL, Sakhuja V, et al. Acute pyelonephritis in diabetes mellitus: Single center experience. Indian J Nephrol. 2014; 24:367–371.
2. Yao J, Gutierrez OM, Reiser J. Emphysematous pyelonephritis. Kidney Int. 2007; 71:462–465.
- TOOLS
- ORCID iDs
-
Chang Seong Kim

https://orcid.org/0000-0001-8753-7641Seong Kwon Ma

https://orcid.org/0000-0002-5758-8189Soo Wan Kim

https://orcid.org/0000-0002-3540-9004 - Similar articles




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download