Abstract
After operation for fracture in the phalangeal bones, rehabilitation is initiated in order to minimize joint stiffness if in the case, complete bony union is confirmed by hand surgeons. The described case demonstrates that bony mallet deformity can occur during physical therapy following by surgical pinning of a proximal phalangeal fracture. This mallet finger deformity occurred due to vigorous rehabilitation for correction of postoperative joint stiffness. So, when hand surgeons treat patients with proximal phalangeal fracture, it is important to minimize joint space involvement and close follow-ups accompanying imaging studies during rehabilitation period.
Go to : 
References
1. Strauch RJ, editor. Extensor tendon injury: specific extensor tendon injuries. Green DP, Wolfe SW, editors. Green’s operative hand surgery. 6th ed.Philadelphia: Elsevier/Churchill Livingstone;2011. p. 168–9.
5. Ishiguro T, Itoh Y, Yabe Y, Hashizume N. Extension block with Kirschner wire for fracture dislocation of the distal interphalangeal joint. Tech Hand Up Extrem Surg. 1997; 1:95–102.

6. Backdahl M. Ruptures of the extensor aponeurosis at the distal digital joints. Acta Chir Scand. 1956; 111:151–7.
7. Patel MR, Lipson LB, Desai SS. Conservative treatment of mallet thumb. J Hand Surg Am. 1986; 11:45–7.

Go to : 
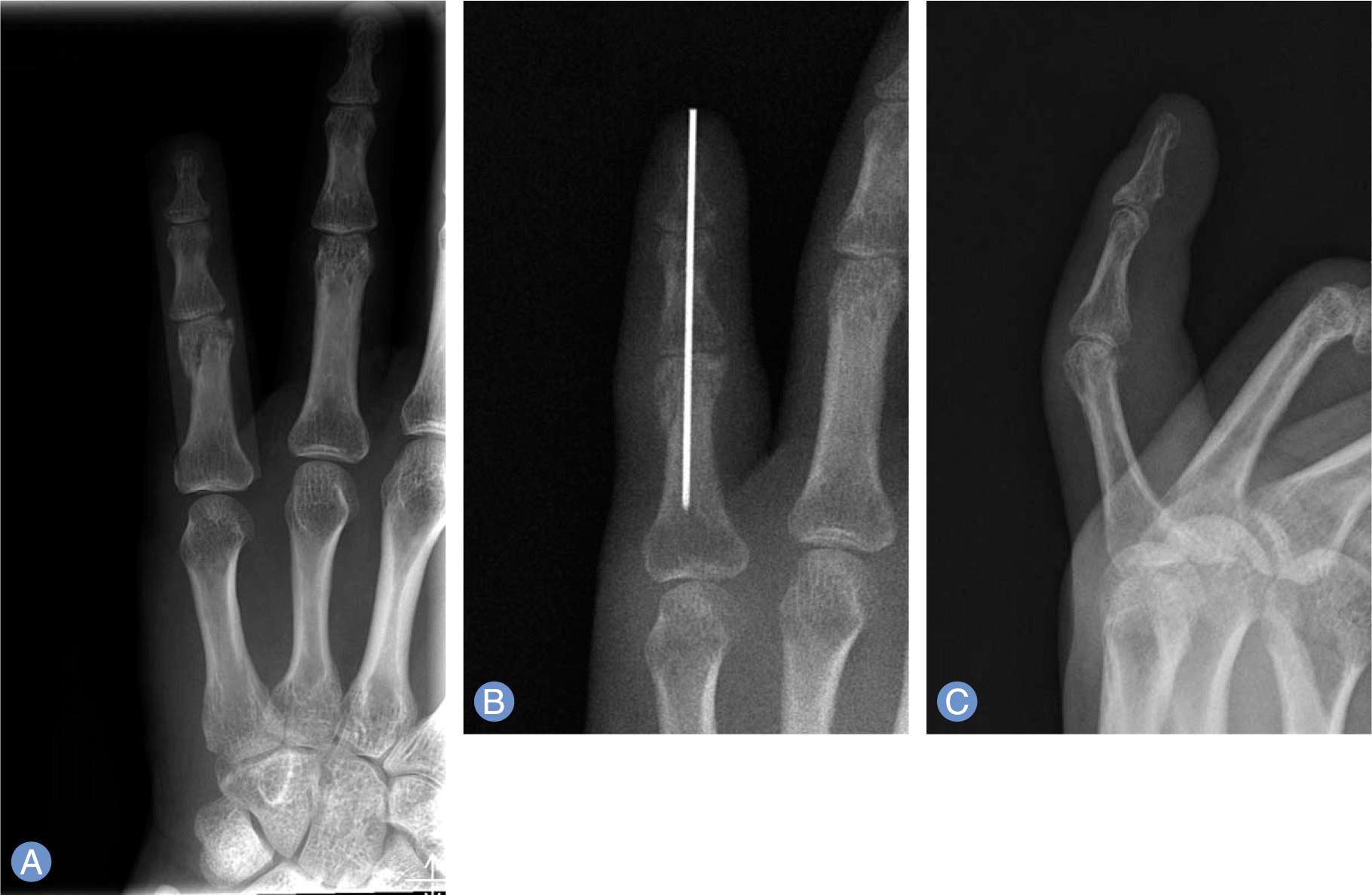 | Fig. 1.Primary little finger fracture. (A) Radiographs depicted a comminuted fracture of the head of the proximal phalanx. (B) Postoperative radiograph demonstrating anatomic reduction by Kirschner wire fixation at 7 days after injury. (C) Lateral radiograph taken two months after closed reduction demonstrating complete bony union. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download