Abstract
Chronic lateral ankle instability occurs in 10% to 20% of individuals after acute ankle sprain. The management of chronic lateral ankle instability is traditionally conservative treatment in the acute phase. On the other hand, surgical intervention is considered if conservative treatment fails and the symptoms are ongoing. This review focuses on the surgical approaches to treatment of chronic lateral ankle instability, including Broström surgical techniques, with a review of the traditional procedure and newer techniques.
Go to : 
References
1. Elmslie R. Recurrent subluxation of the ankle-joint. Ann Surg. 1934; 100:364–7.
2. Broström L. Sprained ankles, anatomic lesions in recent sprains. Acta Chir Scand. 1964; 128:483–95.
3. Broström L. Sprained ankles. VI. Surgical treatment of chronic ligament ruptures. Acta Chir Scand. 1966; 132:551–65.
4. Gould N, Seligson D, Gassman J. Early and late repair of lateral ligament of the ankle. Foot Ankle. 1980; 1:84–9.

5. Karlsson J, Bergsten T, Lansinger O, Peterson L. Reconstruction of the lateral ligaments of the ankle for chronic lateral instability. J Bone Joint Surg Am. 1988; 70:581–8.

6. Ahlgren O, Larsson S. Reconstruction for lateral ligament injuries of the ankle. J Bone Joint Surg Br. 1989; 71:300–3.

7. Anderson ME. Reconstruction of the lateral ligaments of the ankle using the plantaris tendon. J Bone Joint Surg Am. 1985; 67:930–4.

8. Baker J, Ouzounian T. Complex ankle instability. Foot Ankle Clin. 2000; 5:887–96.
9. Brodsky AR, O'Malley MJ, Bohne WH, Deland JA, Kennedy JG. An analysis of outcome measures following the Broström-Gould procedure for chronic lateral ankle instability. Foot Ankle Int. 2005; 26:816–9.

10. Hamilton WG, Thompson FM, Snow SW. The modified Brostrom procedure for lateral ankle instability. Foot Ankle. 1993; 14:1–7.

11. Schmidt R, Benesch S, Friemert B, Herbst A, Claes L, Gerngross H. Anatomical repair of lateral ligaments in patients with chronic ankle instability. Knee Surg Sports Traumatol Arthrosc. 2005; 13:231–7.

13. Coughlin MJ, Saltzman CL, Mann RA. Mann's surgery of the foot and ankle e-book: expert consult–online. St. Louis: Mobsy;2013.
14. Ferkel RD, Chams RN. Chronic lateral instability: arthroscopic findings and longterm results. Foot Ankle Int. 2007; 28:24–31.

15. Kibler WB. Arthroscopic findings in ankle ligament reconstruction. Clin Sports Med. 1996; 15:799–804.
16. Taga I, Shino K, Inoue M, Nakata K, Maeda A. Articular cartilage lesions in ankles with lateral ligament injury: an arthroscopic study. Am J Sports Med. 1993; 21:120–7.
17. Ferkel RD, Small HN, Gittins JE. Complications in foot and ankle arthroscopy. Clin Orthop Relat Res. 2001; 391:89–104.

18. Imade S, Takao M, Miyamoto W, Nishi H, Uchio Y. Leg anterior compartment syndrome following ankle arthroscopy after Maisonneuve fracture. Arthroscopy. 2009; 25:215–8.

19. Canale ST, Beaty JH. Campbell's operative orthopaedics (e-book). Philadelphia: Elsevier Health Sciences;2012.
20. Maffulli N, Del Buono A, Maffulli GD, Oliva F, Testa V, Capasso G, et al. Isolated anterior talofibular ligament broström repair for chronic lateral ankle instability: 9-year follow-up. Am J Sports Med. 2013; 41:858–64.
21. Wainright WB, Spritzer CE, Lee JY, Easley ME, DeOrio JK, Nunley JA, et al. The effect of modified Broström-Gould repair for lateral ankle instability on in vivo tibiotalar kinematics. Am J Sports Med. 2012; 40:2099–104.

24. Chung HJ. Anatomical repair for chronic lateral ankle instability. J Korean Orthop Assoc. 2014; 49:13–21.

25. Jeong BO, Kim MS, Song WJ, SooHoo NF. Feasibility and outcome of inferior extensor retinaculum reinforcement in modified Broström procedures. Foot Ankle Int. 2014; 35:1137–42.

26. Behrens SB, Drakos M, Lee BJ, Paller D, Hoffman E, Koruprolu S, et al. Biomechanical analysis of Brostrom versus Brostrom-gould lateral ankle instability repairs. Foot Ankle Int. 2013; 34:587–92.

27. Trichine F, Friha T, Boukabou A, Belaid L, Bouzidi T, Bouzitouna M. Surgical treatment of chronic lateral ankle instability using an inferior extensor retinaculum flap: a retrospective study. J Foot Ankle Surg. 2018; 57:226–31.

28. Paden M, Stone P, McGarry J. Modified Brostrom lateral ankle stabilization utilizing an implantable anchoring system. J Foot Ankle Surg. 1994; 33:617–22.
29. Messer TM, Cummins CA, Ahn J, Kelikian AS. Outcome of the modified Broström procedure for chronic lateral ankle instability using suture anchors. Foot Ankle Int. 2000; 21:996–1003.

30. Yeo ED, Lee KT, Sung IH, Lee SG, Lee YK. Comparison of all-inside arthroscopic and open techniques for the modified Broström procedure for ankle instability. Foot Ankle Int. 2016; 37:1037–45.

31. Yasui Y, Murawski CD, Wollstein A, Takao M, Kennedy JG. Operative treatment of lateral ankle instability. JBJS Rev. 2016. 4. doi:. DOI: 10.2106/JBJS.RVW.15.00074.

32. Guelfi M, Zamperetti M, Pantalone A, Usuelli FG, Salini V, Oliva XM. Open and arthroscopic lateral ligament repair for treatment of chronic ankle instability: a systematic review. Foot Ankle Surg. 2018; 24:11–8.

33. Lee KT, Kim ES, Kim YH, Ryu JS, Lee YK. All-inside arthroscopic modified Broström operation for chronic ankle instability: a biomechanical study. Knee Surg Sports Traumatol Arthrosc. 2016; 24:1096–100.

34. Baumhauer JF, O'brien T. Surgical considerations in the treatment of ankle instability. J Athl Train. 2002; 37:458–62.
35. Buerer Y, Winkler M, Burn A, Chopra S, Crevoisier X. Evaluation of a modified Broström–Gould procedure for treatment of chronic lateral ankle instability: a retrospective study with critical analysis of outcome scoring. Foot Ankle Surg. 2013; 19:36–41.

36. Cho BK, Kim YM, Kim DS, Choi ES, Shon HC, Park KJ. Outcomes of the modified Brostrom procedure using suture anchors for chronic lateral ankle instability—a prospective, randomized comparison between single and double suture anchors. J Foot Ankle Surg. 2013; 52:9–15.

37. Bell SJ, Mologne TS, Sitler DF, Cox JS. Twenty-six-year results after Broström procedure for chronic lateral ankle instability. Am J Sports Med. 2006; 34:975–8.

38. Choi WJ, Lee JW, Han SH, Kim BS, Lee SK. Chronic lateral ankle instability: the effect of intraarticular lesions on clinical outcome. Am J Sports Med. 2008; 36:2167–72.
39. Hua Y, Chen S, Li Y, Chen J, Li H. Combination of modified Broström procedure with ankle arthroscopy for chronic ankle instability accompanied by intraarticular symptoms. Arthroscopy. 2010; 26:524–8.

40. Lee J, Hamilton G, Ford L. Associated intraarticular ankle pathologies in patients with chronic lateral ankle instability: arthroscopic findings at the time of lateral ankle reconstruction. Foot Ankle Spec. 2011; 4:284–9.

41. Li X, Killie H, Guerrero P, Busconi BD. Anatomical reconstruction for chronic lateral ankle instability in the high-demand athlete: functional outcomes after the modified Broström repair using suture anchors. Am J Sports Med. 2009; 37:488–94.
42. Nery C, Raduan F, Del Buono A, Asaumi ID, Cohen M, Maffulli N. Arthroscopic-assisted Broström-Gould for chronic ankle instability: a longterm follow-up. Am J Sports Med. 2011; 39:2381–8.
43. Hennrikus WL, Mapes RC, Lyons PM, Lapoint JM. Outcomes of the Chrisman-Snook and modified-Broström procedures for chronic lateral ankle instability: a prospective, randomized comparison. Am J Sports Med. 1996; 24:400–4.
44. Viens NA, Wijdicks CA, Campbell KJ, LaPrade RF, Clanton TO. Anterior talofibular ligament ruptures, part 1: biomechanical comparison of augmented Broström repair techniques with the intact anterior talofibular ligament. Am J Sports Med. 2014; 42:405–11.
45. DiGiovanni CW, Brodsky A. Current concepts: lateral ankle instability. Foot Ankle Int. 2006; 27:854–66.

Go to : 
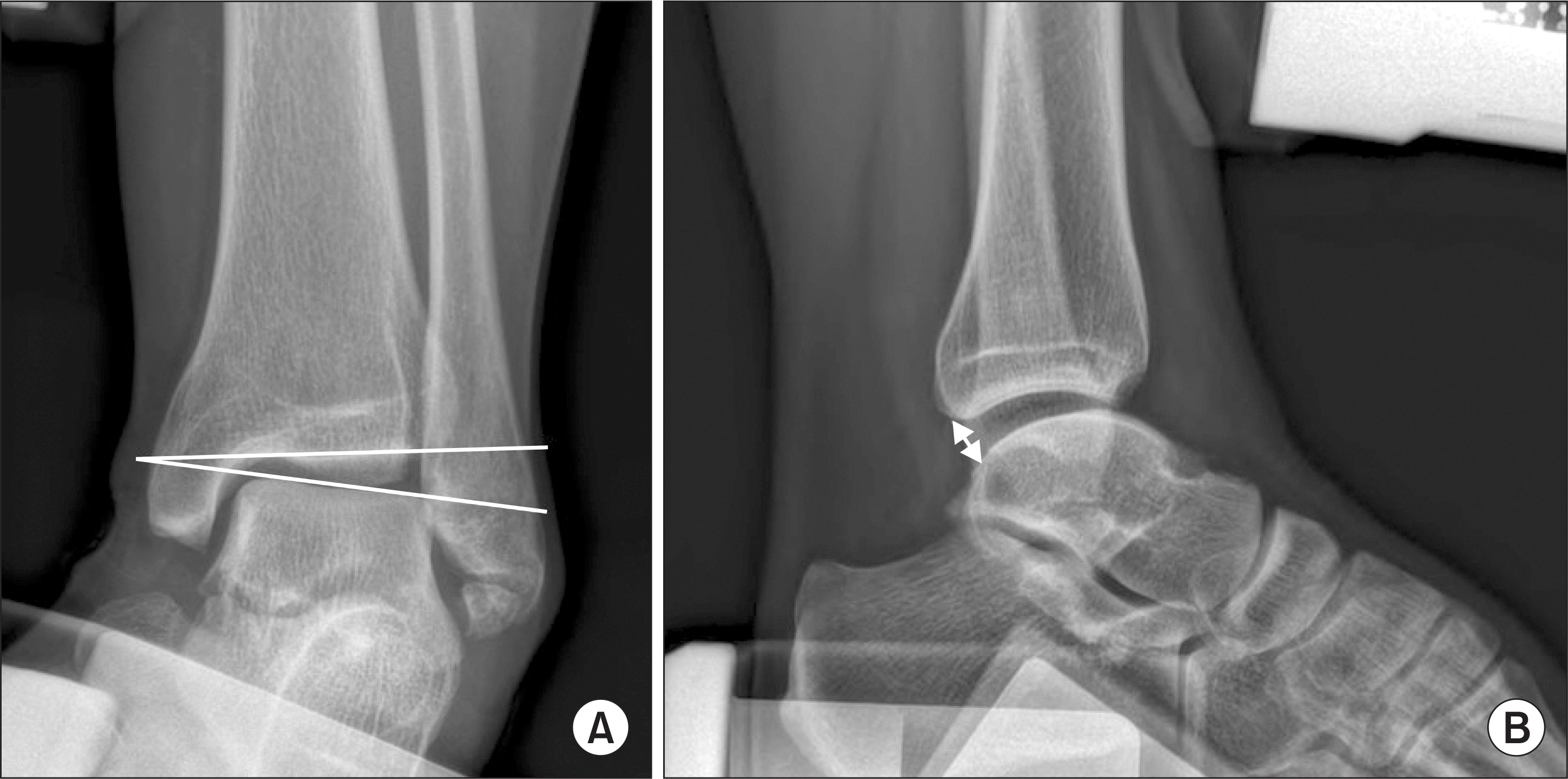 | Figure 1.(A) Varus stress test and anterior draw test; It can be seen that there is a widening of the joint space on the basis of the varus stress test. (B) In the anterior draw test, the talus was displaced anteriorly. |
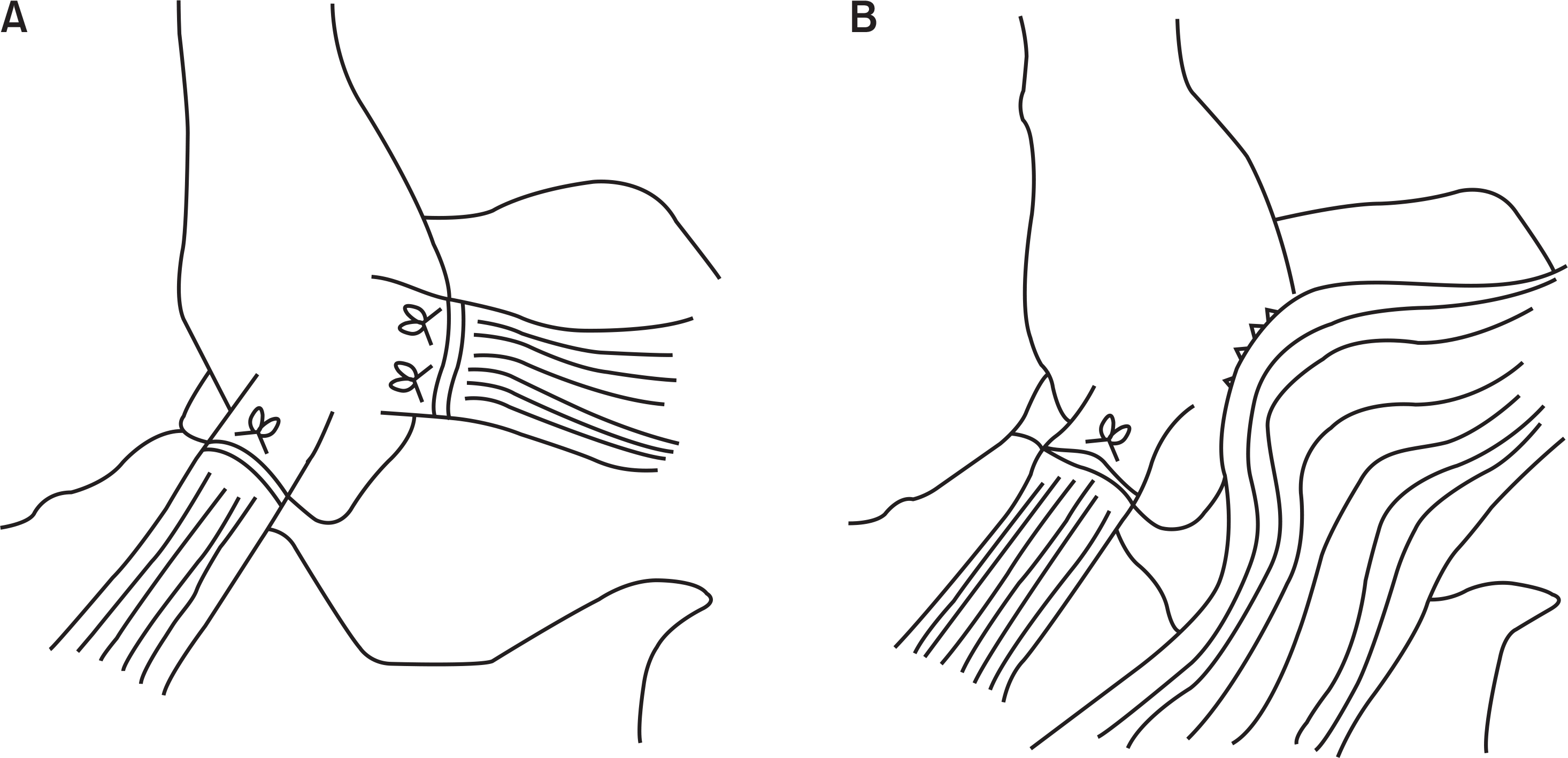 | Figure 2.(A) Broström procedure (1966). (B) Gould modification procedure (1980). Revised from the article of Chung (J Korean Orthop Assoc. 2014;49:13–21)24) in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 3.0) license. |
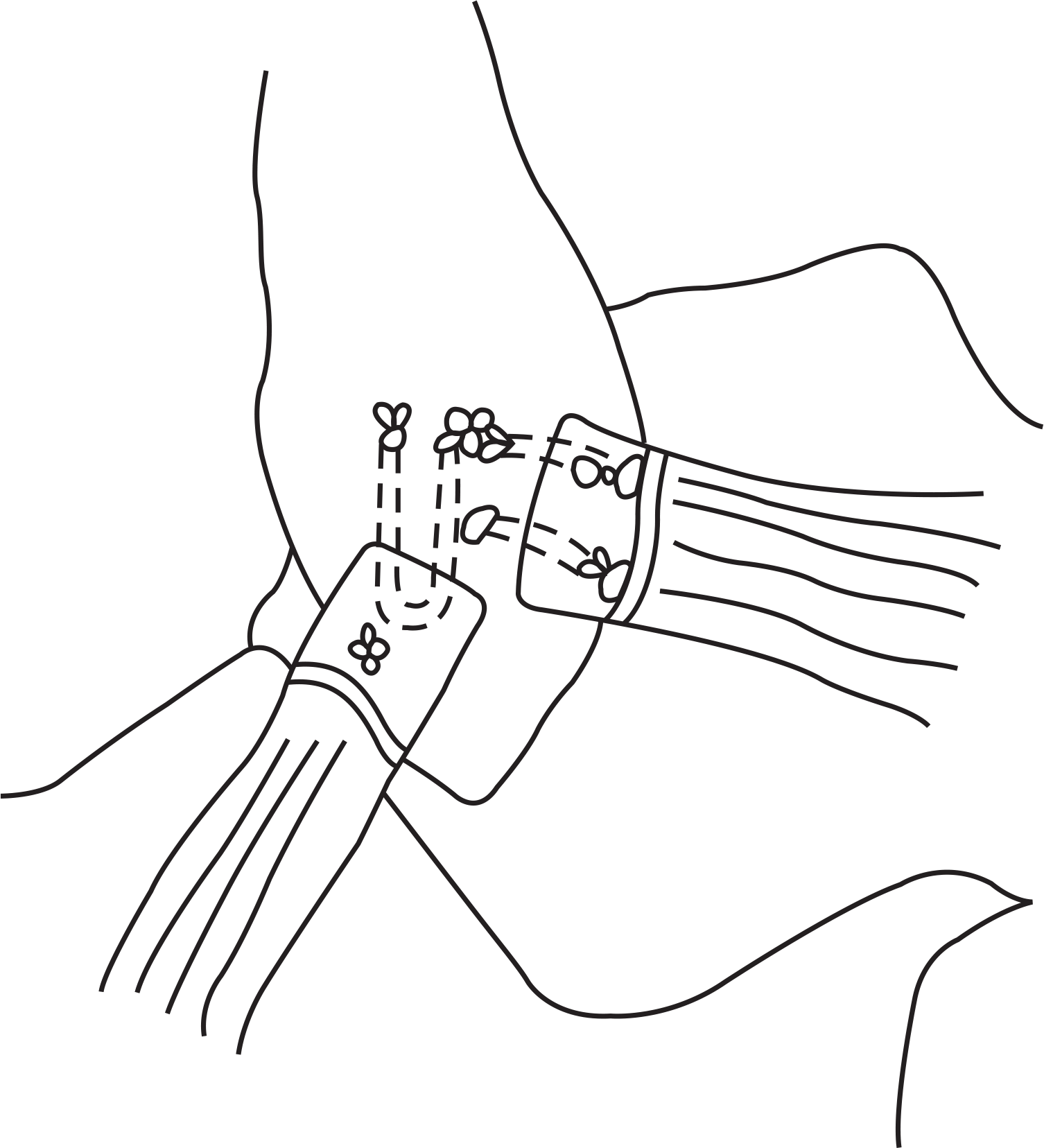 | Figure 3.Karlsson procedure (1988). Revised from the article of Chung (J Korean Orthop Assoc. 2014;49:13–21)24) in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 3.0) license. |
 | Figure 4.(A) Complete tear of anterolateral capsule and anterior talofibular and calcaneofibular ligament. (B, C) Repair of anterior talofibular ligament with suture anchor. (D) Completion of surgical repair. |
Table 1.
Results of Broström and Broström-Gould Procedures




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download