Abstract
Purpose
To identify the effects of delivery-nursing simulation education using team-based learning on the delivery nursing knowledge, self-efficacy, and clinical competence of nursing students.
Methods
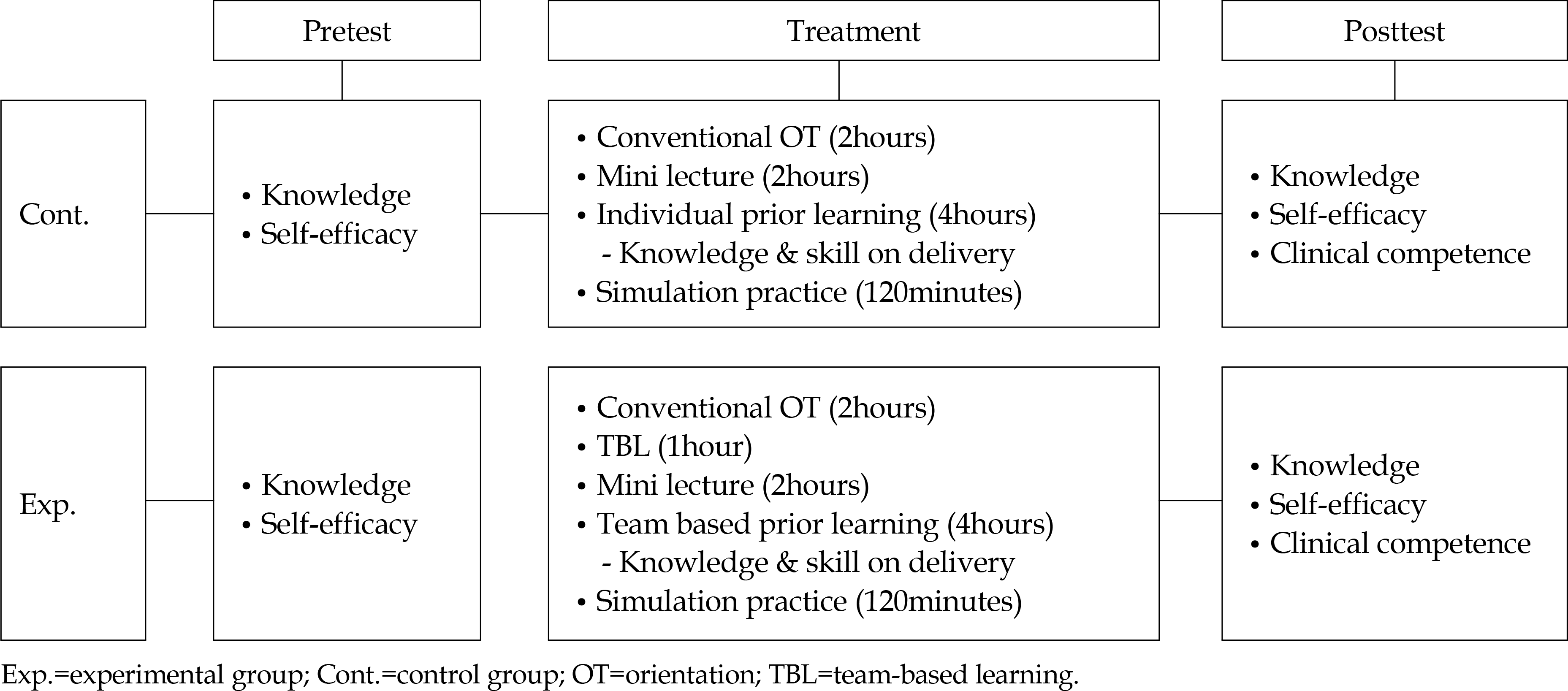
The study used a nonequivalent, control group, quasi-experimental design. The team-based learning was applied to the experimental group, while the individual learning was applied to the control group. Data were collected from October 12 to December 7, 2016, and analyzed using the SPSS/WIN 22.0 program.
Results
Comparison between the experimental and control group showed no significant difference in delivery-nursing knowledge (t=-0.33, p=.741) or self-efficacy (t=-0.65, p=.515). However, a significant difference(t=-2.09, p=.048) in the nursing-skills aspect of clinical competence was found between the experimental and control groups after the practical simulation education.
References
1. Choi DW. Clinical competence according to experiences on the essential of fundamental nursing skills in nursing students. Journal of Korean Academic Society of Nursing Education. 2014; 20(2):184–191. https://doi.org/10.5977/jkasne.2014.20.2.184.

2. Kim EH, Jang KS. Effect of a simulation-based education on cardiopulmonary emergency care knowledge, clinical performance ability and problem solving process in new nurses. Journal of Korean Academy of Nursing. 2011; 41(2):245–255. https://doi.org/10.4040/jkan.2011.41.2.245.

3. Park HJ, Lee SH. Development and effects of integrated simulation program (maternal-child) on nursing students. Child Health Nursing Research. 2015; 21(4):293–301. https://doi.org/10.4094/chnr.2015.21.4.293.
4. Lee WS, Kim MO. Effects and adequacy of highfidelity simulation-based training for obstetrical nursing. Journal of Korean Academy of Nursing. 2011; 41(4):433–443. https://doi.org/10.5977/jkasne.2014.20.2.203.

5. Yang SH, Hong SH. Development and effects of simulation practice program about family centered delivery care. Korean Journal of Women Health Nursing. 2017; 23(1):52–61. https://doi.org/10.4069/kjwhn.2017.23.1.52.

6. Chung KS. RN of this year, ‘Man licence' 2,344 people [Internet]. Seoul: korean nurses association;2018. [cited 2018 May 04]. Available from. http://www.nursenews.co.kr/main/ArticleDetailView.asp?sSection=61&idx=22522&intPage=1.
7. Kim DH, Lee YJ, Hwang MS, Park JH, Kim HS, Cha HG. Effects of a simulation-based integrated clinical practice program (SICPP) on the problem solving process, clinical competence and critical thinking in a nursing student. Korean Academic Society of Nursing Education. 2012; 8(3):499–509. https://doi.org/10.5977/jkasne.2012.18.3.499.
8. Seomun GA. Revision standards by area (2). Yang S, editor. editors.Three-cycle nursing education certification evaluation presentation. Seoul: Korean Accreditation Board of Nursing;2016. p. 86. p.
9. Cooper S, Cant R, Porter J, Bogossian F, McKenna L, Brady S, et al. Simulation based learning in midwifery education: A systematic review. Women and Birth. 2011; 25(2):64–78. https://doi.org/10.1016/j.wombi.2011.03.004.

10. Lee JO. The effects of simulation-based training, underwent before or after the clinical practice for the nursing students. Journal of the Korean Society of Maternal and Child Health. 2014; 20(2):203–211. https://doi.org/10.21896/jksmch.2014.18.1.125.

11. Kim SH. Effects of simulation-based practice using standardized patients for the care of women with postpartum hemorrhage on nursing student's clinical performance competence and critical thinking deposition. Korean Parent Child Health Journal. 2012; 15(2):71–79.
12. Shim CS, Park MK, Kim JH. Effects of simulation-based delivery education regarding to obstetric clinical practice before and after of nursing students. Journal of the Korean Society of Maternal and Child Health. 2014; 18(1):125–133. https://doi.org/10.21896/jksmch.2014.18.1.125.
13. Song YA, Son YJ. Effects of simulation-based practice by applying problem based learning on problem solving process, self-confidence in clinical performance and nursing competence. Korean Journal of Women Health Nursing. 2014; 20(4):246–254. https://doi.org/10.4069/kjwhn.2014.20.4.246.
14. Lee SK. The effect of simulation practice education on the clinical judgment, self-confidence and clinical performance ability in nursing student. International Journal of Contents. 2017; 17(17):577–587. https://doi.org/10.5392/JKCA.2017.17.11.577.
15. Kim KA. Effects of a simulation-based labor education program on skill competence, knowledge, and satisfaction for education in nursing students [dissertation]. Seoul: The Catholic University of Korea;2014. p. 55. p.
16. Lee SH, Chun YE, Kim KM, Park HJ. Effects of integrated simulation (delivery-operation-newborn) practice program for nursing students. Journal of Learner-Centered Curriculum and Instruction. 2015; 15(9):577–599.
17. Yang JJ. Effects of a simulation-based education on the knowledge and clinical competence for nursing students. Journal Korean Academic Society of Nursing Education. 2012; 18:14–23. https://doi.org/10.5977/jkasne.2012.18.1.014.
18. Kim JS, Kim YH. The effects of simulation practice education applying problem-based learning on problem solving ability, critical thinking and learning satisfaction of nursing students. Journal of the Korea Contents Association. 2016; 16(12):203–212. https://doi.org/10.5392/JKCA.2016.16.12.203.

19. Lee WS, Cho KC, Yang SH, Roh YS, Lee GY. Effects of problem-based learning combined with simulation on the basic nursing competency of nursing students. Korean Journal of Fundamental of Nursing. 2009; 16(1):64–72.
20. Kim MN, Chung HI, Kim YA. A metaanalysis of the effect of simulation-based education for delivery nursing in Korea. Journal of the Korean Society of Maternal and Child Health. 2016; 20(3):297–309. https://doi.org/10.21896/jksmch.2016.20.3.297.
21. Michaelsen LK, Parmelee DX, McMahon K, Levine RE. Team based learning for health professions education. Sterling: Stylus Publishing;2007. p. 256. p.
22. Kim HR, Choi EY, Kang HY. Simulation module development and team competency evaluation. Korean Journal of Fundamentals of Nursing. 2011; 18(3):392–400.
23. Roh YS, Ryoo EN, Choi DW, Baek SS, Kim SS. A survey of student perceptions, academic achievement, and satisfaction of team based learning in a nursing course. Journal of Korean Academic Society of Nursing Education. 2012; 18(2):239–247. https://doi.org/10.5977/jkasne.2012.18.2.239.
24. Clark MC, Nguyen HT, Bray C, Levine RE. Team-based learning in an undergraduate nursing course. Journal of Nursing Education. 2008; 47(3):111–117. https://doi.org/10.3928/01484834–20080301–02.

25. Choi KO, Park YM. The effects of team-based learning on problem solving ability, critical thinking disposition and self-directed learning in undergraduate nursing students. Journal of East-West Nursing Research. 2014; 20(2):154–159. https://doi.org/10.14370/jewnr.2014.20.2.154.

26. Jeffries PR. A framework for designing, implementing, and evaluating simulations used as teaching strategies in nursing. Nursing Education Perspectives. 2005; 26(2):96–103. https://doi.org/10.5480/1536–5026–26.2.96.
27. Levine AI, DeMaria JrS, Schwartz AD, Sim AJ. The comprehensive textbook of healthcare simulaion. 2nd ed.New York: Springer;2014. p. 697. p.
28. Marken PA, Zimmerman C, Kennedy C, Schremmer R, Smith KV. Human simulators and standardized patients to teach difficult conversations to inter professional health care teams. American Journal of Pharmaceutical Education. 2010; 74(7):120.
29. Taekman JM, Shelley K. Virtual environments in healthcare: Immersion, disruption, and flow. International Anesthesiology Clinics. 2010; 48(3):101–121. https://doi.org/10.1097/AIA.0b013e3181eace73.

30. Weaver A. Highfidelity patient simulation in nursing education. Nursing Education Perspectives. 2011; 32(1):37–40. https://doi.org/10.5480/1536–5026–32.1.37.
Table 1.
Homogeneity Test of General Characteristics and Dependent Variables (N=91)
Table 2.
Comparison of Knowledge and Self-efficacy on Delivery between Experimental and Control Group (N=91)
Table 3.
Comparison of Clinical Competency between Two Groups at Posttest (N=91)




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download