Abstract
In this study, we present the commissioning and validation results of a dedicated scanning nozzle. The dedicated scanning nozzle is installed in one of the two gantry treatment rooms at Samsung Proton Therapy Center. Following a successful completion of the acceptance test, the commissioning process including the beam data measurement for treatment planning system has been conducted. Extended measurements have been conducted as a validation of the clinical performance of the nozzle and various quality assurance protocols have been prepared.
Go to : 
REFERENCES
1. Wilson R. R.Radiology. 47:487. 1946.
2. Jermann M.Int J Particle Ther. 2:50. 2015.
3. Chung K., Han Y., Kim J., et al. Radiat Oncol J. 33:337. 2015.
4. Chung K., Kim J., Kim D.-H., Ahn S., Han Y.J. Korean Phys Soc. 67:170. 2015.
Go to : 
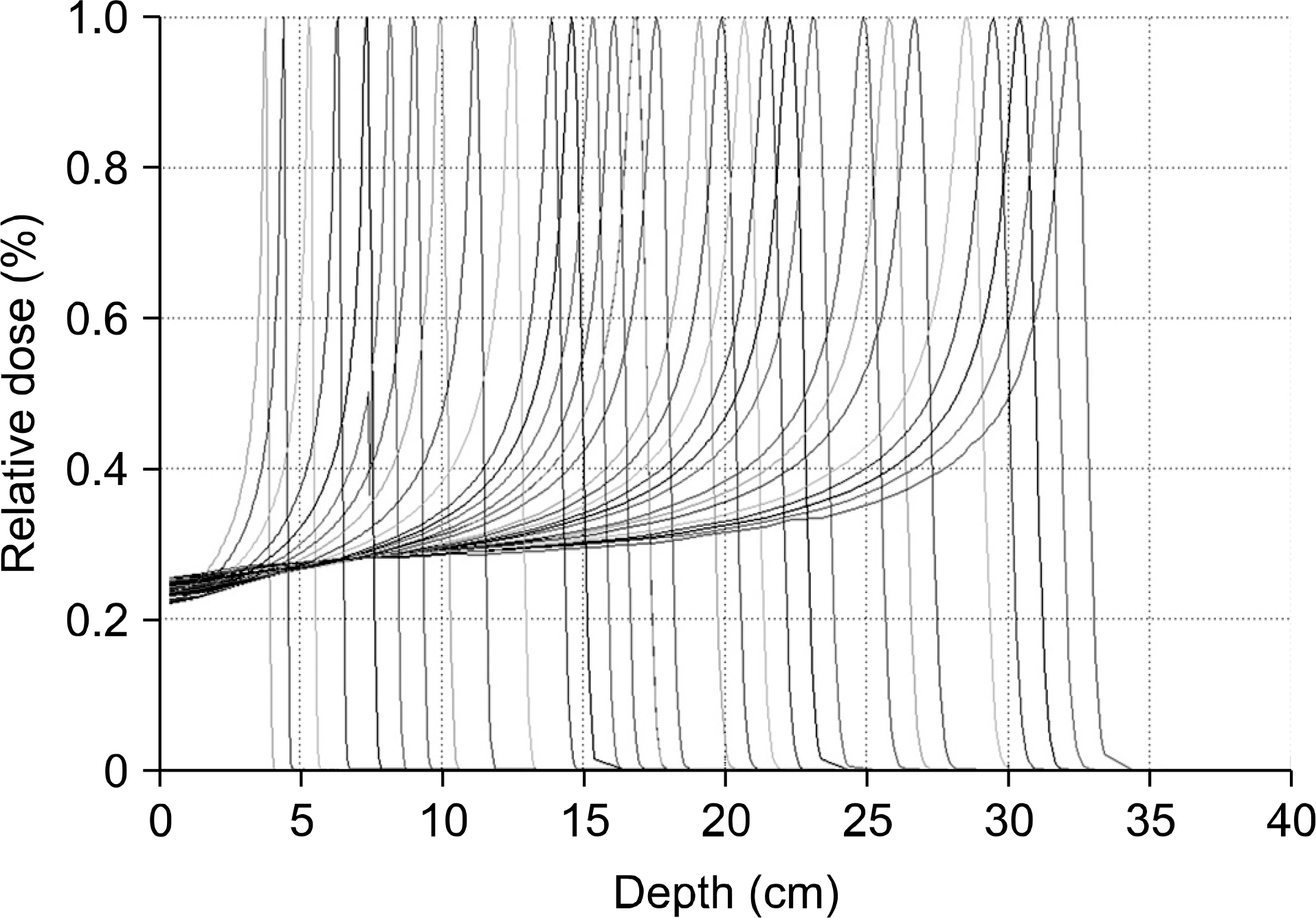 | Fig. 1.The integrated depth dose curves for the selected beam energies (normalized at peak values). |
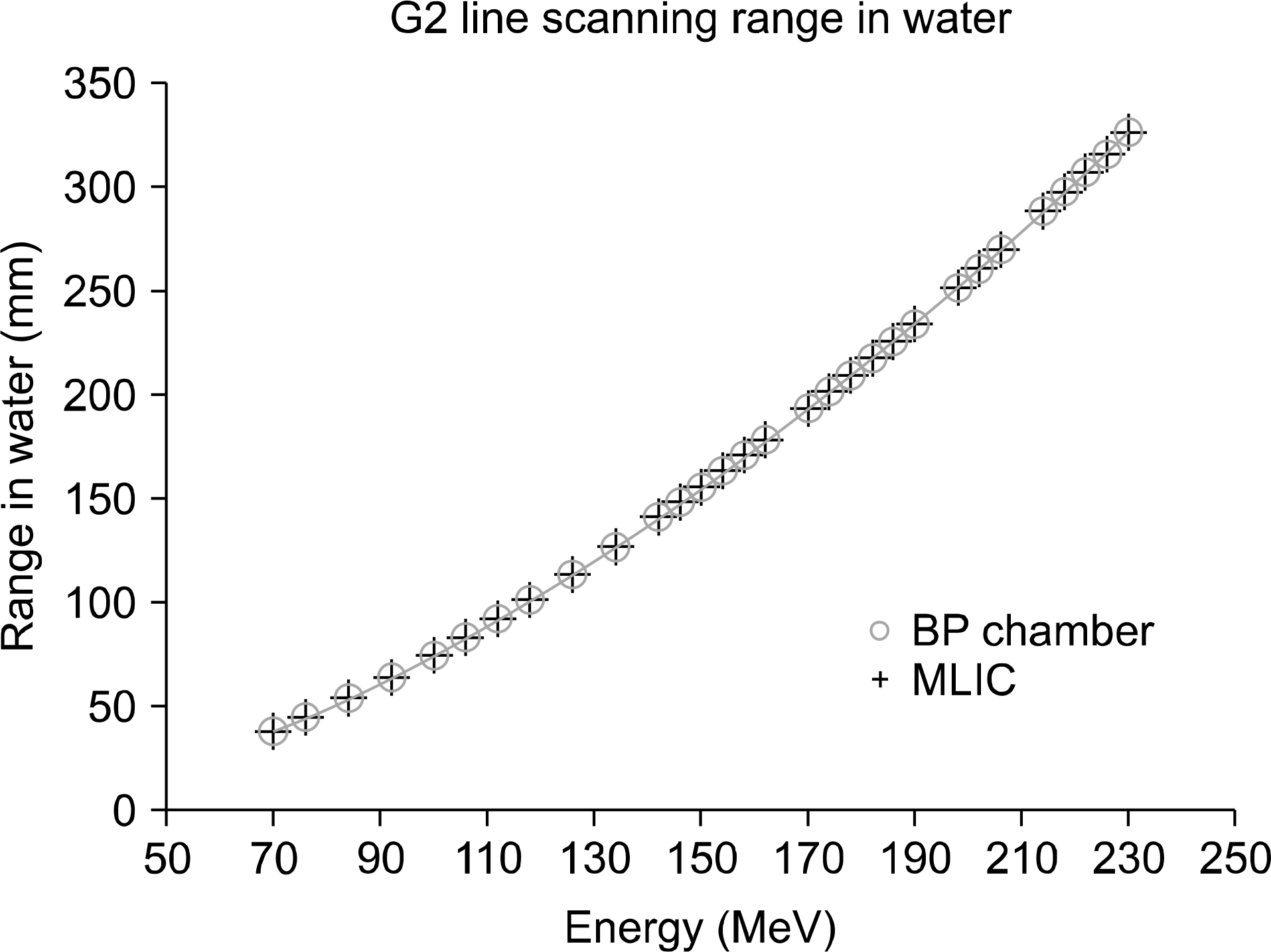 | Fig. 2.The clinical range (D90) of the dedicated scanning nozzle at Samsung PTC measured by PTW Bragg peak chamber and MLIC. |
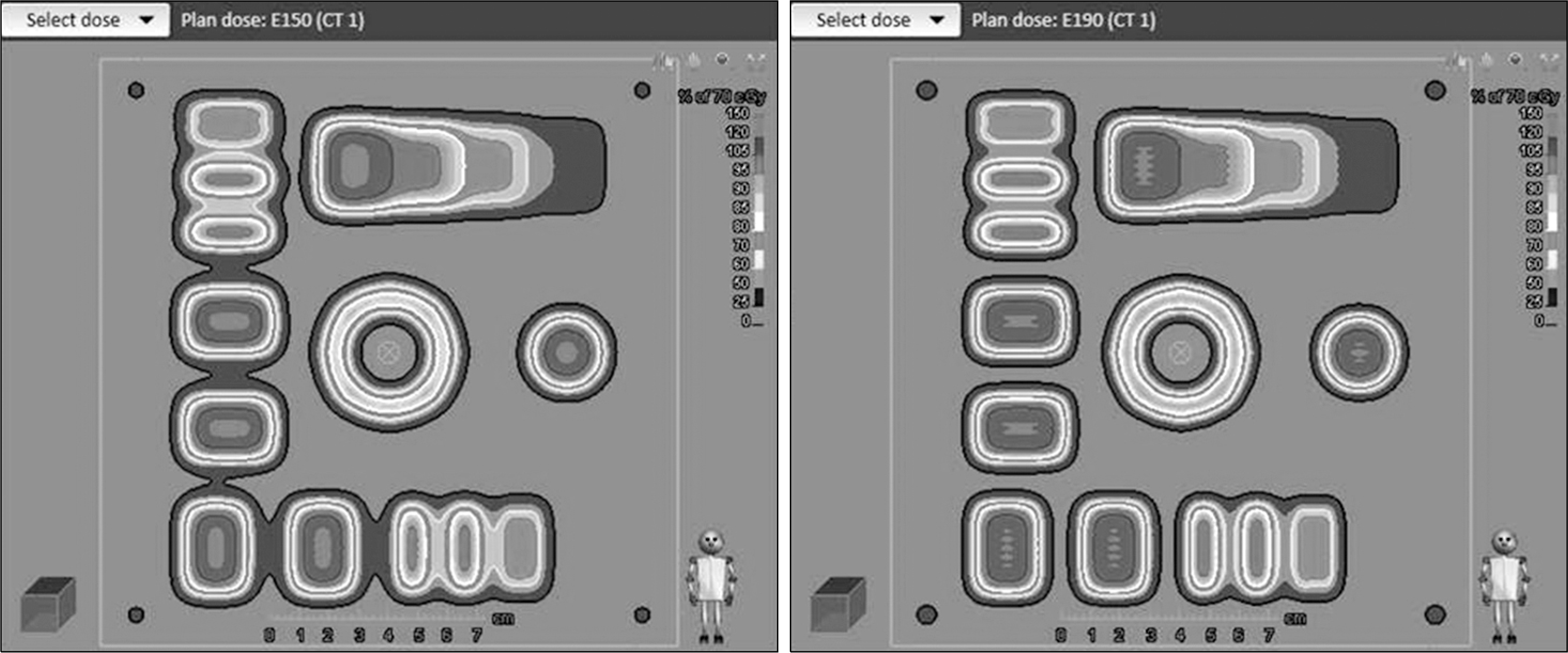 | Fig. 4.Example of mono energetic scan patterns (Left: 150 MeV, Right: 190 MeV) created for validation and daily QA. The gamma passing rates were all above 95% with 3%, 3 mm criteria for both beam energies. |
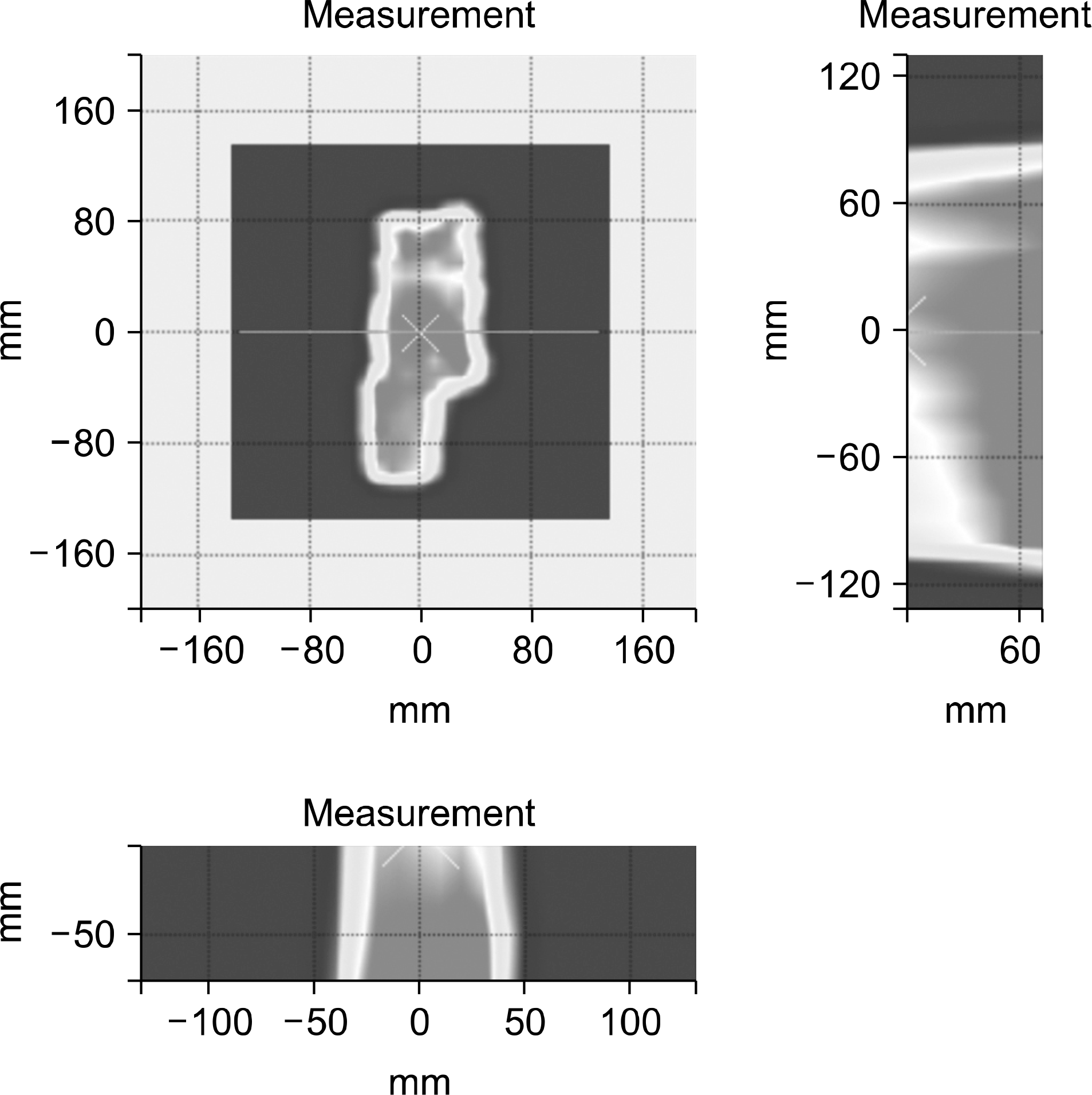 | Fig. 5.Pseudo 3D dose distribution reconstructed from multi-depth measurement of 2D dose map (With 3% and 3 mm criteria, all XY, XZ, and YZ planes have a passing rate of 100%). |
Table 1.
Selected rehearsal cases for the physical and clinical commissioning of the dedicated scanning nozzle.
| Case number | Dx. Site | ∗2D Dose QA | Note |
|---|---|---|---|
| 1 | PED | 99.0% | CSI |
| 2 | HCC | 97.8% | |
| 3 | Brain | 98.1% | |
| 4 | Lung | 98.5% | |
| 5 | PED | 99.5% | Brain |
| 6 | Recurrent rectal | 98.8% | |
| 7 | Head and neck | 99.3% | |
| 8 | Prostate | 99.5% | Definitive |
| 9 | Esophagus | 97.5% | Long Y-extent |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download