Abstract
At present, megavoltage computed tomography (MVCT) is the only method used to correct the position of tomotherapy patients. MVCT produces extra radiation, in addition to the radiation used for treatment, and repositioning also takes up much of the total treatment time. To address these issues, we suggest the use of a video image–guided setup (VIGS) system for correcting the position of tomotherapy patients. We developed an in-house program to correct the exact position of patients using two orthogonal images obtained from two video cameras installed at 90º and fastened inside the tomotherapy gantry. The system is programmed to make automatic registration possible with the use of edge detection of the user-defined region of interest (ROI). A head-and-neck patient is then simulated using a humanoid phantom. After taking the computed tomography (CT) image, tomotherapy planning is performed. To mimic a clinical treatment course, we used an immobilization device to position the phantom on the tomotherapy couch and, using MVCT, corrected its position to match the one captured when the treatment was planned. Video images of the corrected position were used as reference images for the VIGS system. First, the position was repeatedly corrected 10 times using MVCT, and based on the saved reference video image, the patient position was then corrected 10 times using the VIGS method. Thereafter, the results of the two correction methods were compared. The results demonstrated that patient positioning using a video-imaging method (41.7±11.2 seconds) significantly reduces the overall time of the MVCT method (420±6 seconds) (p<0.05). However, there was no meaningful difference in accuracy between the two methods (x=0.11 mm, y=0.27 mm, z=0.58 mm, p>0.05). Because VIGS provides a more accurate result and reduces the required time, compared with the MVCT method, it is expected to manage the overall tomotherapy treatment process more efficiently.
Go to : 
REFERENCES
1. Chavaudra J, Bridier A. Definition of volumes in external radiotherapy: ICRU reports 50 and 62. Cancer Radiother. 5(5):472–478. 2001.
2. Mackie TR, Holmes T, Swerdloff S, et al. Tomotherapy: a new concept for the delivery of dynamic conformal radiotherapy. Med Phys. 20(6):1709–1719. 1993.

3. Mackie TR, Kapatoes J, Ruchala K, et al. Image guidance for precise conformal radiotherapy. Int J Radiat Oncol Biol Phys. 56(1):89–105. 2003.

4. Milliken BD, Rubin SJ, Hamilton RJ, Johnson LS, Chen GT. Performance of a video-image-subtraction-based patient positioning system. Int J Radiat Oncol Biol Phys. 38(4):855–866. 1997.

5. Schoffel PJ, Harms W, Sroka-Perez G, Schlegel W, Karger CP. Accuracy of a commercial optical 3D surface imaging system for realignment of patients for radiotherapy of the thorax. Phys Med Biol. 52(13):3949–3963. 2007.
6. Tao S, Wu A, Wu Y, Chen Y, Zhang J. Patient setup in radiotherapy with video-based positioning system. Clin Oncol (R Coll Radiol). 18(4):363–366. 2006.

7. Yan Y, Song Y, Boyer AL. An investigation of a video- based patient repositioning technique. Int J Radiat Oncol Biol Phys. 54(2):606–614. 2002.
8. Johnson LS, Milliken BD, Hadley SW, Pelizzari CA, Haraf DJ, Chen GT. Initial clinical experience with a video- based patient positioning system. Int J Radiat Oncol Biol Phys. 45(1):205–213. 1999.
9. MacKay RI, Graham PA, Logue JP, Moore CJ. Patient positioning using detailed three-dimensional surface data for patients undergoing conformal radiation therapy for carcinoma of the prostate: a feasibility study. Int J Radiat Oncol Biol Phys. 49(1):225–230. 2001.

10. Cervino LI, Pawlicki T, Lawson JD, Jiang SB. Frame-less and mask-less cranial stereotactic radiosurgery: a feasibility study. Phys Med Biol. 55(7):1863–1873. 2010.
11. Xu SP, Xie CB, Ju ZJ, et al. Measurement and analysis of the imaging dose with megavoltage computed tomography for helical tomotherapy. Ai Zheng. 28(8):886–889. 2009.

12. Beldjoudi G, Yartsev S, Bauman G, Battista J, Van Dyk J. Schedule for CT image guidance in treating prostate cancer with helical tomotherapy. Br J Radiol. 83(987):241–251. 2010.

13. Ju SG, Huh W, Hong CS, et al. Development of a video- guided real-time patient motion monitoring system. Med Phys. 39(5):2396–2404. 2012.
Go to : 
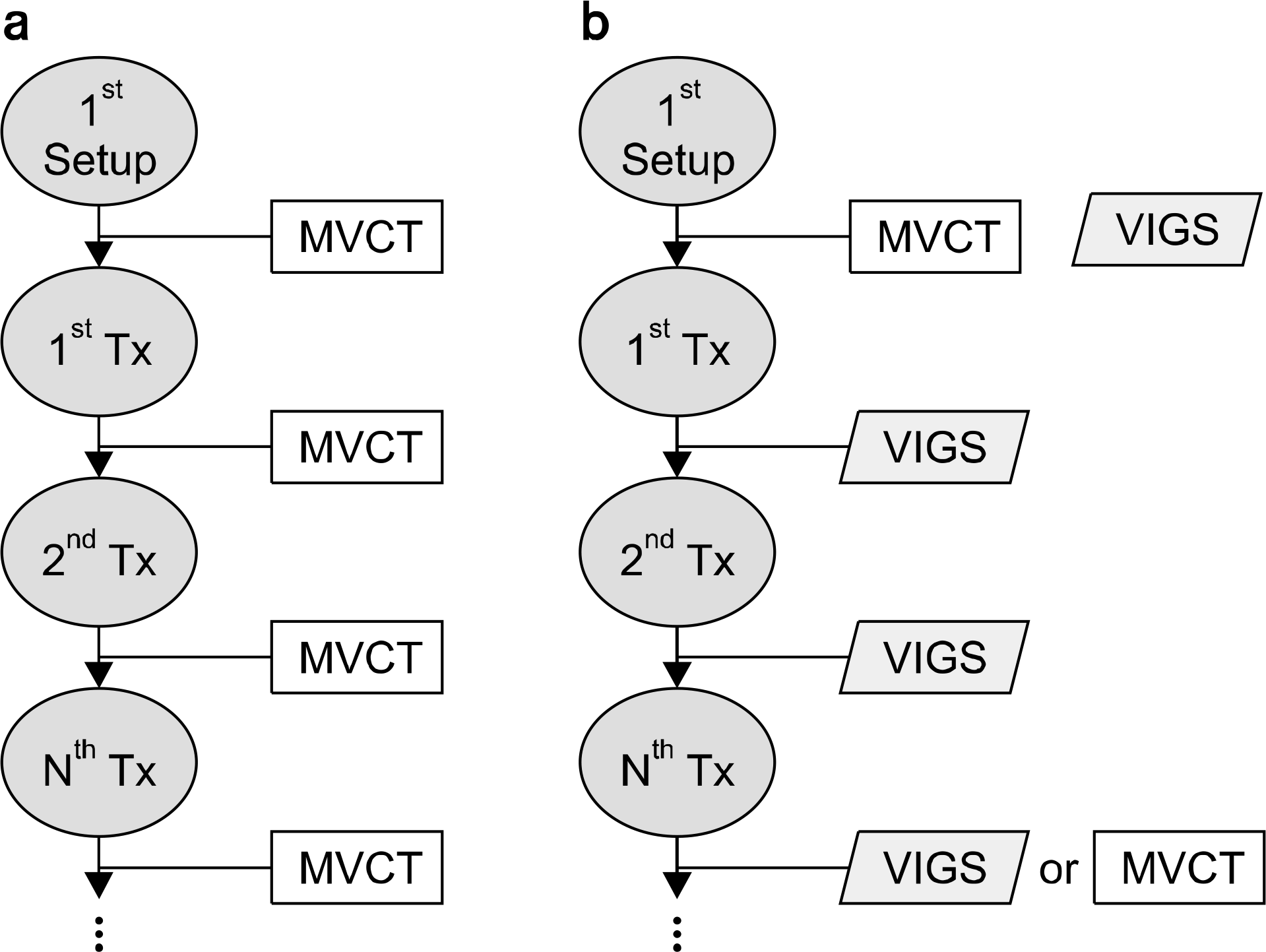 | Fig. 1.Comparison of treatment process using (a) MVCT and (b) VIGS (Video Image-Guided Setup). The treatment process is shown for the typical patient using the first video image obtained after the MVCT correction as a reference image. |
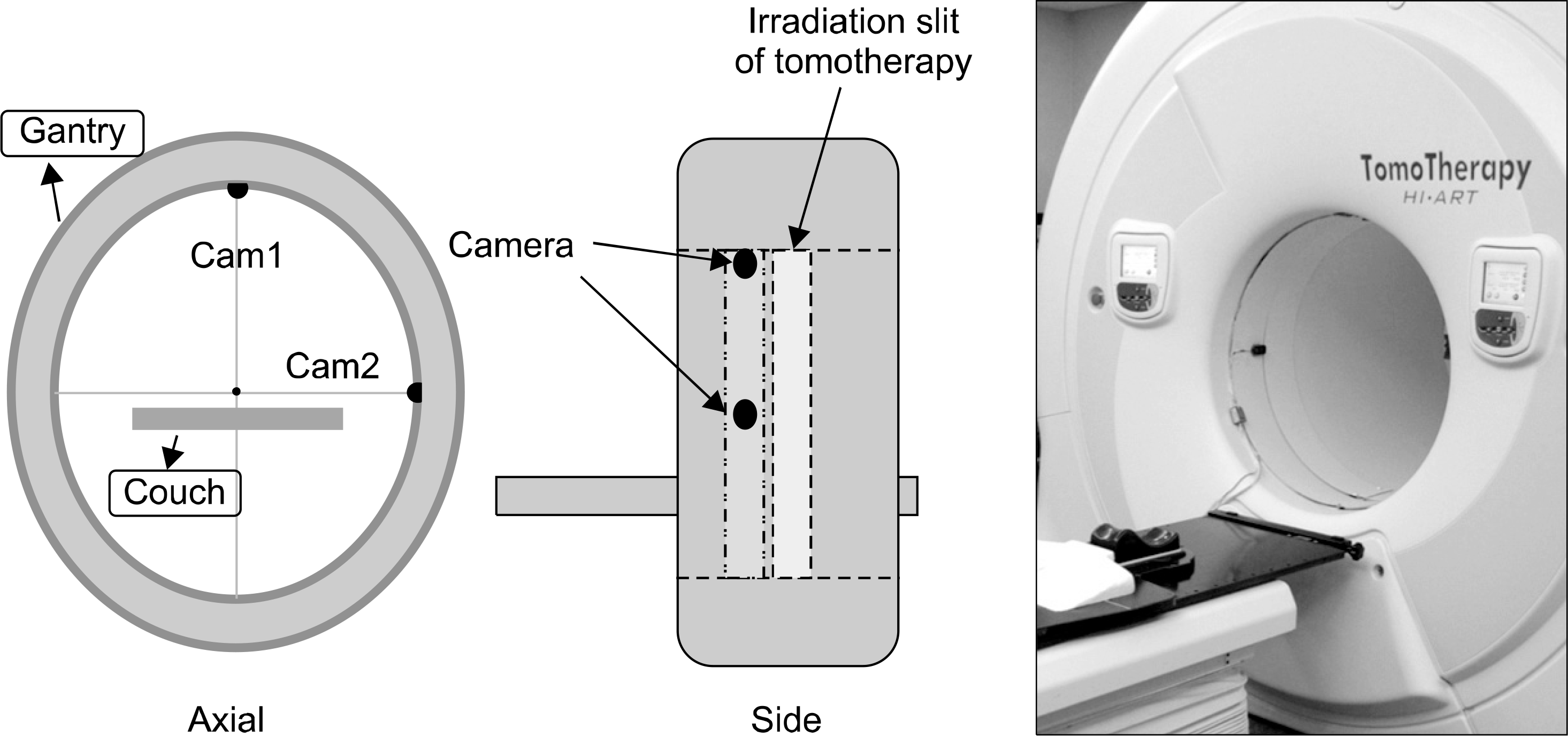 | Fig. 2.In the closed-tomotherapy gantry, two cameras that meet at right angles are installed to take the patient's orthogonal image. It is important to install the cameras so that they do not block the slit through which radiation is emitted. |
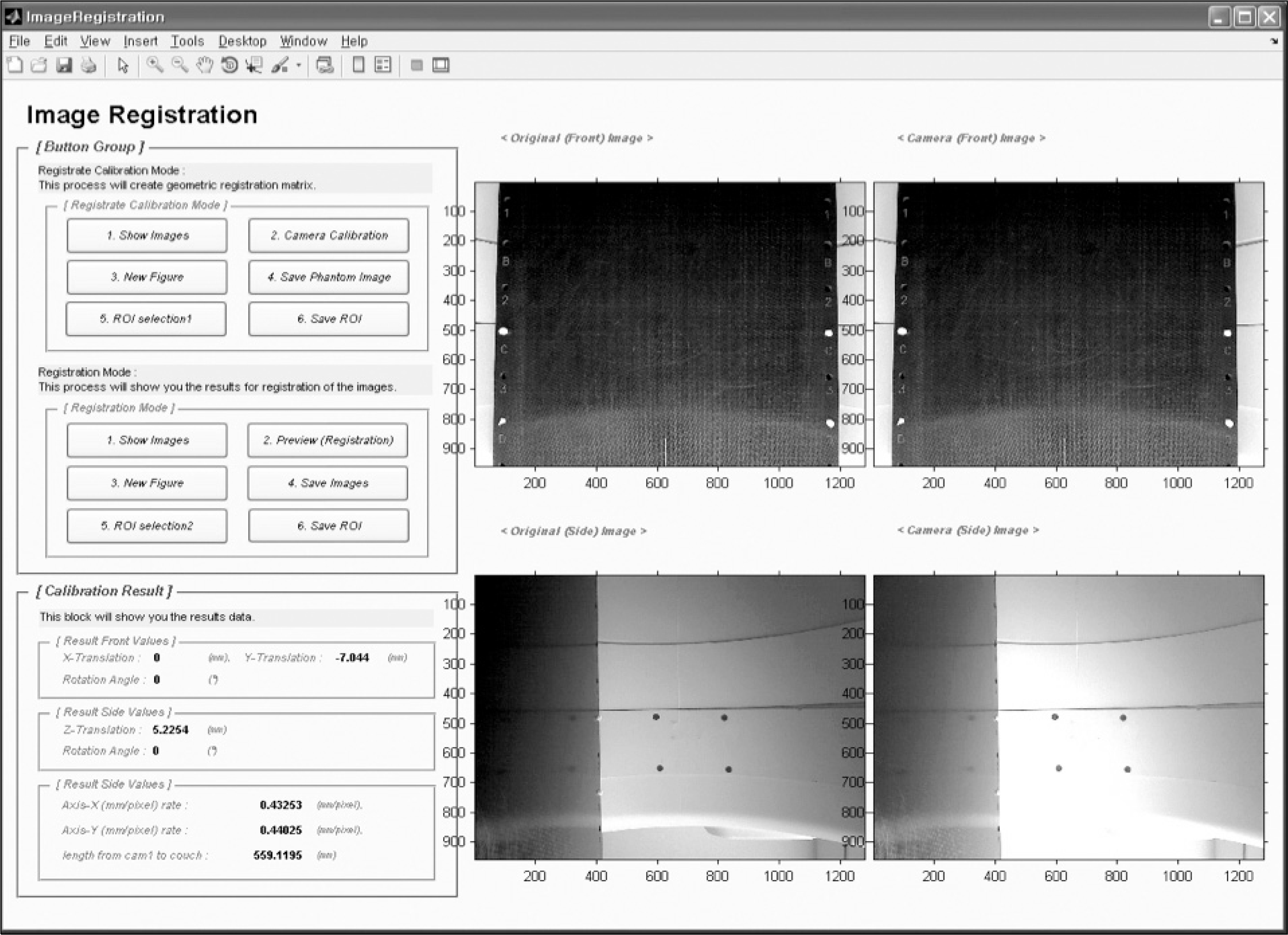 | Fig. 3.The GUI program for the camera calibration. The empty couch image (anterior-posterior image) with 4 holes is acquired with the camera 1 (on Fig. 2) and in-house made fixed pattern on gantry ring image is also capture with the camera 2 (on Fig. 2). With pre-known distance between holes, the calibration program calculates the spatial transformation between original image and each calibration image and defines the number of pixels on the distance in millimeters per pixel for the correction. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download