Abstract
Breast cancer is the leading cause of cancer death in women worldwide and the number of women breast cancer patient was increased continuously. Most of breast cancer patient has suffered from unnecessary radiation exposure to heart, lung. Low radiation dose to the heart could lead to the worsening of preexisting cardiovascular lesions caused by radiation induced pneumonitis. Also, several statistical reports demonstrated that left-sided breast cancer patient showed higher mortality than right-sided breast cancer patient because of heart disease. In radiation therapy, Deep Inspiration Breath Hold (DIBH) technique which the patient takes a deep inspiration and holds during treatment and could move the heart away from the chest wall and lung, has showed to lead to reduction in cardiac volume and to minimize the unnecessary radiation exposure to heart during treatment. In this study, we investigated the displacement of heart using DIBH CT data compared to free-breathing (FB) CT data and radiation exposure to heart. Treatment planning was performed on the computed tomography (CT) datasets of 10 patients who had received lumpectomy treatments. Heart, lung and both breasts were outlined. The prescribed dose was 50 Gy divided into 28 fractions. The dose distributions in all the plans were required to fulfill the International Commission on Radiation Units and Measurement specifications that include 100% coverage of the CTV with ≥95% of the prescribed dose and that the volume inside the CTV receiving >107% of the prescribed dose should be minimized. Scar boost irradiation was not performed in this study. Displacement of heart was measured by calculating the distance between center of heart and left breast. For the evaluation of radiation dose to heart, minimum, maximum and mean dose to heart were calculated. The present study demonstrates that cardiac dose during left-sided breast radiotherapy can be reduced by applying DIBH breathing control technique.
Go to : 
REFERENCES
2. Early Breast Cancer Trialists'Collaborative Group (EBCTCG). Effects of radiotherapy and of differences in the extent of surgery for early breast cancer on local recurrence and 15-year survival: an overview of the randomised trials. Lancet. 366(9503):2087–2106. 2005.
3. Sarah CD, Paul MG, Carolyn WT, et al. Longterm mortality from heart disease and lung cancer after radiotherapy for early breast cancer: prospective cohort study of about 300 000 women in US SEER cancer registries. Lancet Oncol. 6(8):557–565. 2005.
4. Ross CS, Hussey DH, Pennington EC, et al. Analysis of movement of intrathoracic neoplasms using ultrafast computerized tomography. Int J Radiat Oncol Biol Phys. 18(3):671–677. 1990.

5. Korin HW, Ehman RL, Riederer SJ, Felmlee JP, Grimm RC. Respiratory kinematics of the upper abdominal organs: a quantitative study. Magn Reson Med. 23(1):172–178. 1992.

6. Davies SC, Hill AL, Holmes RB, Haliwell M, Jackson PC. Ultrasound quantitation of respiratory organ motion in the upper abdomen. Br J Radiol. 67(803):1096–1102. 1994.

7. Kubo HD, Hill BC. Respiration gated radiotherapy treatment: a technical study. Phys Med Biol. 41(1):83–91. 1996.

8. Underberg RW, Lagerwaard FJ, Cuijpers JP, et al. Four Dimensional CT scans for treatment planning in stereotactic radiotherapy for stage 1 lung cancer. Int J Radiat Oncol Biol Phys. 60(4):1283–1290. 2004.
9. Keall PJ, Mageras GS, Balter JM, et al. The management of respiratory motion in radiation oncology report of AAPM Task Group 76. Med Phy. 33(10):3874–3900. 2006.
10. Lu W, Xiaoming C, Lin MH, et al. Evaluation of the cone beam CT for internal target volume localization in lung stereotactic radiotherapy in comparison with 4D MIP images. Med Phy. 40(11):111709. 2013.
11. Guckenberger M, Sweeney RA, Wilbert J, et al. Imageguided radiotherapy for liver cancer using respiratory-correlated computed tomography and cone-beam computed tomography. Int J Radiat Oncol Biol Phys. 71(1):297–304. 2008.

12. Shim JG, Kim JK, Park W, et al. Dose-volume analysis of lung and heart according to respiration in breast cancer patients treated with breast conserving surgery. J Breast Cancer. 15(1):105–110. 2012.

13. Victy YWW, Stewart YT, Ng Alice WY, et al. Real-time monitoring and control on deep inspiration breath-hold for lung cancer radiotherapy combination of ABC and external marker tracking. Med Phys. 37(9):4673–46833. 2010.
14. Bernd G, Cengiz D, Aline K, et al. Active breathing control (ABC): Determination and reduction of breathing-induced organ motion in the chest. Int J Radiat Oncol Biol Phys. 67(3):742–749. 2007.
15. Borst GR, Sonke JJ, Hollander SD, et al. Clinical results of image-guided deep inspiration breath hold breast irradiation. Int J Radiat Oncol Biol Phys. 78(5):1345–1351. 2010.

16. Pemler P, Besserer J, Lombriser N, Pescia R, Schneider U. Influence of respiration-induced organ motion on dose distributions in treatments using enhanced dynamic wedges. Med Phys. 28(11):2234–2240. 2001.

Go to : 
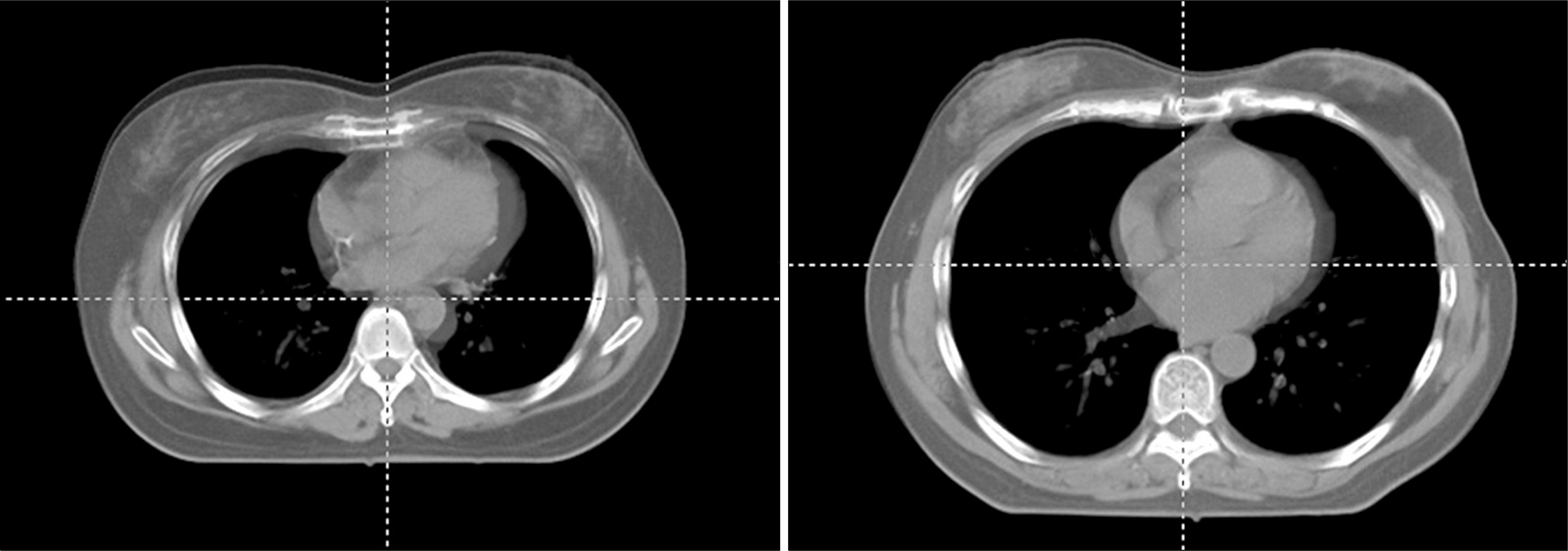 | Fig. 2.Superimposed free breathing CT images (in light gray) and DIBH technique image (in gray). |
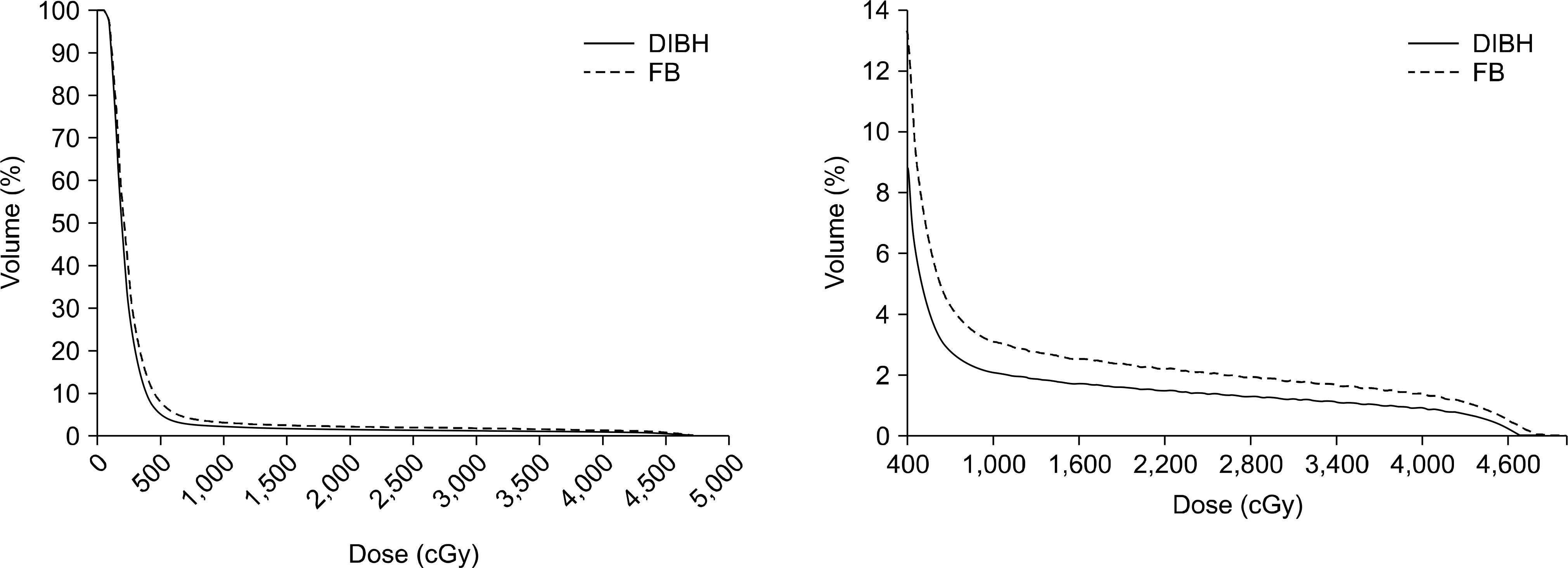 | Fig. 3.Dose-volume histogram (DVH) for heart between free-breathing (FB) and deep-inspiration breath-hold (DIBH) technique. |
Table 1.
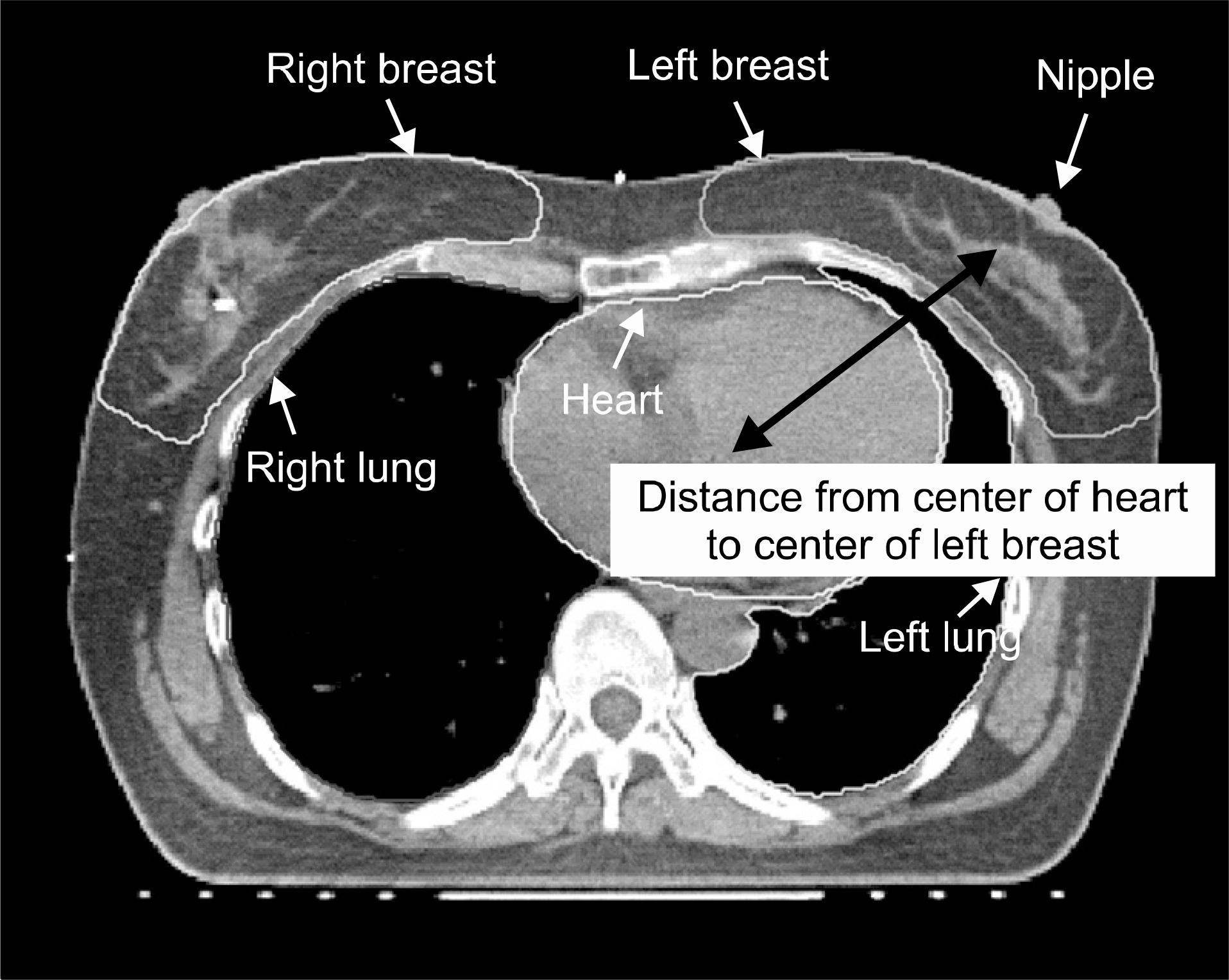
Distances from center of heart to center of lef breast. Unit: mm.
Table 2.
Exposure doses for heart between free-breathing (FB) and deep-inspiration breath-hold (DIBH) technique in each patient. Unit: cGy.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download