Abstract
Background
Alternatives to carbapenem are increasingly needed to decrease the usage of carbapenem. We evaluated the possibility of using non-carbapenem antibiotics against urinary tract infections (UTI) caused by extended-spectrum beta-lactamase-producing Enterobacteriaceae (ESBL-PE).
Methods
This retrospective study was performed at 2 university hospitals between October 2010 and December 2012. All diagnosed adult cases of ESBL-PE UTI were identified from the microbiological database. The subjects were divided into 3 groups based on the empirical antibiotic classes and susceptibility: carbapenem (C) group, susceptible non-carbapenem (SNC) group, and non-susceptible non-carbapenem (NSNC) group.
Results
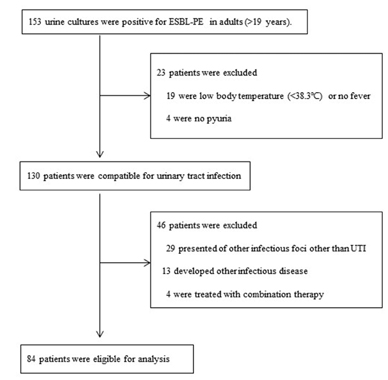
A total of 84 patients were eligible for analysis. For empirical therapy, 41, 23, and 20 patients were included in the NSNC, SNC, and C empirical groups, respectively. During the empirical therapy, 7 patients (17.1%) in the NSNC group, 18 patients (78.3%) in the SNC group, and 19 patients (78.3%) in the C group experienced clinical improvement. No significant difference was observed between the SNC and C empirical groups (P=0.192). Severe sepsis or shock was the predictor of empirical SNC treatment failure (P=0.048). There was a tendency to use carbapenem as a definite therapy in cases of NSNC. In contrast, empirical SNC was maintained as a definite therapy.
REFERENCES
1. Pitout JD, Laupland KB. Extended-spectrum beta-lactamase-producing Enterobacteriaceae: an emerging public-health concern. Lancet Infect Dis. 2008; 8:159–166.
2. Schwaber MJ, Carmeli Y. Carbapenem-resistant Enterobacteriaceae: a potential threat. JAMA. 2008; 300:2911–2913.
3. Patel G, Huprikar S, Factor SH, Jenkins SG, Calfee DP. Outcomes of carbapenem-resistant Klebsiella pneumoniae infection and the impact of antimicrobial and adjunctive therapies. Infect Control Hosp Epidemiol. 2008; 29:1099–1106.

4. Rodríguez-Baño J, Navarro MD, Retamar P, Picón E, Pascual Á. Extended-Spectrum Beta-Lactamases-Red Española de Investigación en Patología Infecciosa/Grupo de Estudio de Infección Hospitalaria Group. β-Lactam/β-lactam inhibitor combinations for the treatment of bacteremia due to extended-spectrum β-lactamase-producing Escherichia coli: a post hoc analysis of prospective cohorts. Clin Infect Dis. 2012; 54:167–174.
5. Vardakas KZ, Tansarli GS, Rafailidis PI, Falagas ME. Carbapenems versus alternative antibiotics for the treatment of bacteraemia due to Enterobacteriaceae producing extended-spectrum β-lactamases: a systematic review and meta-analysis. J Antimicrob Chemother. 2012; 67:2793–2803.

6. Lee NY, Lee CC, Huang WH, Tsui KC, Hsueh PR, Ko WC. Cefepime therapy for monomicrobial bacteremia caused by cefepime-susceptible extended-spectrum beta-lactamase-producing Enterobacteriaceae: MIC matters. Clin Infect Dis. 2013; 56:488–495.

7. Jansåker F, Frimodt-Møller N, Sjögren I, Dahl Knudsen J. Clinical and bacteriological effects of pivmecillinam for ESBL-producing Escherichia coli or Klebsiella pneumoniae in urinary tract infections. J Antimicrob Chemother. 2014; 69:769–772.
8. Doi A, Shimada T, Harada S, Iwata K, Kamiya T. The efficacy of cefmetazole against pyelonephritis caused by extended-spectrum beta-lactamase-producing Enterobacteriaceae. Int J Infect Dis. 2013; 17:e159–e163.

9. Pogue JM, Marchaim D, Abreu-Lanfranco O, Sunkara B, Mynatt RP, Zhao JJ, et al. Fosfomycin activity versus carbapenem-resistant Enterobacteriaceae and vancomycin-resistant Enterococcus, Detroit, 2008-10. J Antibiot (Tokyo). 2013; 66:625–627.

10. Garau J. Other antimicrobials of interest in the era of extended-spectrum beta-lactamases: fosfomycin, nitrofurantoin and tigecycline. Clin Microbiol Infect. 2008; 14 Suppl 1:198–202.
11. Tamma PD, Han JH, Rock C, Harris AD, Lautenbach E, Hsu AJ, et al. Carbapenem therapy is associated with improved survival compared with piperacillin-tazobactam for patients with extended-spectrum β-lactamase bacteremia. Clin Infect Dis. 2015; 60:1319–1325.

12. Kassakian SZ, Mermel LA. Changing epidemiology of infections due to extended spectrum beta-lactamase producing bacteria. Antimicrob Resist Infect Control. 2014; 3:9.

13. Paterson DL, Bonomo RA. Extended-spectrum beta-lactamases: a clinical update. Clin Microbiol Rev. 2005; 18:657–686.
14. Pullukcu H, Tasbakan M, Sipahi OR, Yamazhan T, Aydemir S, Ulusoy S. Fosfomycin in the treatment of extended spectrum beta-lactamase-producing Escherichia coli-related lower urinary tract infections. Int J Antimicrob Agents. 2007; 29:62–65.

15. von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Epidemiology. 2007; 18:800–804.
16. Johansen TE, Botto H, Cek M, Grabe M, Tenke P, Wagenlehner FM, et al. Critical review of current definitions of urinary tract infections and proposal of an EAU/ESIU classification system. Int J Antimicrob Agents. 2011; 38 Suppl:64–70.

17. Senol S, Tasbakan M, Pullukcu H, Sipahi OR, Sipahi H, Yamazhan T, et al. Carbapenem versus fosfomycin tromethanol in the treatment of extended-spectrum beta-lactamase-producing Escherichia coli-related complicated lower urinary tract infection. J Chemother. 2010; 22:355–357.
18. Auer S, Wojna A, Hell M. Oral treatment options for ambulatory patients with urinary tract infections caused by extended-spectrum-beta-lactamase-producing Escherichia coli. Antimicrob Agents Chemother. 2010; 54:4006–4008.
Table 1.
Characteristics of patients with urinary tract infectionscaused by extended-spectrum beta-lactamase-producing Enterobacteriaceae based on empirical antibiotic groups
Table 2.
Differences in clinical outcomes among empirical antibiotic groups
Table 3.
Factors associated with failure of empirical treatment for urinary tract infections caused by extended-spectrum beta-lactamase-producing Enterobacteriaceae




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download