Dear Editor:
Schnitzler syndrome (SchS) is a rare autoinflammatory disease characterized by a recurrent urticaria and monoclonal gammopathy1. Herein, to our knowledge, we report the first case of SchS in Korea. The study protocol was approved by the Institutional Review Board of Seoul St. Mary's Hospital, The Catholic University of Korea (KC16ZISE0262).
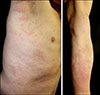
A 64-year-old man presented with two year history of daily urticaria. On physical examination, wheals and erythematous patches were found on the trunk and both extremities (Fig. 1). In contrast to most patients with urticaria, there was no pruritus, and antihistamine therapies did not have any effect. Only systemic steroid treatment yielded transient symptom improvement. The individual lesions lasted about 24 hours and resolved completely. Associated symptoms were musculoskeletal pain, and bouts of fever. Laboratory investigations showed leukocytosis (10.57×109/L), an elevated erythrocyte sedimentation rate (77 mm/hr; 0~20 mm/hr) and an increased C-reactive protein (CRP) level (11.95 mg/L; 0.01~0.47 mg/L). Increased immunoglobulin (Ig)M levels (852 mg/dL; 46~260 mg/dL), decreased IgG (831 mg/dL; 870~1,700 mg/dL) and IgA (99 mg/dL; 110~410 mg/dL) were detected. Elevated levels of free kappa light chain (32.95 mg/L; 3.30~19.40 mg/L) were detected. Immunofixation analysis confirmed a monoclonal gammopathy of the IgM type (Fig. 2A, B). Based on these clinical and laboratory findings, he was diagnosed with SchS. Various steroid sparing agents such as cyclosporine, methotrexate, and dapsone were tried, and he showed relatively good effect to cyclosporine. We treated with cyclosporin 100~200 mg and antihistamines, and additionally systemic steroid and nonsteroidal anti-inflammatory drug for the acute exacerbation. He showed wax and waning course during the 5-year follow up periods.
According to the largest retrospective study of SchS, male/female ratio was 1.76 and the mean onset age was 51.6 years1. IgM (κ) light-chain gammopathy is predominantly reported in SchS (more than 90%)2. Simon et al.1 proposed a set of Strasbourg diagnostic criteria that included two obligate criteria: (1) chronic urticarial rash and (2) monoclonal IgM or IgG, and four minor criteria: (1) recurrent fever, (2) objective findings of abnormal bone remodeling with or without bone pain, (3) neutrophilic dermal infiltrate on skin biopsy, and (4) leukocytosis and/or elevated CRP. Definite diagnosis can be made for a patient who satisfies the two obligate criteria and at least two minor criteria if the patient has monoclonal IgM gammopathy, and at least three minor criteria if the patient has monoclonal IgG gammopathy. Therefore, our case was diagnosed as definite SchS. Possible exacerbating factors such as alcohol, spicy food, and psychological stress should be avoided, if identified3. Recommended treatment modalities include observation, colchicine, short-course nonsteroidal anti-inflammatory drugs and anakinra based on the degree of quality of life and inflammatory markers1. Long term follow-up is recommended due to risk of a lymphoproliferative disorders4.
Although cases of SchS have been reported worldwide, there was no report of SchS in Korea. One retrospective study reviewed 609 patients with recurrent urticaria who received laboratory investigations of CRP and protein electrophoresis, and found that none fulfilled criteria for SchS5. We speculated that genetic factors and unrecognized cases might contribute to the low incidence in Korea. Physicians should suspect SchS in cases of recurrent urticaria with atypical clinical features.
Figures and Tables
References
1. Simon A, Asli B, Braun-Falco M, De Koning H, Fermand JP, Grattan C, et al. Schnitzler's syndrome: diagnosis, treatment, and follow-up. Allergy. 2013; 68:562–568.

2. Sokumbi O, Drage LA, Peters MS. Clinical and histopathologic review of Schnitzler syndrome: the Mayo Clinic experience (1972-2011). J Am Acad Dermatol. 2012; 67:1289–1295.

3. de Koning HD, Bodar EJ, van der Meer JW, Simon A. Schnitzler Syndrome Study Group. Schnitzler syndrome: beyond the case reports: review and follow-up of 94 patients with an emphasis on prognosis and treatment. Semin Arthritis Rheum. 2007; 37:137–148.

4. Gameiro A, Gouveia M, Pereira M, Tellechea O, Gonçalo M. Clinical characterization and long-term follow-up of Schnitzler syndrome. Clin Exp Dermatol. 2016; 41:461–467.

5. SShin JJ, Lee JM, Jang HW, Jung SK, Kim IH. Chronic urticaria and monoclonal gammopathy: does Schnitzler syndrome exist in Koreans? In : Proceedings of the 66th Annual Conference of Korean Dermatological Association; 2014 Oct 18-19; p. 280.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download