Abstract
Purpose
The purpose of the study was to investigate the effects of laughter therapy on depression and sleep among patients at two long-term care (LTC) hospitals.
Methods
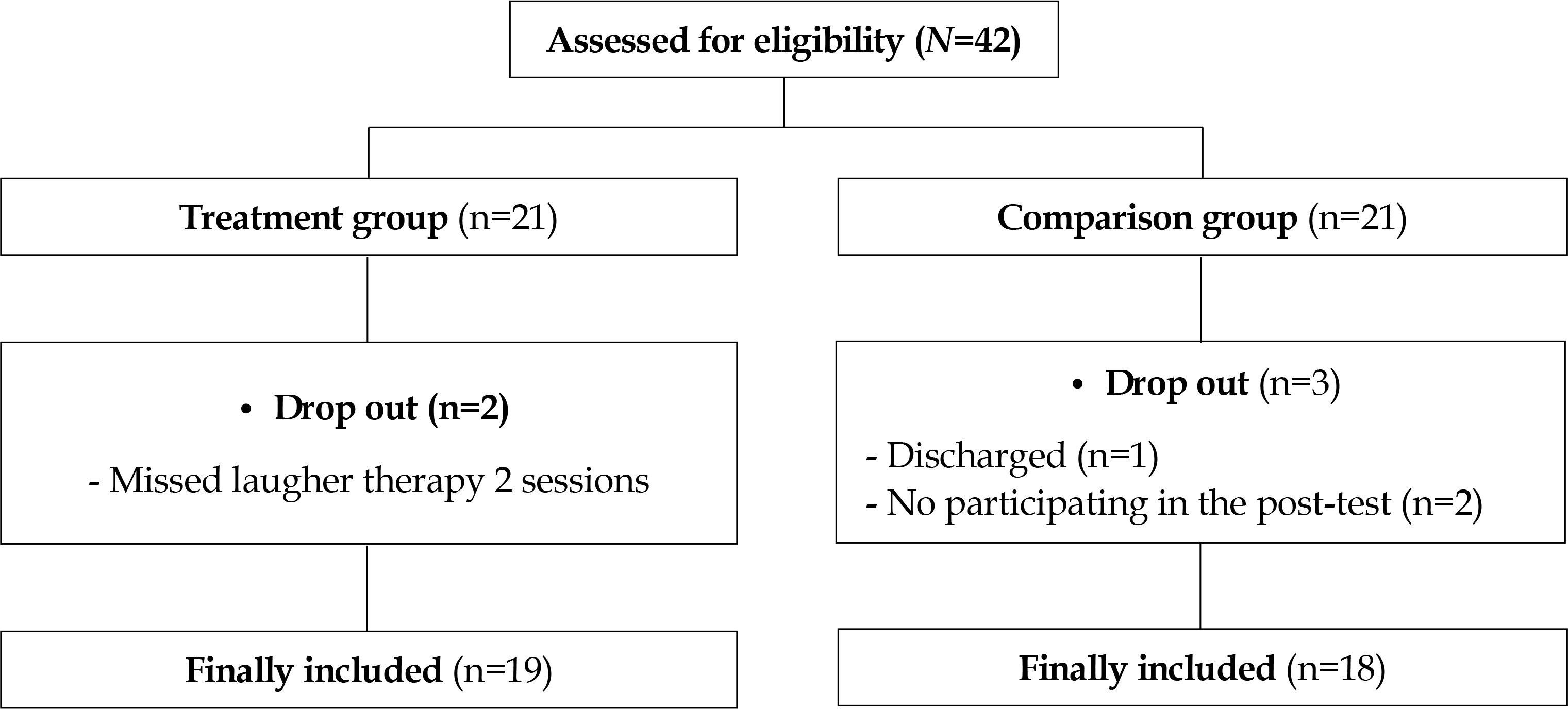
Forty-two residents from two LTC hospitals participated in this study. Twenty-one residents at one LTC hospital received the laugher therapy treatment and 21 at the other LTC hospital received no treatment as a comparison group. The laugher therapy protocol consisted of singing funny songs, laughing for diversion, stretching, playing with hands and dance routines, laughing exercises, healthy clapping, and laughing aloud. The participants engaged in the protocol 40 minutes twice a week (Monday/Thursday) for a total of eight sessions held in the patients’ lounge.
Go to : 
REFERENCES
1. Health Insurance Review & Assessment Service. Status of me-dicalinstitutions [Internet]. Seoul: Health Insurance Review & Assessment Service;2015. [cited 2015 Oct 15]. Available from:. http://opendata.hira.or.kr/op/opc/yadmOpCloPrsnt.do?searchType=&dateType=&frYear=2015&frMonth=09&ykihoPl cTpCd=&ykihoPlcTpCdNm=&clCd=28&shwSbjtCd=.
2. Eun Y, Ko SH, Kim MJ, Kim JS, Park MH. Introduction to gerontological nursing. Seoul: Hyeonmunsa;2010.
3. Park EO. Effects of visiting laughter therapy on depression and insomnia among the vulnerable elderly. Journal of Korean Academy of Community Health Nursing. 2013; 24(2):205–13. https://doi.org/10.12799/jkachn.2013.24.2.205.

4. Almeida OP, Pfaff JJ. Sleep complaints among older general practice patients: association with depression. British Journal of General Practice. 2005; 55(520):864–6.
5. Park YH. Physical activity and sleep patterns in elderly who visited a community senior center. Journal of Korean Academy of Nursing. 2007; 37(1):5–13.

6. Redeker NS. Sleep in acute care settings: an integrative review. Journal of Nursing Scholarship. 2000; 32(1):31–8.

7. Jang HY, Kim TI. Sleep patterns and it's influencing factors of hospitalized elderly in long-term care hospital. Journal of the Korean Data & Information Science Society. 2016; 27(3):773–89.

8. Won WY, Lee CU. Pharmacological treatment of psychiatric disorders of the elderly. The Journal of the Korean Medical Association. 2010; 53(11):972–83. https://doi.org/10.5124/jkma.2010.53.11.972.

9. Takeda M, Hashimoto R, Kudo T, Okochi M, Tagami S, Mori-hara T, et al. Laughter and humor as complementary and alternative medicines for dementia patients. BMC Complement and Alternative Medicine. 2010; 10(1):28. https://doi.org/10.1186/1472-6882-10-28.

10. Berk LS, Felten DL, Tan SA, Bittman BB, Westengard J. Modulation of neuroimmune parameters during the eustress of humor-associated mirthful laughter. Alternative Therapies in Health Medicine. 2001; 7(2):62–76.
11. Cha MY, Hong HS. Effect and path analysis of laughter therapy on serotonin, depression and quality of life in middle- aged women. Journal of Korean Academy of Nursing. 2015; 45(2):221–30. https://doi.org/10.4040/jkan.2015.45.2.221.
12. Jung HW, Yoon CH, Cho NR, Lee MK, Lee JB. The effect of laughter therapy on sleep in the community-dwelling elderly. Korean Journal of Family Medicine. 2009; 30(7):511–8. https://doi.org/10.4082/kjfm.2009.30.7.511.

13. Kim YS, Jeon SS. The influence of one-time laughter therapy on stress response in the elderly. Journal of Korean Academy of Psychiatric and Mental Health Nursing. 2009; 18(3):269–77.
14. Ko HJ, Youn CH. Effects of laughter therapy on depression, cognition and sleep among the community-dwelling elderly. Geriatrics and Gerontology International. 2011; 11(3):267–74. https://doi.org/10.1111/j.1447-0594.2010.00680.x.

15. Lee HK, Byeon DH, Park YS, Kim JS, Gil JH. Effects of the laughter therapy on blood pressure, depression and quality of life in rural elderly women. Journal of the Korea Academia-Industrial cooperation Society. 2013; 14(4):1810–9. https://doi.org/10.5762/kais.2013.14.4.1810.

16. Lee KI, Eun Y. Effect of laugher therapy on pain, depression and sleep with elderly patients in long term care facility. Journal of Muscle and Joint Health. 2011; 18(1):28–38. https://doi.org/10.5953/JMJH.2011.18.1.028.

17. Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed.Hillsdale, New Jersey: L. Erlbaum;1988.
18. Seo SY, Chang SY. Effect of laughing therapy on sleep, depression and self-esteem of elderly women in senior home. Journal of Regional Studies. 2011; 19(4):211–25.
19. Kwon YC, Park JH. Korean version of Mini-Mental State Examination (MMSE-K). Part I: development of the test for the elderly. Journal of Korean Neuropsychiatr Association. 1989; 28(1):125–35.
20. Kee BS. A preliminary study for the standardization of geriatric depression scale short form-Korea version. Journal of Korean Neuropsychiatr Association. 1996; 35(2):298–307.
21. Choi HJ, Kim SJ, Kim BJ, Kim IJ. Korean versions of self-reported sleep questionnaires for research and practice on sleep disturbance. The Korean Journal of Rehabilitation Nursing. 2012; 15(1):1–10. https://doi.org/10.7587/kjrehn.2012.1.

22. Han GI. Laughter therapy. Seoul: Samho MEDIA;2014.
23. Folstein MF, Folstein SE, McHugh PR. "Mini-mental state": a practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research. 1975; 12(3):189–98.
24. Won CW, Yang KY, Rho YG, Kim SY, Lee EJ, Yoon JL, et al. The development of Korean activities of daily living (K-ADL) and Korean instrumental activities of daily living (K-IADL) scale. Journal of the Korean Geriatrics Society. 2002; 6(2):107–20.
25. Yesavage JA, Sheikh JI. 9/Geriatric Depression Scale (GDS) recent evidence and development of a shorter violence. Clinical Gerontologist. 1986; 5(1-2):165–73. https://doi.org/10.1300/J018v05n01_09.
26. Chae KS. Effects of the laughing and music therapy on the depression and activities of autonomic nervous system for elderly with dementia. Journal of Korean Biological Nursing Science. 2015; 17(3):245–52. https://doi.org/10.7586/jkbns.2015.17.3.245.
27. Lee JS, Kim KS, Kim MY, Oh SM, Oh SH, Lee HS. The effects of laughter therapy on sleep disturbance and depression among hemodialysis patient. Journal of Clinical Nursing Research. 2006; 9:107–50.
28. Ersser S, Wiles A, Taylor H, Wade S, Walsh R, Bentley T. The sleep of older people in hospital and nursing homes. Journal of Clinical Nursing. 1999; 8(4):360–8. https://doi.rog/10.1046/j.1365-2702.1999.00267.x.

29. Lee IS, Bae GH, Baek JS. Laughter therapy introduction. Seoul: Changjisa;2009.
Go to : 
Table 1.
Contents of Laughter Therapy
Table 2.
Characteristics of Participants at the Long-term Care Hospitals (N=37)
| Characteristics | Categories | Treatment group (n=19) | Comparison group (n=18) | x2 or t or Z | p |
|---|---|---|---|---|---|
| n (%)/M± SD | n (%)/M± SD | ||||
| Gender | Male | 11 (57.9) | 8 (44.4) | 0.67 | .313 |
| Female | 8 (42.1) | 10 (55.6) | |||
| Age (year) | 65~79 | 12 (63.2) | 10 (55.6) | 0.22 | .446 |
| ≥80 | 7 (36.8) | 8 (44.4) | |||
| Education | ≤ Elementary school | 11 (57.9) | 13 (72.2) | 0.83 | .286 |
| ≥ Middle school | 8 (42.1) | 5 (27.8) | |||
| Medical diagnosis | CVD | 9 (47.4) | 8 (44.4) | 0.25 | .882 |
| MCI | 4 (21.0) | 3 (16.7) | |||
| Others† | 6 (31.6) | 7 (38.9) | |||
| Sleeping pills‡ | Yes | 5 (26.3) | 6 (33.3) | 0.22 | .457 |
| No | 14 (73.7) | 12 (66.7) | |||
| Antidepressants | Yes | 5 (26.3) | 5 (27.8) | 0.01 | .605 |
| No | 14 (73.7) | 13 (72.2) | |||
| Hospitalization | ≤1 year | 11 (57.9) | 11 (61.1) | 0.04 | .554 |
| >1 year | 8 (42.1) | 7 (38.9) | |||
| Cognition | 26.47±2.86 | 25.94±2.62 | -0.59 | .562 | |
| ADL | 12.00±3.63 | 10.83±2.68 | -1.35 | .179 | |
| Depression | 8.37±1.54 | 8.17±1.98 | -0.35 | .730 | |
| Sleep | 8.98±3.08 | 9.22±3.39 | -0.28§ | .783 |
Table 3.
Difference in Depression and Sleep between the Two Groups (N=37)
| Variables | Groups | Pretest | Posttest | Difference | Paired t or Z | p | t or Z | p |
|---|---|---|---|---|---|---|---|---|
| M± SD | M± SD | M± SD | ||||||
| Depression | Treatment (n=19) | 8.37±1.54 | 5.32±1.20 | -3.05±1.31 | 8.96< | <.001 | 7.12 | <.001 |
| Comparison (n=18) | 8.17±1.98 | 7.94±2.49 | -0.22±1.17 | 0.81 | .429 | |||
| Sleep | Treatment (n=19) | 8.68±3.38 | 6.53±2.34 | -2.42±1.22 | -3.62† < | <.001 | 4.16‡ | <.001 |
| Comparison (n=18) | 9.22±3.39 | 8.83±3.13 | -0.39±0.92 | -0.88† | .378 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download