Abstract
Purpose
This study aimed to examine the perception of food allergy among parents and school health instructors in Korea.
Methods
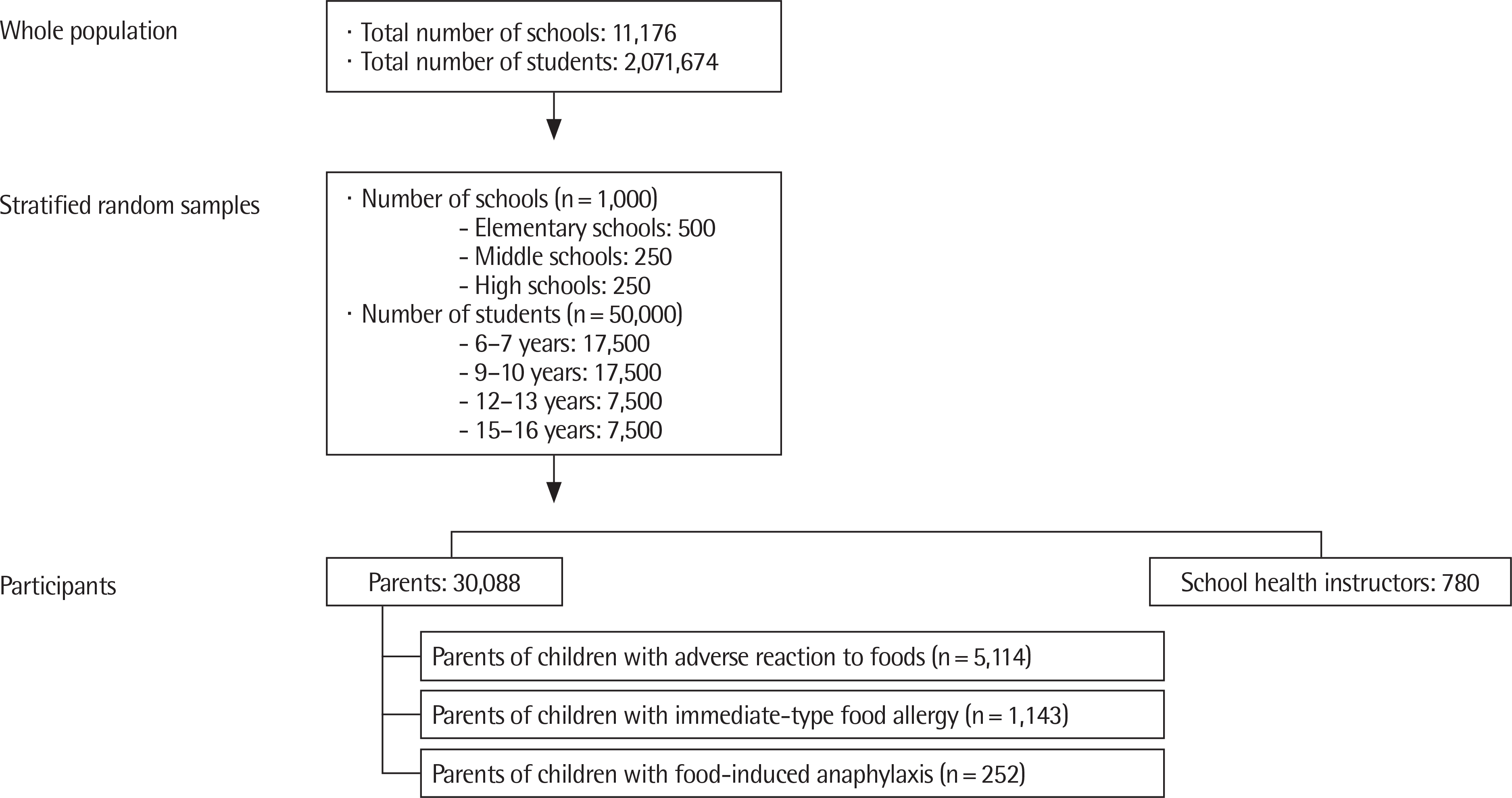
A nationwide epidemiological survey in Korea was conducted in September 2015. From 17 cities and provinces, a total of 1,000 elementary, middle and high schools were selected by stratified random sampling. Parents and school health instructors were surveyed using a questionnaire on the perception of food allergy.
Results
The prevalence of food-induced anaphylaxis was 22.3%. Of 252 children with anaphylaxis, 47.6% were prescribed epinephrine autoinjector (EAI). Forty-three parents (37.7%) were educated about the use of EAI. Parents carrying their own EAI at all times or keeping them at schools were 5.6% and 3.8%, respectively. For the food allergen-labeling system, 42.1% of parents read food labels, and 32.1% were satisfied with the system. Only 35.2% of school health instructors received education on food allergy and anaphylaxis, and 42.5% of them knew how to use EAI. There were 70 children (9.4%) with anaphylaxis in school, and 75.9% of schools had the emergency management system.
Conclusion
The awareness of Korean parents and school health instructors on food allergy is still low, and many parents are dissat-isfied with the food allergen labeling system. Many school health instructors have difficulty in using EAI in case of anaphylaxis and are insufficiently educated about food allergy. Therefore, it is necessary to establish more systematic food allergy management plans by providing high-quality education to parents and school health instructors and by utilizing legal systems.
Go to : 
REFERENCES
2. Kim WK. Diagnosis and treatment of food allergy in children. Pediatr Allergy Respir Dis. 2006; 16:274–83.
3. Ahn K. Food allergy: diagnosis and management. Korean J Asthma Allergy Clin Immunol. 2011; 31:163–9.
4. Mukoyama T, Nishima S, Arita M, Ito S, Urisu A, Ebisawa M, et al. Guidelines for diagnosis and management of pediatric food allergy in Japan. Allergol Int. 2007; 56:349–61.

6. Branum AM, Lukacs SL. Food allergy among U.S. children: trends in prevalence and hospitalizations. NCHS Data Brief. 2008; (10):1–8.
7. Kanny G, Moneret-Vautrin DA, Flabbee J, Beaudouin E, Morisset M, Thevenin F. Population study of food allergy in France. J Allergy Clin Immunol. 2001; 108:133–40.

8. Rona RJ, Keil T, Summers C, Gislason D, Zuidmeer L, Sodergren E, et al. The prevalence of food allergy: a metaanalysis. J Allergy Clin Immunol. 2007; 120:638–46.

9. Oh JW, Pyun BY, Choung JT, Ahn KM, Kim CH, Song SW, et al. Epidemiological change of atopic dermatitis and food allergy in school-aged children in Korea between 1995 and 2000. J Korean Med Sci. 2004; 19:716–23.

10. Son KY, Park KS, Hwang HH, Yun BS, Lee SJ, Kim MA, et al. Prevalence of allergic diseases among primary school children in Ilsan, Gyeonggi and changes of symptoms after environmental control in 2005. Pediatr Allergy Respir Dis. 2007; 17:384–93.
11. Seo WH, Jang EY, Han YS, Ahn KM, Jung JT. Management of food allergies in young children at a child care center and hospital in Korean. Pediatr Allergy Respir Dis. 2011; 21:32–8.

12. Vale S, Smith J, Said M, Mullins R, Loh R. ASCIA guidelines for prevention of anaphylaxis in schools, pre-schools and childcare: 2015 update. J Paediatr Child Health. 2015; 51:949–54.

13. Rosen J, Albin S, Sicherer SH. Creation and validation of web-based food allergy audiovisual educational materials for caregivers. Allergy Asthma Proc. 2014; 35:178–84.

14. Contreras-Porta J, Ruiz-Baqués A, Gabarron Hortal E, Capel Torres F, Ariño Pla MN, Zorrozua Santisteban A, et al. Evaluation of an educational programme with workshops for families of children with food allergies. Allergol Immunopathol (Madr). 2016; 44:113–9.

15. Choi Y, Ju S, Chang H. Food allergy knowledge, perception of food allergy labeling, and level of dietary practice: a comparison between children with and without food allergy experience. Nutr Res Pract. 2015; 9:92–8.

17. Lee Y, Kim HH, Ko YS. Perception on food allergy labelling and management of nutritional education among higher grade elementary school students in Jeju area. J Nutr Health. 2015; 48:530–41.

18. Kim YM, Heo YR, Ro HK. Perception and practices regarding food allergy of elementary and middle school nutritionists in the Jeonnam area. J Korean Soc Food Sci Nutr. 2014; 43:151–61.

19. Lee AH, Kim KE, Lee KE, Kim SH, Wang TW, Kim KW, et al. Prevalence of food allergy and perceptions on food allergen labeling in school food-service among Korean students. Allergy Asthma Respir Dis. 2013; 1:227–34.

20. Seo AD, Lee JY, Yang SI, Lee HR, Lee SY. Food allergic reactions in the community: a questionnaire survey of caregivers. Allergy Asthma Respir Dis. 2017; 5:27–33.

21. Kim YG, Yu KH, Ly SY. Perception of elementary school parents in Gyeongbuk area on allergenic food labeling system and children's food allergy status. Korean J Hum Ecol. 2013; 22:491–506.

22. Kim M, Lee JY, Jeon HY, Yang HK, Lee KJ, Han Y, et al. Prevalence of im-mediate-type food allergy in Korean schoolchildren in 2015: a nationwide, population-based study. Allergy Asthma Immunol Res. 2017; 9:410–6.

23. Sampson HA, Muñoz-Furlong A, Campbell RL, Adkinson NF Jr, Bock SA, Branum A, et al. Second symposium on the definition and management of anaphylaxis: summary report–Second National Institute of Allergy and Infectious Disease/Food Allergy and Anaphylaxis Network symposium. J Allergy Clin Immunol. 2006; 117:391–7.

24. Gang JS, Kim HS, Bang HH, Kim TH, Lee HJ, Hwangbo Y, et al. Pediatric anaphylaxis at a university hospital including the rate of prescribing epinephrine autoinjectors. Allergy Asthma Respir Dis. 2017; 5:135–40.

25. Gold MS, Sainsbury R. First aid anaphylaxis management in children who were prescribed an epinephrine autoinjector device (EpiPen). J Allergy Clin Immunol. 2000; 106(1 Pt 1):171–6.

26. Pouessel G, Deschildre A, Castelain C, Sardet A, Sagot-Bevenot S, de Sauve-Boeuf A, et al. Parental knowledge and use of epinephrine autoinjector for children with food allergy. Pediatr Allergy Immunol. 2006; 17:221–6.

27. Sicherer SH, Forman JA, Noone SA. Use assessment of self-administered epinephrine among food-allergic children and pediatricians. Pediatrics. 2000; 105:359–62.

28. Sabroe RA, Glendinning AK, Sabroe I, Lawlor F, Kobza Black A. An au-dit of the use of self-administered adrenaline syringes in patients with angio-oedema. Br J Dermatol. 2002; 146:615–20.

29. Hu W, Grbich C, Kemp A. Parental food allergy information needs: a qualitative study. Arch Dis Child. 2007; 92:771–5.

30. Lee SY, Kim KW, Ahn K, Kim HH, Pyun BY, Park YM, et al. Consumer's use and satisfaction of allergic food labels. Pediatr Allergy Respir Dis. 2011; 21:294–301.

31. Taylor CL, Wilkening VL. How the nutrition food label was developed, part 1: the Nutrition Facts panel. J Am Diet Assoc. 2008; 108:437–42.

32. Wootan MG, Osborn M. Availability of nutrition information from chain restaurants in the United States. Am J Prev Med. 2006; 30:266–8.

33. Polloni L, Baldi I, Lazzarotto F, Bonaguro R, Toniolo A, Celegato N, et al. School personnel's self-efficacy in managing food allergy and anaphylaxis. Pediatr Allergy Immunol. 2016; 27:356–60.

34. Carlisle SK, Vargas PA, Noone S, Steele P, Sicherer SH, Burks AW, et al. Food allergy education for school nurses: a needs assessment survey by the consortium of food allergy research. J Sch Nurs. 2010; 26:360–7.
Go to : 
Table 1.
Characteristics of children with food allergies (n=30,088)
Table 2.
Patterns of epinephrine autoinjector use in parents of children with food-induced anaphylaxis
Table 3.
Perception of food allergen labeling in parents of children with adverse reaction to foods
Table 4.
Perception of anaphylaxis among school health instructors
Table 5.
Problems that school health instructors are concerned about when using epinephrine autoinjector in case of anaphylaxis




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download