Abstract
Background
Optic disc drusen, which are calcified deposits that form anterior to the lamina cribrosa in the optic nerve, may mimic papilledema.
Case Report
We report herein three cases referred to us with suspicion of disc swelling and papilledema. Following ophthalmologic evaluation with B-scan ultrasound, red-free fundus photography, and computed tomography, the diagnosis of papilledema was excluded in all cases and optic disc drusen was diagnosed.
Conclusions
Clinical suspicion of optic disc drusen in cases presenting with swelling of the optic nerve head is important in order to avoid unnecessary interventions and anxiety. The reported cases highlight the commonly encountered clinical presentations and the practical aspects of diagnosis and management of optic disc drusen.
Optic disc drusen (ODD), which are congenital and developmental anomalies of the optic nerve head, are hyaline-containing bodies that, over time, appear as elevated, lumpy irregularities on the anterior portion of the optic nerve. Buried ODD cannot be detected, but superficial ODD may be diagnosed by fundus examination. ODD primarily result from axonal degeneration, or may form secondarily from compression of the preliminary nerve fibers and blood vessels by these extracellular preliminary deposits.1,2 Patients with ODD are often asymptomatic, with the condition being found incidentally during fundus examination. Visual acuity is well preserved but the visual fields of these patients can be abnormal and may deteriorate over time.1
ODD may mimic papilledema. Thus, clinical suspicion of ODD is important in cases with optic disc swelling in order to avoid unnecessary interventions, such as lumbar puncture. Several tests can aid the diagnosis of ODD, such as red-free fundus photography, ophthalmic ultrasonography (USG), computed tomography (CT), optical coherence tomography (OCT), and scanning laser ophthalmoscopy.
It is important to consider ODD in the differential diagnosis of optic nerve swelling, and particularly in cases of papilledema. We presented herein three cases of ODD that had previously been misdiagnosed as papilledema. Informed consent was obtained from all patients.
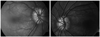
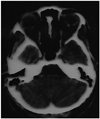
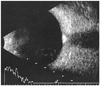
A 20-year-old female patient was referred from another clinic with a diagnosis of bilateral papilledema. On ocular examination, a posterior capsular cataract was the only remarkable finding of both anterior segments. Her best corrected visual acuity was 8/10 in the right eye and 10/10 in the left eye. Fundoscopy revealed swelling and a fluffy appearance of both optic discs. Red-free fundus photography revealed autofluorescence of the optic discs (Fig. 1). B-scan USG and orbital CT revealed calcification on the optic nerve head (Figs. 2 and 3). The patient was found to have no general or neurological signs. She was diagnosed with bilateral ODD. The diagnosis was explained and the patient discharged.
A 14-year-old female was admitted to a pediatric clinic with a complaint of headache. She was considered to have bilateral papilledema and consulted with our department for lumbar puncture evaluation. Her best corrected visual acuity was 10/10 in both eyes. Anterior segment evaluation was also found to be normal. Examination of the fundus revealed mild swelling and ill-defined boundaries of the optic disc. Visual field analysis did not reveal any defect, including enlargement of the blind spot. The diagnosis of ODD was confirmed by CT and B-scan USG, which yielded a calcified image of the optic nerve head.
A 22-year-old male was referred to our neurology clinic with a diagnosis of papilledema, and then to our department with bilateral disc swelling. His visual acuity and anterior segment examination were unremarkable. The fundus examination revealed bilateral disc swelling. The visual field test and Ichihara color test findings were normal. The CT and B-scan USG were unremarkable except for bilateral calcification of the optic nerve heads. The diagnosis was changed accordingly, previous treatment was stopped, and the patient was discharged.
ODD are yellow, opalescent, hyaline excrescences derived from calcified axonal debris present on the surface of the optic disc or buried within it. They reportedly occur in 0.3-2% of the general population, are bilateral in 70% of cases, and have no sex predilection.1,3 ODD are inherited in an irregular dominant fashion.4 Thus, it may be useful to examine relatives of the patients.
The ophthalmoscopic appearance of ODD depends upon their location within the optic nerve head. They may be buried (usually in young patients)1 or superficial. The diagnosis of ODD is very easy in cases with superficial ODD, but most young children with ODD present with elevated optic discs due to buried drusen.5 Therefore, children and young adults are particularly vulnerable to misdiagnosis, such as papilledema.
Papilledema due to increased intracranial pressure is associated with optic disc hyperemia and a swollen peripapillary retina, which obscures the retinal vessels at the disc margin. The detection of soft exudates and peripapillary hemorrhage is more likely with papilledema. Furthermore, a spontaneous venous pulsation is absent in papilledema. There is often a severe frontal headache and it is occasionally associated with nausea and vomiting. Apart from the difficulties associated with examining young children, accurate imaging and lumbar puncture assessment may require separate anesthetics.
Impairment of visual acuity is rare in ODD, but insignificant visual field defects may occur in up to half of cases.6 The frequency of associated visual field defects is significantly lower for buried ODD identified by USG than for visible ODD.7 Lee and Zimmerman8 reported that the most common visual field defects in ODD are inferior nerve fiber bundle defects, enlargement of the blind spot, and generalized constriction.
USG, CT, fluorescein angiography, and OCT are required for a correct diagnosis of ODD.1,9 However, ODD are generally not calcified in young patients and USG cannot detect them in such cases. Orbital and cranial CT are suitable for excluding the diagnosis of an intracranial mass lesion and possibly to simultaneously detect buried drusen of the optic nerve head at the same time.10 A very recent study has shown that OCT can differentiate papilledema from ODD. Although we performed B-scan USG in all patients with ODD, they still harbored anxiety regarding the possibility of having intracranial pathology. Thus, CT was performed in all patients at the neurology clinic to exclude any intracranial pathology. ODD may be diagnosed incidentally during ophthalmological examinations. In patients without any neurological signs, no further examination or radiologic imaging is required after confirming the diagnosis of ODD with autofluorescence of the optic discs on red-free fundus photography and a hyperechoic region over the optic nerve head on orbital B-scan USG. The clinical differences between papilledema and ODD are listed in Table 1.
While there is no effective treatment for ODD, regular examinations should be carried out in order to rule out accompanying disorders such as elevated intraocular pressure and subretinal neovascularization.1
All three of our patients expressed anxiety regarding the possibility of intracranial pathology. We diagnosed ODD via a fundus examination, autofluorescence of the optic discs, and B-scan USG. We then further confirmed the diagnosis of ODD with CT to assure the patients they did not have any intracranial pathology.
Swelling of the optic discs does not always mean elevated intracranial pressure, and therefore other causes should be kept in mind before coming to a final conclusion based on all relevant clinical findings. Importantly, the early diagnosis of ODD spares the patient unnecessary anxiety about intracranial disease and prevents unnecessary interventions. Misdiagnosis may increase the incidence of somatization of these patients, particularly in the young. The ophthalmologist, neuro-logist, and the reporting radiologist must therefore consider ODD when dealing with atypical cases of disc swelling.
Figures and Tables
Acknowledgements
This study was presented as a poster at the 44th National Congress of Turkish Ophthalmology Society, in Antalya, TURKEY (29 September-03 October 2010).
References
2. Tso MO. Pathology and pathogenesis of drusen of the optic nervehead. Ophthalmology. 1981. 88:1066–1080.

4. Lorentzen SE. Drusen of the optic disk, an irregularly dominant hereditary affection. Acta Ophthalmol (Copenh). 1961. 39:626–643.

5. Boldt HC, Byrne SF, DiBernardo C. Echographic evaluation of optic disc drusen. J Clin Neuroophthalmol. 1991. 11:85–91.
7. Wilkins JM, Pomeranz HD. Visual manifestations of visible and buried optic disc drusen. J Neuroophthalmol. 2004. 24:125–129.

8. Lee AG, Zimmerman MB. The rate of visual field loss in optic nerve head drusen. Am J Ophthalmol. 2005. 139:1062–1066.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download