Abstract
Purpose
Groove pancreatitis is a rare specific form of chronic pancreatitis that extends into the anatomical area between the pancreatic head, the duodenum, and the common bile duct, which are referred to as the groove areas. We present the diagnostic modalities, pathological features and clinical outcomes of a series of symptomatic patients with groove pancreatitis who underwent pancreaticoduodenectomy.
Methods
Six patients undergoing pancreaticoduodenectomy between May 2006 and May 2009 due to a clinical diagnosis of symptomatic groove pancreatitis were retrospectively included in the study.
Results
Five cases were male and one case was female, with a median age at diagnosis of 50 years. Their chief complaints were abdominal pain and vomiting. Abdominal computed tomography, endoscopic ultrasound and endoscopic retrograde cholangiopancreatography were performed. Preoperative diagnosis of all patients was groove pancreatitis. Histological finding was compatible with clinically diagnosed groove pancreatitis in five patients and the pathologic diagnosis of the remaining patient was adenocarcinoma of distal common bile duct. Following pancreaticoduodenectomy, four living patients experienced significant pain alleviation.
Groove pancreatitis is a specific form of chronic pancreatitis that extends into the anatomical area between the pancreatic head, the duodenum, and the common bile duct, which is referred to as the groove areas. In 1973, groove pancreatitis was first used to describe segmental pancreatitis of the groove area [1].
Groove pancreatitis is not common, and only three cases have been published in Korea [2-4]. Because of its rarity, the distinct incidence of groove pancreatitis is unknown, but it accounts for 19.5 to 24.4% of pancreaticoduodenectomy performed to treat chronic pancreatitis [1,5]. Most patients with groove pancreatitis are 40 to 50-year-old males with a history of alcohol abuse [1,5]. The pathogenesis is still unclear but anatomical and functional obstruction of the minor papilla is one of the issues considered.
We present a series of symptomatic patients with groove pancreatitis who underwent pancreaticoduodenectomy, and review the diagnostic imaging modalities, pathological features and clinical outcomes.
Patients undergoing pancreaticoduodenectomy due to a clinical diagnosis of symptomatic groove pancreatitis supported by radiological imaging that included computed tomography (CT), endoscopic ultrasonography (EUS) and endoscopic retrograde cholangiopancreatography (ERCP) were retrospectively included in the study from May 2006 to May 2009. Groove pancreatitis was confirmed histologically in 5 patients, and the final diagnosis of one patient was distal common bile duct cancer. Collected data included demography, clinical presentation, diagnostic imaging work-up, histologic results and clinical outcomes.
Six patients were included in the study. Five cases were male and one case was female, with a median age at diagnosis of 50 years (range, 17 to 68 years). Among these, four patients were heavy alcohol drinkers and smokers. All patients had epigastric or right upper quadrant abdominal pain requiring regular non-opiate analgesia. Severe weight loss (16 kg for 1 month) was detected in one patient. Intermittent nausea and vomiting was featured in 3 patients and gastric outflow obstruction due to duodenal wall thickening and swelling was inspected in these patients during endoscopic examination. Liver function test was within normal range in all 6 patients and none were jaundiced at presentation. Mild hyperamylasemia was detected in 2 patients. Serum carcinoembryonic antigen and CA 19-9 levels were within normal range in all patients.
Six patients underwent a contrast-enhanced CT scan of the abdomen which showed focal low attenuated lesion in groove area. Such specific diagnostic features of groove pancreatitis on CT were present in 5 patients. Cystic lesions in the head of pancreas at the interface with the duodenum were observed in 2 cases and mass-like lesions on the head of pancreas in 3 patients (Fig. 1).
Ectopic pancreatic tissue was suspected on EUS in one patient, but pathologic findings revealed only pancreatic pseudocyst. ERCP didn't show any specific features relating to groove pancreatitis.
Hypoechoic areas at the head of pancreas with loss of duodenal wall layers at the 2nd portion of duodenum was revealed on preoperative performed EUS in the patient with distal bile duct cancer. And the finding by EUS was compatible with CT. Endoscopy and EUS were performed 2 times for biopsy and the pathologic results were chronic inflammation (Fig. 2).
All patients underwent a pancreaticoduodenectomy. One patient, who was a 17-year-old male, underwent a classical Whipple procedure because his duodenal wall was severely inflamed in the operative field and a huge mucosal ulceration of the duodenal bulb was inspected in preoperative endoscopic finding. Two patients expired due to asphyxia and postoperative upper gastrointestinal bleeding; the bleeding focus was not identified by angiography or endoscopy. The postoperative period in the 4 surviving cases was uneventful with a median hospitalization of 20 days (range, 14 to 21 days). After a median follow-up period of 32 months (range, 18 to 53 months), the four living patients have experienced significant pain alleviation and have not required any analgesia. One of the four patients with pain relief has resumed heavy alcohol abuse and pancreatic pseudocyst was identified in his remnant pancreas tail.
Histologic findings of 5 cases were compatible with clinically diagnosed groove pancreatitis. Four cases showed chronic inflammation of the pancreaticoduodenal interface and adjacent duodenal wall and pancreatic head, with extensive scarring and widening of the pancreaticoduodenal groove (Fig. 3), and acute inflammation of groove area and involved duodenum was shown in the 17-year-old male (Fig. 4). In the 68-year-old woman without a history of alcoholism or smoking, histologic analysis revealed surrounding foci of adenocarcinoma of the distal common bile duct. Brunner's gland hyperplasia was seen in one case. Two cases revealed cystic change in the duodenal wall and pancreatic pseudocyst extended into the duodenal wall in one case.
The pathogenesis of groove pancreatitis remains unclear. Anatomical or functional obstruction of the minor papilla is one of the issues considered. It is explained that Brunner gland hyperplasia and stasis of pancreatic juice in the dorsal pancreas leads to pancreatitis in the groove area [1]. And anatomical factors, including a duodenal bud and ectopic pancreas, are other possible reasons for groove pancreatitis [6]. We experienced six patients diagnosed with groove pancreatitis by clinical diagnostic modalities and pathologic examination. Ectopic pancreas in groove area was suspected by EUS but was not confirmed by pathology.
In 3 of the 5 cases (60%), cystic changes in the duodenal wall including one pseudocyst were detected. Thickening and scarring of the duodenal wall close to the minor papilla usually causes stenosis of the second portion of the duodenum. In three cases, gastric outlet obstruction developed due to stenosis of the involved duodenum. Cystic change in the thickened duodenal wall is a characteristic feature and intraduodenal cysts are identified in 49% of patients with groove pancreatitis [5]. Lymphocyte infiltration, fibrosis or scarring in the groove area are also significant [1,7]. In the present study, these histologic features were confirmed in 4 cases except in one case with distal common bile duct cancer.
The clinical manifestations of groove pancreatitis comprise upper abdominal pain, weight loss, postprandial vomiting and nausea due to duodenal stenosis, but jaundice is rare [7-9]. The chief complaint of all cases was epigastric or right upper quadrant abdominal pain in the present study. Clinical complications associated with groove pancreatitis are related to inflammatory changes affecting the duodenal wall. And major gastrointestinal hemorrhage, perforation, chronic debilitating abdominal pain, recurrent pancreatitis, duodenal stenosis, and, albeit a small risk, malignant transformation of ectopic pancreas have been reported [1,8].
Upper endoscopy often shows an inflamed and polypoid duodenal mucosa with stenosis of the duodenal lumen [10]. EUS reveals smooth stenosis of the common bile duct; Santorini's duct is usually undetectable. Duct-penetrating signs are evident in the irregular hypoechoic mass [9]. In our experience, EUS was also effective in diagnosing groove pancreatitis. However, EUS makes insertion impossible due to duodenal stenosis and the accuracy of EUS is dependent on operator and experience. CT scan for groove pancreatitis reveals a hypodense, poorly enhanced mass between the pancreatic head and a thickened duodenal wall. Cystic lesions and a thickened duodenal wall are also useful indicators of groove pancreatitis on dynamic CT images [11]. Endoscopic retrograde cholangiopancreatography reveals tapering of the lower bile duct [9,10]. When the duodenum of patients with groove pancreatitis is too narrow to perform gastrointestinal endoscopy and distinction between groove pancreatitis and pancreatic malignancy is difficult, magnetic resonance cholangiopancreatography is a useful diagnostic option [12].
Clinicians must consider peripancreatic cancer for a differential diagnosis of groove pancreatitis. The appearance of groove pancreatitis may resemble: 1) pancreatic diseases, such as acute pancreatitis; exophytic pancreatic ductal adenocarcinoma; or neoendocrine tumors; 2) bile ducts diseases such as cholangiocarcinoma and choledochal cysts; and 3) duodenal diseases. Other differential diseases include autoimmune pancreatitis and duodenal hamartoma [6]. In our experience, an older female without a history of alcoholism was diagnosed with groove pancreatitis by preoperative imaging studies including CT and EUS. Endoscopic biopsy demonstrated chronic inflammation. However, the final pathologic diagnosis was cholangiocarcinoma of distal common bile duct. Accordingly, careful follow-up of patients with a diagnosis of groove pancreatitis is necessary, because some conditions closely resemble peri-pancreatic carcinoma. And in cases where the diagnosis is in doubt, there are local complications, or when conservative treatment is ineffective, a pancreaticoduodenectomy with histological examination should be performed. In patients with groove pancreatitis, resection is often performed for the diagnosis of a peripancreatic malignancy [13].
Conservative treatments are to stop tobacco/alcohol consumption, recovery of pancreatic function, and analgesics. However, such treatments are only temporarily effective, as a rule [14]. Isayama et al. [15] reported the treatment of groove pancreatitis by endoscopic stenting of the minor papilla, but the long-term clinical course remains obscure.
Surgery is the treatment of choice when symptoms do not improve, or when the condition is too difficult to distinguish from pancreatic carcinoma. In a study by Rahman et al. [16], body weight increased and chronic abdominal pain was relieved in all patients who underwent pancreatoduodenectomy. Complete pain relief was reported in 76% of the patients after pancreatoduodenectomy [17]. There are three cases of 4 living patients who recovered from their pain after successful pancreaticoduodenectomy. The preservation of the pylorus during pancreaticoduodenectomy is not always feasible. We performed the Whipple procedure on one patient. We could not preserve the duodenal bulb and pylorus due to severe inflammation and mucosal erosion of his duodenal bulb. And we experienced two fatal complications including asphyxia and postoperative gastrointestinal bleeding. So, morbidity and mortality of pancreaticoduodenectomy should be considered.
In conclusion, patients with groove pancreatitis have clinical characteristics similar to those of chronic pancreatitis. The diagnostic imaging modalities of choice are computed tomography and endoscopic ultrasonography. And careful follow-up of patients is necessary if groove pancreatitis is suspected, because some conditions closely resemble peri-pancreatic carcinoma. Based on our surgical experience, pancreaticoduodenectomy seems to be a reasonable treatment option in patients with groove pancreatitis.
Figures and Tables
Fig. 1
Computed tomography reveals typical cystic and mass-like lesions in head of pancreas at interface with duodenum.
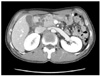
Fig. 2
Computed tomography (A) and endoscopy (B) are compatible with groove pancreatitis, but patient's pathologic diagnosis was distal common bile duct cholangiocarcinoma.
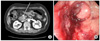
Fig. 3
Gross findings. A specific form of chronic pancreatitis that extended into anatomical area between pancreatic head, duodenum, and common bile duct is shown.

Fig. 4
Acute inflammation of groove area is shown in histologic examination of 17-year-old male (H&E, ×40).
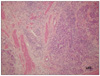
Table 2
Radiological characteristics and histologic findings

CT, computed tomography; EUS, endoscopic ultrasonography; ERCP, endoscopic retrograde cholangiopancreatography.
a)Cystic change, cystic change of duodenal wall. b)Hyperplasia, Brunner gland hyperplasia. c)Mass, low attenuated mass lesion. d)Cyst, cystic mass in pancreas head. e)Thickening, duodenal wall thickening. f)EP, ectopic pancreatic tissue. g)Swelling, mucosal swelling at 2nd portion of duodenum.
References
1. Stolte M, Weiss W, Volkholz H, Rösch W. A special form of segmental pancreatitis: "groove pancreatitis". Hepatogastroenterology. 1982. 29:198–208.
2. Hwang JY, Park KS, Cho KB, Hwang JS, Ahn SH, Park SK, et al. Segmental groove pancreatitis: report of one case. Korean J Intern Med. 2003. 18:234–237.
3. Lee TH, Park SH, Lee CK, Chung IK, Kim SJ. Ectopic opening of the common bile duct accompanied by groove pancreatitis: diagnosis with magnetic resonance cholangiopancreatography. Gastrointest Endosc. 2010. 71:1301–1302.
4. Park KH, Yoo KS, Chung YW, Kim KO, Park CH, Kim JH, et al. A case of groove pancreatitis with a characteristic pathologic feature. Korean J Gastroenterol. 2007. 49:187–191.
5. Becker V, Mischke U. Groove pancreatitis. Int J Pancreatol. 1991. 10:173–182.
6. Zamboni G, Capelli P, Scarpa A, Bogina G, Pesci A, Brunello E, et al. Nonneoplastic mimickers of pancreatic neoplasms. Arch Pathol Lab Med. 2009. 133:439–453.
7. Adsay NV, Zamboni G. Paraduodenal pancreatitis: a clinico-pathologically distinct entity unifying "cystic dystrophy of heterotopic pancreas", "para-duodenal wall cyst", and "groove pancreatitis". Semin Diagn Pathol. 2004. 21:247–254.
8. Shudo R, Obara T, Tanno S, Fujii T, Nishino N, Sagawa M, et al. Segmental groove pancreatitis accompanied by protein plugs in Santorini's duct. J Gastroenterol. 1998. 33:289–294.
9. Balakrishnan V, Chatni S, Radhakrishnan L, Narayanan VA, Nair P. Groove pancreatitis: a case report and review of literature. JOP. 2007. 8:592–597.
10. Mohl W, Hero-Gross R, Feifel G, Kramann B, Püschel W, Menges M, et al. Groove pancreatitis: an important differential diagnosis to malignant stenosis of the duodenum. Dig Dis Sci. 2001. 46:1034–1038.
11. Itoh S, Yamakawa K, Shimamoto K, Endo T, Ishigaki T. CT findings in groove pancreatitis: correlation with histopathological findings. J Comput Assist Tomogr. 1994. 18:911–915.
12. Blasbalg R, Baroni RH, Costa DN, Machado MC. MRI features of groove pancreatitis. AJR Am J Roentgenol. 2007. 189:73–80.
13. Yamaguchi K, Tanaka M. Groove pancreatitis masquerading as pancreatic carcinoma. Am J Surg. 1992. 163:312–316.
14. Levenick JM, Gordon SR, Sutton JE, Suriawinata A, Gardner TB. A comprehensive, case-based review of groove pancreatitis. Pancreas. 2009. 38:e169–e175.
15. Isayama H, Kawabe T, Komatsu Y, Sasahira N, Toda N, Tada M, et al. Successful treatment for groove pancreatitis by endoscopic drainage via the minor papilla. Gastrointest Endosc. 2005. 61:175–178.
16. Rahman SH, Verbeke CS, Gomez D, McMahon MJ, Menon KV. Pancreatico-duodenectomy for complicated groove pancreatitis. HPB (Oxford). 2007. 9:229–234.
17. Casetti L, Bassi C, Salvia R, Butturini G, Graziani R, Falconi M, et al. "Paraduodenal" pancreatitis: results of surgery on 58 consecutives patients from a single institution. World J Surg. 2009. 33:2664–2669.




 Citation
Citation Print
Print



 XML Download
XML Download