Abstract
Objectives
In this systematic review, the effectiveness of herbal medicines in improving depression and anxiety in menopausal women was assessed.
Methods
Three following databases were individually searched: MEDLINE (1966-March 2017), SCOPUS (1990-March 2017), and the Cochrane Library (Cochrane Central Register of Controlled Trials; 2017).
Results
A total of 9 trials were included in this systematic review. Overall, soy was found to have a beneficial effect. Also, fennel had a significant positive effect on menopausal women with depression and anxiety disorder, but not on healthy women. Red clover showed varying effects ranging from significant to non-significant on depression and anxiety. Moreover, kava was found to have a significant beneficial effect on depression and anxiety at dose of 200 mg/days.
Given the increased life expectancy, women often spend a third of their life in the postmenopause era. In Iran, it is estimated that the number of postmenopausal women will reach 5 million in 2021.1 Menopause indicates the termination of a woman's reproductive life. It is defined as the permanent cessation of menstruation induced by the loss of ovarian follicular activity.2 Menopause represents an important stage in female lives, which is often associated with a plethora of complaints and sufferings.3 Mood disturbances, especially anxiety and depression, are commonly associated with menopause.4
The adoption of preventive measures for proper management of menopause can improve the quality of life of women.5
There are growing evidences on the effectiveness of hormone therapy in alleviating menopausal symptoms and other age-related conditions.67 The use of hormone replacement therapy (HRT) was hampered with unexpected findings reported in the Women's Health Initiative (WHI) according to which HRT regimen was associated with increased risk of cardiovascular events and breast cancer.8 Benzodiazepines and antidepressants are commonly used for mood disturbances, but they have proved side effects. For example, benzodiazepines are characterized by drowsiness, prolonged reaction time, and antidepressants are anticholinergic and cardiotoxic effects.4 Given the side effects of HRT, benzodiazepines and anti-depressants, many users have withdrawn from HRT. Instead, many former users of HRT have been attracted to herbal medicine such as soy, hops and red clover as a way of handling menopausal symptoms. This review seeks to investigate the effect of herbal medicines on alleviating the effect of anxiety and depression.
Three databases including MEDLINE (1966-March 2017), SCOPUS (1990-March 2017), and the Cochrane Library (Cochrane Central Register of Controlled Trials; 2017) were individually searched to review trials investigating the effect of herbal medicines on depression and anxiety. Also the same terms put into each database and hand-searching the references of publications were performed to find relevant publications
For this purpose, a number of keywords such as depression AND anxiety, depression OR anxiety, complementary treatments, alternative treatments. evening primrose oil, hypericum perforatum, herbal treatments herbs, St. John's wort, phytomedicine, racemosa rhizome, Salvia officinalis Trigonella foenum-graecum, Avacado plus, Black cohosh, cimicifuga, Evening primrose oil, flaxseed, fenugreek, dong quai, Ginseng, licorice red, Red clover, Vitex agnus-castus, kava, Piascledine and yam were searched. The search was performed without any language restriction.
Randomized controlled trials (RCT) were included in the systematic review if they met the following criteria: 1) including perimenopausal, and postmenopausal women; 2) studying parallel or crossover groups; and 3) including participants with depression or anxiety.
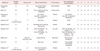
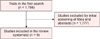
The process of searching and selecting RCTs is shown in Fig. 1. The 1786 studies were found in the first search. 1,777 studies were excluded by initial screening of titles and abstract. 9 final trials were included in this systematic. Characteristics of trials are shown in Table 1.
Balk et al.9 compared the effect of soy flour containing 100 mg isoflavones and wheat cereal as placebo on 19 menopausal women. There was no statistical difference between groups regarding depression symptoms (P = 0.58) at the end of a six-month period. Also, the two groups did not show any improvement compared to the baseline. Kotsopoulos et al.10 examined the effectiveness of soy on menopausal women. They randomized menopausal women in two groups of Soy protein dietary supplements (n = 44) and Casein placebo (n = 50). The score of depression dropped by 25% in soy group but it remained unchanged in placebo group. The score of anxiety dropped by 17% in the soy group and 16% in the placebo group. Statistical analysis by multivariate analysis of covariance (MANOCA) showed no significant differences between groups for psychological symptoms (irritability, depression, anxious, tiredness and sleeplessness). Hanachi and Golkho11 designed a randomized three-group study comparing the efficacy: 1) soymilk supplementation; 2) soymilk supplementation and exercise; and 3) placebo on depression and anxiety. Both groups were not different from placebo group regarding anxiety and depression. The effect on soymilk supplementation and exercise on depression and nervousness was less significant than Soymilk supplementation. To sum up, soy improved slightly anxiety and depression.
A study by Aghamiri et al.12 compared the efficiency of Hops with placebo. Intervention group received 500 mg hop once daily for 12 weeks. The Hops group showed a statistically significant decrease in anxiety compared to the placebo group in three intervals at 2 (P < 0.001), 4 (P < 0.001), 8 (P < 0.001) and 12 (P < 0.001) weeks. The corresponding values for depression were 2 (P < 0.001), 4 (P < 0.001), 8 (P < 0.001) and 12 (P < 0.001) respectively.
In Cagnacci et al. study,4 all patient received 1 g/day of calcium and then were randomized into three groups of control group (no treatment), 100 mg Kava and 200 mg Kava. Mean score of depression dropped from 37.0 ± 1.8 to 34.9 ± 1.7 in the calcium d, from 38.2 ± 2.4 to 33.7 ± 1.4 in Kava-Kava (100 mg) and from 38.7 ± 2 to 33.5 ± 1.9 in Kava (200 mg) groups. The reduction between the baseline and 3-month follow-up was only significant in the group of Kava 200 mg. Comparison of the three groups using ANOVA test did not show any statistically significant difference between groups in terms of depression score. The score anxiety remained unchanged in the calcium group. In 100 mg and 200 mg groups, anxiety score dropped significantly from 47.3 ± 2.2 to 22.5 and from 46.6 ± 1.6 to 41.3 ± 1.6 respectively.
Lipovac et al.13 conducted a double-blind, randomized, crossover study (with a wash-out period of one week) on two groups (red clover and placebo) for 12 weeks. After administering red clover, Hospital Anxiety subscale decreased from (9.98 ± 4.65 to 2.40 ± 2.53) in red clover group and from 9.98 ± 4.65 to 8.05 ± 4.76 (P < 0.001) in placebo group (P < 0.001). Hospital depression subscale decreased from 6.91 ± 4.02 to 1.50 ± 2.06 (P < 0.001) in red clover group and from 6.91 ± 4.02 to 5.23 ± 3.65 (P < 0.001) in placebo group. Zung Self-Rating Depression Scale revealed a significant decrease (P < 0.001 compared to baseline and placebo). Tice et al.14 compared three groups of Promensil (82 mg red clover-derived isoflavones), Rimostil (82 mg red clover-derived isoflavones) and placebo. They did not find any significant improvement in subscale of ‘depression’ either in Promensil (P = 0.23) or Rimostil (0.79) groups compared to the placebo group. The corresponding values for subscale of anxiety were (P = 0.33) and (P = 0.80) respectively. Hidalgo et al.15 conducted a double-blind, randomized, crossover study (with a wash-out period of one week) on two groups of red clover (80 mg) and placebo for 90 days. According to Kupperman index, the subscales of ‘depression’ and ‘nervousness’ revealed a significant improvement in the red clover group compared to the placebo group (both, P = 0.05). Geller et al.16 randomized menopausal women into four groups of black cohosh, red clover, placebo and 0.625 mg conjugated equine estrogens (CEE) plus 2.5 mg medroxyprogesterone acetate (MPA) (CEE/MPA; n = 89). The comparison of two groups in terms of Greene Anxiety Score did not show any significant difference after 12 weeks (P = 0.12); however, at 12 months, significant levels (P = 0.04) were observed. The comparison between Placebo and Black cohosh was non-significant. However, there was a significant improvement in CEE/MPA group compared to placebo at 3 months and 12 months.
This paper was designed to assess the efficacy of herbal medicines on two psychological variables of depression and anxiety. Overall, soy was found to have a beneficial effect on these subscales. The effect of red clover on depression and anxiety varied from significant to non-significant. Kava also had a significant at 100 mg dose, but this effect became significant only at 200 mg dose. According to only one trial, Hops had a positive effect on depression and anxiety.
In their study, Bu and Lephart17 investigated the levels of brain Bcl-2-associated death protein (a proapoptotic member of Bcl-2 protein family) and neuron-specific β-III tubulin (an early marker of neuronal differentiation/survival) in male rats, which were fed with either a standard chow rich of soy isoflavones (Phyto-600) or isoflavones free of soy (Phyto-free) in their entire life (since conception until tissue collection). In the group of rats fed with the Phyto-600 diet, a significant decline in the levels of β-III tubulin was observed in amygdala, frontal cortex, hippocampus and medial basal hypothalamus (MBH) compared to Phyto-free group. In short, the results of this study provided evidences for the neuroprotective power of soy isoflavones in the amygdala, frontal cortex, hippocampus and MBH. This suggests that soy isoflavones can potentially improve learning and memory, behaviors related to anxiety, and recovery from trauma.
Koppula and Kumar18 conducted a study on anti-stress and memory-enhancing features of fennel extract in lab rats. Fennel is a phytoestrogen. The extract was administered orally with an orogastric tube at doses of 50, 100, and 200 mg/kg body weight. The anti-stress activity of rats was assessed based on urinary levels of vanillylmandelic acid (VMA) and ascorbic acid. Daily administration of Foeniculum vulgare (F. vulgare) extract 1 h before the induction of stress had a significant effect (P < 0.05) of alleviating stress-induced urinary biochemical levels of VMA. It should be noted that these changes were in a dose-dependent fashion. As such, F. vulgare could be useful in the management of stress and stress-related disorders.
Future studies can compare the effect of herbal medicines and current treatments such as Fluoxetine. Given the weak methodology of this study, it is recommended that future studies adopt a design based on Consolidated Standards of Reporting Trials (CONSORT) guidelines.
There were several limitations in our study including poor methodology (such as inadequate treatment allocation, small sample size and unclear blinding method), few clinical trials and limited review of relevant studies. Only one study 13 measured depression and anxiety level by specific questionnaire. The rest of studies measured the anxiety and depression symptoms base on menopausal symptom questionnaire. The random sequence generation, Allocation concealment and blinding of outcome assessment was either not performed or not reported in sufficient detail in most of studies. The overall methodological quality was moderate to high.
Figures and Tables
References
1. Direkvand-Moghadam A, Delpisheh A, Montazeri A, Sayehmiri K. Quality of life among Iranian infertile women in postmenopausal period: A cross-sectional study. J Menopausal Med. 2016; 22:108–113.
2. Golshiri P, Akbari M, Abdollahzadeh MR. Age at natural menopause and related factors in Isfahan, Iran. J Menopausal Med. 2016; 22:87–93.
3. Abdi F, Mobedi H, Roozbeh N. Hops for menopausal vasomotor symptoms: Mechanisms of action. J Menopausal Med. 2016; 22:62–64.
4. Cagnacci A, Arangino S, Renzi A, Zanni AL, Malmusi S, Volpe A. Kava-Kava administration reduces anxiety in perimenopausal women. Maturitas. 2003; 44:103–109.
5. Kwak EK, Park HS, Kang NM. Menopause knowledge, attitude, symptom and management among midlife employed women. J Menopausal Med. 2014; 20:118–125.
6. Zweifel JE, O'Brien WH. A meta-analysis of the effect of hormone replacement therapy upon depressed mood. Psychoneuroendocrinology. 1997; 22:189–212.
7. Ghazanfarpour M, Kaviani M, Abdolahian S, Bonakchi H, Najmabadi Khadijeh M, Naghavi M, et al. The relationship between women's attitude towards menopause and menopausal symptoms among postmenopausal women. Gynecol Endocrinol. 2015; 31:860–865.
8. Rossouw JE, Anderson GL, Prentice RL, LaCroix AZ, Kooperberg C, Stefanick ML, et al. Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results from the Women's Health Initiative randomized controlled trial. JAMA. 2002; 288:321–333.
9. Balk JL, Whiteside DA, Naus G, DeFerrari E, Roberts JM. A pilot study of the effects of phytoestrogen supplementation on postmenopausal endometrium. J Soc Gynecol Investig. 2002; 9:238–242.
10. Kotsopoulos D, Dalais FS, Liang YL, McGrath BP, Teede HJ. The effects of soy protein containing phytoestrogens on menopausal symptoms in postmenopausal women. Climacteric. 2000; 3:161–167.
11. Hanachi P, Golkho S. Assessment of soy phytoestrogens and exercise on lipid profiles and menopause symptoms in menopausal women. J Biol Sci. 2008; 8:789–793.
12. Aghamiri V, Mirghafourvand M, Mohammad-Alizadeh-Charandabi S, Nazemiyeh H. The effect of Hop (Humulus lupulus L.) on early menopausal symptoms and hot flashes: A randomized placebo-controlled trial. Complement Ther Clin Pract. 2016; 23:130–135.
13. Lipovac M, Chedraui P, Gruenhut C, Gocan A, Stammelr M, Imhof M. Improvement of postmenopausal depressive and anxiety symptoms after treatment with isoflavones derived from red clover extracts. Maturitas. 2010; 65:258–261.
14. Tice JA, Ettinger B, Ensrud K, Wallace R, Blackwell T, Cummings SR. Phytoestrogen supplements for the treatment of hot flashes: the Isoflavone Clover Extract (ICE) Study: a randomized controlled trial. JAMA. 2003; 290:207–214.
15. Hidalgo LA, Chedraui PA, Morocho N, Ross S, San Miguel G. The effect of red clover isoflavones on menopausal symptoms, lipids and vaginal cytology in menopausal women: a randomized, double-blind, placebo-controlled study. Gynecol Endocrinol. 2005; 21:257–264.
16. Geller SE, Shulman LP, van Breemen RB, Banuvar S, Zhou Y, Epstein G, et al. Safety and efficacy of black cohosh and red clover for the management of vasomotor symptoms: a randomized controlled trial. Menopause. 2009; 16:1156–1166.
17. Bu L, Lephart ED. Soy isoflavones modulate the expression of BAD and neuron-specific beta III tubulin in male rat brain. Neurosci Lett. 2005; 385:153–157.
18. Koppula S, Kumar H. Foeniculum vulgare Mill (Umbelliferae) attenuates stress and improves memory in wister rats. Trop J Pharm Res. 2013; 12:553–558.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download