This article has been
cited by other articles in ScienceCentral.
Abstract
A patient, who underwent partial masseter muscle resection and mandibular angle reduction at a plastic surgery clinic, visited this hospital with major complaints of trismus and dysesthesia. A secondary angle formation due to a wrong surgical method was observed via clinical and radiological examinations, and the patient complained of trismus due to the postoperative scars and muscular atrophy caused by the masseter muscle resection. The need for a masseter muscle resection in square jaw patients must be approached with caution. In addition, surgical techniques must be carefully selected in order to prevent complications, and obtain effective and satisfactory surgery results.
Go to :

Keywords: Masseter muscle resection, Mandibular angle reduction, Trismus, Nerve damage, Secondary angle
I. Introduction
Square jaw refers to an enlarged masseter muscle, along with an increased bony growth in the mandibular angle area. In general, masseter muscle hypertrophy appears and is characterized by sleep bruxism symptoms, etc. In most cases, square jaw is associated with masseter muscle hypertrophy in the Caucasian, while it is associated with mandibular protrusion in the Asian. However, the exact cause is not known
1.
Caucasians generally have dolichocephalic head forms, while Asians have brachycephalic or mesocephalic head forms. The shape of the mandibular angle is important in determining the impression of the face; therefore, the square-shaped face of Asians may cause a negative impact aesthetically. There are two types of square jaw treatment method. First, a botulinum toxin injection or radiofrequency therapy can be performed, which reduces the volume of the masseter muscle. Second, a mandibular angle reduction can be done via an extraoral or intraoral approach, or a cortical bone resection in cases where the mandibular width is wide or the mandibular angle area protrudes outward. Complications include excessive bleeding due to negligence during the surgery, overcorrection or undercorrection, asymmetry, infection, mandibular condylar fracture, inferior alveolar nerve injury and trismus
12.
The aims of this case report were to describe a patient who experienced trismus, dysesthesia and a newly formed secondary angle after receiving bilateral mandibular angle reduction and partial masseter muscle resection for square jaw in a plastic surgery clinic. This study analyzed complications that appeared after mandibular angle reduction and masseter muscle resection, and considered the methods needed to resolve and prevent them.
Go to :

II. Case Report
A 20-year-old male patient visited the Department of Oral and Maxillofacial Surgery at SMG-SNU Boramae Medical Center (Seoul, Korea) with major complaints of bilateral mandibular angle trismus and dysesthesia after having undergone surgery. The patient received bilateral mandibular angle reduction and partial masseter muscle resection via a pre-auricular approach at a plastic surgery clinic approximately 10 months previously, but did not receive additional treatment during the postoperative recovering period.
The patient did not have a history of systemic disease, and clinical and radiological diagnostic examinations were performed. Upon palpation, he complained of dysesthesia in the bilateral mandibular area with a maximum mouth opening of 11 mm, based on the edge of maxillary and mandibular central incisors, thereby showing severe trismus symptoms. The patient also experienced mastication problems due to this. (
Fig. 1) For the radiological examination, routine panoramic and temporomandibular joint panoramic radiographs were taken. The radiographic images showed that the bilateral mandibular angle area and inferior margin were resected very close to the mandibular canal, and the secondary angle was formed in the resected anterior and posterior margins.(
Fig. 2. A) In addition, it was observed that only a rotational movement occurred without translation in the bilateral mandibular condyle upon opening the mouth.(
Fig. 2. B)
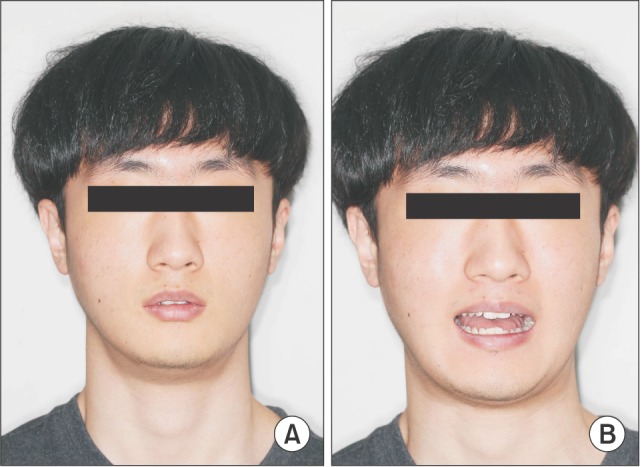 | Fig. 1Patient's clinical facial images. A. Rest position. B. The length of maximum mouth opening was 11 mm.
|
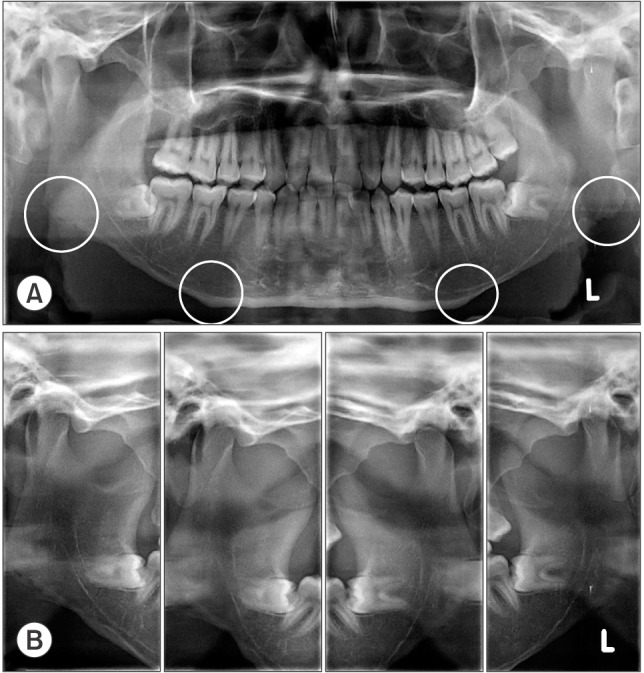 | Fig. 2Radiographic images of the patient. A. Panoramic view (bilateral mandibular angle resection; the resected mandibular inferior margin is very close to the inferior margin of the inferior alveolar nerve canal; the formation of secondary angle at the resected anterior and posterior border is seen). B. Temporomandibular joint panoramic view showed only rotational movement of the mandibular condyle without translation during mouth opening.
|
Despite these postoperative complications, the plastic surgery clinic that conducted the surgery did not perform any treatment to improve the patient's trismus and dysesthesia signs and symptoms, which became more severe over time after the surgery.
In this hospital, physical therapy (transcutaneous electrical nerve stimulation, heat therapy, and ultrasound physical therapy) and mouth opening exercises combined with botulinum toxin injection therapy were planned in order to improve the patient's trismus. If the improvement effect is minimal, increasing the mouth opening via scar revision will be taken into consideration. In case of further need, bilateral coronoidotomy and masseter muscle stripping may be performed. In addition, conservative treatment for his sensory disturbance is planned including muscle physical therapy or the administration of antidepressants.
The written informed consent was obtained from the patient.
Go to :

III. Discussion
Square jaw surgery methods include extraoral and intraoral approaches. In this case, the patient was treated with partial masseter muscle resection and mandibular angle reduction simultaneously via a pre-auricular approach. The extraoral approach has advantages in that it provides a good field of view and carries a small risk of infection; however, its shortcomings include scar formation, and high risks for facial nerve injury.
The need for a masseter muscle resection in square jaw patients must be carefully approached because the reason for square jaw in Asians is bony growth, and not muscle hypertrophy, in most cases. Moreover, postoperative swelling caused by bleeding within the muscle, muscle atrophy, and scar formation due to the masseter muscle resection may result in short-term or long-term trismus. Furthermore, masseter muscle resection may cause facial nerve injury, which is less predictable, as compared to mandibular angle ostectomy
3. According to a survey that was conducted on 40 plastic surgeons in 2006, 55% did not conduct masseter muscle resection during a mandibular angle ostectomy, and 45% conducted masseter muscle resection and mandibular angle ostectomy for certain cases
4. In this case, since masseter muscle resection was performed along with mandibular angle ostectomy, trismus occurred due to severe atrophy of the masseter muscle and scar tissue formation. Around 22% of masseter muscle reductions occur without special complications after a mandibular angle ostectomy. In the case of severe masseter muscle hypertrophy that requires a masseter muscle resection
5, the masseter muscle can be reduced with an additional botulinum toxin injection. Even in cases of square jaw symptoms due to masseter muscle hypertrophy after a mandibular angle ostectomy, it is questionable to consider masseter muscle resection as a primary treatment.
After surgery in the oral and maxillofacial area, trismus and sensory disturbance can occur often. But there are few reports about complications related to trismus and nerve injury after mandibular angle surgery combined with masseter muscle resection. This is why there is still no consensus on the efficacy of masseter muscle resection. Also, masseter muscle resection is limitedly performed in severe cases of masseter muscle hypertrophy
6. If necessary, minimal resection of the masseter muscle in the deep portion and an intraoral approach may prevent major complications including trismus and nerve injury. Yoshida reported injecting botulinum toxin, coronoidotomy and masseter muscle stripping for oromandibular dystonia patient-related limited mouth opening were effective
7. Daily muscle physical therapy or the administration of antidepressants can also be effective therapies for dysesthesia patients
8.
In this case, clinical examination and radiography showed a secondary angle formation in the mandible. The secondary angle was a newly formed angle between the resection line and the mandibular inferior border. In such cases, the dissatisfaction of patients becomes more evident and revision surgery is sometimes conducted. Such a phenomenon occurs when the mandibular angle area is resected in a straight line without considering the mandibular contour; however, this can be prevented using a careful curve resection or mandibular outer cortical bone resection
2.
For square jaw surgery, the approach or surgical technique must be carefully selected in order to obtain effective and satisfactory results. In order to prevent the problems seen in this case, the anatomical structures around the jaw must be sufficiently understood, and preventive methods and solutions must be identified for any complications that may occur. After surgery-related problems occur, the advice of a surgical technique specialist who can provide the patient with a proper treatment, must be obtained as early as possible in order to fix major complications.
Go to :







 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download