Abstract
Bilateral coronoid process hyperplasia is a rare condition characterized by an enlarged mandibular coronoid process. The painless progressive reduction of a mouth opening is caused by coronoid process impingement on the posterior aspect of the zygomatic bone. Hyperplasia of the bilateral coronoid process leads to the restriction of a mandibular opening consequent to the impingement of the enlarged coronoid process on the temporal surface of the zygomatic bone or with the medial surface of the zygomatic arch. The process has been diagnosed as developmental hyperplasia. Otherwise, the development of the coronoid process may be associated with growth hormone. This paper describes a case of trismus caused by coronoid hyperplasia in an idiopathic short-stature patient who received growth hormone therapy by somatropin injections.
Bilateral Coronoid Process Hyperplasia is a rare condition characterized by an enlarged mandibular coronoid process. Continuously proliferating coronoid process causes trismus due to impingement on the temporal surface of the zygomatic bone or the medial surface of the zygomatic arch. According to Isberg et al.1, coronoid process hyperplasia is the cause of approximately 5% of trismus patients. Many hypotheses suggest stimulating endocrine, increased activity of temporal muscle, injury, and heredity as the possible factors contributing to coronoid process hyperplasia, but the cause has yet to be identified clearly2.
The most common clinical feature of coronoid process hyper plasia is painless and progressive trismus. Unilateral coro noid process hyperplasia is commonly combined with facial asymmetry and sometimes combined with mobile uplift on the upper part of the zygomatic arch and mandibular displace ment toward the affected side during mouth opening. Unilateral and bilateral coronoid process hyperplasia may occur in all age groups (average 25) but rarely in people aged 10 or under. Moreover, most patients were male, but female patients were rare.
As a treatment method, coronoidectomy can achieve meaningful enhancement of mouth opening, but there is a need to check for fibrosis caused by surgery or regrowth of coronoid process for a long time2.
This case report deals with a patient diagnosed with idiopathic short stature (ISS) in 2008 by the Department of Pediatrics and administered growth hormone therapy and whose trismus-caused by bilateral coronoid process hyperplasia-was treated with coronoidectomy.
On April 4, 2006, a 12-year-old male patient visited the Department of Pediatric Dentistry and Orthodontics, Pusan National University Hospital Korea due to the delayed eruption of permanent teeth and facial asymmetry. The patient weighed 34 kg, and he was 135 cm tall; he was relatively small compared with other children in his age, and many of his teeth had birth defects. The patient had received treatment at the Department of Pediatric Dentistry and Orthodontics without trismus; in August 2008 when he was 14, he was referred to Department of Oral and Maxillofacial Surgery by the Department of Orthodontics due to facial asymmetry and trismus. Clinical examinations revealed facial asymmetry, mouth opening level of 15 mm, and displacement to the left of the mandible during mouth opening; the panoramic photographs showed left coronoid process hyperplasia. The patient did not have any particular injury or infection or family history of similar symptoms, but he was diagnosed with ISS in January 2008 by the Department of Pediatrics in our hospital and administered growth hormone therapy using Eutropin (Recombinant Human Growth Hormone [somatropin], LG Eutropin Inj.; LG Life Sciences, Seoul, Korea) injection. Our Department planned to encourage active mouth opening movement, observe his status during the growth period, and perform surgery, but the patient did not visit again. Later, the patient visited again in July 2011 when he was 17 due to restriction of mouth opening. Clinical examinations revealed facial asymmetry, displacement to the left of the mandible during mouth opening, and maximum mouth opening level of 10 mm, decreasing compared to 2008.(Fig. 1) Moreover, he had a hard-end-feel on both sides when opening his mouth to the left and right. The panoramic radiographic inspection and dental cone-beam computed tomography (CT) (Pax-Zenith 3D; Vatech, Hwaseong, Korea) images showed hyperplasia on both sides of the mandi bular coronoid process.(Fig. 2) In particular, the three dimensional (3D) images obtained by reorganizing the dental cone-beam CT images with 3D analysis program (Simplant; Materialise, Leuven, Belgium) revealed that the left coronoid process was close to the medial surface of the left zygomatic bone, and that the inner side of the left zygomatic bone was transformed.(Fig. 3) The patient's height increased from 143 cm in January 2008 when the growth hormone therapy was started to 153 cm when the patient visited us in August 2008 due to trismus. And in comparing panoramic radiographs, the panoramic images taken in August 2008 showed a more noticeable hyperplasia in the left coronoid process.(Fig. 4) The patient kept receiving growth hormone therapy until October 2009, and his height increased from 153 cm to 167 cm in July 2011. The maximum mouth opening level decreased from 15 mm in August 2008 to 10 mm in July 2011.(Table 1)
Therefore, based on the patient's medical history, clinical examinations, and radiographic inspection, we determined that the growth hormone therapy caused hyperplasia in the bilateral mandibular coronoid process and diagnosed the transformation of the left coronoid process and impingement on the inner side of the zygomatic bone as the cause of trismus. As such, we planned to perform coronoidectomy on both sides of the mandible under general anesthesia in August 2011.
General anesthesia was performed with nasotracheal intubation using fiber optic scope because it was hard to execute nasotracheal intubation using head scope due to the insufficient mouth opening level. Considering the diagnostic process, left coronoidectomy was carried out first due to the hard-end-feeling and transformation of coronoid process. At first, left coronoidectomy was performed through the mouth; however, due to insufficient mouth opening level, the submandibular approach was taken. After the surgery, the maximum mouth opening level increased by 37 mm. Afterward, right coronoidectomy was done through the intraoral approach. After the surgery, the maximum mouth opening level increased by 53 mm.(Fig. 5) Extracted left coronoid process had hyperplasia horizontally; cartilage proliferating 2 mm thick was noted at the end. Extracted right coronoid process was not transformed, but it had overall hyperplasia.(Fig. 6)
One month after the surgery when the patient visited again, the maximum voluntary mouth opening level was 40 mm without edema, pain, and neural damage.(Fig. 7)
Generally, trismus means all problems in mouth opening. The normal mouth opening level is 40-60 mm, based on the distance between the maxillary and mandibular teeth3. A clinical method involves measuring finger breadth (FB, breadth of index finger's nail), generally 17-19 mm. The normal value is 2FB or 3FB4.
For the reason and classification of trismus, many researchers proposed various hypotheses5-7. Therefore, when a trismus patient visits, there is a need to perform diagnosis based on clinical opinions and diagnostic radiographic inspections considering possible reasons such as temporomandibular joint disorder, temporomandibular joint ankylosis, benign tumor, malignant tumor, dental infection, maxillo facial fracture, and other diseases.
When the patient in this case visited us, though the panoramic radiography inspection revealed hyperplasia of the left coronoid process and calcification of bilateral stylohyoid liga ment, the clinical examinations did not find any feeling of irri tation, throat discomfort, and odynophagia during mouth opening; only a hard feeling was noted. Therefore, we found that the calcified stylohyoid ligament does not influence mouth opening; with an additional dental cone-beam CT examination, the patient was diagnosed with trismus caused by the overgrowth of the left coronoid process and transformation of the left zygomatic bone.
When the patient visited us for the first time in August 2008 due to trismus, he was diagnosed with ISS; he had been administered growth hormone therapy since January 2008 using Eutropin (Eutropin, recombinant methionyl-hGH) injection (Somatropin). In particular, he had been treated by the Department of Orthodontics until August 2007, but there was no symptom of trismus. After the patient received growth hormone therapy, the deterioration of hyperplasia in the left coronoid process and generation of trismus were observed in the panoramic radiographic images.
Idiopathic short-stature patients have short stature (below -2.0 standard deviation compared to the average stature of children of the same age and sex8); though their blood growth hormone concentration is higher than the standard of growth hormone deficiency, their stature is similar to that of children with growth hormone deficiency9. Such is caused by the insuffi cient secretion of growth hormone, decrease of sensitivity to growth hormone, or combination of both factors.
Spiegel et al.10, Kjellberg et al.11, and van Erum et al.12 reported that, based on the cephalometric analysis of boys with short stature, not only height but the growth and development of face were influenced by growth delay; they had small, flat basis cranii and mandible located in the posterior area. On the other hand, Isaksoon et al.13 reported that the growth hormone stimulates overall bones and muscles particularly the growth of cartilage through the insulin-like growth factor I (IGF-I). Pirinen et al.14 also stated that the growth of basis cranium and mandibular cartilage is affected by both excess and insufficiency of the growth hormone. Considering these research studies, insufficient vertical growth in the mandibular condyle and posterior skull base in charge of cartilage growth causes small mandible and short posterior facial height, eruption of dentition increase, lower facial height, and mandible rotated clockwise; hence the unique craniofacial shape of short-stature patients. The patient in this case also had the facial shape of short-stature patients.
A growth hormone agent (Somatropin) means a synthetic human growth hormone. Since 1958 when Raben15 injected a human growth hormone extracted from the pituitary gland of a cadaver into a patient with growth hormone deficiency for the first time and reported its effects, it has been used for 40 years. The growth hormone stimulates the growth of bones and muscles as well as the composition of IGF-I in liver. Therefore, the injection of growth hormone can resolve the problem of insufficient hormone as well as low sensitivity to growth hormone, thereby increasing the final height by stimulating growth during childhood and triggering the growth of spheno-occipital synchondrosis in basis cranii and mandibular condyle. Actually, Chung et al.16 reported that 2 years of growth hormone therapy for children with short stature led to the increase of posterior facial height and growth of the mandible.
Though there is no other case report on the relationship between the growth of the mandibular coronoid process and growth hormone as well as consequent complications such as trismus, this case report concluded that the coronoid process originating with cartilage may have hyperplasia of the mandibular coronoid process due to the growth hormone agent and contraction of temporal muscle. Nonetheless, more research on the evident reason is needed to identify the mechanism of coronoid process hyperplasia.
Figures and Tables
Fig. 1
Preoperative clinical photograph. A. Lateral photo view. B. Frontal photoview. C. Preoperaive maximum mouth opening mesurement was 10 mm.
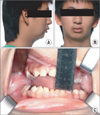
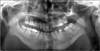
Fig. 2
Preoperative radiologic view show both hyperplasic coronoid preocess. A. Panoramic view. B. Dental conbeam computed tomography (CT) view (mandible right). C. Dental conbeam CT view (mandible left).
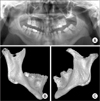
Fig. 3
Three dimensional simplant image. A. The image show morphological abnomality of left zygomatic bone. B. Left coronoid process extend above the zygomatic bone and impinge on the posterior surface of the zygomatic bone. C. Right coronoid process have just hyperplastic morphology.
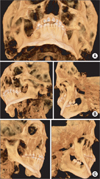
Fig. 4
Serial panoramic view. A. April 2006. B. August 2007. C. August 2008 after growth hormone therapy (January 2008). D. July 2011.

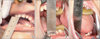
Fig. 5
A. Perioperative mouth opening was 10 mm. B. Mouth opening after left coronoidectomy was 40 mm. C. Mouth opening after both coronoidectomy was 53 mm.
References
1. Isberg A, Isacsson G, Nah KS. Mandibular coronoid process locking: a prospective study of frequency and association with internal derangement of the temporomandibular joint. Oral Surg Oral Med Oral Pathol. 1987. 63:275–279.

2. McLoughlin PM, Hopper C, Bowley NB. Hyperplasia of the mandibular coronoid process: an analysis of 31 cases and a review of the literature. J Oral Maxillofac Surg. 1995. 53:250–255.
3. Kang HJ, Hwang DS, Kim YD, Shin SH, Kim UK, Kim JR, et al. Clinical study on the etiology, differential diagnosis and treatment of trismus. J Korean Assoc Oral Maxillofac Surg. 2006. 32:544–558.
4. Nelson SJ, Nowlin TP, Boeselt B. Consideration of linear and angular values of maximum mandibular opening. Compendium. 1992. 13:362. 364. 366.
5. Luyk NH, Steinberg B. Aetiology and diagnosis of clinically evident jaw trismus. Aust Dent J. 1990. 35:523–529.

6. Marien M Jr. Trismus: causes, differential diagnosis, and treatment. Gen Dent. 1997. 45:350–355.
7. Okeson JP. Orofacial pain: guidelines for assessment, diagnosis, and management. 1996. 3rd ed. Chicago: Quintessence Publishing;45–52.
8. Cohen P, Rogol AD, Deal CL, Saenger P, Reiter EO, Ross JL, et al. 2007 ISS Consensus Workshop participants. 2007 ISS Consensus statement on the diagnosis and treatment of children with idiopathic short stature: a summary of the Growth Hormone Research Society, the Lawson Wilkins Pediatric Endocrine Society, and the European Society for Paediatric Endocrinology Workshop. J Clin Endocrinol Metab. 2008. 93:4210–4217.

9. Hintz RL, Attie KM, Baptista J, Roche A. Genentech Collaborative Group. Effect of growth hormone treatment on adult height of children with idiopathic short stature. N Engl J Med. 1999. 340:502–507.

10. Spiegel RN, Sather AH, Hayles AB. Cephalometric study of children with various endocrine diseases. Am J Orthod. 1971. 59:362–375.

11. Kjellberg H, Beiring M, Albertsson Wikland K. Craniofacial morphology, dental occlusion, tooth eruption, and dental maturity in boys of short stature with or without growth hormone deficiency. Eur J Oral Sci. 2000. 108:359–367.

12. van Erum R, Mulier M, Carels C, Verbeke G, de Zegher F. Craniofacial growth in short children born small for gestational age: effect of growth hormone treatment. J Dent Res. 1997. 76:1579–1586.

13. Isaksson OG, Lindahl A, Nilsson A, Isgaard J. Mechanism of the stimulatory effect of growth hormone on longitudinal bone growth. Endocr Rev. 1987. 8:426–438.

14. Pirinen S, Majurin A, Lenko HL, Koski K. Craniofacial features in patients with deficient and excessive growth hormone. J Craniofac Genet Dev Biol. 1994. 14:144–152.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download