Abstract
A number of reports regarding atypical fractures of the femur have raised questions concerning the possible correlation between long-term bisphosphonate treatment and the occurrence of insufficiency fractures in the proximal femur. However, clinically, it is often confused whether is it a fatigue fracture because of implant induced stress concentration or a bisphosphonate-related atypical fracture, especially in a patient with a subtrochanteric fracture who receive bisphosphonate therapy after open reduction and internal fixation, such as dynamic hip screw (DHS) fixation for previous ipsilateral femoral neck or intertrochanteric fracture. The authors experienced a case of a progressive femoral insufficiency fracture in a woman who had been on Fosamax (Alendronic acid with Vitamin D; Merck & Co. Inc, NJ, USA) therapy for four years after ipsilateral femoral neck fracture treated with a two hole DHS system. Despite a high suspicion of an insufficiency femoral subtrochanteric fracture by bone scan, the occult fracture progressed to a displaced femoral subtrochanteric fracture one year after. The fracture site was fixed with a 6 hole DHS plate, and six months after reoperation the patient had no symptoms and the fracture site had united without any complication.
Although bisphosphonate, a potent inhibitor of bone resorption, is generally safe and effective, it carries the potential risk of over-suppressing bone turnover. Therefore, bisphosphonate therapy can potentially impair some of the biomechanical properties of bone.[1] A number of reports have been issued regarding insufficiency femoral fractures in patients on long-term bisphosphonate therapy,[2,3] and recently several studies have reported suspicious relationship between atypical femoral fractures and long-term bisphosphonate medication.[2,3]
However, it is often confused clinically whether is it a fatigue fracture because of implant induced stress concentration or a bisphosphonate-related atypical fracture, especially in a patient with a subtrochanteric fracture who receive bisphosphonate therapy after open reduction and internal fixation, such as dynamic hip screw (DHS) system for previous ipsilateral femoral neck or intertrochanteric fracture.
In this report, we present a case of progressive femoral insufficiency fracture or stress fracture in a woman on long-term alendronate therapy who had had an ipsilateral femoral neck fracture treated using a DHS.
A 76-year old woman visited our out-patient clinic in May 2010 complaining of a left thigh pain while walking. Medical history taking revealed a diagnosis of a left femur neck fracture fixed with a DHS in July 2006, and in January 2010, she had undergone surgery due to a right distal radius and ulnar fracture and a right femoral intertrochanteric fracture. She had been treated with 70 mg alendronate per week since 2006. A physical examination revealed no limitation of range of motion of the left hip joint, and a radiologic evaluation, including a computed tomography scan, showed no suspicious lesion, such as, hypertrophied cortical bone or a fracture line on the left proximal femoral shaft area. However, a bone scan showed increased uptake in the proximal femoral area just below the fixed plate (Fig. 1). The average T-score of bone mineral density was -3.9 for lumber spine. She was managed conservative treatment using analgesics, and the anti-osteoporosis medication was continued.
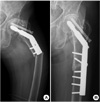
In June 2011, she was transferred from a local hospital due to left thigh pain. The pain started after rising from a sitting position without any trauma history. Pelvic plain anteroposterior radiography revealed a displaced subtrochanteric fracture at the left femur. The fracture site was located at the contact margin at the end of the plate. The characteristics of fracture were cortical hypertrophy, medical spike, and a transverse fracture line, which are features commonly associated with atypical femoral subtrochanteric fracture. On the other hand, the fracture line is just distal to the DHS plate where the maximal stress is concentrated which is a definite feature commonly presented at stress related fatigue fracture. The fracture was fixed by replacing the 2 hole DHS plate with a with a 6 hole plate. Alendronate was stopped after reoperation, and six months after the reoperation the patient was asymptomatic and the fracture had united without any complication (Fig. 2).
The above case report is limited in a specific situation that anti-resorptive medication such as bisphosphonate is prescribed for osteoporosis-related fracture after open reduction and internal fixation, but clinically not unusual. Newly developed isiplateral subtrochanteric fractures in such patients could be induced not only previously fixated hardware but also anti-resorptive medication. Both fatigue fracture due to stress concentration and bisphosphonate related insufficiency or atypical femoral fracture has similar feature of slowly progression.
Many authors have recommended that fatigue or insufficiency femoral fractures be treated by preventive internal fixation, because it is difficult to fix fracture sites.[4-6] Therefore, the early diagnosis of undisplaced occult fracture is important in terms of starting appropriate treatment. McKiernan et al.[7] concluded that a longer dual-energy X-ray absorptiometry femoral scan might be helpful for detecting atypical subtrochanteric femur fractures based on the idea that the femoral scan field would depict hypertrophied femoral cortex or a transverse fracture line. However, in our case, plain radiography and computed tomography showed no structural abnormality. Only a bone scan detected the fracture prior to cortical bone change in the proximal femur. We were not able to perform magnetic resonance imaging due to the presence of the metal implant.
In this case, the fracture initiated at just distal to the plate of DHS system. Biomechanically, weight stress concentrates on the most distal margin of a plate after internal fixation. We consider that in our case, over-suppression of bone turnover interfered with normal bone healing after microfracture induced by stress concentration. To our knowledge, this is the first study to report on the development of an insufficiency or stress-induced fatigue femoral fracture and to describe the effectiveness of bone scan as early diagnostic modality.
In retrospect, the bisphosphonate should have been stopped after we detected the insufficiency femoral fracture. Puah and Tan[8] reported that a bisphosphonate-associated atypical fracture of the femur spontaneous heal after drug suspension and re-appeared after resumption. Unfortunately, we did not recognize the possible affect of bisphosphonate at the time.
Most studies that have addressed insufficiency femoral fractures have recommended that physicians should check plain femoral radiographs when patients with a history of long-term bisphosphonate medication complain of persistent thigh pain.[3] It is also recommended for cases with suspicious fatigue fracture. We would add that a bone scan be added for early detection purposes when no structural bone abnormality is detected by plain radiography. In these situation, preventive internal fixation before development of displaced femoral fracture could be a beneficial.
Figures and Tables
References
1. Odvina CV, Zerwekh JE, Rao DS, et al. Severely suppressed bone turnover: a potential complication of alendronate therapy. J Clin Endocrinol Metab. 2005. 90:1294–1301.

2. Goh SK, Yang KY, Koh JS, et al. Subtrochanteric insufficiency fractures in patients on alendronate therapy: a caution. J Bone Joint Surg Br. 2007. 89:349–353.
3. Kwek EB, Goh SK, Koh JS, et al. An emerging pattern of subtrochanteric stress fractures: a long-term complication of alendronate therapy? Injury. 2008. 39:224–231.

4. Capeci CM, Tejwani NC. Bilateral low-energy simultaneous or sequential femoral fractures in patients on long-term alendronate therapy. J Bone Joint Surg Am. 2009. 91:2556–2561.

5. Ha YC, Cho MR, Park KH, et al. Is surgery necessary for femoral insufficiency fractures after long-term bisphosphonate therapy? Clin Orthop Relat Res. 2010. 468:3393–3398.

6. Visekruna M, Wilson D, McKiernan FE. Severely suppressed bone turnover and atypical skeletal fragility. J Clin Endocrinol Metab. 2008. 93:2948–2952.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download