Abstract
Purpose
This study was performed to determine the relative frequency of positioning errors, to identify those errors directly responsible for diagnostically inadequate images, and to assess the quality of panoramic radiographs in a sample of records collected from a dental college.
Materials and Methods
This study consisted of 1,782 panoramic radiographs obtained from the Department of Oral and Maxillofacial Radiology. The positioning errors of the radiographs were assessed and categorized into nine groups: the chin tipped high, chin tipped low, a slumped position, the patient positioned forward, the patient positioned backward, failure to position the tongue against the palate, patient movement during exposure, the head tilted, and the head turned to one side. The quality of the radiographs was further judged as being 'excellent', 'diagnostically acceptable', or 'unacceptable'.
Results
Out of 1,782 radiographs, 196 (11%) were error free and 1,586 (89%) were present with positioning errors. The most common error observed was the failure to position the tongue against the palate (55.7%) and the least commonly experienced error was patient movement during exposure (1.6%). Only 11% of the radiographs were excellent, 64.1% were diagnostically acceptable, and 24.9% were unacceptable.
Fundamental to the practise of radiation protection is the production of a radiograph of high diagnostic quality with significance to treatment while exposing the patient to the lowest practicable dose.1 However, it has been shown that a considerable number of radiographs exposed in dentistry are of marginal or non-diagnostic quality.2-8 The value of a panoramic radiograph is reduced when it is of poor diagnostic quality.9 Low quality radiographs can lead to misinterpretation, resulting in incorrect diagnosis and treatment planning.10
A non-diagnostic quality image often requires a need for supplementary images and a repetition of examinations.1,11 This repetition of panoramic radiography carries an associated risk of inducing cancer which has been estimated as 0.21 or 1.9 cases per million examinations.12,13
A non-diagnostic quality image which leads to repetition is not a result of an inherent limitation of the equipment but rather is a result of errors made by the operator during patient positioning and processing of the image.7,9,14,15 Compared with intraoral radiography, panoramic radiography poses particular challenges in both of these aspects of image production.9 Processing errors can be eliminated by the use of digital processing, which has recently been increasing in popularity among dentists. However, the appropriate positioning and preparation of the patient is essential for a sharp, accurate, and undistorted image, which is not affected by ghost images.2,7,9 Furthermore, panoramic radiographs may contain radiopaque and radiolucent spots that are reflections of various structures on the examined areas as well as shadows of soft tissues and anatomical air spaces making patient positioning even more important.9,16 Inaccuracies in patient positioning lead to discrepancies between horizontal and vertical magnification, with consequent distortion of the image.17
The aim of this study was to assess the quality of panoramic radiographs and to evaluate common positioning errors in order to prevent further occurrence in radiology departments.
This study was carried out on 1,782 panoramic radiographs that were taken from January 2007 to March 2010 in the Department of Oral and Maxillofacial Radiology. All the radiographs were of patients referred from various departments of the dental college for clinical and diagnostic purposes. The radiographs of paediatric patients less than 18 years of age and edentulous patients were excluded from this study.
All projections were made with the same radiographic equipment (Strato 2000D, Villa Sistemi Medicali, Milan, Italy), operating at 50-80 kVp and 4-10 mA according to the manufacturer's instructions. The exposure time was 15 seconds with a magnification factor of 1.23. All radiographs were taken by 2 qualified radiographers with more than 3 years of experience. The radiographs were viewed under identical conditions without any modifications, on a 15-inch, 1280×800 resolution, 32 bit color mode computer monitor (Dell Inc, Round Rock, TX, USA), in a room with subdued lighting.
The digital radiographs were evaluated by a professor of oral and maxillofacial radiology with more than 12 years of experience. The observer evaluated all the images once, and a randomly selected sub-sample (comprising 25% images i.e. 446 images) after 3 months' time had elapsed, for the second time. The frequency of positioning errors was recorded. The assessed errors included the chin tipped high, the chin tipped low, a slumped position, the patient positioned forward, the patient positioned backward, failure to position the tongue against the palate, patient movement during exposure, the head tilted, and the head turned to one side (Figs. 1-9). The criteria for including a radiograph in a particular positioning error group are given in Table 1.
As the images were viewed on the monitor, processing and handling artifacts did not need to be taken into consideration. In the end, the observer deemed the diagnostic acceptability of each radiograph to be 'excellent', 'diagnostically acceptable', or 'unacceptable' according to previously published guidelines.12 The term 'excellent' was applicable where there were no errors of positioning. In any case where the observers were unable to reach a consensus, the radiograph was scored as 'diagnostically acceptable'. In cases in which the radiograph was found to be non-diagnostic and required repetition, it was categorized as diagnostically unacceptable. The repeated images were not included in the study. In case multiple panoramic images were taken for a patient, only the first image was included in the study.
Data tabulation and analysis was processed using SPSS 15.0 software (SPSS Inc., Chicago. IL., USA). Repeatability was calculated both in terms of percentage agreement and by calculation of the kappa (k) statistic.18 Intra-examiner variability was assessed according to Altman19 where poor was k<0.21, fair was k=0.21-0.40, moderate was k=0.40-0.60, and good was k>0.60.
Out of the 1,782 panoramic radiographs viewed, 196 (11.0%) radiographs had no errors while 1,586 (89.0%) radiographs showed one or more positioning error. The most common positioning error observed in the radiographs was failure to position the tongue against the palate (993, 55.7%) whereas the least common error recorded was patient movement during exposure (28, 1.6%). Table 2 shows the frequency distribution of common errors observed in the sample studied.
Only 196 (11.0%) of the radiographs were free of positioning errors and therefore classifiable as 'excellent' using the recommended criteria. 1,142 (64.1%) were 'diagnostically acceptable', containing errors which did not detract from the diagnostic utility of the radiograph. The remaining 444 (24.9%) were 'unacceptable' (Table 3).
The overall kappa statistic for intra-examiner reliability for positioning errors was 0.77, the proportional agreement being 92% and for quality assessment was 0.63, the proportional agreement being 83%. Overall, the intra-examiner agreement was found to be good.
The images evaluated in the present study were gathered from inactive patient files from the Department of Oral and Maxillofacial Radiology of a dental college for the purpose of assessing positioning errors and quality in panoramic radiography. Since the subjects whose images were assessed were randomly selected, and the dentists, at the time when the radiographs were taken, were unaware of this study, the sample may be regarded as representative of everyday radiograph quality.
In our study, processing and handling errors were not considered since the radiographs were taken from a digital panoramic machine with digital printing. The study was conducted on the digital images directly viewed on a monitor, as in the present scenario most of the dental radiologists have started using digital machines despite the availability of manual machines.
This study only included images of adult patients over 18 years of age. A greater incidence of certain positioning errors might be expected with children, but no study appears to have been carried out comparing panoramic film quality for adult and pediatric patients.
The high frequency of positioning errors was striking. The limited dimensions of the focal plane (image layer) in panoramic radiography mean that minor errors in positioning manifest as distortions due to unequal vertical and horizontal magnification, overlap of teeth, and a loss of image sharpness.
In this study, from the 1,782 panoramic radiographs evaluated, failure to position the tongue against the palate during exposure was the most common error identified; this result was in concordance with the results obtained in the studies performed by many other investigators.7,20 The possible explanation for this error might be a lack of communication of the dental technicians instructing the patients to swallow and to keep the tongue on the roof of the mouth. Another explanation was that the patients sometimes might misunderstand the instructions, putting only the tip of the tongue on the palate, or the patients did not pay much attention to the instruction given by the technician. In this study, this error was found in 55.7% of the radiographs, which was less than what was found by Rushton et al.7 The reason might be the fact that in their study the radiographs were collected from different centers, unlike ours where radiographs were taken from only one center.
A ghost shadow on the symphysis may be attributed to patient slumping; there is a natural tendency for patients, when holding the handles of the machine, to slump. The dental technician needs to be certain before taking the radiograph that the patient's back and spine are erect with the neck extended. In this study, the slumped position was the second most common error encountered. It was found in 624 radiographs (35%), which was more frequent than the result obtained by Rushton et al7 and Akarslan et al.20
Our study demonstrated separately the positioning errors caused by forward and backward positioning of the patient on the notched bite block. In our study, backward positioning of the patient (30%) was more prevalent than forward positioning (18.3%). These errors might be attributed either to a misunderstanding of the patients or even to his/her underestimation of the importance of proper positioning. Rushton et al7 combined the backward and forward position together, so they had a result of 58.8% in their study sample, which was higher than the result obtained in this study. There was agreement between this study and the other studies7,20 in terms of other positioning errors. In many instances, multiple errors occurred in one image; this could be due to spending inadequate time for patient preparation and positioning.
The Guidelines on Radiology Standards for Primary Dental Care set quality standards for dental radiography, defining the terms 'excellent', 'diagnostically acceptable', and 'unacceptable'.12 The basic standard was that the rate of 'unacceptable' radiographs should not exceed 10%. If the current sample was a representative one, then this standard would be a challenge for the majority of dentists. Good quality radiography aids diagnosis. Furthermore, it maximizes the benefits to the patient, which must be balanced against the radiation risk and the financial outlay. Thus, in addition to being an issue of radiation protection, the production of non-diagnostic radiographs becomes a consumer issue for the patient and/or health service purchaser.
A target of not less than 70% 'excellent' (fault-free) films was also suggested in the guidelines.12 Our results in this study, similar to those in previous studies,2,7 suggested that this standard might prove to be a considerable challenge. Most of the radiographs (89%) exhibited some positioning fault, usually several. In view of the results of this study, it might be appropriate to re-think the quality standards set in the guidelines, removing any mention of 'excellent' films and concentrating upon achieving a significant reduction in 'unacceptable' radiographs. It is likely that efforts to improve quality and reduce rejection rates would coincidentally lead to an increase in 'excellent' films thereafter.
The clinical situation was not considered in this study while assessing a radiograph. Panoramic radiography might not be suitable for some patients due to their physical stature, swelling/growth, facial asymmetry, or their inability to properly follow the instructions. These factors might hinder the proper positioning of the patients in the machine. In such cases, panoramic error might be inevitable.
In our study, 24.9% of the radiographs were unacceptable, which fell between the results of studies conducted by Brezden and Brooks (18.2%)2 and Rushton et al (33%).7 The percentage was probably low in the former study2 because the radiographs in that study were being submitted for claim purposes and it was likely that the dentist might have repeated poor quality films to avoid risk of claim rejection. The percentage in the latter study7 was higher because the radiographs were collected from 41 dentists, and it was previously reported that over one third of dentists in a questionnaire survey used unqualified personnel to take panoramic radiographs.21 In our study, radiographs were taken by several trained technicians.
In conclusion, the value of any diagnostic procedure depends upon the amount of information gained by its utilization. In panoramic radiography, there are numerous factors only pertinent to panoramic radiography, which can reduce the diagnostic quality of radiographs. Foremost among these factors is improper patient positioning. The dentist should take care to monitor the quality of panoramic radiographs, ensuring that they are free of positioning errors. In light of our findings, it seemed that operator skill, better communication with the patient, and spending time in patient positioning could decrease the number of errors and help produce high quality radiographs. Carrying out this film rejection analysis, which included the identification of faults and what caused them, should contribute to individualising quality control measures.
Figures and Tables
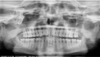 | Fig. 1The patient's chin is too high, causing a flat occlusal plane, splayed condyles, and loss of sharpness of the maxillary incisors. |
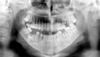 | Fig. 2The patient's chin is too low. The occlusal plane is "smiling" and the apices of the mandibular incisors are fuzzy. |
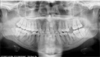 | Fig. 3The cervical spine is slumped, appearing as a pyramid shaped opacity, centred at the lower half of the film. |
 | Fig. 4The central incisors are in front of the bite groove, causing them to appear thin and fuzzy. The cervical spine is in the focal zone, causing it to be superimposed on the mandible. |
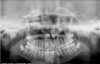 | Fig. 5The anterior teeth are positioned behind the bite groove causing them to appear wider than normal. |
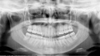 | Fig. 6Panoramic radiograph shows the patient failure to position the tongue against the palate leading to a dark shadow over the maxillary teeth between the palate and dorsum of the tongue. |
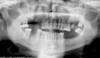 | Fig. 8The head is tilted to one side, causing one condyle to appear higher than the other and the inferior border of the mandible is slanting. |
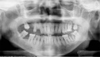 | Fig. 9The head is turned to one side, causing an asymmetry of the condyles, and wider teeth and ramus on one side than the other. |
References
1. Horner K. Review article: radiation protection in dental radiology. Br J Radiol. 1994. 67:1041–1049.
2. Brezden NA, Brooks SL. Evaluation of panoramic dental radiographs taken in private practice. Oral Surg Oral Med Oral Pathol. 1987. 63:617–621.

3. Eliasson S, Lavstedt S, Wouters F, Ostlin L. Quality of intraoral radiographs sent by private dental practitioners for therapy evaluation by the Social Insurance Office. Swed Dent J. 1990. 14:81–89.
4. Akesson L, Håkansson J, Rohlin M, Zöger B. An evaluation of image quality for the assessment of the marginal bone level in panoramic radiography. A comparison of radiographs from different dental clinics. Swed Dent J. 1993. 17:9–21.
5. Svenson B, Eriksson T, Kronström M, Palmqvist S. Image quality of intraoral radiographs used by general practitioners in prosthodontic treatment planning. Dentomaxillofac Radiol. 1994. 23:46–48.

6. Svenson B, Eriksson T, Kronström M, Palmqvist S. Quality of intraoral radiographs used for prosthodontic treatment planning by general dentists in the public dental health service. Swed Dent J. 1995. 19:47–54.
7. Rushton VE, Horner K, Worthington HV. The quality of panoramic radiographs in a sample of general dental practices. Br Dent J. 1999. 186:630–633.

8. Helminen SE, Vehkalahti M, Wolf J, Murtomaa H. Quality evaluation of young adults' radiographs in Finnish public oral health service. J Dent. 2000. 28:549–555.

9. Langland OE, Sippy FH, Morris CR, Langlais RP. Principles and practice of panoramic radiology. 1992. 2nd ed. Philadelphia: WB Saunders.
10. White SC, Pharaoh MJ. Oral Radiology: principles and interpretation. 2004. 5th ed. Philadelphia: CV Mosby;200–217.
11. Pitts NB, Kidd EA. Some of the factors to be considered in the prescription and timing of bitewing radiography in the diagnosis and management of dental caries. J Dent. 1992. 20:74–84.

12. Royal College of Radiologists. National Radiological Protection Board. Guidelines on radiology standards for primary dental care. 1994. London: NRPB;30.
13. Frederiksen NL, Benson BW, Sokolowski TW. Effective dose and risk assessment from film tomography used for dental implant diagnostics. Dentomaxillofac Radiol. 1994. 23:123–127.

14. Nixon PP, Thorogood J, Holloway J, Smith NJ. An audit of film reject and repeat rates in a department of dental radiology. Br J Radiol. 1995. 68:1304–1307.

15. Choi BR, Choi DH, Huh KH, Yi WJ, Heo MS, Choi SC, et al. Clinical image quality evaluation for panoramic radiography in Korean dental clinics. Imaging Sci Dent. 2012. 42:183–190.

16. McDavid WD, Langlais RP, Welander U, Morris CR. Real, double, and ghost images in rotational panoramic radiography. Dentomaxillofac Radiol. 1983. 12:122–128.

17. Rushton VE, Horner K. The use of panoramic radiology in dental practice. J Dent. 1996. 24:185–201.

19. Altman DG. Practical statistics for medical research. 1990. London: Chapman and Hall.




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download