Abstract
Purpose
To evaluate the mid- and long-term outcomes of inferior vena cava (IVC) filter insertion in patients with underlying deep vein thrombosis for prevention of pulmonary thromboembolism, based on a single center experience.
Materials and Methods
A total of 166 IVC filter insertion procedures in 160 patients, between February 2004 and December 2014, were retrospectively reviewed. Severity of deep vein thrombosis, indwelling time of the IVC filter, retrieval rate, and complication rate depending on the type of IVC filter were analyzed based on the patients’ radiologic findings and medical records.
Results
IVC filter insertion procedures were successfully performed in all patients. Among the 99 attempts at filter retrieval, 91 trials succeeded (91.9%, 91/99) and 8 trials failed. Indwelling time of the IVC filter showed a positive correlation with fail-ure of filter retrieval (p = 0.01). There was no procedure-related complication after all IVC filter insertion procedures. Eight delayed complications (5.0%, 8/160 patients with IVC filter insertion) were observed [caval thrombosis below the IVC filter (n = 7) and IVC penetration (n = 1)]. Gü nther Tulip filter was associated with a significant in-cidence of complication (p = 0.036).
REFERENCES
1.Deitelzweig SB., Johnson BH., Lin J., Schulman KL. Prevalence of clinical venous thromboembolism in the USA: current trends and future projections. Am J Hematol. 2011. 86:217–220.

2.Kim YH., Min SK., Kang JM., Kim HK., Bae JI., Choi SY, et al. Di-agnosis and treatment of lower extremity deep vein throm-bosis: Korean practice guidelines. J Korean Soc Radiol. 2016. 75:233–262.

4.Van Ha TG. Complications of inferior vena caval filters. Se-min Intervent Radiol. 2006. 23:150–155.

5.Chow FC., Chan YC., Cheung GC., Cheng SW. Mid- and long-term outcome of patients with permanent inferior vena cava filters: a single center review. Ann Vasc Surg. 2015. 29:985–994.

6.Haut ER., Garcia LJ., Shihab HM., Brotman DJ., Stevens KA., Sharma R, et al. The effectiveness of prophylactic inferior vena cava filters in trauma patients: a systematic review and meta-analysis. JAMA Surg. 2014. 149:194–202.
7.Caplin DM., Nikolic B., Kalva SP., Ganguli S., Saad WE., Zucker-man DA. Society of Interventional Radiology Standards of Practice Committee. Quality improvement guidelines for the performance of inferior vena cava filter placement for the prevention of pulmonary embolism. J Vasc Interv Radiol. 2011. 22:1499–1506.

8.Zhou D., Spain J., Moon E., Mclennan G., Sands MJ., Wang W. Retrospective review of 120 celect inferior vena cava filter retrievals: experience at a single institution. J Vasc Interv Radiol. 2012. 23:1557–1563.

9.Rimon U., Bensaid P., Golan G., Garniek A., Khaitovich B., Dotan Z, et al. Optease vena cava filter optimal indwelling time and retrievability. Cardiovasc Intervent Radiol. 2011. 34:532–535.

10.Smouse HB., Rosenthal D., Thuong VH., Knox MF., Dixon RG., Voorhees WD 3rd, et al. Long-term retrieval success rate profile for the Günther Tulip vena cava filter. J Vasc Interv Radiol. 2009. 20:871–877. quiz 878.

11.Lee MJ., Valenti D., de Gregorio MA., Minocha J., Rimon U., Pellerin O. The CIRSE retrievable IVC filter registry: retriev-al success rates in practice. Cardiovasc Intervent Radiol. 2015. 38:1502–1507.

12.Hoekstra A., Hoogeveen Y., Elstrodt JM., Tiebosch AT. Vena cava filter behavior and endovascular response: an experi-mental in vivo study. Cardiovasc Intervent Radiol. 2003. 26:222–226.

13.Christie DB., Kang J., Ashley DW., Mix W., Lochner FK., Solis MM, et al. Accelerated migration and proliferation of smooth muscle cells cultured from neointima induced by a vena cava filter. Am Surg. 2006. 72:491–496.

14.Blebea J., Wilson R., Waybill P., Neumyer MM., Blebea JS., An-derson KM, et al. Deep venous thrombosis after percutaneous insertion of vena caval filters. J Vasc Surg. 1999. 30:821–828.

15.Athanasoulis CA., Kaufman JA., Halpern EF., Waltman AC., Geller SC., Fan CM. Inferior vena caval filters: review of a 26-year single-center clinical experience. Radiology. 2000. 216:54–66.

16.Sangwaiya MJ., Marentis TC., Walker TG., Stecker M., Wicky ST., Kalva SP. Safety and effectiveness of the celect inferior vena cava filter: preliminary results. J Vasc Interv Radiol. 2009. 20:1188–1192.

17.Jia Z., Wu A., Tam M., Spain J., McKinney JM., Wang W. Caval penetration by inferior vena cava filters: a systematic literature review of clinical significance and management. Circu-lation. 2015. 132:944–952.

18.Bovyn G., Ricco JB., Reynaud P., Le Blanche AF. European Tempofilter II Study Group. Long-duration temporary vena cava filter: a prospective 104-case multicenter study. J Vasc Surg. 2006. 43:1222–1229.

19.Kim HJ., Chang NK., Lim JH., Kim JK. Fracture of a tempofilter II: an initial case report. Korean J Radiol. 2011. 12:626–628.

Fig. 1.
Plain abdominal radiograms show inferior vena cava filters. A. OptEase filter. B. Günther Tulip filter. C. Celect filter. D. Tempofilter II.

Fig. 2.
IVC occlusion by the filter. A 65-year-old woman with pain in her left leg. A. Initial coronal CTV image shows thrombotic occlusion of the left ilio-femoro-popliteo-crural veins. B, C. Three months after IVC filter (Günther Tulip filter) insertion, aspiration thrombectomy and stent deployment in the left iliac vein, coronal (B) and 3D (C) reformatted images show development of thrombotic occlusion in the infrarenal IVC, below the filter (arrows in B, C) and re-occlusion of the left iliac vein. D. Venogram via the left popliteal vein, shows multifocal thrombotic filling defects in the IVC filter (arrowhead) and the infrarenal IVC (arrow). E. After catheter-directed Urokinase thrombolysis (40000 IU bolus injection via the angio-sheath; continuous infusion 100000 IU, total 440000 IU) followed by aspiration thrombectomy, the venogram shows improvement in thrombotic filling defects. CTV = computed tomography venography, IVC = inferior vena cava
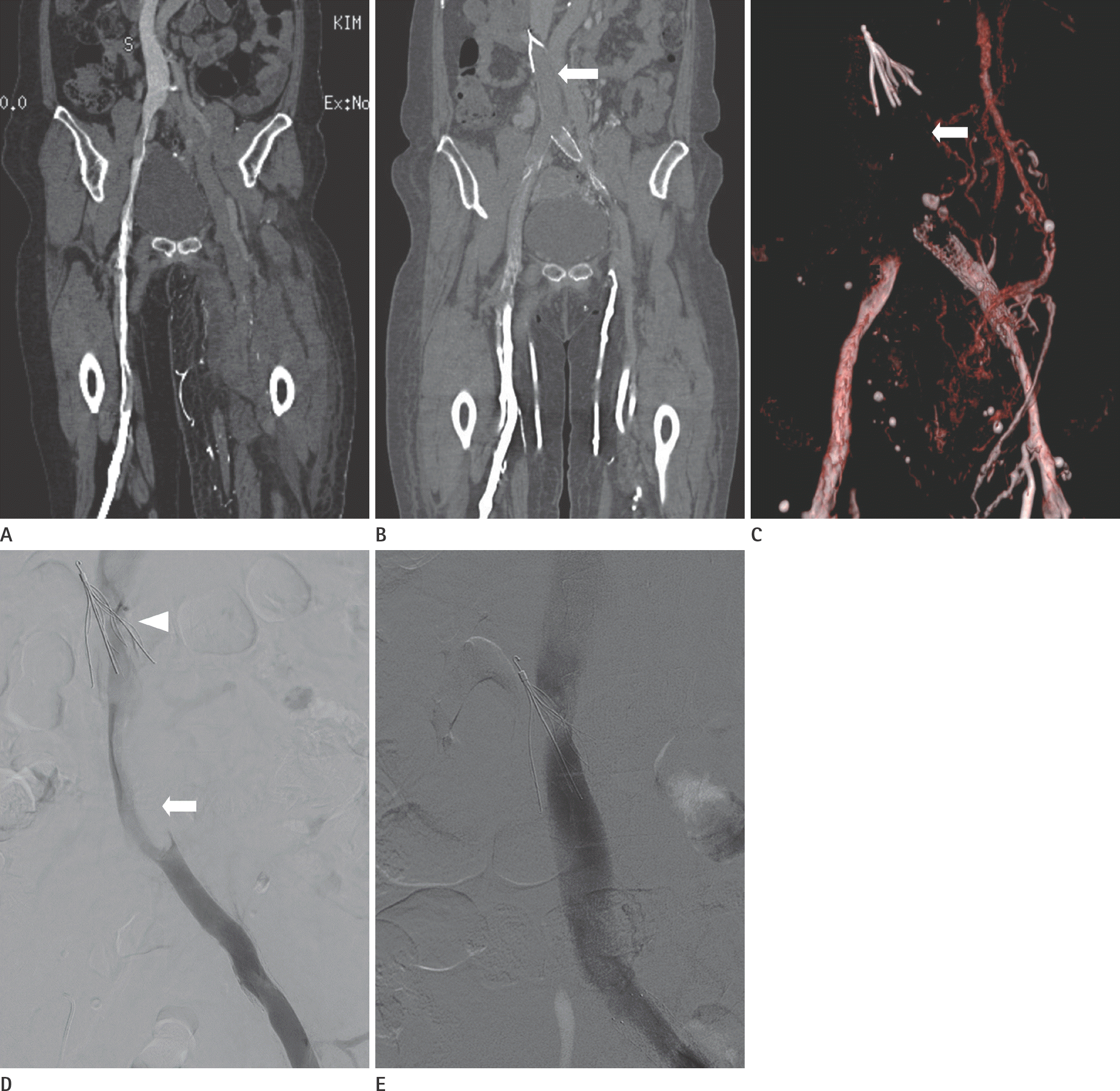
Fig. 3.
IVC perforation by the filter. A 79-year-old woman complained of swelling in both legs. Infrarenal IVC filter (Celect filter) insertion was performed to prevent pulmonary embolism. After six days, additional aspiration thrombectomy and stent deployment in the left common iliac vein were performed. A, B. The axial enhanced CT image after 4 months shows penetration of more than two filter struts (arrows in A) outside the IVC wall (more than 3 mm distance from the IVC wall) (A) and thrombotic occlusion (arrows in B) of the left common iliac vein stent (B). C. A sagittal reformatted image shows a penetrated filter strut (arrow) and an instent thrombus (arrowheads). IVC = inferior vena cava
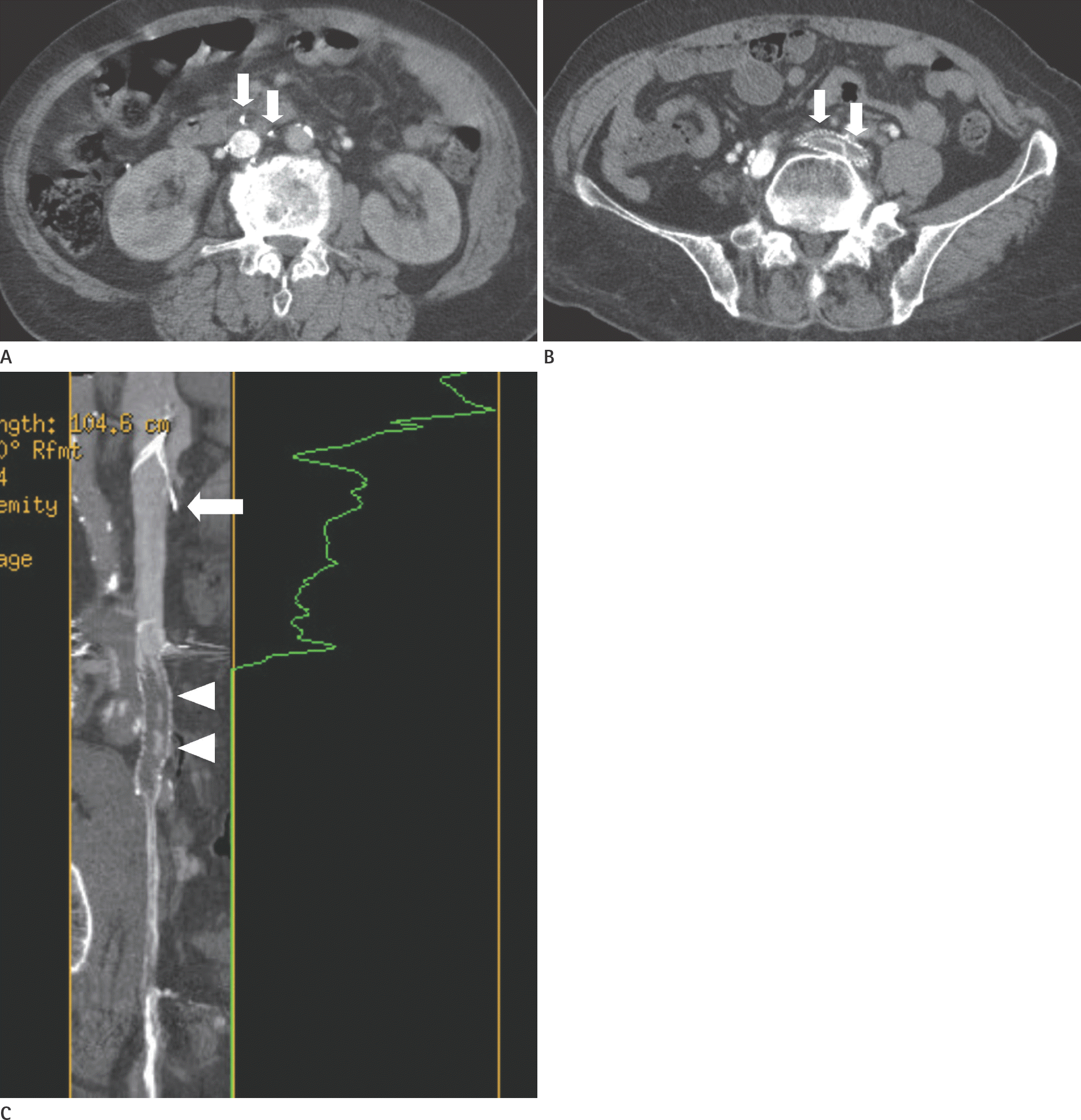
Table 1.
Summary of Study Population
| Factors | |
|---|---|
| Age | 61.7 ± 17.1* |
| (range; 14–92) | |
| Sex | |
| Male | 76 (47.5%) |
| Female | 84 (52.5%) |
| Type of used filter | |
| OptEase filter | 91 |
| Günther Tulip filter | 42 |
| Celect filter | 7 |
| Temopfilter II | 26 |
| Access route | |
| Left vein | 23 (13.9%) |
| Femoral | 13 |
| Popliteal | 10 |
| Right vein | 143 (86.1%) |
| Femoral | 83 |
| Internal jugular | 55 |
| Popliteal | 5 |
| Extent of VTE† | |
| Left | 110 (68.8%) |
| Iliac/crural (1) | 4/2 |
| Iliofemoral/femoropopliteal/popliteocrural (2) | 16/4/1 |
| Iliofemoropopliteal/femoropopliteocrural (3) | 10/12 |
| Iliofemoropopliteocrural (4) | 61 |
| Right | 26 (16.3%) |
| Iliac/femoral (1) | 1/1 |
| Iliofemoral/femoropopliteal/popliteocrural (2) | 7/1/1 |
| Iliofemoropopliteal/femoropopliteocrural (3) | 1/9 |
| Iliofemoropoliteocrural (4) | 5 |
| Both | 16 (10.0%) |
| Isolated IVC thrombosis (1) | 3 (1.9%) |
| Others | 5 (3.1%) |
| IVC and left renal vein | 1 |
| Both renal veins | 1 |
| IVC, right renal and ovarian vein | 3 |
| Score of extent of VTE | 3.62 ± 1.4* |
| (range; 1–9) | |
| Proven PTE before IVC filter insertion | 73 (45.6%) |
| Filter maintenance days | |
| Success of removal (n = 91) | 24.7 ± 20.5* |
| Failure of removal (n = 8)‡ | 107.4 ± 113.3* |
Table 2.
Patient’s Information in Accordance with Type of Filter
Table 3.
Difference of Retrieval Rate of Type of Filter
| Type of Filter | Filter Retrieval | Total | p-Value* | |
|---|---|---|---|---|
| Success | Failure | |||
| OptEase | 49 | 4 | 53 | 0.105 |
| Günther Tulip | 12 | 3 | 15 | |
| Celect | 4 | 1 | 5 | |
| Tempofilter | 26 | 0 | 26 | |
| Total | 91 | 8 | 99 | |
Table 4.
Logistic Regression Analysis of Factors That Affect the Failure of Filter Removal
| Regression Coefficient (B) | Odds Ratio | 95% CI | p-Value | |
|---|---|---|---|---|
| Maintenance time | 0.026 | 1.027 | 1.006–1.047 | 0.010* |
| Age | 0.013 | 1.013 | 0.960–1.070 | 0.627 |
Table 5.
Pearson’s Chi-Square Test of Variable Factors That Affect the Complication of IVC Filter
| Variable | Complication | Odds Ratio | 95% CI | p-Value | |
|---|---|---|---|---|---|
| No | Yes | ||||
| Sex | 0.583 | ||||
| Male | 72 | 4 (5.3) | 0.947 | 0.464–1.933 | |
| Female | 80 | 4 (4.8) | 1.053 | 0.518–2.139 | |
| Filter type* | 0.036† | ||||
| OptEase | 88 | 1 (1.1) | … | ||
| Günther Tulip | 36 | 5 (12.2) | … | ||
| Celect | 6 | 1 (14.3) | … | ||
| Tempofilter | 22 | 1 (4.3) | … | ||
| Filter location | 0.442 | ||||
| Infra-renal | 142 | 7 (4.7) | 1.068 | 0.819–1.392 | |
| Supra-renal | 10 | 1 (9.1) | 0.526 | 0.076–3.622 | |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download