Abstract
Purpose
To evaluate the clinicopathological and imaging features of mammography, ultrasonography, and magnetic resonance imaging (MRI) for breast cancer in Korean women under 40 years of age according to molecular subtypes.
Materials and Methods
We included 183 breast cancers in 176 consecutive women under 40 years old who had been diagnosed with breast cancer between January 2012 and November 2014. The patients’ clinical and pathologic records were available as electronic medical records. A retrospective review of the preoperative imaging studies was performed with 177 mammographies, 183 ultrasonographies, and 178 MRIs.
Results
Eighty-six percent (158/183) of lesions were symptomatic, with masses (147/183) as the most common presentation. Eighty percent (22/25) of the asymp-tomatic lesions were diagnosed via screening ultrasonography. The luminal A subtype was the most common (n = 79, 43%), human epidermal growth factor receptor 2-en-riched subtype showed indistinct margins on mammography (p = 0.006), the triple negative subtype depicted a posterior enhancement on ultrasonography (p < 0.001) and rim enhancement on MRI (p < 0.001).
Conclusion
Breast cancers in Korean women under 40 years of age are commonly presented with a palpable mass, and luminal A is the most common molecular subtype. In our study, the imaging and pathologic characteristics of breast cancer in younger women were similar to those previously reported for older patients.
Index terms
Breast Cancer, Mammography, Ultrasonography, Magnetic Resonance Imaging, Young AdultREFERENCES
1. Jemal A, Clegg LX, Ward E, Ries LA, Wu X, Jamison PM, et al. Annual report to the nation on the status of cancer, 1975-2001, with a special feature regarding survival. Cancer. 2004; 101:3–27.

2. Ko SS. Korean Breast Cancer Society. Chronological chang-ing patterns of clinical characteristics of Korean breast cancer patients during 10 years (1996-2006) using nationwide breast cancer registration on-line program: biannual up-date. J Surg Oncol. 2008; 98:318–323.

3. Ahn SH, Son BH, Kim SW, Kim SI, Jeong J, Ko SS, et al. Poor outcome of hormone receptor-positive breast cancer at very young age is due to tamoxifen resistance: nationwide survival data in Korea–a report from the Korean Breast Cancer Society. J Clin Oncol. 2007; 25:2360–2368.

4. Fredholm H, Eaker S, Frisell J, Holmberg L, Fredriksson I, Lindman H. Breast cancer in young women: poor survival despite intensive treatment. PLoS One. 2009; 4:e7695.

5. Prevalence and penetrance of BRCA1 and BRCA2 mutations in a population-based series of breast cancer cases. Anglian Breast Cancer Study Group. Br J Cancer. 2000; 83:1301–1308.
6. Zhou P, Recht A. Young age and outcome for women with early-stage invasive breast carcinoma. Cancer. 2004; 101:1264–1274.

7. Neal RD, Allgar VL. Sociodemographic factors and delays in the diagnosis of six cancers: analysis of data from the “National Survey of NHS Patients: Cancer”. Br J Cancer. 2005; 92:1971–1975.

8. Partridge AH, Hughes ME, Ottesen RA, Wong YN, Edge SB, Theriault RL, et al. The effect of age on delay in diagnosis and stage of breast cancer. Oncologist. 2012; 17:775–782.

9. Ruddy KJ, Gelber S, Tamimi RM, Schapira L, Come SE, Meyer ME, et al. Breast cancer presentation and diagnos-tic delays in young women. Cancer. 2014; 120:20–25.

10. Keegan TH, DeRouen MC, Press DJ, Kurian AW, Clarke CA. Occurrence of breast cancer subtypes in adolescent and young adult women. Breast Cancer Res. 2012; 14:R55.

11. Park YH, Lee SJ, Jung HA, Kim SM, Kim MJ, Kil WH, et al. Prevalence and clinical outcomes of young breast cancer (YBC) patients according to intrinsic breast cancer subtypes: single institutional experience in Korea. Breast. 2015; 24:213–217.

12. Hammond ME, Hayes DF, Dowsett M, Allred DC, Hagerty KL, Badve S, et al. American Society of Clinical Oncology/College Of American Pathologists guideline recommendations for immunohistochemical testing of estrogen and proges-terone receptors in breast cancer. J Clin Oncol. 2010; 28:2784–2795.

13. Cheang MC, Chia SK, Voduc D, Gao D, Leung S, Snider J, et al. Ki67 index, HER2 status, and prognosis of patients with luminal B breast cancer. J Natl Cancer Inst. 2009; 101:736–750.

14. American College of Radiology. ACR BI-RADS® Atlas, Breast Imaging Reporting and Data System. Reston: American College of Radiology;2013.
15. Collins LC, Marotti JD, Gelber S, Cole K, Ruddy K, Kereako-glow S, et al. Pathologic features and molecular phenotype by patient age in a large cohort of young women with breast cancer. Breast Cancer Res Treat. 2012; 131:1061–1066.

16. Tang J, Wu CC, Xie ZM, Luo RZ, Yang MT. Comparison of clinical features and treatment outcome of breast cancers in young and elderly chinese patients. Breast Care (Basel). 2011; 6:435–440.

17. Kim EK, Noh WC, Han W, Noh DY. Prognostic significance of young age (<35 years) by subtype based on ER, PR, and HER2 status in breast cancer: a nationwide registry-based study. World J Surg. 2011; 35:1244–1253.
18. Bassett LW, Ysrael M, Gold RH, Ysrael C. Usefulness of mammography and sonography in women less than 35 years of age. Radiology. 1991; 180:831–835.

19. Taneja S, Evans AJ, Rakha EA, Green AR, Ball G, Ellis IO. The mammographic correlations of a new immunohistochemical classification of invasive breast cancer. Clin Radiol. 2008; 63:1228–1235.

20. Bullier B, MacGrogan G, Bonnefoi H, Hurtevent-Labrot G, Lhomme E, Brouste V, et al. Imaging features of sporadic breast cancer in women under 40 years old: 97 cases. Eur Radiol. 2013; 23:3237–3245.
21. Lehman CD, Lee CI, Loving VA, Portillo MS, Peacock S, DeMartini WB. Accuracy and value of breast ultrasound for primary imaging evaluation of symptomatic women 30-39 years of age. AJR Am J Roentgenol. 2012; 199:1169–1177.

22. Au-Yong IT, Evans AJ, Taneja S, Rakha EA, Green AR, Paish C, et al. Sonographic correlations with the new molecular classification of invasive breast cancer. Eur Radiol. 2009; 19:2342–2348.

23. Kojima Y, Tsunoda H. Mammography and ultrasound features of triple-negative breast cancer. Breast Cancer. 2011; 18:146–151.

24. Kim JY, Lee SH, Lee JW, Kim S, Choo KS. Magnetic resonance imaging characteristics of invasive breast cancer in women aged less than 35 years. Acta Radiol. 2015; 56:924–932.

Fig. 1.
Luminal A type breast cancer of 37-year-old woman. A. Right mediolateral oblique mammography shows 2 cm-sized isodense mass with irregular shape and indistinct margin (arrow) on the right lower breast. B. Ultrasonography shows 2.5 cm-sized hypoechoic mass with irregular shape and indistinct margin (arrows) in the right 6 o'clock direction. C. Axial contrast-enhanced T1-weighted MR image with fat suppression shows a 2.5 cm-sized heterogeneously enhancing mass with an irregular shape and margin (arrows).
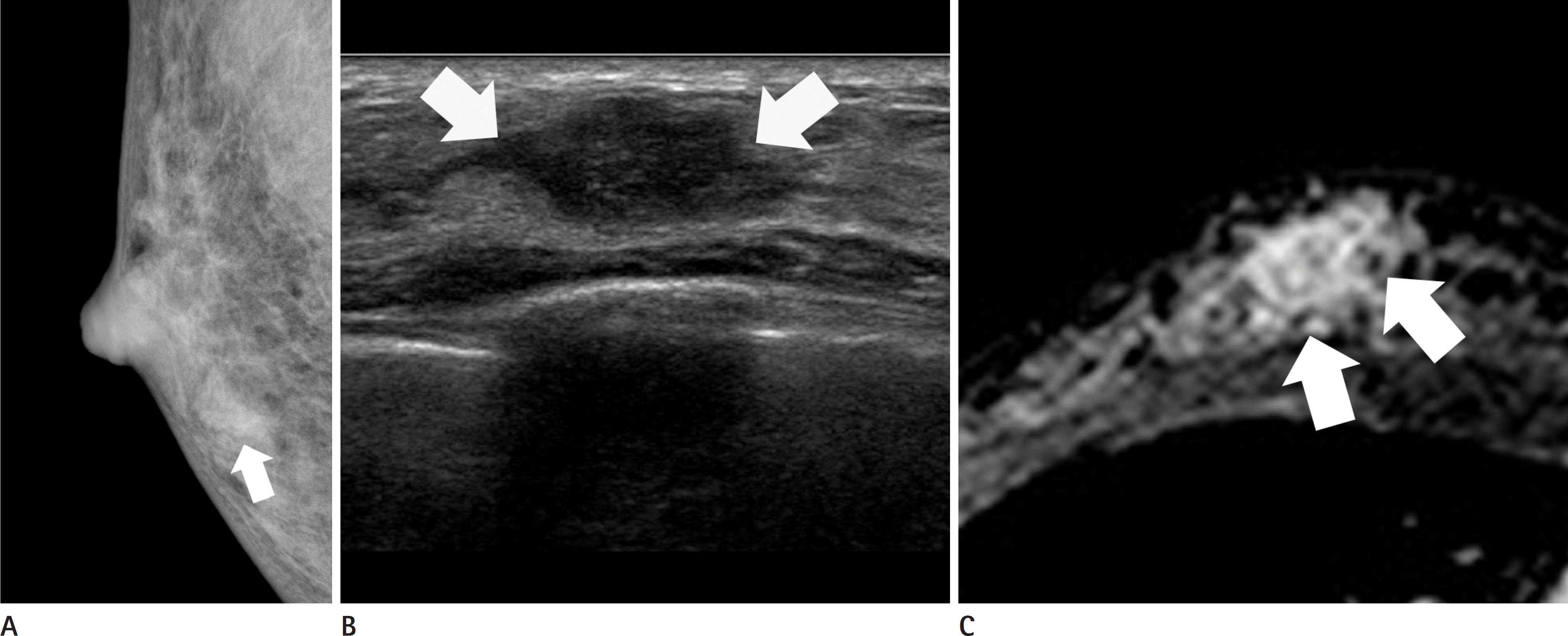
Fig. 2.
Triple negative type breast cancer of 37-year-old woman. A. Right craniocaudal mammography shows 3 cm-sized hyperdense mass with an irregular shape and obscured margin (arrows) on the right outer breast. B. Ultrasonography shows 3.4 cm-sized hypoechoic mass with an oval shape and circumscribed margin with a posterior enhancement (arrows) in the right 9 o'clock direction. C. Axial contrast-enhanced T1-weighted MR image with fat suppression shows a 3.5 cm-sized mass with an oval shape, circumscribed margin and rim enhancement (arrows) in the right outer center breast.
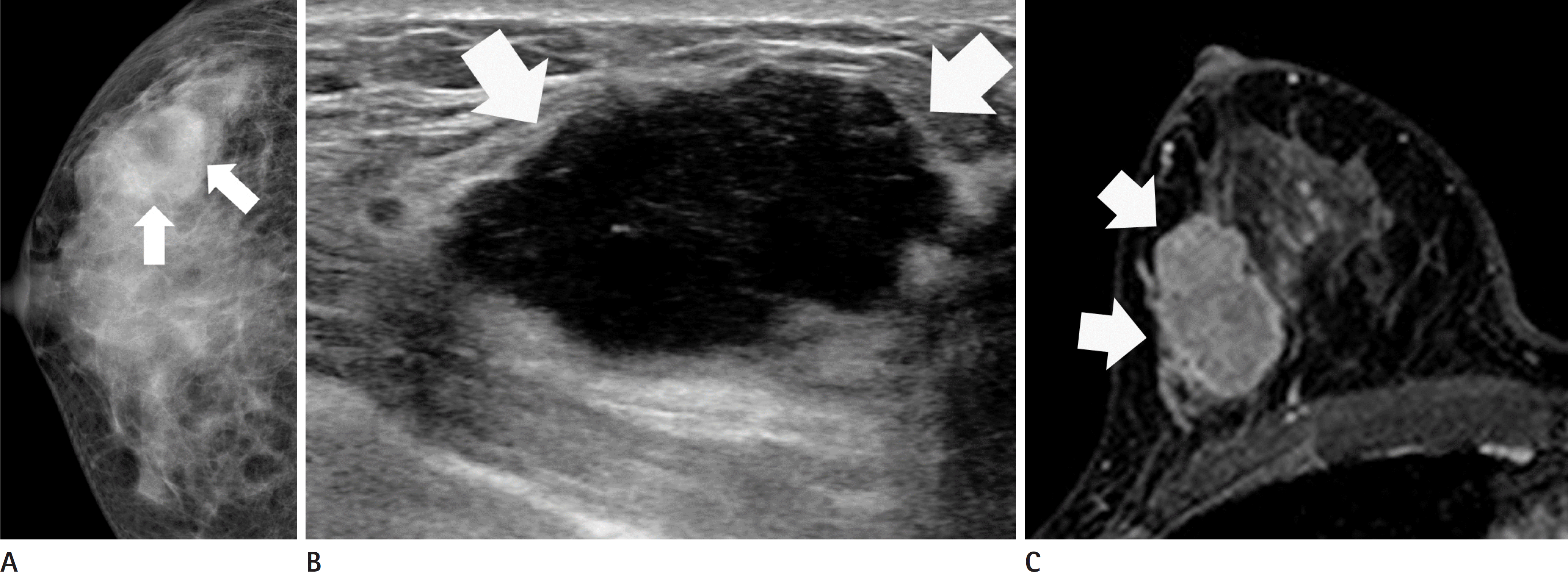
Fig. 3.
Human epidermal growth factor receptor-2 enriched type breast cancer of 38-year-old woman. A. Left mediolateral oblique mammography shows a 9-cm area of segmental fine linear microcalcifications (arrows). B. Ultrasonography shows more than 5 cm-sized heterogeneous echoic mass with an irregular shape and calcifications (arrows) in the left 5 o'clock direction. C. Axial contrast-enhanced T1-weighted MR image with fat suppression shows a 7-cm area of non-mass enhancement with segmental distribution and clustered ring internal enhancement pattern (arrows) on the left lower outer breast.
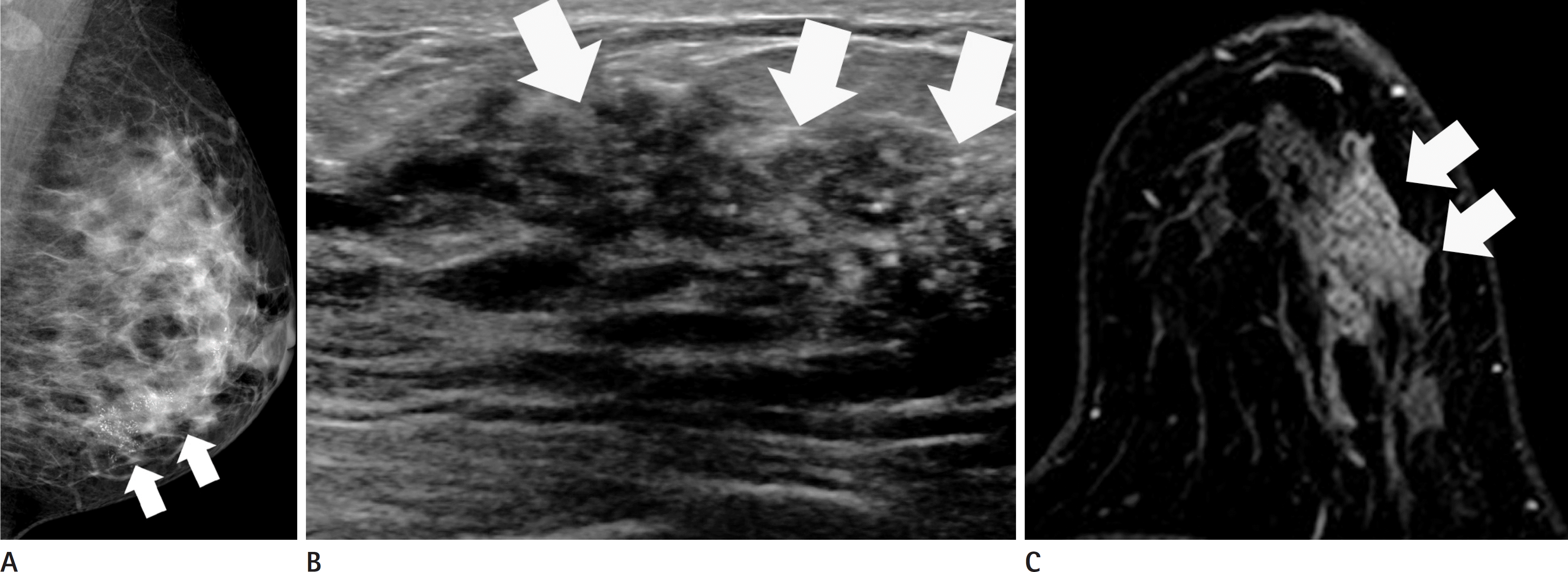
Table 1.
Clinicopathologic Data for 183 Breast Cancers in 176 Patients
| n (%) | |
|---|---|
| Clinical symptom | |
| Negative | 25 (14) |
| Lump | 147 (80) |
| Discharge | 8 (4) |
| Lump with discharge | 3 (2) |
| Histology | |
| IDC | 23 (12) |
| IDC + DCIS | 124 (68) |
| DCIS | 23 (13) |
| ILC | 2 (1) |
| Others | 11 (6) |
| Histologic grade | |
| I | 23 (13) |
| II | 87 (47) |
| III | 73 (40) |
| Molecular subtype | |
| Luminal A | 79 (43) |
| Luminal B | 42 (23) |
| HER2 + | 19 (10) |
| Triple negative | 43 (24) |
| Prior breast biopsy for breast cancer∗ | |
| No | 133 (80) |
| Yes | 33 (20) |
| Family history of breast cancer∗ | |
| No | 138 (81) |
| Yes | 32 (19) |
| Distant metastasis | |
| No | 179 (98) |
| Yes | 4 (2) |
Table 2.
Evaluation of Mammographic Features of Breast Cancer under 40 Years Old
| Characteristics | All (n = 177) | Luminal A (n = 76) | Luminal B (n = 40) | HER2 (n = 19) | TN (n = 42) | p-Value∗ |
|---|---|---|---|---|---|---|
| Finding (%) | 0.019 | |||||
| Negative | 14 (8) | 9 (12) | 2 (5) | 1 (5) | 2 (5) | |
| Mass (± calcification) | 116 (66) | 42 (55) | 26 (65) | 13 (68) | 35 (83) | |
| Calcification only | 32 (18) | 14 (18) | 11 (28) | 5 (26) | 2 (5) | |
| Others† | 15 (8) | 11 (14) | 1 (3) | 0 (0) | 3 (7) | |
| Mass (n = 116) | ||||||
| Shape (%) | 0.668 | |||||
| Oval/round | 13 (11) | 6 (14) | 3 (12) | 0 (0) | 4 (11) | |
| Irregular | 103 (89) | 36 (86) | 23 (88) | 13 (100) | 31 (89) | |
| Margin (%) | 0.006 | |||||
| Circumscribed | 6 (4) | 3 (7) | 0 (0) | 0 (0) | 3 (9) | |
| Obscured | 32 (28) | 8 (19) | 7 (27) | 1 (8) | 16 (46) | |
| Microlobulated | 3 (3) | 2 (5) | 1 (4) | 0 (0) | 0 (0) | |
| Indistinct | 52 (45) | 15 (36) | 12 (46) | 11 (85) | 14 (40) | |
| Spiculated | 23 (20) | 14 (33) | 6 (23) | 1 (8) | 2 (6) | |
| Density (%) | 0.075 | |||||
| High | 75 (65) | 21 (50) | 18 (69) | 11 (85) | 25 (71) | |
| Equal | 41 (35) | 21 (50) | 8 (31) | 2 (15) | 10 (29) | |
| Low | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | |
| Calcification (n = 81) | ||||||
| Shape (%) | 0.399 | |||||
| Round | 7 (9) | 3 (10) | 2 (8) | 1 (8) | 1 (8) | |
| Amorphous | 16 (20) | 8 (27) | 3 (12) | 2 (15) | 3 (31) | |
| Coarse heterogeneous | 8 (10) | 2 (7) | 1 (4) | 1 (8) | 3 (23) | |
| Fine pleomorphic | 28 (35) | 10 (33) | 11 (44) | 3 (23) | 4 (31) | |
| Fine linear branching | 22 (27) | 7 (23) | 8 (32) | 6 (46) | 1 (8) | |
| Distribution (%) | 0.143 | |||||
| Grouped | 40 (49) | 12 (40) | 14 (56) | 5 (38) | 9 (69) | |
| Linear | 8 (10) | 2 (7) | 0 (0) | 3 (23) | 3 (23) | |
| Segmental | 13 (16) | 5 (17) | 6 (24) | 2 (15) | 0 (0) | |
| Regional | 14 (17) | 8 (27) | 3 (12) | 2 (15) | 1 (8) | |
| Diffuse | 6 (7) | 3 (10) | 2 (8) | 1 (8) | 0 (0) |
Table 3.
Evaluation of Ultrasonography Features of Breast Cancer under 40 Years Old
| Characteristics | All (n = 183) | Luminal A (n = 79) | Luminal B (n = 42) | HER2 (n = 19) | TN (n = 43) | p-Value∗ |
|---|---|---|---|---|---|---|
| Finding (%) | 0.211 | |||||
| Mass (± calcification) | 179 (98) | 78 (99) | 40 (95) | 18 (95) | 43 (100) | |
| Negative | 4 (2) | 1 (1) | 2 (5) | 1 (5) | 0 (0) | |
| Mass (± calcification) (n = 179) | ||||||
| Shape (%) | 0.481 | |||||
| Oval/round | 25 (14) | 8 (10) | 8 (20) | 2 (11) | 7 (16) | |
| Irregular | 154 (86) | 70 (90) | 32 (80) | 16 (89) | 36 (84) | |
| Margin (%) | 0.478 | |||||
| Circumscribed | 24 (13) | 11 (14) | 3 (8) | 1 (6) | 9 (21) | |
| Indistinct | 71 (40) | 30 (38) | 18 (45) | 9 (50) | 14 (33) | |
| Angular | 42 (23) | 19 (24) | 9 (23) | 3 (17) | 11 (26) | |
| Microlobulated | 33 (18) | 12 (15) | 7 (18) | 5 (28) | 9 (21) | |
| Spiculated | 9 (5) | 6 (8) | 3 (8) | 0 (0) | 0 (0) | |
| Orientation (%) | 0.095 | |||||
| Parallel | 146 (82) | 60 (77) | 34 (85) | 18 (100) | 34 (79) | |
| Non-parallel | 33 (18) | 18 (23) | 6 (15) | 0 (0) | 9 (21) | |
| Echo pattern (%) | 0.079 | |||||
| Anechoic | 1 (1) | 1 (1) | 0 (0) | 0 (0) | 0 (0) | |
| Hyperechoic | 2 (1) | 2 (3) | 0 (0) | 0 (0) | 0 (0) | |
| Complex cystic and solid | 6 (3) | 3 (4) | 0 (0) | 0 (0) | 3 (7) | |
| Hypoechoic | 93 (52) | 41 (53) | 21 (53) | 6 (33) | 25 (58) | |
| Isoechoic | 23 (13) | 15 (19) | 4 (10) | 4 (22) | 0 (0) | |
| Heterogeneous | 54 (30) | 16 (21) | 15 (38) | 8 (44) | 15 (35) | |
| Posterior feature (%) | < 0.001 | |||||
| Non | 114 (64) | 56 (72) | 33 (83) | 7 (39) | 18 (42) | |
| Enhancement | 46 (26) | 14 (18) | 5 (13) | 6 (33) | 21 (49) | |
| Shadowing | 13 (7) | 6 (8) | 1 (3) | 3 (17) | 3 (7) | |
| Combined | 6 (3) | 2 (3) | 1 (3) | 2 (11) | 1 (2) |
Table 4.
Evaluation of Magnetic Resonance Imaging Features of Breast Cancer under 40 Years Old
| Characteristics | All (n = 178) | Luminal A (n = 76) | Luminal B (n = 41) | HER2 (n = 18) | TN (n = 43) | p-Value∗ |
|---|---|---|---|---|---|---|
| Finding (%) | 0.086 | |||||
| Mass | 143 (80) | 58 (76) | 33 (80) | 12 (67) | 40 (93) | |
| NME | 32 (18) | 15 (20) | 8 (20) | 6 (33) | 3 (7) | |
| Focus | 3 (2) | 3 (4) | 0 (0) | 0 (0) | 0 (0) | |
| Mass (n = 143) | ||||||
| Shape (%) | 0.618 | |||||
| Oval/round | 24 (17) | 9 (16) | 8 (24) | 1 (8) | 6 (15) | |
| Irregular | 119 (83) | 49 (84) | 25 (76) | 11 (92) | 34 (85) | |
| Margin (%) | 0.179 | |||||
| Circumscribed | 41 (29) | 17 (29) | 10 (30) | 2 (17) | 12 (30) | |
| Irregular | 80 (56) | 27 (47) | 18 (55) | 9 (75) | 26 (65) | |
| Spiculated | 22 (15) | 14 (24) | 5 (15) | 1 (8) | 2 (5) | |
| Internal enhancement (%) | < 0.001 | |||||
| Homogenous | 37 (26) | 20 (34) | 11 (33) | 2 (17) | 4 (10) | |
| Heterogeneous | 63 (44) | 31 (53) | 13 (39) | 5 (42) | 14 (35) | |
| Rim | 41 (29) | 7 (12) | 9 (27) | 3 (25) | 22 (55) | |
| Dark internal septation | 2 (1) | 0 (0) | 0 (0) | 2 (17) | 0 (0) | |
| NME (n = 32) | ||||||
| Distribution (%) | 0.587 | |||||
| Focal | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | |
| Linear | 1 (3) | 1 (7) | 0 (0) | 0 (0) | 0 (0) | |
| Segmental | 14 (44) | 6 (40) | 4 (50) | 4 (67) | 0 (0) | |
| Regional | 7 (22) | 4 (27) | 2 (25) | 0 (0) | 1 (33) | |
| Multiple regional | 3 (9) | 2 (13) | 0 (0) | 1 (17) | 0 (0) | |
| Diffuse | 7 (22) | 2 (13) | 2 (25) | 1 (17) | 2 (67) | |
| Internal enhancement (%) | 0.578 | |||||
| Homogenous | 6 (19) | 3 (20) | 3 (38) | 0 (0) | 0 (0) | |
| Heterogeneous | 14 (43) | 7 (47) | 3 (38) | 3 (50) | 1 (33) | |
| Clumped | 8 (25) | 4 (27) | 1 (13) | 1 (17) | 2 (67) | |
| Clustered ring | 4 (13) | 1 (7) | 1 (13) | 2 (33) | 0 (0) |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download