Abstract
Cavernous dural arteriovenous fistula (DAVF), which usually presents with conjunctival injection, proptosis, loss of visual acuity, and ophthalmoplegia, is a rare cause of ophthalmoplegia. Thus, it may be overlooked when the typical symptoms are lacking. There have been some cavernous DAVF case reports presenting with isolated oculomotor, abducens and trochlear nerve palsy. We report a patient presenting with isolated oculomotor palsy, caused by cavernous DAVF, which was treated by transvenous coil embolization. This case suggests that cavernous DAVF should be considered in the differential diagnosis of isolated oculomotor nerve palsy and for which case - selective angiography and embolization may be helpful in reaching a diagnosis and providing a guide for optimal treatment.
Figures and Tables
Fig. 1
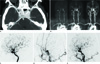
A 76-year-old female patient with a cavernous dural arteriovenous fistula.
A. An axial CT source image shows asymmetrical contrast filling in the left cavernous sinus, especially, in the posterior aspect of the cavernous sinus (arrow).
B. Time-resolved contrast MRA images show a rapid arterial phase filling of both the left cavernous sinus (arrowhead) and the inferior petrosal sinus (arrow) because of the left cavernous dural arteriovenous fistula.
C. Left internal carotid angiography shows early filling of the superoposterior cavernous sinus (arrow) with drainage into the inferior petrosal sinus. Note that the superior ophthalmic vein was not visualized.
D. Left external carotid angiography shows a cavernous dural arteriovenous fistula, supplied by a recurrent meningeal artery (arrow) from the middle meningeal artery, and with drainage into the inferior petrosal sinus.
E. Left common carotid angiography demonstrates complete occlusion of the fistula.
Note.-MRA = magnetic resonance angiography
References
1. Chen PR, Amin-Hanjani S, Albuquerque FC, McDougall C, Zabramski JM, Spetzler RF. Outcome of oculomotor nerve palsy from posterior communicating artery aneurysms: comparison of clipping and coiling. Neurosurgery. 2006. 58:1040–1046. discussion 1040-1046.
2. Kobayashi H, Kawabori M, Terasaka S, Murata J, Houkin K. A possible mechanism of isolated oculomotor nerve palsy by apoplexy of pituitary adenoma without cavernous sinus invasion: a report of two cases. Acta Neurochir (Wien). 2011. 153:2453–2456. discussion 2456.
3. Acierno MD, Trobe JD, Cornblath WT, Gebarski SS. Painful oculomotor palsy caused by posterior-draining dural carotid cavernous fistulas. Arch Ophthalmol. 1995. 113:1045–1049.
4. Kurata A, Takano M, Tokiwa K, Miyasaka Y, Yada K, Kan S. Spontaneous carotid cavernous fistula presenting only with cranial nerve palsies. AJNR Am J Neuroradiol. 1993. 14:1097–1101.
5. Wu HC, Ro LS, Chen CJ, Chen ST, Lee TH, Chen YC, et al. Isolated ocular motor nerve palsy in dural carotid-cavernous sinus fistula. Eur J Neurol. 2006. 13:1221–1225.
6. Kim MS, Han DH, Kwon OK, Oh CW, Han MH. Clinical characteristics of dural arteriovenous fistula. J Clin Neurosci. 2002. 9:147–155.
7. Miyachi S, Negoro M, Handa T, Sugita K. Dural carotid cavernous sinus fistula presenting as isolated oculomotor nerve palsy. Surg Neurol. 1993. 39:105–109.
8. Hawke SH, Mullie MA, Hoyt WF, Hallinan JM, Halmagyi GM. Painful oculomotor nerve palsy due to dural-cavernous sinus shunt. Arch Neurol. 1989. 46:1252–1255.
9. Farb RI, Agid R, Willinsky RA, Johnstone DM, Terbrugge KG. Cranial dural arteriovenous fistula: diagnosis and classification with time-resolved MR angiography at 3T. AJNR Am J Neuroradiol. 2009. 30:1546–1551.
10. Klisch J, Huppertz HJ, Spetzger U, Hetzel A, Seeger W, Schumacher M. Transvenous treatment of carotid cavernous and dural arteriovenous fistulae: results for 31 patients and review of the literature. Neurosurgery. 2003. 53:836–856. discussion 856-857.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download