INTRODUCTION
Radiologic reports of tuberculous aneurysms of the aorta are rare. Tuberculous aneurysms of the aorta are also highly susceptible to rupture. These complications are treatable, but may be fatal if not treated properly (123456). Conventional treatment consists of surgical repair and antituberculosis chemotherapy (1234). Endovascular repair has been proposed as an alternative to open surgery in selected patients (27).
In this report, we present a case with miliary tuberculosis and a tuberculous pseudoaneurysm arising in the tuberculous aortitis of the descending thoracic aorta. The tuberculous pseudoaneurysm was treated with endovascular stent graft insertion. Initial disease control was successfully attained. However, perigraft recurrence of tuberculosis one month after cessation of the antituberculous drugs led to surgical treatment.
CASE REPORT
A 56-year-old man was admitted to the hospital with fever and generalized malaise that had lasted for several weeks.
A chest radiograph revealed diffusely scattered small nodules in both lungs. Contrast-enhanced computed tomography (CT) of the thorax revealed multiple miliary nodules in both lungs, small necrotic mediastinal lymph nodes, and a crescent-shaped periaortic low density lesion (2.5 × 1 × 2.5 cm) encasing the descending thoracic aorta in the superior segment of the lower lobe of the left lung. The descending thoracic aorta was slightly compressed by the periaortic lesion. The adjacent aortic wall demonstrated a slightly irregular appearance. These changes were consistent with aortitis. However, there was no aneurysmal dilatation of the aorta (Fig. 1).
The acid-fast staining and culture of the patient's bronchoalveolar lavage fluid were positive for acid-fast bacilli. The polymerase chain reaction analysis of the bronchoalveolar lavage fluid was positive for Mycobacterium tuberculosis. We diagnosed the patient with miliary tuberculosis and tuberculous aortitis and initiated medical treatment with antituberculous drugs.
Two months later, the patient revisited the emergency room due to active hemoptysis with about 250 mL in 24 hours. Upon physical examination, his vital signs included a blood pressure 120/80 mm Hg, pulse rate of 120 beats per minute, respiratory rate of 24 breaths per minute, and body temperature of 37.1℃. Laboratory tests revealed high C-reactive protein and slightly decreased hemoglobin levels (11.4 g/dL), hematocrit (33.2%), and white blood cell count (3,200/mm3). The results of renal and hepatic function tests and coagulation profile were within normal limits.
A chest radiograph revealed widening of the mediastinum and more prominent miliary nodules in both lungs. Contrast-enhanced CT of the thorax performed on the same day revealed increased sizes of the miliary nodules in both lungs, enlarged mediastinal lymph nodes, and patchy ground glass opacities suggesting aspirated blood in the superior segment of the lower lobe and the lingular division of the upper lobe of the left lung. CT also revealed an approximately 4 × 4 × 4.8 564cm saccular pseudoaneurysm with mural thrombus of the left anterolateral wall of the descending thoracic aorta between the fifth and sixth thoracic vertebral levels (Fig. 2). There was no pleural effusion, pericardial effusion, or any findings suggesting tuberculous spondylitis on CT images.
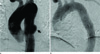
An aortography showed an approximately 3.3 × 3.8 cm pseudoaneurysm of the descending thoracic aorta without evidence of rupture (Fig. 3A). Left bronchial arteriography demonstrated an enlarged left bronchial artery, focal parenchymal staining around the consolidation of the lower lobe of the left lung adjacent to the psedoaneurysm of the descending thoracic aorta, and a shunt at the pulmonary artery. Also, the aortography did not show direct communication between the bronchial artery and aortic pseudoaneurysm. The left bronchial artery was selected and embolized with polyvinyl alcohol particles (350-550 µm) because the patient complained of hemoptysis. Hemoptysis stopped immediately after the procedure. We planned a stent graft insertion covering the origin of the left bronchial artery to repair the pseudoaneurysm.
On the next day, we performed an endovascular repair of the pseudoaneurysm via the right femoral artery approach with a stent graft, 36 mm in diameter and 130 mm in length (SEAL; S&G Biotech Inc., Seoul, Korea). We selected a stent graft of 36 mm in diameter because the largest diameter of the most proximal descending thoracic aorta was about 30 mm. The aortography revealed complete exclusion of the pseudoaneurysm by the stent graft (Fig. 3B). Follow-up CT aortography obtained two days after the procedure showed complete exclusion of the pseudoaneurysm without evidence of endoleak. The patient's recovery was uneventful. He was discharged on the seventh day after the procedure with antituberculous drugs.
One month later, a follow-up CT aortography revealed focal saccular bulging of the stent graft into the slightly decreased pseudoaneurysm of the descending thoracic aorta without contrast filling of the pseudoaneurysm. The patient complained of small amounts of intermittent hemoptysis after the follow-up CT aortography. Two months later, a follow-up CT aortography revealed improving miliary tuberculosis and progression of the bulging of the stent graft. Based on the CT findings and the patient's symptoms of intermittent hemoptysis, a type 1 endoleak was suspected, although the contrast filling of the pseudoaneurysm was not present on CT.
We planned an additional endovascular stent graft insertion. An endovascular graft, 32 mm in diameter and 169 mm in length (Talent; Medtronic Inc., Minneapolis, MN, USA) was deployed across the bulged portion of the stent graft, because the largest diameter of the stent graft in the descending thoracic aorta was 26 mm. Post-deployment aortography revealed complete exclusion of the bulged portion of the previous stent graft. No endovascular leaks were demonstrated (Fig. 4). Hemoptysis did not recur after the procedure.
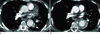
About eight months later, a follow-up CT aortography demonstrated a markedly decreased pseudoaneurysm of the descending thoracic aorta and improved miliary tuberculosis (Fig. 5A).
However, two months later, the patient revisited the emergency room with chest and back pain after one month after cessation of antituberculous drugs for 12 months. A chest CT demonstrated soft tissue density around the endovascular stent graft of the descending thoracic aorta (Fig. 5B). This change was consistent with perigraft recurrence of tuberculosis. The patient underwent surgical resection of the aneurysm and interposition of the tube graft at the other hospital. The patient's further course was uneventful.
DISCUSSION
Tuberculous aneurysms of the aorta are rare complications associated with high rates of mortality if undiagnosed or untreated (23456). Tuberculous false aneurysms are more common than true aneurysms in the aorta. Morphologically, most aneurysms are saccular, and rarely dissecting (126).
Tuberculous arterial disease can be divided into four types: miliary tuberculosis of the intima (type 1 of Haythorn), polyp of tuberculous tissue attached to the intima (type 2 of Haythorn), tuberculosis involving several layers of the wall (type 3 of Haythorn), and tuberculous aneurysm (type 4 Haythorn) (1). Tuberculous aortitis is classified as a type 3 tuberculous arterial disease according to Haythorn, and is usually indicative of disseminated tuberculosis (18). Miliary tuberculosis is a predisposing factor for the development of tuberculous aneurysms, as in the present case (1). Tuberculous aneurysms occur in half of all cases of tuberculous aortitis (58).
In this case, the tuberculous pseudoaneurysm arose from pre-existing tuberculous aortitis detected during antituberculosis chemotherapy. In cases of poor drug penetration into the necrotic tissue, the aneurysm may progress despite improvement in the surrounding pulmonary tuberculosis (7).
Three pathways of tuberculous infection into the aortic wall have been described. The first is direct implantation on the internal surface of the vessel wall in patients with miliary tuberculosis, resulting in arteritis, localized perforation and pseudoaneurysm formation. The second is septic invasion of the vasa vasorum extending into the adventitia or media, resulting in generalized aortic weakening and true aneurysm formation. The third is involvement of the vessel wall by direct extension from contagious lesions, such as infected lymph nodes, empyema, pericarditis, spondylitis, or a paravertebral abscess resulting in pseudoaneurysm formation. The third pathway of tuberculous infection into the aortic wall is the most common (1235679). In this case, we suspected that the aortic aneurysm was caused by direct implantation of the tubercle bacilli on the internal surface of the vessel wall, because the patient had miliary tuberculosis, and CT demonstrated no significant contiguous inflammatory focus.
Medical treatment should be initiated when a tuberculous aneurysm is confirmed (124). However, medical treatment of the tuberculous aneurysm usually only slows the disease progression, so surgical treatment is still necessary (134510). Standard surgical options include radical debridement of the surrounding soft tissue and reconstruction by in situ graft placement or extra-anatomic bypass (467). However, surgery is associated with high mortality and morbidity, especially in patients with risk factors such as old age or severe cardiac, renal, or pulmonary diseases (610).
Currently, insertion of stent grafts is another treatment option available for tuberculous pseudoaneurysm (26910). Major problems with the endovascular approach are associated with the impossibility of performing extensive excision and debridement of the surrounding infected tissue and implantation of the stent, which is a potential focus of infection. However, this procedure is less invasive and is associated with improved mortality and morbidity compared to conventional open surgery, and provides a good treatment alternative for tuberculous pseudoaneurysm (26710).
This patient's miliary tuberculosis led us to avoid a surgical procedure and endovascular treatment could be a bridge treatment to curative surgical treatment during improvement of the miliary tuberculosis.
To our knowledge, there have been seven previous case reports which included endovascular treatment of tuberculous aortic psedoaneurysms, and five involving the thoracic aorta (267910). Two of the five patients with thoracic aortic psedoaneurysms had poor outcomes. The other three patients recovered without complication (27910).
In the present case, a type 1 endoleak was suspected because there was progressive focal bulging of the stent graft into the psedoaneurysm, and intermittent hemoptysis recurred. We were afraid that a fatal rupture of stent graft could occur after progressive bulging of the stent graft. Consequently, the lesion was treated with an additional stent graft insertion.
In this patient, perigraft recurrence of tuberculosis of the aortic stent graft developed after cessation of antituberculous medication. In a review of the literature, chronic or lifelong antimycobacterial treatment is recommended when interventional treatment is performed (27). In this case, lifelong antituberculous medication would be helpful to prevent the perigraft recurrence of tuberculosis of the aortic stent graft.
In conclusion, endovascular procedures with stent graft are alternative strategies to open surgery in selected patients and can be a bridge treatment to curative surgical treatment.




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download