Abstract
Hypothyroid myopathy is observed frequently and the resolution of the clinical manifestations of myopathy following thyroid hormone replacement is well known. However, a specific subtype of hypothyroid myopathy, Hoffmann's syndrome, characterized by increased muscular mass (pseudohypertrophy), proximal muscle weakness, muscle stiffness and cramps, is rarely reported. Herein, we describe a 34-year-old male who presented with proximal muscle weakness and non-pitting edema of the lower extremities. He initially visited the neurology department where he was suspected of having polymyositis. Additional laboratory evaluation revealed profound autoimmune hypothyroidism and elevated muscle enzymes including creatine kinase. The patient was started on levothyroxine treatment and, subsequently, clinical symptoms and biochemical parameters resolved with the treatment. The present case highlights that hypothyroidism should be considered in the differential diagnosis of musculoskeletal symptoms even in the absence of overt manifestations of hypothyroidism. To our knowledge, this is the first case reported in Korea.
Musculoskeletal symptoms are observed in 30% to 80% of patients with hypothyroidism [12]. The symptoms consist of muscle weakness, pain, cramps, and stiffness and are usually mild but tend to become overt especially in untreated severe hypothyroidism [3]. There are four subtypes of myopathy associated with hypothyroidism: Hoffmann's syndrome, myasthenic syndrome, atrophic form, and Kocher-Debre-Semelaigne syndrome [4].
Hoffmann's syndrome, first reported by Johann Hoffmann in 1897, is characterized by increased muscular mass (pseudohypertrophy), muscle stiffness, proximal muscle weakness, and occasional muscle cramps [5]. The reported patient was an adult who developed peroneal muscular atrophy and myopathy associated with hypothyroidism after thyroidectomy. This syndrome has a relatively favorable outcome if the thyroid hormone is replaced. Nevertheless, because of its rarity, this presentation can be mistaken for primary muscular disorders such as polymyositis other than an initial manifestation of hypothyroidism, especially when systemic signs of hypothyroidism are minimal or absent.
Herein, we describe a 34-year-old male who presented mainly with musculoskeletal symptoms and was diagnosed with Hoffmann's syndrome associated with hypothyroidism. To our knowledge, this is the first case reported in Korea.
A 34-year-old male presented in July 2014 with progressive leg swelling and pain on exertion for approximately 6 months and was admitted to the neurology department. The patient had developed considerable difficulty in ascending stairs for approximately 1 month. He had become gradually lethargic and intolerant to cold for 1 year. He had chronic constipation. He had no particular medical history including diabetes mellitus, prior thyroid disease, neuromuscular disorders, or autoimmune diseases and denied any history of medications. On physical examination, his face was puffy with preorbital swelling (Fig. 1A) and his voice was hoarse. He had no goiter. His hands were edematous and had difficulty in grasping (Fig. 1B). His trapezius, biceps, triceps, and gastrocnemius muscles were hypertrophied although he denied that he exercised regularly. He also had non-pitting edema and induration of the skin on the lower extremities (Fig. 1C). On neurological examination, he had normal mentality. Upper and lower limb muscle weakness (grade 4/5) was observed, most markedly in the lower extremities. The deep tendon reflexes were sluggish.
Laboratory findings revealed a hemoglobin level of 12.4 g/dL (normal range, 13.2 to 17.3), elevated total cholesterol level of 327 mg/dL (normal range, 130 to 240), and elevated muscle enzymes as follows: aspartate aminotransferase (AST) 107 IU/L (normal range, 3 to 45); alanine aminotransferase 106 IU/L (normal range, 3 to 45); creatine kinase (CK) 7,332 IU/L (normal range, 43 to 198); lactate dehydrogenase (LDH) 1,958 IU/L (normal range, 238 to 422); serum myoglobin 235.4 ng/mL (normal range, 28 to 72); and aldolase 10.5 U/L (normal range, 0.0 to 7.6). Hepatitis markers, including hepatitis B surface antigen, hepatitis B surface antibody, hepatitis C virus antibody, and hepatitis A virus antibody immunoglobulin M were negative. Urine myoglobin and protein were negative. Other biochemical blood tests revealed a blood urea nitrogen of 10.5 mg/dL (normal range, 7 to 23), a creatinine of 1.58 mg/dL (normal range, 0.7 to 1.44), a protein of 7.9 mg/dL (normal range, 6.6 to 8.3), albumin of 4.7 mg/dL (normal range, 3.5 to 5.2), and total bilirubin of 0.45 mg/dL (normal range, 0.3 to 1.4). Electrolytes were in the normal range. The thyroid function test showed severe hypothyroidism with thyroid stimulating hormone (TSH) above 100 µIU/mL (normal range, 0.17 to 4.05), free thyroxine (FT4) of 0.03 ng/dL (normal range, 0.79 to 1.86), and total triiodothyronine of 75.8 ng/dL (normal range, 78 to 182). Anti-microsomal antibody was positive at 56.26 IU/mL (normal range, 0 to 5.61), and anti-thyroglobulin antibody was also elevated at 348.02 IU/mL (normal range, 0 to 4.11). The value of erythrocyte sedimentation rate was 9 mm/hr (normal range, 0 to 15) and C-reactive protein was 0.16 mg/L (normal range, 0 to 5). Fluorescent antinuclear antibody, anti-neutrophil cytoplasmic antibody, and rheumatoid factor were negative.
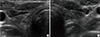
Ultrasonography of the neck revealed an atrophied thyroid (Fig. 2). Electrocardiogram showed sinus bradycardia (51 beats per minute) and a first-degree atrioventricular block; echocardiography showed a small amount of pericardial effusion (post, 8 mm) with preserved left ventricular systolic function. Electromyography showed mild spontaneous activity and short amplitude with polyphasic myopathic motor unit potential (Fig. 3). In addition, electroneurography revealed bilateral carpal tunnel syndrome and reduced nerve conduction velocity on the superficial peroneal nerve. Magnetic resonance imaging of the lower extremities revealed symmetric multifocal patchy muscle enhancements with diffuse muscle swelling in thighs and lower legs, especially in the superficial posterior compartment and gastrocnemius muscles that showed hyperintensity on T2-weighted images (Fig. 4). Muscle biopsy was recommended but was not performed due to the patient's refusal.
Based on the above findings, the patient was diagnosed with autoimmune hypothyroidism with Hoffmann's syndrome. He was treated with oral levothyroxine starting with 125 µg/day and gradually increased up to 200 µg/day. At the 1 month follow-up, his condition had improved significantly; the puffiness of his face and eyelids had regressed, the calf muscle size was decreased and muscle strength had returned to normal. After 2 months of thyroid hormone replacement, the muscle enzymes and creatinine were decreased as follows: CK, 103 IU/L; LDH, 409 IU/L; myoglobin, 55.8 ng/mL; and creatinine, 1.32 mg/dL. At 3 months, the TSH value was reduced to 3.04 µIU/mL, FT4 increased to 1.26 ng/dL, and creatinine was decreased to 0.9 mg/dL. He is receiving levothyroxine (200 µg/day) at an outpatient clinic.
The manifestations of hypothyroid myopathy depend on the severity and duration of hypothyroidism [4]. Most patients with hypothyroidism have few apparent musculoskeletal symptoms at the time of diagnosis. The patient in our case suffered from proximal weakness of the lower extremities and initially visited the neurology department where he was suspected of having polymyositis and was admitted for further evaluation of his muscular symptoms including progressive muscle weakness, hypertrophy and CK elevation. Polymyositis is an autoimmune inflammatory myopathy that presents with muscle weakness and elevated muscle enzymes, which requires long-term immunosuppressive therapy [2] and can be confused with hypothyroid myopathy because of clinical and biochemical similarities. However, the laboratory findings on admission revealed highly elevated TSH and, therefore, he was referred to the endocrinology department and was finally diagnosed as having autoimmune hypothyroidism with Hoffmann's syndrome.
Hoffmann's syndrome is a rare manifestation of hypothyroid myopathy characterized by pseudohypertrophy, proximal muscle weakness and stiffness [6]. The syndrome is usually observed in patients with severe and untreated hypothyroidism, as in our case. Pseudohypertrophy is a rare presentation of hypothyroidism and its etiology remains obscure [4]. However, its mechanism involves an increase in the deposition of glucosaminoglycans and in the number and size of muscle fibers, as well as a change in muscle fiber type from fast twitch type II to slow twitch type I leading to delayed muscle contraction [7]. Previous reports on Hoffmann's syndrome showed that calf muscles are usually affected, but any part of the muscles could be involved including thigh, arm, and forearm [7]. The presence of calf muscle hypertrophy requires differential diagnosis from other diseases such as Duchenne and Becker muscle dystrophy, focal myositis, sarcoid granulomas, and amyloid deposits [4].
CK is the representative biochemical marker of myopathy [8]. However, CK is elevated even in patients with mild hypothyroidism regardless of the severity of myopathy [910]. Other enzymes such as aldolase, AST and LDH have a supportive role in the absence of hepatic dysfunction. The pathophysiology of elevated CK in hypothyroidism is not fully understood but, presumably, decreased CK clearance, a reversible defect in glycogenolysis and direct cell damage are the responsible factors [11]. Due to the decreased CK clearance, the resolution time of elevated CK is usually longer in hypothyroidism compared with patients with myocardial infarction [12]. The CK level in our patient decreased to normal after 2 months of thyroid hormone replacement.
Electrophysiological studies may reveal non-specific features suggestive of myopathic, neurogenic or mixed patterns in hypothyroid myopathy [6]. In Hoffmann's syndrome, myopathic patterns are observed, especially in calf muscles, as in our case [13]. Abnormal findings on electrophysiological study may persist in some patients despite the improvement of symptoms and muscle enzymes [6]. On biopsy, the affected muscles may show type I fiber hypertrophy as a compensatory response to type II fiber atrophy with increased numbers of central nuclei and increased connective tissue, which are the representative findings of hypothyroid myopathy [14].
Hoffmann's syndrome has a favorable prognosis after thyroid hormone replacement has been initiated. Clinical symptoms resolve slowly with time. It has been reported that the decline of CK to normal levels may not be a reliable indicator of the rate of recovery of hypothyroid myopathy. The decline of the muscle enzyme levels may occur slowly, varying from weeks, months, or even years [2].
If Hoffmann's syndrome presents without other manifestations of hypothyroidism, then a high degree of caution is necessary. Kaux et al. [15] reported a patient with Hoffmann's syndrome who presented emergently with severe asthenia and arthralgia without other prominent characteristics of hypothyroidism; in that case, early diagnosis and hormone replacement brought rapid stabilization.
This case emphasizes that hypothyroidism should be considered in the differential diagnosis of musculoskeletal symptoms in the absence of overt manifestations of hypothyroidism. Consideration of hypothyroidism and the routine measurement of serum TSH are important during the evaluation of patients with progressive muscle weakness and swelling.
Figures and Tables
Fig. 1
(A) Puffy face and preorbital swelling. (B) Edematous hands and lower legs. (C) Non-pitting edema of the lower extremities and hypertrophy of the calf muscles, with skin changes (dry coarse skin and hyperpigmentation). These photos were taken after obtaining prior consent from the patient.

Fig. 3
Electromyography showed mild spontaneous activity and short amplitude with polyphasic myopathic motor unit potential.

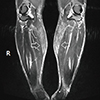
Fig. 4
Magnetic resonance imaging of the lower extremities shows symmetric multifocal patchy muscle enhancements with diffuse muscle swelling in both lower legs (superficial posterior compartment). Hypertrophy of the gastrocnemius; affected muscles show hyperintensity on T2-weighted images (arrows).
References
1. Khaleeli AA, Griffith DG, Edwards RH. The clinical presentation of hypothyroid myopathy and its relationship to abnormalities in structure and function of skeletal muscle. Clin Endocrinol (Oxf). 1983; 19:365–376.
2. Madariaga MG. Polymyositis-like syndrome in hypothyroidism: review of cases reported over the past twenty-five years. Thyroid. 2002; 12:331–336.
3. Ciompi ML, Zuccotti M, Bazzichi L, Puccetti L. Polymyositis-like syndrome in hypothyroidism: report of two cases. Thyroidology. 1994; 6:33–36.
4. Senanayake HM, Dedigama AD, De Alwis RP, Thirumavalavan K. Hoffmann syndrome: a case report. Int Arch Med. 2014; 7:2.
5. Qureshi W, Hassan G, Khan GQ, Kadri SM, Kak M, Ahmad M, et al. Hoffmann's syndrome: a case report. Ger Med Sci. 2005; 3:Doc05.
6. Vasconcellos LF, Peixoto MC, de Oliveira TN, Penque G, Leite AC. Hoffman's syndrome: pseudohypertrophic myopathy as initial manifestation of hypothyroidism. Case report. Arq Neuropsiquiatr. 2003; 61:851–854.
7. Nalini A, Govindaraju C, Kalra P, Kadukar P. Hoffmann's syndrome with unusually long duration: report on clinical, laboratory and muscle imaging findings in two cases. Ann Indian Acad Neurol. 2014; 17:217–221.
8. Giampietro O, Clerico A, Buzzigoli G, Del Chicca MG, Boni C, Carpi A. Detection of hypothyroid myopathy by measurement of various serum muscle markers: myoglobin, creatine kinase, lactate dehydrogenase and their isoenzymes. Correlations with thyroid hormone levels (free and total) and clinical usefulness. Horm Res. 1984; 19:232–242.
9. Graig FA, Smith JC. Serum creatine phosphokinase activity in altered thyroid states. J Clin Endocrinol Metab. 1965; 25:723–731.
10. Mastropasqua M, Spagna G, Baldini V, Tedesco I, Paggi A. Hoffman's syndrome: muscle stiffness, pseudohypertrophy and hypothyroidism. Horm Res. 2003; 59:105–108.
11. Finsterer J, Stollberger C, Grossegger C, Kroiss A. Hypothyroid myopathy with unusually high serum creatine kinase values. Horm Res. 1999; 52:205–208.
12. Klein I, Mantell P, Parker M, Levey GS. Resolution of abnormal muscle enzyme studies in hypothyroidism. Am J Med Sci. 1980; 279:159–162.
13. Tuncel D, Cetinkaya A, Kaya B, Gokce M. Hoffmann's syndrome: a case report. Med Princ Pract. 2008; 17:346–348.
14. Khaleeli AA, Gohil K, McPhail G, Round JM, Edwards RH. Muscle morphology and metabolism in hypothyroid myopathy: effects of treatment. J Clin Pathol. 1983; 36:519–526.
15. Kaux JF, Castermans C, Delmotte P, Bex M. Hoffmann syndrome presenting to the emergency department. Ann Readapt Med Phys. 2007; 50:310–312.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download