Abstract
Background
Current guidelines for follow-up of adrenal incidentalomas are extensive and hampered by lack of follow-up studies. We tested the hypothesis that small lipid-rich adrenal incidentalomas, initially characterized by tumor size <40 mm and <10 Hounsfield units (HUs) on unenhanced computed tomography (CT) may not demonstrate excessive growth/hormonal hypersecretion on follow-up.
Methods
Sixty-nine incidentalomas in 56 patients were restudied with unenhanced CT and screening for hypercortisolism (dexamethasone suppression test [DST], plasma adrenocorticotropic hormone) and pheochromocytoma (24-hour urinary metanephrines and normetanephrines) 5 years later. Primary hyperaldosteronism was excluded at base-line.
Results
Tumor (n=69) size was similar before and after 5 years follow-up (19±6 mm vs. 20±7 mm). Mean tumor growth was 1±2 mm. Largest increase in tumor size was 8 mm, this tumor was surgically removed and histopathology confirmed cortical adenoma. DST was normal in 54 patients and two patients (3.6%) were still characterized by subclinical hypercortisolism. Initial tumor size was >20 mm for the patient with largest tumor growth and those with subclinical hypercortisolism. All patients had normal 24-hour urinary metanephrines and normetanephrines. Low attenuation (<10 HU) was demonstrated in 97% of 67 masses re-evaluated with unenhanced CT.
Conclusion
None of the patients developed clinically relevant tumor growth or new subclinical hypercortisolism. Biochemical screening for pheochromocytoma in incidentalomas demonstrating <10 HU on unenhanced CT is not needed. For such incidentalomas <40 mm, it seems sufficient to perform control CT and screen for hypercortisolism after 5 years.
Adrenal incidentalomas are common with a prevalence ranging from 1% to 8.7% [123456]. Most authors recommend hormonal screening for pheochromocytoma and excessive cortisol secretion for all and screening for primary aldosteronism in hypertensive patients [6789]. Surgical resection is recommended for functional tumors and tumors greater than 40 mm in diameter. For smaller masses that are compatible with benign adenomas (<10 Hounsfield units, HU) on unenhanced computed tomography (CT), imaging and biochemical re-evaluation at 1 to 2 years is generally recommended [6789]. However, current guidelines on follow-up of adrenal incidentalomas are hampered by the lack of prospective studies.
We previously reported that, in the initial work-up of adrenal incidentalomas, pheochromocytoma can be ruled out based on an unenhanced attenuation value <10 HU on CT [10] and that it therefore is not necessary to also perform biochemical screening for pheochromocytoma for such lipid-rich incidentalomas. However, the long-term natural history of adrenal incidentalomas is not well characterized and there are open questions, such as whether imaging findings may predict who should or should not undergo further testing, what percentage of incidentalomas will increase in size to ≥40 mm over time and when hypercortisolism or subclinical hypercortisolism will develop. Morelli et al. [11] recently published a large retrospective study on 206 patients with adrenal incidentalomas and concluded that initial adenoma size >24 mm associates with future development of subclinical hypercortisolism. However, the study did not include data on unenhanced CT, and did not evaluate the subgroup of lipid-rich adrenal incidentalomas. Furthermore, the retrospective design of the study does not allow for a standardized study protocol [11].
The present study was undertaken to evaluate the hypothesis that lipid-rich adrenal incidentalomas, a hallmark of benign adrenal adenomas, may not show excess growth and/or develop excess hormonal secretion during short-term follow-up and that it might be possible to re-evaluate them after 5-year follow-up instead of at 1 to 2 years intervals. If this would be the case, it would allow for a less extensive and more cost-effective follow-up scheme for such adrenal incidentalomas in the future. We prospectively evaluated our cohort of adrenal incidentalomas initially characterized by a low unenhanced CT value (<10 HU) and tumor size <40 mm [10] for rate and extent of tumor growth, evaluated possible excess cortisol secretion (serum cortisol >100 nmol/L after a 1 mg dexamethasone suppression test [DST] and measured plasma adrenocorticotropic hormone [ACTH; <10 ng/L]), screened for pheochromocytoma by measuring 24-hour urinary metanephrines and normetanephrines and re-evaluated the HU units of these incidentalomas with unenhanced CT 5 years later. We invited all patients (n=78) of our original cohort [10] who did not undergo surgery or, who after unilateral adrenalectomy had a lipid-rich adrenal incidentaloma in their remaining adrenal gland. Primary hyperaldosteronism had been ruled out in all of these patients at baseline and was not re-studied. Fifty-six patients with altogether 69 adrenal masses agreed to participate. All patients underwent repeat CT, biochemical screening and clinical examination. The results of the follow-up study were compared to those at baseline.
The study material consists of 56 patients, who all belong to the original cohort of 115 patients who were referred to the outpatient Department of Endocrinology at the Helsinki University Central Hospital between 1 January 2007 and 31 December 2009 because of an adrenal mass. Of the 115 patients, 15 underwent surgery after initial work-up. The patients participating in the present study all had a follow-up of at least 5 years. The adrenal masses had been detected incidentally on abdominal or chest CT in all cases. Only adrenal masses of 10 mm or more were included in the study. Patients diagnosed with or treated for any cancer within 5 years were excluded from the primary study [10]. The patients underwent clinical examination (CSJ and TS), repeat non-contrast CT imaging as well as measurements of 24-hour urinary metanephrines and normetanephrines, a 1 mg DST test and measurements of plasma ACTH.
CT imaging data was evaluated by an experienced adrenal radiologist (MR). All study subjects underwent repeat adrenal CT imaging at the Department of Radiology at the Helsinki University Central Hospital using a 64-slice CT scanner and a 3 mm reconstructed slice thickness in the axial and coronal plane. Maximal diameter of the adrenal mass was determined with a distance cursor in the axial plane of the CT scan. The density of the adrenal mass expressed as HU values was measured from unenhanced CT scans by placing a circular region-of-interest (ROI) cursor on each mass. The diameter of ROI was dependent of the size of the mass and a ROI as large as possible still avoiding the edges of the mass was always used. Measurement of each mass was done mostly thrice and the mean value was used in analysis. None of the tumors had become cystic or necrotic during follow-up.
Laboratory measurements were performed at HUSLAB, the laboratory of the Helsinki University Central Hospital. For biochemical evaluation of pheochromocytoma, 24-hour urine collections were performed in all study subjects and fractionated urinary metanephrine (reference value <1.7 µmol) and normetanephrine (reference value <4.0 µmol) were measured by high pressure liquid chromotography (HPLC) as previously described [10]. For evaluation of autonomous cortisol production, an overnight DST was performed with a dose of 1 mg taken at 11:00 PM, blood samples for determination of serum cortisol were drawn at 8:00 AM the following morning. Serum cortisol was measured using a chemiluminescent microparticle immunoassay (Abbott Architect i2000SR analyser, Abbott Diagnostics, Lake Forest, IL, USA) and plasma ACTH with a chemiluminescent immunometric assay (Immulite 2000 Xpi, Siemens Healthcare Diagnostics, Munich, Germany). The cut-off criteria for autonomous cortisol production were impaired suppression of serum cortisol >100 nmol/L after an overnight 1 mg DST and a low plasma ACTH concentration of <10 ng/L (reference value <46).
At baseline aldosterone overproduction was excluded in all hypertensive patients by measuring plasma renin activity and serum aldosterone with RIA and using increased aldosterone to renin ratio (>800) and an increased diurnal aldosterone excretion (>40 nmol) as criteria for aldosterone overproduction. These data have been presented in a previous study of the cohort [10].
The study was approved by the Ethics Committee of the Helsinki University Central Hospital and the Board of the Department of Internal Medicine. All results are given as mean±SD. The statistical difference between the subgroups was analyzed with the Student t test or Mann-Whitney U test when appropriate and with chi-square for categorical data. Paired t test were used to analyse the differences between baseline and follow-up. Statistical analyses were performed with the SPSS version 19.0 (IBM Co., Armonk, NY, USA). A P<0.05 was considered statistically significant.
A flowsheet depicting the original cohort and the 56 patients comprising the present study cohort is given in Fig. 1. The patients participating in the follow-up study had altogether 69 adrenal masses. Characteristics of patients are given in Table 1. Of all study patients, 44 (78%) had one, 11 (20%) had two, and one patient (2%) three separate adrenal incidentalomas. Of all 69 adrenal masses, 23 (33%) were located in the right adrenal gland and 46 (67%) in the left adrenal gland.
Mean change in tumor size after follow-up for the whole cohort was 1±2 mm (P<0.001) (Table 1). Change in tumor size ranged from -4 to 8 mm (Fig. 2). Five masses (7.2%) demonstrated a decrease in tumor size of 1 to 4 mm. When the incidentalomas were divided into two groups based on tumor size at baseline (<20 or ≥20 mm), the mean change in size was 0.3 and 1.9 mm, respectively (Table 1). The tumor disposing the largest tumor growth of 8 mm during follow-up was also the largest one (39 mm) after follow-up. It was non-functional and characterized by a density of <10 HU at follow-up. The patient, a female aged 67 years, underwent laparoscopic adrenalectomy and histopathological examination demonstrated a cortical adenoma. For all other masses, size at 5 years follow-up remained <37 mm.
At baseline, all masses were characterized by <10 HU attenuation on CT. After 5 years follow-up (Table 1), 66 of 69 masses (96 %), for which evaluation of HU on nonenhanced CT was available were characterized by <10 HU. Three incidentalomas classified as lipid-rich adenomas at baseline had 5-year follow-up HU values of 10, 10, and 22, respectively. At baseline, the mean diameter of these masses was 19±6 mm (range, 10 to 34) and the corresponding diameter after follow-up was 20±7 mm (range, 10 to 39). Fig. 3 demonstrates the typical CT findings of one of the adrenal incidentalomas of the present series after follow-up.
In the whole cohort, at the end of follow-up, mean serum cortisol concentration after 1 mg DST was 44±22 nmol/L and mean basal plasma ACTH 15±8 ng/L. Morning serum cortisol after 1 mg DST was <50, 50 to 100, and >100 nmol/L in 33, 19, and 2 patients, respectively. Corresponding plasma ACTH concentrations in patients with normal (<50 nmol/L) or subnormal (50 to 100 nmol/L) serum cortisol after the 1 mg DST were 16.2±8.1 ng/L versus 14.5±8.5 ng/L, respectively (not significant).
Two females aged 62 and 70 years had non-suppressed serum cortisol concentrations of 110 and 167 nmol/L after 1 mg DST, respectively and both of them also had low plasma ACTH concentrations (6 and <5 ng/L, respectively). These patients had had biochemical findings indicating subclinical hypercortisolism also at baseline, but had rejected operation at that time. Neither of them had any clinical signs of hypercortisolism. Their body mass index was 30.8 and 28.7 kg/m2, respectively. They both had normal blood pressure and they did not have type 2 diabetes. The 62-year-old female underwent surgery, and a cortical adenoma was confirmed. The 70-year-old female did not want surgery and she was scheduled for further follow-up. None of the other patients fulfilled the biochemical criteria for subclinical hypercortisolism. Thus, the conversion rate to subclinical hypercortisolism after 5 years follow-up was 0%.
As shown in Table 1, none of the patients had increased 24-hour fractionated urinary metanephrine or normetanephrine concentrations after 5 years of follow-up. Urinary metanephrine concentrations ranged from 0.2 to 1.1 µmol/L (reference value <1.7) and normetanephrines from 0.1 to 2.2 µmol/L (reference value <4).
This is the first prospective study on lipid-rich adrenal incidentalomas. The main findings of the present study are that there was no relevant tumor growth after 5 years of follow-up and that the conversion rate to subclinical or clinical hypercortisolism was zero. In addition, we could confirm that pheochromocytoma is outruled in such adrenal incidentalomas also after medium-term follow-up, as measurements of 24-hour fractionated metanephrines and normetanephrines were normal.
The recommendations for initial diagnostic work-up of adrenal incidentalomas are fairly uniform [789121314]. The different algorithms currently proposed for follow-up of adrenal incidentalomas are rather extensive and hampered by the lack of prospective follow-up studies [789121314]. There are several open questions regarding what percentage of incidentalomas will increase in size to ≥40 mm over time, when hypercortisolism or subclinical hypercortisolism will occur, as well as whether imaging findings could predict who should or should not undergo further testing.
Most authors recommend continuous annual screening for hyperfunction up to 4 to 5 years and one to three interval CT scans to evaluate potential tumor growth. The initial work-up should adequately identify all potentially malignant and hormonally active adrenal tumors in order to refer these patients for surgery. The follow-up scheme should confirm the benign nature of the adrenal mass and, alternatively, identify malignant transformation and ensure that the adrenal mass does not become hormonally active. The follow-up strategy should not only be safe but also cost-effective, avoiding unnecessary and expensive investigations of patients who do not need such investigations.
In our 5-year prospective follow-up study of altogether 69 incidentally found lipid-rich adrenal masses in 56 patients, we demonstrate that mean growth of all lipid-rich adrenal masses was only 1±2 mm, i.e., not significant. Some of these adrenal masses even decreased in size over time. A limitation of the present study is the fairly small number of patients (n=56) and adrenal masses (n=69). Therefore, future prospective studies including larger numbers of lipid-rich adrenal tumors are warranted. However, in line with the present study, we did not observe tumor growth in our larger initial cohort including 174 patients and 214 lipid-rich adrenal masses during 15.8 months of follow-up [10].
In the present study, the tumor demonstrating the largest increase in diameter, 8 mm, was also the largest one (39 mm) at the end of follow-up. The patient harbouring this tumor underwent laparoscopic surgery and histopathology confirmed a benign cortical adenoma. When the patients were divided into two groups based on initial tumor size <20 or ≥20 mm, we found that none of the tumors (35 tumors, 26 patients) characterized by initial tumor size <20 mm demonstrated clinically significant tumor growth during follow-up and none had or developed subclinical hypercortisolism.
Another important finding of the present study is that the conversion rate to subclinical hypercortisolism in such lipid-rich adrenal incidentalomas was 0%. Two patients (3.6%) who were biochemically characterized by subclinical hypercortisolism at baseline had subclinical hypercortisolism also after 5 years of follow-up. None of the patients developed overt hypercortisolism. While one of these females was operated on and histopathology demonstrated a benign adenoma, the other female did not want surgery. These females did not show clinical signs of hypercortisolism and had not developed type 2 diabetes or hypertension during follow-up. In the future, further studies including larger sample size are needed to confirm these results.
The present study also confirms our previous finding [10] that pheochromocytoma does not underlie homogenous tumors originally characterized by a HU <10 on non-contrast CT. It is not necessary to perform biochemical screening for pheochromocytoma in such tumors, neither at baseline nor at follow-up.
The NIH consensus statement from 2002 [7] suggest initial endocrine testing with 1 mg DST, plasma free metanephrines and measurement of potassium and screening for aldosterone overproduction in hypertensive patients. Annual biochemical screening for 4 years is recommended in masses <4 cm, with two repeat CTs at least 6 months apart. The algorithm proposed be Young [3] in 2007 is very similar, recommending initial testing with 1 mg DST, urinary metanephrines and catecholamines, potassium and screening for aldosterone overproduction in hypertensive patients. According to this algorithm, biochemical screening should also be performed yearly for 4 years and masses <4 cm should be monitored by CT at 6, 12, and 24 months. The French Society of Endocrinology recommend similar initial endocrine testing in their consensus statement of 2008 [12], with repeat 1 mg DST and plasma and urinary metanephrines at 6 months, thereafter repeat 1 mg DST at 2 and 5 years, while CT imaging of masses <4 cm is recommended at 6 months, 2 and 5 years.
The American Association of Clinical Endocrinologists/American Association of Endocrine Surgeons Medical Guidelines from 2009 [13] is rather extensive, recommending screening for aldosterone overproduction in hypertensive patients and otherwise endocrine testing annually for 5 years and imaging re-evaluation of masses <4 cm at 3 to 6 months and then annually for 1 to 2 years. Nieman [9] recommends annual endocrine testing (except for aldosteronism if excluded at baseline) for 4 years in masses <3 cm, non-functional and benign as characterized by imaging at 1 to 2 years. She suggests imaging monitoring of masses <4 cm at 1 to 2 years and the use of additional imaging criteria in addition to size. Imaging is recommended at 1 to 2 years or more and when needed at 3 to 6 months.
In the Italian Association of Clinical Endocrinologists' (AME) position paper from 2011 [6], frequency and duration of repeat endocrine testing is recommended to be judged individually, after clinical monitoring. Imaging characteristics other than size should be included and masses 2 to 4 cm in size should be monitored. CT or magnetic resonance imaging (MRI) is recommended at 3 to 6 months, thereafter, no repeat imaging is recommended in masses <2 cm with benign features, while imaging of masses >2 cm is recommended on an individual base.
Lastly, in their review from 2012, Arnaldi and Boscaro [14] recommend annual biochemical screening for 5 years (except for aldosterone overproduction), monitoring of masses <4 cm with CT or MRI and the use of additional imaging criteria in addition to size. Repeat imaging is recommended at 6 months.
In conclusion, this is the first 5-year follow-up study on the natural course of lipid-rich adrenal incidentalomas <40 mm, not characterized by overt hypercortisolism or aldosteronism at baseline. The results indicate that it is not necessary to biochemically screen for pheochromocytoma in patients with such incidentalomas and that their next follow-up can be scheduled 5 years ahead and should include an unenhanced CT and screening for hypercortisolism. It is debatable whether further screening is needed at all in elderly subjects with lipid-rich incidentalomas <2 cm in size. The results of the present study should, however, be confirmed in future studies including larger patient numbers.
Figures and Tables
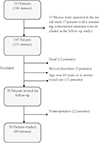 | Fig. 1The original study cohort with adrenal incidentaloma and number of patients and adrenal masses eligible for the 5-year follow-up study. |
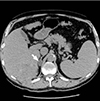 | Fig. 3Unenhanced computed tomography of a typical adrenal incidentaloma (arrow) on the right. Placement of region of interest (ROI) cursor for measurement of Hounsfield units (HU) is also shown. HU was negative. |
Table 1
Characteristics of 56 Patients with 69 Lipid-Rich Adrenal Incidentalomas (<10 HU)
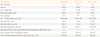
Values are expressed as mean±SD unless other indicated. Data for incidentalomas <2 and ≥2 cm in diameter is given separately.
HU, Hounsfield unit; DST, dexamethasone suppression test.
aP<0.001; bP<0.01 and for difference between subgroups; cTwo patients with subclinical hypercortisolism at baseline were excluded from these data.
ACKNOWLEDGMENTS
The technical help of Ms. Marketta Halinen is greatfully acknowledged. This study was supported by grants from Research Funding of Helsinki University Hospital (erityisvaltionosuus).
References
1. Bulow B, Ahren B. Swedish Research Council Study Group of Endocrine Abdominal Tumours. Adrenal incidentaloma: experience of a standardized diagnostic programme in the Swedish prospective study. J Intern Med. 2002; 252:239–246.
2. Barzon L, Sonino N, Fallo F, Palu G, Boscaro M. Prevalence and natural history of adrenal incidentalomas. Eur J Endocrinol. 2003; 149:273–285.
3. Young WF Jr. Clinical practice: the incidentally discovered adrenal mass. N Engl J Med. 2007; 356:601–610.
4. Terzolo M, Bovio S, Pia A, Reimondo G, Angeli A. Management of adrenal incidentaloma. Best Pract Res Clin Endocrinol Metab. 2009; 23:233–243.
5. Zeiger MA, Siegelman SS, Hamrahian AH. Medical and surgical evaluation and treatment of adrenal incidentalomas. J Clin Endocrinol Metab. 2011; 96:2004–2015.
6. Terzolo M, Stigliano A, Chiodini I, Loli P, Furlani L, Arnaldi G, et al. AME position statement on adrenal incidentaloma. Eur J Endocrinol. 2011; 164:851–870.
7. Grumbach MM, Biller BM, Braunstein GD, Campbell KK, Carney JA, Godley PA, et al. Management of the clinically inapparent adrenal mass ("incidentaloma"). Ann Intern Med. 2003; 138:424–429.
8. Thompson GB, Young WF Jr. Adrenal incidentaloma. Curr Opin Oncol. 2003; 15:84–90.
9. Nieman LK. Approach to the patient with an adrenal incidentaloma. J Clin Endocrinol Metab. 2010; 95:4106–4113.
10. Sane T, Schalin-Jantti C, Raade M. Is biochemical screening for pheochromocytoma in adrenal incidentalomas expressing low unenhanced attenuation on computed tomography necessary? J Clin Endocrinol Metab. 2012; 97:2077–2083.
11. Morelli V, Reimondo G, Giordano R, Della Casa S, Policola C, Palmieri S, et al. Long-term follow-up in adrenal incidentalomas: an Italian multicenter study. J Clin Endocrinol Metab. 2014; 99:827–834.
12. Tabarin A, Bardet S, Bertherat J, Dupas B, Chabre O, Hamoir E, et al. Exploration and management of adrenal incidentalomas. French Society of Endocrinology Consensus. Ann Endocrinol (Paris). 2008; 69:487–500.
13. Zeiger MA, Thompson GB, Duh QY, Hamrahian AH, Angelos P, Elaraj D, et al. The American Association of Clinical Endocrinologists and American Association of Endocrine Surgeons medical guidelines for the management of adrenal incidentalomas. Endocr Pract. 2009; 15:Suppl 1. 1–20.
14. Arnaldi G, Boscaro M. Adrenal incidentaloma. Best Pract Res Clin Endocrinol Metab. 2012; 26:405–419.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download