Abstract
Background
We wanted to evaluate whether a minimal extrathyroid extension (METE) is associated with the clinicopathological parameters that are indicative of a poor prognosis, including lymph node metastasis, distant metastasis at the time of the initial diagnosis and tumor recurrence, in patients with papillary thyroid carcinoma (PTC), and especially in the patients with papillary thyroid microcarcinoma (PTMC).
Methods
We retrospectively evaluated the medical records of patients with PTC and who had undergone total thyroidectomy with/ without subsequent 131 I remnant ablation at the Korea Cancer Center Hospital from January 1998 through December 2005. A total of 557 patients with PTC were enrolled in the study. We excluded 13 patients with an unknown status of extension and 29 patients with massive ETE.
Results
Of the 515 patients, 401 were found to have a METE. We analyzed the 464 patients who were without distant metastasis at the time of the initial diagnosis and who had a follow-up duration of more than 6 months. METE was not significantly associated with tumor recurrence during the follow-up period (median follow-up period: 122 months, range: 6–142 months): 8% vs. 15% of the patients with and without METE had tumor recurrence, respectively (P = 0.069 by the log–rank test). We analyzed the effect of tumor size in the patients with METE. Size was not significantly associated with tumor recurrence (P = 0.374 by the log–rank test).
References
1. Ortiz S, Rodriguez JM, Soria T, Perez-Flores D, Pinero A, Moreno J, Parrilla P. Extrathyroid spread in papillary carcinoma of the thyroid: clinicopathological and prognostic study. Otolaryngol Head Neck Surg. 124:261265. 2001.

2. Andersen PE, Kinsella J, Loree TR, Shaha AR, Shah JP. Differentiated carcinoma of the thyroid with extrathyroidal extension. Am J Surg. 170:467–470. 1995.

3. Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol. 17:1471–1474. 2010.

4. Byar DP, Green SB, Dor P, Williams ED, Colon J, van Gilse HA, Mayer M, Sylvester RJ, van Glabbeke M. A prognostic index for thyroid carcinoma. A study of the E.O.R.T.C. Thyroid Cancer Cooperative Group. Eur J Cancer. 15:1033–1041. 1979.

5. Cady B, Rossi R. An expanded view of risk-group definition in differentiated thyroid carcinoma. Surgery. 104:947–953. 1988.
6. DeGroot LJ, Kaplan EL, McCormick M, Straus FH. Natural history, treatment, and course of papillary thyroid carcinoma. J Clin Endocrinol Metab. 71:414–424. 1990.

7. Hay ID, Bergstralh EJ, Goellner JR, Ebersold JR, Grant CS. Predicting outcome in papillary thyroid carcinoma: development of a reliable prognostic scoring system in a cohort of 1,779 patients surgically treated at one institution during 1940 through 1989. Surgery. 114:1050–1057. 1993.
8. Arora N, Turbendian HK, Scognamiglio T, Wagner PL, Goldsmith SJ, Zarnegar R, Fahey TJ 3rd. Extrathyroidal extension is not all equal: implications of macroscopic versus microscopic extent in papillary thyroid carcinoma. Surgery. 144:942–947. 2008.

9. Hu A, Clark J, Payne RJ, Eski S, Walfish PG, Freeman JL. Extrathyroidal extension in well-differentiated thyroid cancer: macroscopic vs microscopic as a predictor of outcome. Arch Otolaryngol Head Neck Surg. 133:644649. 2007.
10. Ito Y, Tomoda C, Uruno T, Takamura Y, Miya A, Kobayashi K, Matsuzuka F, Kuma K, Miyauchi A. Minimal extrathyroid extension does not affect the relapse-free survival of patients with papillary thyroid carcinoma measuring 4 cm or less over the age of 45 years. Surg Today. 36:12–18. 2006.
11. Ito Y, Tomoda C, Uruno T, Takamura Y, Miya A, Kobayashi K, Matsuzuka F, Kuma K, Miyauchi A. Prognostic significance of extrathyroid extension of papillary thyroid carcinoma: massive but not minimal extension affects the relapse-free survival. World J Surg. 30:780–786. 2006.

12. Leboulleux S, Rubino C, Baudin E, Caillou B, Hartl DM, Bidart JM, Travagli JP, Schlumberger M. Prognostic factors for persistent or recurrent disease of papillary thyroid carcinoma with neck lymph node metastases and/or tumor extension beyond the thyroid capsule at initial diagnosis. J Clin Endocrinol Metab. 90:5723–5729. 2005.

13. Baudin E, Travagli JP, Ropers J, Mancusi F, Bruno-Bossio G, Caillou B, Cailleux AF, Lumbroso JD, Parmentier C, Schlumberger M. Microcarcinoma of the thyroid gland: the Gustave-Roussy Institute experience. Cancer. 83:553–559. 1998.
14. Chow SM, Law SC, Chan JK, Au SK, Yau S, Lau WH. Papillary microcarcinoma of the thyroid-Prognostic significance of lymph node metastasis and multifocality. Cancer. 98:31–40. 2003.

15. Kim TY, Hong SJ, Kim JM, Kim WG, Gong G, Ryu JS, Kim WB, Yun SC, Shong YK. Prognostic parameters for recurrence of papillary thyroid microcarcinoma. BMC Cancer. 8:296. 2008.

16. Mercante G, Frasoldati A, Pedroni C, Formisano D, Renna L, Piana S, Gardini G, Valcavi R, Barbieri V. Prognostic factors affecting neck lymph node recurrence and distant metastasis in papillary microcarcinoma of the thyroid: results of a study in 445 patients. Thyroid. 19:707–716. 2009.

17. Pelizzo MR, Boschin IM, Toniato A, Piotto A, Bernante P, Pagetta C, Rampin L, Rubello D. Papillary thyroid microcarcinoma (PTMC): prognostic factors, management and outcome in 403 patients. Eur J Surg Oncol. 32:1144–1148. 2006.

18. Pellegriti G, Scollo C, Lumera G, Regalbuto C, Vigneri R, Belfiore A. Clinical behavior and outcome of papillary thyroid cancers smaller than 1.5 cm in diameter: study of 299 cases. J Clin Endocrinol Metab. 89:37133720. 2004.

19. Perrino M, Vannucchi G, Vicentini L, Cantoni G, Dazzi D, Colombo C, Rodari M, Chiti A, Beck-Peccoz P, Fugazzola L. Outcome predictors and impact of central node dissection and radiometabolic treatments in papillary thyroid cancers < or =2 cm. Endocr Relat Cancer. 16:201–210. 2009.
20. Cross S, Wei JP, Kim S, Brams DM. Selective surgery and adjuvant therapy based on risk classifications of well-differentiated thyroid cancer. J Surg Oncol. 94:678–682. 2006.

22. American Thyroid Association (ATA) Guidelines Taskforce on Thyroid Nodules and Differentiated Thyroid Cancer. Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, Mazzaferri EL, McIver B, Pacini F, Schlumberger M, Sherman SI, Steward DL, Tuttle RM. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 19:1167–1214. 2009.

23. Hay ID, Grant CS, Taylor WF, McConahey WM. Ipsilateral lobectomy versus bilateral lobar resection in papillary thyroid carcinoma: a retrospective analysis of surgical outcome using a novel prognostic scoring system. Surgery. 102:1088–1095. 1987.
24. Shaha AR, Loree TR, Shah JP. Intermediate-risk group for differentiated carcinoma of thyroid. Surgery. 116:1036–1040. 1994.
25. Cheema Y, Repplinger D, Elson D, Chen H. Is tumor size the best predictor of outcome for papillary thyroid cancer? Ann Surg Oncol. 13:1524–1528. 2006.

26. Orlov S, Orlov D, Shaytzag M, Dowar M, Tabatabaie V, Dwek P, Yip J, Hu C, Freeman JL, Walfish PG. Influence of age and primary tumor size on the risk for residual/recurrent well-differentiated thyroid carcinoma. Head Neck. 31:782–788. 2009.

Fig. 1.
Disease-free survival according to extrathyroid extension in 464 patients who were without distant metastasis at the time of the initial diagnosis. The Kaplan-Meier method for recurrence with the log rank test was used for statistical comparisons.
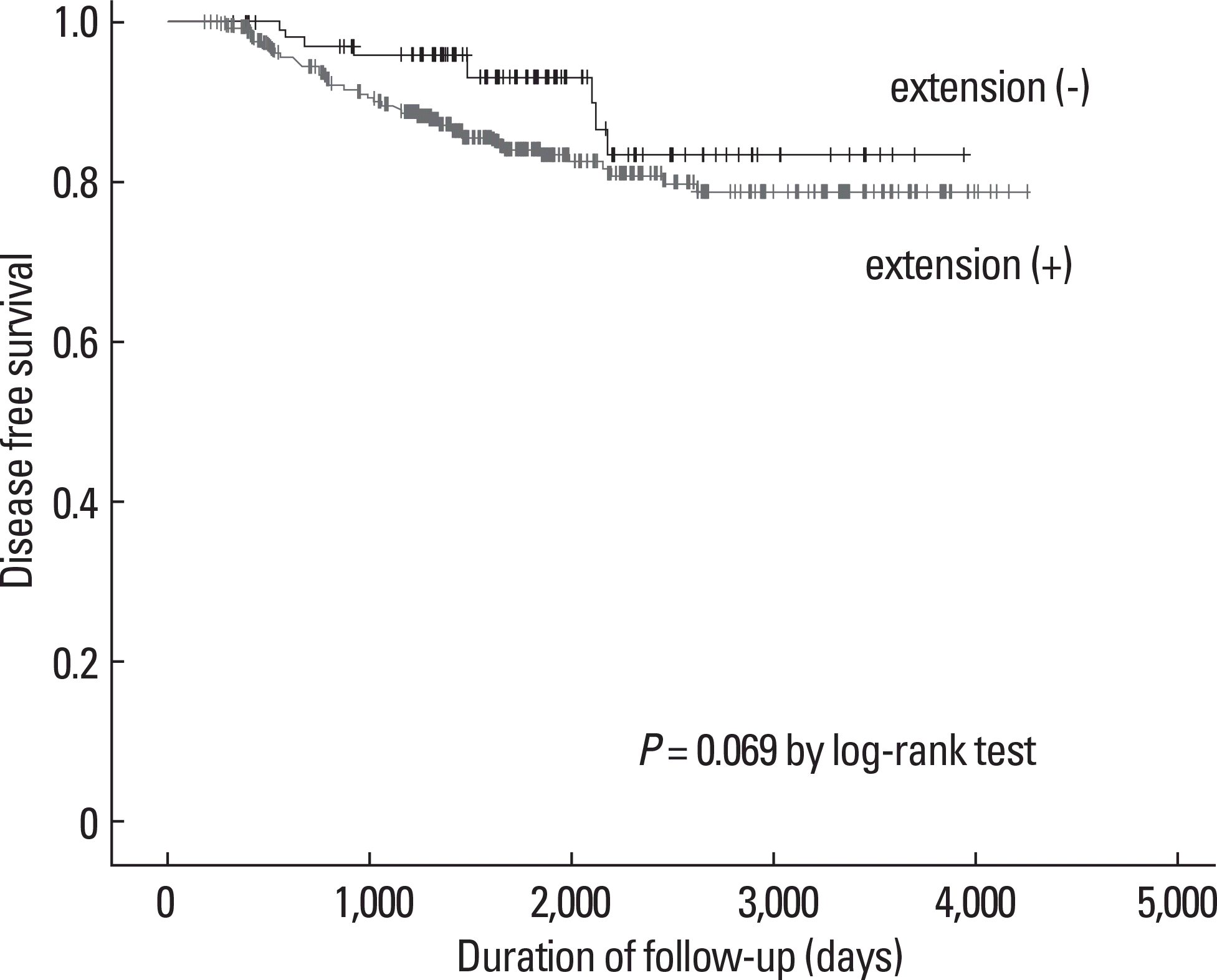
Fig. 2.
Disease-free survival according to extrathyroid extension in the 429 patients with tumor smaller than 4 cm and without distant metastasis at the time of the initial diagnosis. The Kaplan-Meier method for recurrence with the log rank test was used for statistical comparisons.
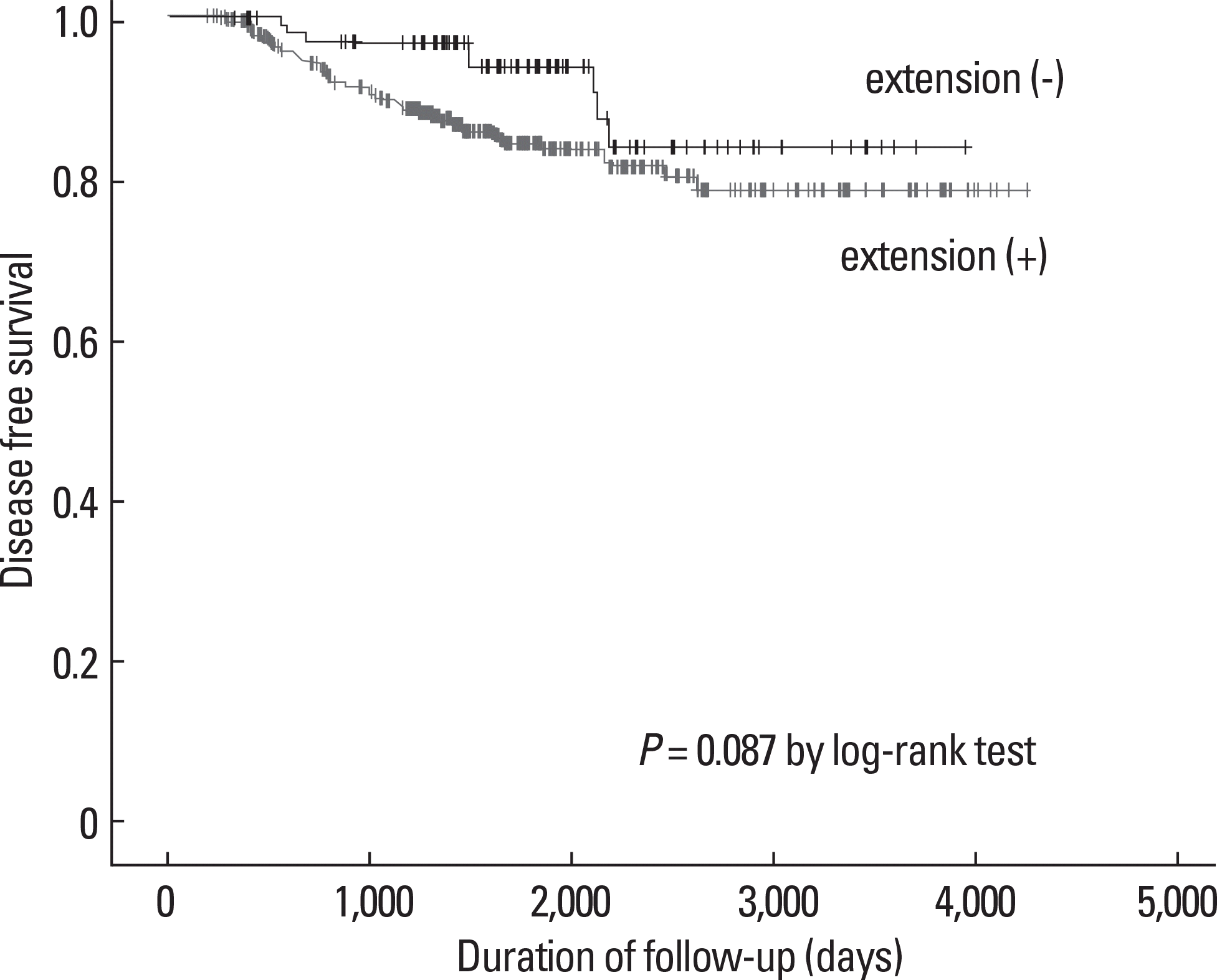
Fig. 3.
Disease-free survival according to extrathyroid extension in the 121 patients with papillary thyroid microcarcinoma and without distant metastasis at the time of the initial diagnosis. The Kaplan-Meier method for recurrence with the log rank test was used for statistical comparisons.
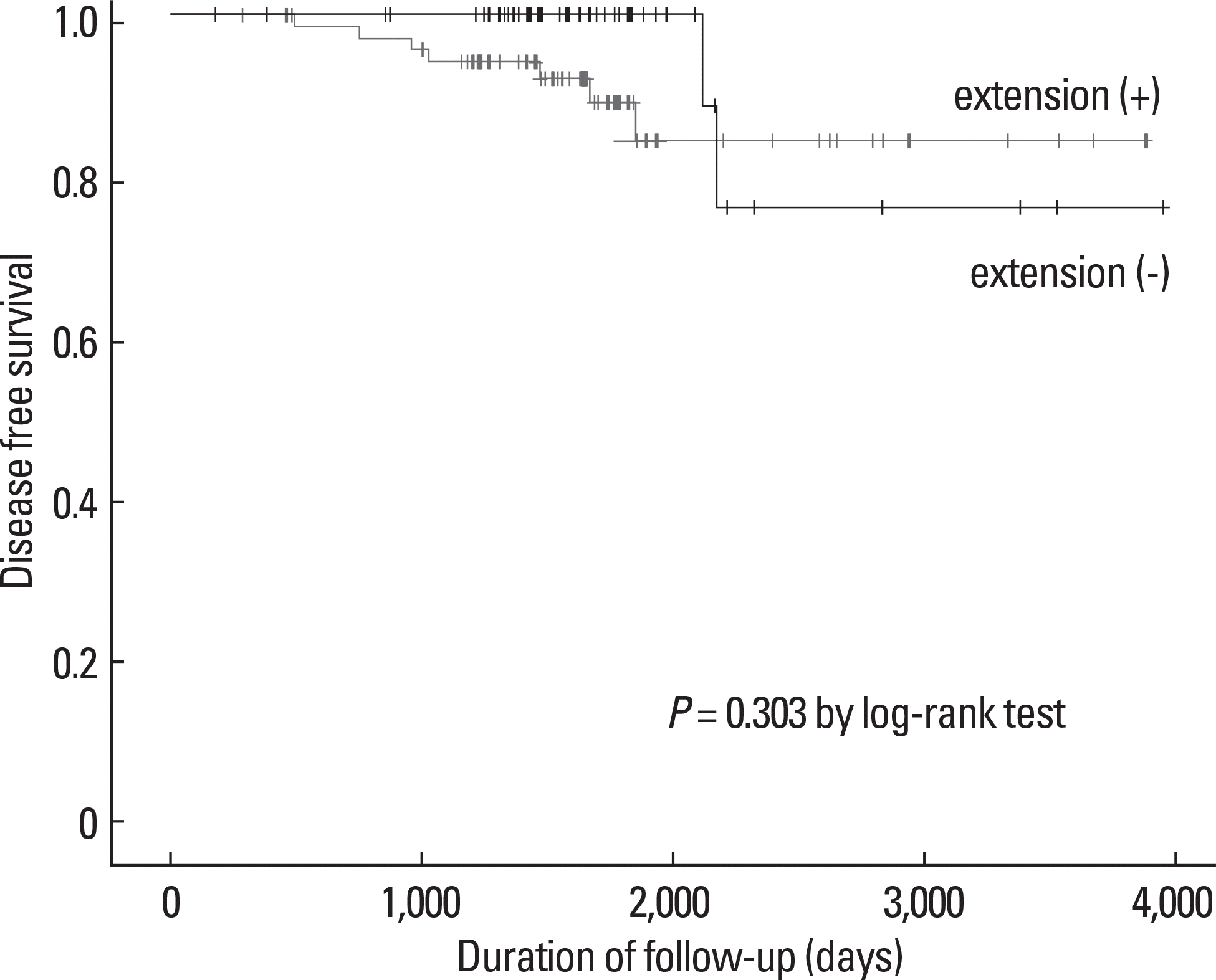
Fig. 4.
Disease-free survival according to tumor size in the 358 patients with tumor with minimal extrathyroid extension and without distant metastasis at the time of the initial diagnosis. The Kaplan-Meier method for recurrence with the log rank test was used for statistical comparisons.
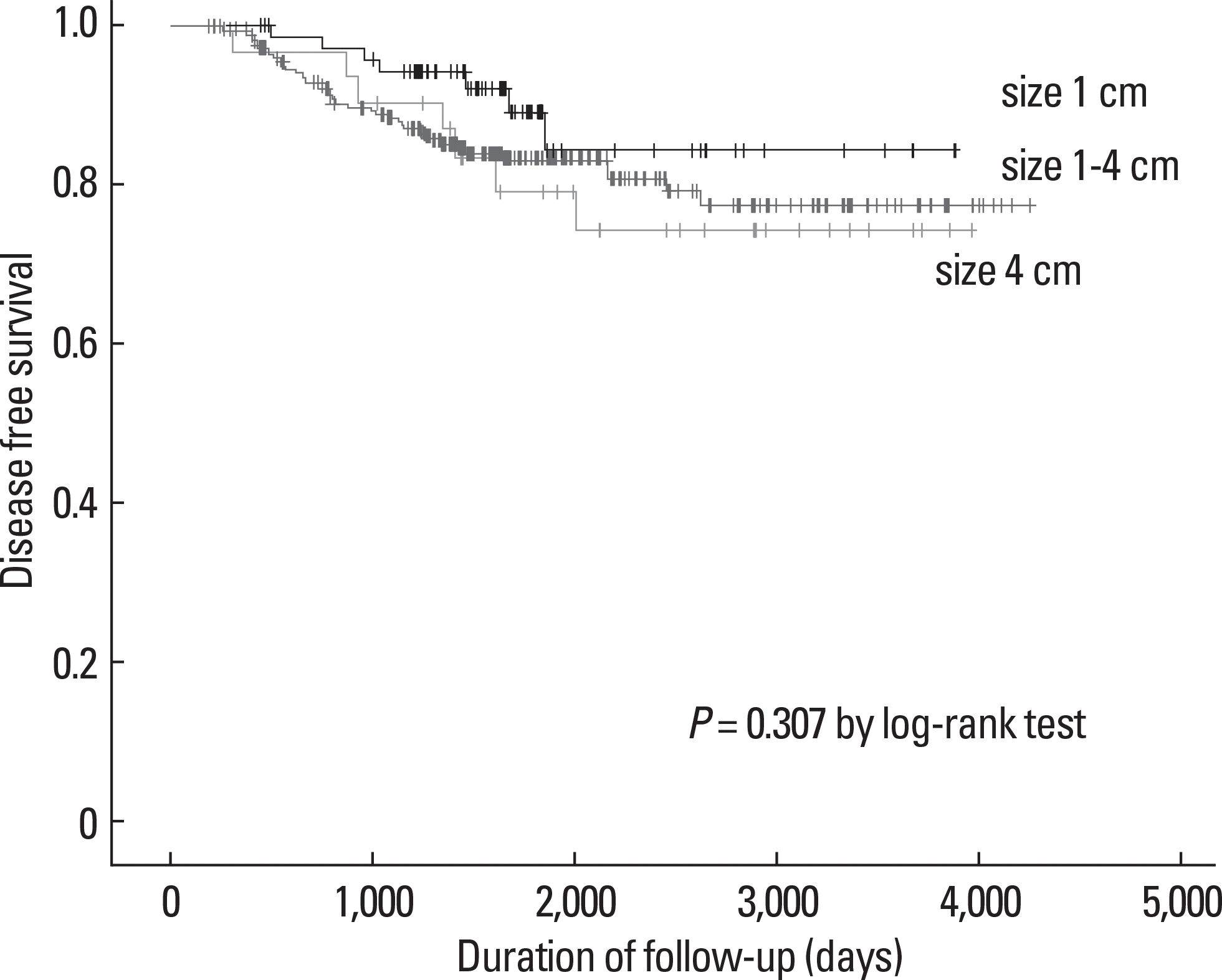
Table 1.
The clinicopathological characteristics according to the presence of minimal extrathyroid extension
| Clinicopathological parameters | METE- (n = 114) | METE+ (n = 401) | P-value |
|---|---|---|---|
| Age (years) | 45 ± 12 | 47 ± 13 | 0.057‡ |
| Gender (M:F) | 16:98 | 81:320 | 0.174§ |
| Size (cm) | 1.5 ± 1.3 | 2.2 ± 1.5 | < 0.001 |
| Lymph node metastasis | 0.015 | ||
| No metastasis | 41 (36) | 93 (23) | |
| Metastasis to central cervical lymph node* | 45 (40) | 168 (42) | |
| Metastasis to lateral cervical lymph node† | 28 (24) | 140 (35) | |
| Distant metastasis | 0.059§ | ||
| Absent | 112 (98) | 376 (94) | |
| Present | 2 (2) | 25 (6) | |
| 131 I Remnant ablation | 0.057§ | ||
| No | 11 (10) | 20 (5) | |
| Yes | 103 (90) | 381 (95) |
* Central cervical lymph nodes are defined as lymph nodes of level VI (i.e., the pretracheal, paratracheal, and prelaryngeal/Delphian lymph nodes), and these are classified as N1a in 2010 TNM staging.
Table 2.
Multivariate analysis of the associations between minimal extrathyroid extension and various clinicopathological parameters




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download