Abstract
With a developing worldwide epidemic of diabetes mellitus, the renal complications associated with diabetes have become a serious health concern. Primary therapy for treating diabetic nephropathy is a multifactorial process. Peroxisome proliferator-activated receptor alpha (PPARα) agonists have been used primarily in clinical practice for the treatment of dyslipidemia and insulin resistance. Given that PPARα expression and regulation of metabolic pathways are involved in oxidative stress, inflammation, blood pressure regulation, and the renin-angiotensin aldosterone system, PPARα likely influences the development and pathogenesis of diabetic nephropathy via indirect effects on glucose and lipid homeostasis and also by direct action on the kidneys. These findings suggest that PPARα may become an important therapeutic target for treating diabetic renal complications.
Peroxisome proliferator-activated receptors (PPAR) are ligand-activated transcription factors that are members of the nuclear hormone receptor superfamily [1,2]. There are three PPAR isoforms of the distinct genes commonly designated as PPARα (NR1C1), PPARγ (NR1C3) and PPARβ/δ (NR1C2) (or simply δ) [1]. The identification and designation of this PPAR subfamily of nuclear receptors in the 1990s was the result of over 25 cumulative years of work with peroxisome proliferators [2]. The PPARs heterodimerize with another nuclear receptor, the 9-cis-retinoic acid receptor (RXR), to form a complex that interacts with specific DNA-response elements within the promoter regions of the target genes. This heterodimer complex is activated by appropriate ligand binding, so it can therefore recruit transcription coactivators and oversee the transcription of genes involved in the regulation of lipid and carbohydrate metabolism [3].
Tissue expressions differ based on the PPAR subtype [4,5]. PPARα is highly expressed in the liver, renal cortex, intestinal mucosa, and heart, which are all organs that possess high mitochondrial and β-oxidation activity. Lower expression of PPARα is also observed in several other tissues. Similar tissue expression profiles of PPARα have been found in rodents and humans [4]. PPARα is abundantly expressed in the proximal tubules and the medullary thick ascending limbs, and to a lesser extent, in the glomerular mesangial cells [6,7]. Given the high level of expression in the renal proximal tubules, PPARα has been implicated in the metabolic control of the kidney in maintaining a sustained balance of energy production and expenditure.
PPARs basically function as sensors for fatty acid derivatives and control important metabolic pathways involved in lipid and energy metabolism. PPARs also play an important role in various pathophysiologic conditions, such as immunity, inflammation, apoptosis, and cell differentiation [8]. Each member of the PPAR subfamily has additional actions [9,10]. PPARα plays an additional role in lipoprotein synthesis, inflammatory responses and the fatty acid oxidation system [2]. In general, PPARα functions as catabolic regulators of energy [2,11].
Numerous studies in experimental and clinical models have shown the beneficial effects of PPARs in improving organ function in some diseases [12,13]. The PPARα agonists, such as fenofibrate and clofibrate, are traditionally proven lipid-lowering drugs [13]. Despite their serendipitous discovery and clinical use in the treatment of dyslipidemia, the actual pharmacological profile of activity of the PPARα agonists is a new discovery [14]. In addition to their involvement in lipid and lipoprotein metabolism, recent evidence supports the theory that PPARα critically regulates inflammation and vascular function in the kidney, which has led to renewed interest in PPARα as a renal protective option.
The PPARα gene in the human, which spans ~93.2 kb, is located on chromosome 22q12-q13.1 and, encodes a protein of 468 amino acids. The PPARα gene that encodes mRNA is derived from 8 exons with a 5' untranslated region encoded by exons 1, 2, and part of exon 3 [15]. The remainder of exon 3 and exons 4-8 are known to contribute to the coding region of PPARα. The last 232 bp of exon 8 contribute to the 3'-untranslated region. In the mouse, the PPARα gene is located on chromosome 15E2, and it encodes a protein of 468 amino acids [2]. The encoded protein shares functional domains with other nuclear hormone receptors. As with other nuclear receptors and PPARs, PPARα contains four major functional domains, including the N-terminal ligand-independent transactivation domain (A/B domain), the DNA binding domain (DBD or C domain), the co-factor docking domain (D domain), and the C-terminal E/F domain (including the ligand binding domain [LBD] and the ligand-dependent transactivation domain (AF-2 domain)) (Fig. 1) [13]. The A/B domain contains an activation function-1 (AF-1) region, which has a low level of basal transactivation activity and functions independently of ligand-binding. In humans, DBD encompasses amino acids 101-166, which contain two very highly conserved zinc finger motifs and architectural elements that are capable of sequence-specific binding to DNA [15]. D domain, a flexible hinge domain, connects the DBD and LBD. This hinge region binds co-repressor proteins, with the characteristic LXXXIXXXL repressor motif, to the receptor in its quiescent, unliganded state [2]. LBD in the human PPARα protein, which contains an AF-2 region composed of two α-helices flanking one four-stranded β-sheet, extends from amino acids 280 to 468 [15]. The AF-2 domain is repressed until ligand-binding occurs. Following ligand-binding, the AF-2 domain undergoes a conformational shift, which allows the formation of hydrogen bonds between Tyr-314 and Tyr-464 as well as the formation of a charge clamp between Glu-462 and Lys-292. This conformational change in the protein allows interaction of the receptor with the LXXLL (L, leucine; X, any amino acid) motifs located in co-activator proteins [16]. In a similar fashion as other nuclear receptors, PPARα undergoes conformational adjustment upon binding to a ligand to achieve the co-regulator exchanges and activation of the target genes [2,16].
PPARα, like the other two PPAR isoforms, is localized to the nucleus, which is characteristic of the type II nuclear receptor family [2]. PPARα regulates many target genes, and the expression of the PPARα gene is also affected by other transcription factors [17]. According to an experimental study, PPARα is regulated by various physiological conditions such as stress, hormones, glucocorticoids, insulin, and leptin [18]. Its expression additionally appears to be related to aging [19]. PPARα is also regulated at the transcriptional level by nuclear receptors such as hepatocyte nuclear factor 4 (HNF4) and the orphan receptor, known as chicken ovalbumin upstream promoter-transcription factor II (COUP-TFII). HNF4 positively affects PPARα expression via a direct repeat 1 (DR1) element, which is composed of the consensus sequence AGG(A/T)CA separated with a single nucleotide spacing between two repeats [17]. The DR1 element in the human PPARα promoter is antagonized by COUP-TFII. PPARα also appears to modulate its own expression [20]; transcript levels are induced during macrophage differentiation by high glucose levels, and PPARα is regulated by the ubiquitin proteasomal degradation system [21,22].
PPARα functions as an obligate heterodimer with another nuclear receptor: retinoid X receptor (RXR; NR2B) [2]. The PPARα/RXR heterodimers bind to a specific DNA sequence element called a peroxisome proliferator response element (PPRE), which is located in the promoter region of the target genes [23,24]. PPRE consists of a direct repeat of hexametric core recognition elements spaced by 1 bp (DR1, 5'AGGTCANAGGTCA-3') located in the promoter regions of target genes [13]. The upstream extended hexamer of DR1 interacts with PPARs, whereas the downstream hexamer is known to interact with RXR of the PPAR/RXR heterodimer [15]. Interestingly, PPARγ binds more strongly than the other isoforms, while conservation of the 5'-flanking extension is more important for the binding of PPARα and PPARβ/δ [25]. After activation of the PPARα/RXR heterodimer at the PPRE, the PPARα/RXR complex recruits diverse nuclear receptor co-factors that modulate transcriptional activity of the PPAR and RXR receptor heterodimer [13]. As with other nuclear receptors, transcriptional activation of PPAR genes involves the participation of many transcription co-regulators, and PPARs interact with co-activators, such as steroid receptor co-activator-1 (SRC-1), or co-repressors, such as the nuclear co-repressor (N-CoR) and the silencing mediator for retinoid and thyroid hormone receptors (SMRT) [26,27]. PPARα-interacting co-activators and co-repressors augment or repress, respectively, the PPARα transactivation activity [28].
PPAR activities are regulated by postranslational modification such as phosphorylation. This phosphorylation of PPARα is mediated by insulin and stress. Stress stimuli cause an increase in PPARα phosphorylation in rat neonatal cardiac myocytes via the p38 mitogen-activated protein kinase (MAPK) pathway [29]. PPARα is also reported to be phosphorylated by protein kinase C (PKC). Inhibition of PKC activity impairs ligand-activated PPARα transactivation activity but enhances PPARα transexpression activity, which suggests that the PKC signaling pathway may act as a molecular switch for the transactivation and transexpression properties of PPARα and also that PKC phosphorylation may play a role in statin-mediated anti-inflammatory effects [30,31].
PPARα basically regulates all three fatty acid oxidation systems, mitochondrial and peroxisomal β-oxidative processing and microsomal ω-oxidation, which indicates that PPARα functions mostly as a catabolic regulator of energy expenditure [32]. In this regard, activation of PPARα by pharmacological intervention proved useful in combating diet-induced obesity-associated complications [33,34]. PPARα also has hypolipidemic effects, which shows that PPARα ligands reduce VLDL production and enhance the catabolism of triglyceride (TG)-rich particles. This process indirectly decreases small dense LDL particles, enhancing the formation of HDL particles and hepatic elimination of excess cholesterol [35].
In association with their critical role as a primary sensor and regulator of lipid metabolism, PPARα agonists have been reported to decrease inflammation. According to numerous experimental studies, PPARα appears to influence both acute and chronic inflammatory disorders involving neutrophils and macrophages. Since some preference for specific fatty acids by each PPAR has been demonstrated, fatty acids and their derivatives (including 8(S)-hydroxyeicosatetraenoic acid, lipoxygenase metabolite leukotriene B4 [LTB4], and the arachidonate mono-oxygenase metabolite epoxyeicosatrienoic acids) have been shown to activate PPARα [13]. Among them, LTB4 is a powerful chemotactic inflammatory eicosanoid that induces transcription of genes of the β- and ω-oxidation pathways that neutralize and degrade LTB4 itself to regulate the inflammatory response [2,35]. Without PPARα regulation, the LTB4-induced inflammatory response tends to continue. Furthermore, experimental agents containing LTB4 (or its precursor arachidonic acid) when applied to the ears of PPARα knockout and wild-type mice showed that the inflammatory response was significantly prolonged in PPARα-null mice compared to the wild-type controls, suggesting that PPARα affects the duration of the inflammatory response, possibly by limiting cytokine expression and also by inducing genes that metabolize LTB4 [35]. In addition, PPARα activation may result in reduced leukocyte adhesion to activated endothelial cells of the arterial lumen and subsequent inhibition of the formation of macrophage foam cells by regulating the expression of genes involved in reverse cholesterol transport and reactive oxygen species (ROS) output [36]. PPARα agonists seem to inhibit lipopolysaccharide activation of peritoneal macrophages, indicating a role in inflammation that is independent of macrophage polarization [37]. Fibrate treatment also has been reported to reduce atherosclerosis in apoE-deficient mice and in human ApoAI transgenic apoE-deficient mice [38]. Therefore, activation of PPARα may be beneficial in ameliorating the formation and progression of atherosclerotic plaques by minimizing lipoprotein oxidative modifications.
According to several experimental studies, PPARα ligands influence the levels of pro-inflammatory cytokines, such as interleukin (IL)-1, IL-6, tumor necrosis factor-α (TNF-α), cyclooxygenase-2, and inducible nitric oxide synthase (iNOS). They regulate these cytokines by inhibiting the translocation of the p65 subunit of nuclear factor κB (NF-κB), increasing IκB (the inhibitor of NF-κB) and decreasing phosphorylation of the c-jun subunit of AP-1 [37,39]. PPARα agonists appear to inhibit TNF-α-induced vascular cell adhesion molecule (VCAM)-1 expression in endothelial cells by suppressing transcriptional activity of NF-κB [37]. Considering that PPARα is expressed in both vascular endothelial cells and smooth muscle cells, PPARα can therefore be expected to be involved in vascular pathologic processes. PPARα activation has been reported to inhibit vascular smooth muscle cell (VSMC) proliferation by suppressing telomerase activity through the p16/retinoblastoma/E2F transcriptional pathway. In addition, PPARα agonists have been shown to inhibit inflammation in VSMCs; conversely, PPARα deficiency leads to more profound inflammation in these cells [37]. PPARα has the ability to inhibit vascular inflammation, oxidative stress, and cell growth and migration, as evidenced by experimental results that showed that PPARα blocked NF-κB, transforming growth factor (TGF)-β/Smad and MAPK pathways [40]. Additionally, several other studies have demonstrated a similar, important role for PPARα in modulating inflammation in vascular endothelial cells, cartilage and bone tissue, kidney, adipose tissue, and the central nervous system [2].
PPARα has also been implicated in blood pressure regulation. Experimental studies demonstrated that PPARα agonists reduced angiotensin II-induced hypertension in rats, probably by improving endothelial cell function [41]. A PPARα agonist has also been reported to decrease blood pressure in a deoxycorticosterone acetate (DOCA)-salt-induced hypertensive mouse model by increasing renal 20-hydroxyeicosatetraenoic acid production and therefore decreasing sodium retention [37]. In addition, PPARα has been found to co-localize with arachidonic CYP450 4A enzymes in the renal proximal tubule; knockout cyp4A14 mice exhibited androgen-dependent hypertension [42], which suggested that regulation of CYP4A by PPARα may play a role in sodium homeostasis and blood pressure regulation. Interestingly, PPARα also appears to be associated with tissue renin-angiotensin system (RAS) activity. Our recent study showed that PPARα content in the kidney was negatively correlated with activation of intrarenal RAS [33]. Fenofibrate treatment in spontaneously hypertensive rats fed with a high-fat diet attenuated weight gain, fat mass and insulin resistance, whereas angiotensin receptor blockers or antioxidant treatment did not improve metabolic parameters [33,43]. Besides the recovery of the diet-induced decrease in intrarenal PPARα expression and the increase in lipid accumulation with administration of PPARα agonists, the most important finding was that PPARα abolished intrarenal RAS activation and oxidative stress while also providing protection against increased blood pressure and renal injury [33].
Based on these observations, we surmised that PPARα ligands exerted potential organ-protective effects in modulating inflammatory processes, atherosclerosis, blood pressure, and the RAS.
Hyperglycemia, endothelial dysfunction, lipotoxicity, and dyslipidemia are common denominators of the pathological mechanism that gives rise to diabetic renal complications in both type 1 and type 2 diabetes mellitus [44]. Increasing evidence suggests that PPARα may play critical regulatory roles in a variety of biologic events, such as lipid metabolism, energy homeostasis, insulin sensitivity, inflammation and blood pressure regulation; a therapeutic potential for PPARα agonists in renal complications of diabetes has also been suggested. PPARα has been implicated in the pathogenesis of obesity and insulin resistance, which are among the diagnostic criteria for the metabolic syndrome seen in up to 75% of patients with type 2 diabetes [13].
Activation of PPARα reduces weight gain in animals, and a high-fat diet in PPARα-null mice leads to a more dramatic increase in body weight [33,45]. Treatment with PPARα agonists also improves insulin resistance and glycemic control in db/db mice and OLETF rats and prevents the development of diabetes in obese OLETF rats [46,47].
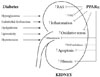
In addition to systemic effects, multiple intrarenal mechanisms have been implicated in the beneficial effect of PPARα ligands (Fig. 2). An experimental study with a type 2 diabetic model showed that PPARα activation by fenofibrate improved insulin sensitivity, glucose control, and diabetic nephropathy, as evidenced by urinary albumin excretion and attenuated glomerular mesangial expansion [48]. Such beneficial effects on renal outcome with fibrates may result from anti-inflammatory, anti-atherosclerotic, antihypertensive, and anti-RAS actions as noted above. In an experimental study to investigate the role of PPARα in type 1 diabetic nephropathy, more severe structural changes (such as glomerulosclerosis and mesangial area expansion) as well as an effect on albuminuria were noted in diabetic PPARα-knockout mice; these changes were associated with an increase in the profibrotic, pro-inflammatory and pro-apoptotic pathways implicated in renal extracellular matrix accumulation [49]. In PPARα deficiency, the glomerular lesions exhibited increased type IV collagen and TGF-β expression in diabetic kidney disease, suggesting that the activation of PPARα ligands effectively prevents the glomerular matrix expansion that accompanies apoptosis and inflammatory cell infiltration in the glomerulus [49].
In our study, which investigated the effect of the glucagon-like peptide-1 analog exendin-4 on the progression of type 2 diabetic nephropathy, we observed significantly increased PPARα expression in a dose-dependent manner in exendin-4-treated db/db kidneys in mice compared with that seen in control db/db kidneys [50]. This increase in PPARα expression was accompanied by reduced glomerular immunostaining for F4/80 and caspase-3 as well as for TGF-β1. Furthermore, exendin-4 treatment decreased 24-hour urinary 8-hydroxy-deoxyguanosine concentration, which was consistent with the reduction in oxidative DNA damage and oxidative stress. These findings suggest that TGF-β1 expression mediated by oxidative stress may be suppressible by PPARα activation [50]. Interestingly, there is evidence that starved PPARα-null mice develop increased albuminuria and exhibit albumin accumulation in the proximal tubules, which indicates that PPARα activity may facilitate albumin reabsorption and degradation in this nephron segment [51]. This mechanism may contribute to the beneficial effect of PPARα agonists on albuminuria in type 2 diabetic nephropathy.
In mesangial cells, PPARα agonists reduce the production of TGF-β and extracellular matrix. The TGF-β signaling pathway may be one possible mechanism that relates to the effect of PPARα agonists on the mesangial matrix production. One study showed that clofibrate directly inhibits oxidant stress-induced TGF-β1 expression in these cells, indicating that PPARα agonists block the TGF-β signaling pathway, thereby attenuating glomerular matrix production [52]. PPRE3X luciferase reporter analysis demonstrated that the fenofibrate significantly increased luciferase activity in mesangial cells, which is consistent with the existence of endogenous PPARα activity in these cells [48,49]. This finding suggests that increased PPARα activity in the tubule may exert anti-inflammatory and anti-fibrotic effects via paracrine action resulting from increased PPRE activity in the glomeruli [49].
Importantly, we need to pay attention to the role PPARα in vascular biology. PPARα ligands appear to modulate renal endothelial cell proliferation and migration, probably through their ability to interfere with the vascular endothelial growth factor (VEGF)-mediated signaling pathway. VEGF is crucial for maintaining the function and integrity of the endothelium [44]. In the kidney, the VEGF receptors (VEGFR) are expressed in the endothelium of the glomeruli, the peritubular capillaries and, to a lesser extent, the mesangial and tubular cells [53]. In the glomerular endothelial cells, VEGF-A stimulates the VEGFR-2/Akt axis to regulate endothelial NOS (eNOS) phosphorylation. eNOS is activated by the phosphorylation of serine (Ser1177) of the protein kinase Akt/PKB and is also known to regulate glomerular hemodynamics by generation of nitric oxide (NO) [53,54]. Several type 1 or type 2 animal models have shown that VEGF stimulates renal pathological progressions, as demonstrated by glomerular hyperfiltration and hypertrophy and urinary albumin excretion [44]. By contrast, excessively low levels of VEGF are associated with renal deterioration in the type 2 diabetic model [44,53], suggesting that a too-low VEGF level can be just as damaging as when the VEGF level is too high [53]. Interestingly, PPARα agonists have been shown to inhibit endothelial VEGFR-2 expression, and fenofibrate treatment induces a significant reduction of VEGF levels in serum [53,55]. Although the data regarding the effects of administration with PPARα agonists on VEGF changes in diabetic kidneys are lacking, angiogenic modulation and endothelial cell stabilization by PPARα agonists might be responsible for the potential renoprotective effects in diabetic nephropathy models. Recently, we found that dual VEGFR1 and VEGFR2 inhibition in db/db mice aggravated diabetic peripheral neuropathy, including a decrease in nerve conduction velocity and an increase in the tactile threshold of the sciatic nerve associated with vascular rarefaction resulting from endothelial cell apoptosis, which completely recovered to levels of non-diabetic db/m mice by fenofibrate (unpublished data).
As renal lipotoxicity can lead to chronic kidney disease, an overload of free fatty acid-bound albumin in the proximal epithelial cells induced tubular cell injury resulting from not only a decrease in the lipolytic enzymes but also increases in lipid accumulation and oxidative stress [56]. Fenofibrate, by contrast, inhibited palmitate-induced expressions of both monocyte chemoattractant protein-1 and PAI-1 and oxidative stress in the proximal tubular cells, which were associated with the overexpression of lipolytic enzymes and enhancement of renal lipolysis. Therefore, we need more experimental evidences using various types of renal cells including podocytes in order to investigate whether pharmacological activation of PPARα could be a therapeutically suitable strategy against glomerular and tubuleinterstitial lesions in diabetic nephropathy.
Recent studies have shown a beneficial effect of fibrate treatment on type 2 diabetes and diabetic nephropathy [57-59]. In normotensive patients with non-insulin-dependent diabetes, effective treatment of dyslipidemia by a PPARα activator gemfibrozil for one year was associated with significant stabilization of urine albumin excretion [58]. The Fenofibrate Intervention and Event Lowering in Diabetes (FIELD) study reported that fenofibrate treatment was associated with reductions in cardiovascular disease outcomes [59]. This study included 9,795 patients with type 2 diabetes. The results demonstrated that fenofibrate treatment was associated with an 11% reduction in total cardiovascular disease events [59]. Interestingly, the FIELD study showed that fenofibrate resulted in significantly more patients' regressing or not progressing in their urinary albumin excretion. In the fenofibrate group, albuminuria progressed in 9.5% of the patients compared to 11.0% of patients in the placebo group. Albuminuria regressed in 9.4% of patients in the fenofibrate treatment group and in 8.2% in the placebo group participants [44,59]. The Action to Control Cardiovascular Risk in Diabetes (ACCORD) study also demonstrated that fibrate therapy with intensive glucose control could significantly reduce microalbuminuria (38.2% vs. 41.6%, P=0.01) and macroalbuminuria (10.5% vs. 12.3%, P=0.03) despite the marginal effects of fibrates in the management of dyslipidemia [60,61]. Unfortunately, most trials with PPARα agonists have been designed for cardiovascular disease, not renal disease, as a primary end point. The effect of fenofibrate on urinary protein excretion appears to be minor compared with the major effects on cardiovascular disease events [62]. Another weakness is that most studies have been limited to people with type 2 diabetes. In the future, more large-scale, prospective, randomized trials will be necessary to evaluate the efficacy of fibrates on renal outcomes in patients with type 1 or type 2 diabetes.
Despite evidence of the beneficial effects of PPARα agonists in patients with diabetes, there are still many issues to be addressed concerning their safety in clinical use. The most important concern is due to the fact that fibrate treatment typically results in increased serum levels of creatinine and cystatin C and might potentially decrease the estimated glomerular filtration rate and creatinine clearance [44]. More care should be taken when prescribing fibrates to patients with mild-to-moderate renal insufficiency. Currently, it is recommended that fenofibrate dosages should be reduced by one third in chronic kidney disease (CKD) stage 2, by an additional one third in CKD stage 3 and 4, and avoided in CKD stage 5 [62]. Although the mechanisms of deterioration in renal function with fibrates are not clear, renal hemodynamic changes in association with the reduction of cylcooxygenase 2 levels, an inhibitory action of fenofibrate on the excretion of creatinine by the kidneys, or an increase in the flow of creatinine from muscle might be an explanation [44,63].
In addition, the fact that PPARα is subject to tissue-specific regulation should be considered. Over-expression of PPARα in the heart results in increased fatty acid oxidation, elevated lipid droplets, and worsened cardiomyopathy, suggesting that cardiac PPARα activation may be harmful [54,64]. By contrast, an increase in PPARα expression in the diabetic kidney is evident [49], indicating compensatory PPARα activation in response to the renal damage suffered. The proper balance between overactivation and underactivation of PPARα may differ in each type of affected organ or tissue. To maximize the therapeutic potential and minimize the harmful effects of PPARα, future investigations should examine the development of selective agents with tissue-, organ- or disease-specific effects and targeted gene-selective activities. This will require development of more selective PPARα modulators.
Recent studies have suggested beneficial roles for PPARα and PPARα target genes as therapeutic targets in the treatment of disorders involving inflammation, atherosclerosis, oxidative stress, angiogenesis, and RAS. PPARα agonists have traditionally been used to lower circulating fatty acids and TG. Currently, considerable evidence suggests that PPARα is involved in the pathogenesis of diabetic nephropathy and contributes to the extrametabolic control of renal function. Although the mechanisms of the beneficial effects of fibrates in the kidneys are still under investigation, PPARα would be a promising therapeutic target in the management of diabetes and diabetic nephropathy.
Figures and Tables
Fig. 1
Structure and molecular mechanism of action of peroxisome proliferator-activated receptor alpha (PPARα). (A) PPARα has four functional domains: the N-terminal ligand-independent transactivation domain (A/B domain); DNA binding domain (DBD or C domain), including an activation function-1 (AF-1); co-factor docking domain (D domain); and C-terminal E/F domain including a ligand binding domain (LBD) and an activation function-2 (AF-2). (B) The PPARα and retinoid X receptor-α (RXRα) heterodimer, which can recruit diverse coactivators and corepressors that modulate the transcriptional activity of PPARα, binds to PPAR-response elements (PPRE) to activate target gene transcription.
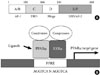
Fig. 2
Protective actions of peroxisome proliferator-activated receptor alpha (PPARα) agonists for the improvement of diabetic nephropathy. In diabetic patients, symptoms such as hyperglycemia, dyslipidemia, endothelial dysfunction, lipotoxicity, and high blood pressure all can contribute to renal complications of diabetes systemically or locally via increased inflammation, activation of the renin-angiotensin system (RAS), enhanced oxidative stress, increased apoptosis and vasculopathy, which can be attenuated by the activation of PPARα. TGF, transforming growth factor; VEGF, vascular endothelial growth factor.
ACKNOWLEDGMENTS
This research was supported by a grant of the Korean Health Technology R&D Project, Minister of Health and Welfare, Republic of Korea, (to C. W. Park; A111055) and also by Seoul St. Mary's Hospital Clinical Medicine Research Program year of 2010 through The Catholic University of Korea.
References
1. Cheng CF, Chen HH, Lin H. Role of PPARα and its agonist in renal diseases. PPAR Res. 2010. 2010:345098.
2. Pyper SR, Viswakarma N, Yu S, Reddy JK. PPARalpha: energy combustion, hypolipidemia, inflammation and cancer. Nucl Recept Signal. 2010. 8:e002.
3. Berger JP, Akiyama TE, Meinke PT. PPARs: therapeutic targets for metabolic disease. Trends Pharmacol Sci. 2005. 26:244–251.
4. Bookout AL, Jeong Y, Downes M, Yu RT, Evans RM, Mangelsdorf DJ. Anatomical profiling of nuclear receptor expression reveals a hierarchical transcriptional network. Cell. 2006. 126:789–799.
5. Guan Y, Zhang Y, Schneider A, Davis L, Breyer RM, Breyer MD. Peroxisome proliferator-activated receptor-gamma activity is associated with renal microvasculature. Am J Physiol Renal Physiol. 2001. 281:F1036–F1046.
6. Guan Y, Zhang Y, Davis L, Breyer MD. Expression of peroxisome proliferator-activated receptors in urinary tract of rabbits and humans. Am J Physiol. 1997. 273(6 Pt 2):F1013–F1022.
7. Ruan XZ, Moorhead JF, Fernando R, Wheeler DC, Powis SH, Varghese Z. PPAR agonists protect mesangial cells from interleukin 1beta-induced intracellular lipid accumulation by activating the ABCA1 cholesterol efflux pathway. J Am Soc Nephrol. 2003. 14:593–600.
8. Maeda T, Kishioka S. PPAR and pain. Int Rev Neurobiol. 2009. 85:165–177.
9. Kliewer SA, Xu HE, Lambert MH, Willson TM. Peroxisome proliferator-activated receptors: from genes to physiology. Recent Prog Horm Res. 2001. 56:239–263.
10. Yu S, Matsusue K, Kashireddy P, Cao WQ, Yeldandi V, Yeldandi AV, Rao MS, Gonzalez FJ, Reddy JK. Adipocyte-specific gene expression and adipogenic steatosis in the mouse liver due to peroxisome proliferator-activated receptor gamma1 (PPARgamma1) overexpression. J Biol Chem. 2003. 278:498–505.
11. Ruan X, Zheng F, Guan Y. PPARs and the kidney in metabolic syndrome. Am J Physiol Renal Physiol. 2008. 294:F1032–F1047.
12. Letavernier E, Perez J, Joye E, Bellocq A, Fouqueray B, Haymann JP, Heudes D, Wahli W, Desvergne B, Baud L. Peroxisome proliferator-activated receptor beta/delta exerts a strong protection from ischemic acute renal failure. J Am Soc Nephrol. 2005. 16:2395–2402.
13. Guan Y. Peroxisome proliferator-activated receptor family and its relationship to renal complications of the metabolic syndrome. J Am Soc Nephrol. 2004. 15:2801–2815.
14. Fruchart JC. Peroxisome proliferator-activated receptor-alpha (PPARalpha): at the crossroads of obesity, diabetes and cardiovascular disease. Atherosclerosis. 2009. 205:1–8.
15. Desvergne B, Wahli W. Peroxisome proliferator-activated receptors: nuclear control of metabolism. Endocr Rev. 1999. 20:649–688.
16. Xu HE, Lambert MH, Montana VG, Plunket KD, Moore LB, Collins JL, Oplinger JA, Kliewer SA, Gampe RT Jr, McKee DD, Moore JT, Willson TM. Structural determinants of ligand binding selectivity between the peroxisome proliferator-activated receptors. Proc Natl Acad Sci U S A. 2001. 98:13919–13924.
17. Pineda Torra I, Jamshidi Y, Flavell DM, Fruchart JC, Staels B. Characterization of the human PPARalpha promoter: identification of a functional nuclear receptor response element. Mol Endocrinol. 2002. 16:1013–1028.
18. Inoue J, Satoh S, Kita M, Nakahara M, Hachimura S, Miyata M, Nishimaki-Mogami T, Sato R. PPARalpha gene expression is up-regulated by LXR and PXR activators in the small intestine. Biochem Biophys Res Commun. 2008. 371:675–678.
19. Poynter ME, Daynes RA. Peroxisome proliferator-activated receptor alpha activation modulates cellular redox status, represses nuclear factor-kappaB signaling, and reduces inflammatory cytokine production in aging. J Biol Chem. 1998. 273:32833–32841.
20. Corton JC, Anderson SP, Stauber A. Central role of peroxisome proliferator-activated receptors in the actions of peroxisome proliferators. Annu Rev Pharmacol Toxicol. 2000. 40:491–518.
21. Rigamonti E, Chinetti-Gbaguidi G, Staels B. Regulation of macrophage functions by PPAR-alpha, PPAR-gamma, and LXRs in mice and men. Arterioscler Thromb Vasc Biol. 2008. 28:1050–1059.
22. Genini D, Carbone GM, Catapano CV. Multiple interactions between peroxisome proliferators-activated receptors and the ubiquitin-proteasome system and implications for cancer pathogenesis. PPAR Res. 2008. 2008:195065.
23. Chandra V, Huang P, Hamuro Y, Raghuram S, Wang Y, Burris TP, Rastinejad F. Structure of the intact PPAR-gamma-RXR-nuclear receptor complex on DNA. Nature. 2008. 456:350–356.
24. van der Meer DL, Degenhardt T, Vaisanen S, de Groot PJ, Heinaniemi M, de Vries SC, Muller M, Carlberg C, Kersten S. Profiling of promoter occupancy by PPARalpha in human hepatoma cells via ChIP-chip analysis. Nucleic Acids Res. 2010. 38:2839–2850.
25. Juge-Aubry C, Pernin A, Favez T, Burger AG, Wahli W, Meier CA, Desvergne B. DNA binding properties of peroxisome proliferator-activated receptor subtypes on various natural peroxisome proliferator response elements. Importance of the 5'-flanking region. J Biol Chem. 1997. 272:25252–25259.
26. Zhu Y, Qi C, Calandra C, Rao MS, Reddy JK. Cloning and identification of mouse steroid receptor coactivator-1 (mSRC-1), as a coactivator of peroxisome proliferator-activated receptor gamma. Gene Expr. 1996. 6:185–195.
27. Dowell P, Ishmael JE, Avram D, Peterson VJ, Nevrivy DJ, Leid M. Identification of nuclear receptor corepressor as a peroxisome proliferator-activated receptor alpha interacting protein. J Biol Chem. 1999. 274:15901–15907.
28. Feige JN, Gelman L, Michalik L, Desvergne B, Wahli W. From molecular action to physiological outputs: peroxisome proliferator-activated receptors are nuclear receptors at the crossroads of key cellular functions. Prog Lipid Res. 2006. 45:120–159.
29. Barger PM, Browning AC, Garner AN, Kelly DP. p38 mitogen-activated protein kinase activates peroxisome proliferator-activated receptor alpha: a potential role in the cardiac metabolic stress response. J Biol Chem. 2001. 276:44495–44501.
30. Burns KA, Vanden Heuvel JP. Modulation of PPAR activity via phosphorylation. Biochim Biophys Acta. 2007. 1771:952–960.
31. Blanquart C, Mansouri R, Paumelle R, Fruchart JC, Staels B, Glineur C. The protein kinase C signaling pathway regulates a molecular switch between transactivation and transrepression activity of the peroxisome proliferator-activated receptor alpha. Mol Endocrinol. 2004. 18:1906–1918.
32. Ricote M, Valledor AF, Glass CK. Decoding transcriptional programs regulated by PPARs and LXRs in the macrophage: effects on lipid homeostasis, inflammation, and atherosclerosis. Arterioscler Thromb Vasc Biol. 2004. 24:230–239.
33. Shin SJ, Lim JH, Chung S, Youn DY, Chung HW, Kim HW, Lee JH, Chang YS, Park CW. Peroxisome proliferator-activated receptor-alpha activator fenofibrate prevents high-fat diet-induced renal lipotoxicity in spontaneously hypertensive rats. Hypertens Res. 2009. 32:835–845.
34. Zhao X. Prevention of local lipotoxicity: a new renoprotective mechanism of peroxisome proliferator-activated receptor-alpha activation in hypertension and obesity? Hypertens Res. 2009. 32:821–823.
35. Devchand PR, Keller H, Peters JM, Vazquez M, Gonzalez FJ, Wahli W. The PPARalpha-leukotriene B4 pathway to inflammation control. Nature. 1996. 384:39–43.
36. Zandbergen F, Plutzky J. PPARalpha in atherosclerosis and inflammation. Biochim Biophys Acta. 2007. 1771:972–982.
37. Duan SZ, Usher MG, Mortensen RM. PPARs: the vasculature, inflammation and hypertension. Curr Opin Nephrol Hypertens. 2009. 18:128–133.
38. Duez H, Chao YS, Hernandez M, Torpier G, Poulain P, Mundt S, Mallat Z, Teissier E, Burton CA, Tedgui A, Fruchart JC, Fievet C, Wright SD, Staels B. Reduction of atherosclerosis by the peroxisome proliferator-activated receptor alpha agonist fenofibrate in mice. J Biol Chem. 2002. 277:48051–48057.
39. Ramanan S, Kooshki M, Zhao W, Hsu FC, Robbins ME. PPARalpha ligands inhibit radiation-induced microglial inflammatory responses by negatively regulating NF-kappaB and AP-1 pathways. Free Radic Biol Med. 2008. 45:1695–1704.
40. Kintscher U, Lyon C, Wakino S, Bruemmer D, Feng X, Goetze S, Graf K, Moustakas A, Staels B, Fleck E, Hsueh WA, Law RE. PPARalpha inhibits TGF-beta-induced beta5 integrin transcription in vascular smooth muscle cells by interacting with Smad4. Circ Res. 2002. 91:e35–e44.
41. Diep QN, Amiri F, Touyz RM, Cohn JS, Endemann D, Neves MF, Schiffrin EL. PPARalpha activator effects on Ang II-induced vascular oxidative stress and inflammation. Hypertension. 2002. 40:866–871.
42. Holla VR, Adas F, Imig JD, Zhao X, Price E Jr, Olsen N, Kovacs WJ, Magnuson MA, Keeney DS, Breyer MD, Falck JR, Waterman MR, Capdevila JH. Alterations in the regulation of androgen-sensitive Cyp 4a monooxygenases cause hypertension. Proc Natl Acad Sci U S A. 2001. 98:5211–5216.
43. Chung S, Park CW, Shin SJ, Lim JH, Chung HW, Youn DY, Kim HW, Kim BS, Lee JH, Kim GH, Chang YS. Tempol or candesartan prevents high-fat diet-induced hypertension and renal damage in spontaneously hypertensive rats. Nephrol Dial Transplant. 2010. 25:389–399.
44. Hiukka A, Maranghi M, Matikainen N, Taskinen MR. PPARalpha: an emerging therapeutic target in diabetic microvascular damage. Nat Rev Endocrinol. 2010. 6:454–463.
45. Kim BH, Won YS, Kim EY, Yoon M, Nam KT, Oh GT, Kim DY. Phenotype of peroxisome proliferator-activated receptor-alpha(PPARalpha)deficient mice on mixed background fed high fat diet. J Vet Sci. 2003. 4:239–244.
46. Aasum E, Belke DD, Severson DL, Riemersma RA, Cooper M, Andreassen M, Larsen TS. Cardiac function and metabolism in type 2 diabetic mice after treatment with BM 17.0744, a novel PPAR-alpha activator. Am J Physiol Heart Circ Physiol. 2002. 283:H949–H957.
47. Koh EH, Kim MS, Park JY, Kim HS, Youn JY, Park HS, Youn JH, Lee KU. Peroxisome proliferator-activated receptor (PPAR)-alpha activation prevents diabetes in OLETF rats: comparison with PPAR-gamma activation. Diabetes. 2003. 52:2331–2337.
48. Park CW, Zhang Y, Zhang X, Wu J, Chen L, Cha DR, Su D, Hwang MT, Fan X, Davis L, Striker G, Zheng F, Breyer M, Guan Y. PPARalpha agonist fenofibrate improves diabetic nephropathy in db/db mice. Kidney Int. 2006. 69:1511–1517.
49. Park CW, Kim HW, Ko SH, Chung HW, Lim SW, Yang CW, Chang YS, Sugawara A, Guan Y, Breyer MD. Accelerated diabetic nephropathy in mice lacking the peroxisome proliferator-activated receptor alpha. Diabetes. 2006. 55:885–893.
50. Park CW, Kim HW, Ko SH, Lim JH, Ryu GR, Chung HW, Han SW, Shin SJ, Bang BK, Breyer MD, Chang YS. Long-term treatment of glucagon-like peptide-1 analog exendin-4 ameliorates diabetic nephropathy through improving metabolic anomalies in db/db mice. J Am Soc Nephrol. 2007. 18:1227–1238.
51. Kamijo Y, Hora K, Tanaka N, Usuda N, Kiyosawa K, Nakajima T, Gonzalez FJ, Aoyama T. Identification of functions of peroxisome proliferator-activated receptor alpha in proximal tubules. J Am Soc Nephrol. 2002. 13:1691–1702.
52. Wilmer WA, Dixon CL, Hebert C, Lu L, Rovin BH. PPAR-alpha ligands inhibit H2O2-mediated activation of transforming growth factor-beta1 in human mesangial cells. Antioxid Redox Signal. 2002. 4:877–884.
53. Kim HW, Lim JH, Kim MY, Chung S, Shin SJ, Chung HW, Choi BS, Kim YS, Chang YS, Park CW. Long-term blockade of vascular endothelial growth factor receptor-2 aggravates the diabetic renal dysfunction associated with inactivation of the Akt/eNOS-NO axis. Nephrol Dial Transplant. 2011. 26:1173–1188.
54. Park CW, Kim HW, Lim JH, Yoo KD, Chung S, Shin SJ, Chung HW, Lee SJ, Chae CB, Kim YS, Chang YS. Vascular endothelial growth factor inhibition by dRK6 causes endothelial apoptosis, fibrosis, and inflammation in the heart via the Akt/eNOS axis in db/db mice. Diabetes. 2009. 58:2666–2676.
55. Grau R, Diaz-Munoz MD, Cacheiro-Llaguno C, Fresno M, Iniguez MA. Role of peroxisome proliferator-activated receptor alpha in the control of cyclooxygenase 2 and vascular endothelial growth factor: involvement in tumor growth. PPAR Res. 2008. 2008:352437.
56. Tanaka Y, Kume S, Araki S, Isshiki K, Chin-Kanasaki M, Sakaguchi M, Sugimoto T, Koya D, Heneda M, Kashiwagi A, Maegawa H, Uzu T. Fenofibrate, a PPARα agonist, has renoprotective effects in mice by enhancing renal lipolysis. Kidney Int. 2011. 79:871–882.
57. Fried LF, Orchard TJ, Kasiske BL. Effect of lipid reduction on the progression of renal disease: a meta-analysis. Kidney Int. 2001. 59:260–269.
58. Smulders YM, van Eeden AE, Stehouwer CD, Weijers RN, Slaats EH, Silberbusch J. Can reduction in hypertriglyceridaemia slow progression of microalbuminuria in patients with non-insulin-dependent diabetes mellitus? Eur J Clin Invest. 1997. 27:997–1002.
59. Keech A, Simes RJ, Barter P, Best J, Scott R, Taskinen MR, Forder P, Pillai A, Davis T, Glasziou P, Drury P, Kesaniemi YA, Sullivan D, Hunt D, Colman P, d'Emden M, Whiting M, Ehnholm C, Laakso M. FIELD study investigators. Effects of long-term fenofibrate therapy on cardiovascular events in 9795 people with type 2 diabetes mellitus (the FIELD study): randomised controlled trial. Lancet. 2005. 366:1849–1861.
60. Ismail-Beigi F, Craven T, Banerji MA, Basile J, Calles J, Cohen RM, Cuddihy R, Cushman WC, Genuth S, Grimm RH Jr, Hamilton BP, Hoogwerf B, Karl D, Katz L, Krikorian A, O'Connor P, Pop-Busui R, Schubart U, Simmons D, Taylor H, Thomas A, Weiss D, Hramiak I. ACCORD trial group. Effect of intensive treatment of hyperglycaemia on microvascular outcomes in type 2 diabetes: an analysis of the ACCORD randomised trial. Lancet. 2010. 376:419–430.
61. ACCORD Study Group. Ginsberg HN, Elam MB, Lovato LC, Crouse JR 3rd, Leiter LA, Linz P, Friedewald WT, Buse JB, Gerstein HC, Probstfield J, Grimm RH, Ismail-Beigi F, Bigger JT, Goff DC Jr, Cushman WC, Simons-Morton DG, Byington RP. Effects of combination lipid therapy in type 2 diabetes mellitus. N Engl J Med. 2010. 362:1563–1574.
62. Molitch ME. Management of dyslipidemias in patients with diabetes and chronic kidney disease. Clin J Am Soc Nephrol. 2006. 1:1090–1099.
63. Valensi P, Picard S. Lipids, lipid-lowering therapy and diabetes complications. Diabetes Metab. 2011. 37:15–24.
64. Finck BN, Han X, Courtois M, Aimond F, Nerbonne JM, Kovacs A, Gross RW, Kelly DP. A critical role for PPARalpha-mediated lipotoxicity in the pathogenesis of diabetic cardiomyopathy: modulation by dietary fat content. Proc Natl Acad Sci U S A. 2003. 100:1226–1231.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download