Abstract
Paratracheal air cyst (PTAC) is a small air collection in the right paratracheal area and mainly diagnosed by computed tomography (CT). Increased with ultrasonographic (US) screening of the thyroid, PTAC can be detected incidentally. However, the US findings of PTAC have not been well described. Herein, we report our experience with a rare instance of a PTAC. A 64-year-old female was referred to our hospital for fine-needle aspiration (FNA) cytology of a thyroid nodule. The lesion was identified as an ovoid, hypoechoic lesion with internal hyperechoic foci, abutting on the inferior pole of the right thyroid lobe. The margin was smooth without hypoechoic rim, which is typical in upper esophageal diverticula. US-guided FNA suggested a benign bronchial epithelial lining cyst. If a hypoechoic neck mass containing air without a thick hypoechoic rim is observed, especially at the right side of the trachea, the possibility of PTAC should be considered.
Go to : 
References
1. Tanaka H, Mori Y, Kurokawa K, Abe S. Paratracheal air cysts communicating with the trachea: CT findings. J Thorac Imaging. 1997; 12(1):38–40.
2. Goo JM, Im JG, Ahn JM, Moon WK, Chung JW, Park JH, et al. Right paratracheal air cysts in the thoracic inlet: clinical and radiologic significance. AJR Am J Roentgenol. 1999; 173(1):65–70.

3. Tanaka H, Igarashi T, Teramoto S, Yoshida Y, Abe S. Lymphoepithelial cysts in the mediastinum with an opening to the trachea. Respiration. 1995; 62(2):110–3.

4. Buterbaugh JE, Erly WK. Paratracheal air cysts: a common finding on routine CT examinations of the cervical spine and neck that may mimic pneumomediastinum in patients with traumatic injuries. AJNR Am J Neuroradiol. 2008; 29(6):1218–21.

5. Polat AV, Elmali M, Aydin R, Ozbay A, Celenk C, Murat N. Paratracheal air cysts: prevalence and correlation with lung diseases using multi-detector CT. J Med Imaging Radiat Oncol. 2014; 58(2):144–8.

6. Bae HJ, Kang EY, Yong HS, Kim YK, Woo OH, Oh YW, et al. Paratracheal air cysts on thoracic multidetector CT: incidence, morphological characteristics and relevance to pulmonary emphysema. Br J Radiol. 2013; 86(1021):20120218.

7. Morgan J, Perone R, Yeghiayan P. Paratracheal air collection in a trauma patient: a case report. Clin Imaging. 2009; 33(1):67–9.

8. Ampollini L, Bobbio A, Carbognani P, Rusca M. Incidental radiological finding of tracheal diverticulum. Eur J Cardiothorac Surg. 2007; 31(3):545.

9. Kim YJ, Kim EK, Kim J, Park CS. Paratracheal air cysts: sonographic findings in two cases. Korean J Radiol. 2003; 4(2):136–9.

10. Haghi Z, Towhidi M, Fattahi H, Lari SM. Right paratracheal air cyst (tracheal diverticulum). Respir Care. 2009; 54(10):1409–11.
11. Kim JS, Kim AY, Yoon Y. Paratracheal air cysts using low-dose screening chest computed tomography: clinical significance and imaging findings. Jpn J Radiol. 2011; 29(9):644–8.

12. Kim HK, Lee JI, Jang HW, Bae SY, Lee JH, Kim YS, et al. Characteristics of Killian-Jamieson diverticula mimicking a thyroid nodule. Head Neck. 2012; 34(4):599–603.

13. Infante M, Mattavelli F, Valente M, Alloisio M, Preda F, Ravasi G. Tracheal diverticulum: a rare cause and consequence of chronic cough. Eur J Surg. 1994; 160(5):315–6.
Go to : 
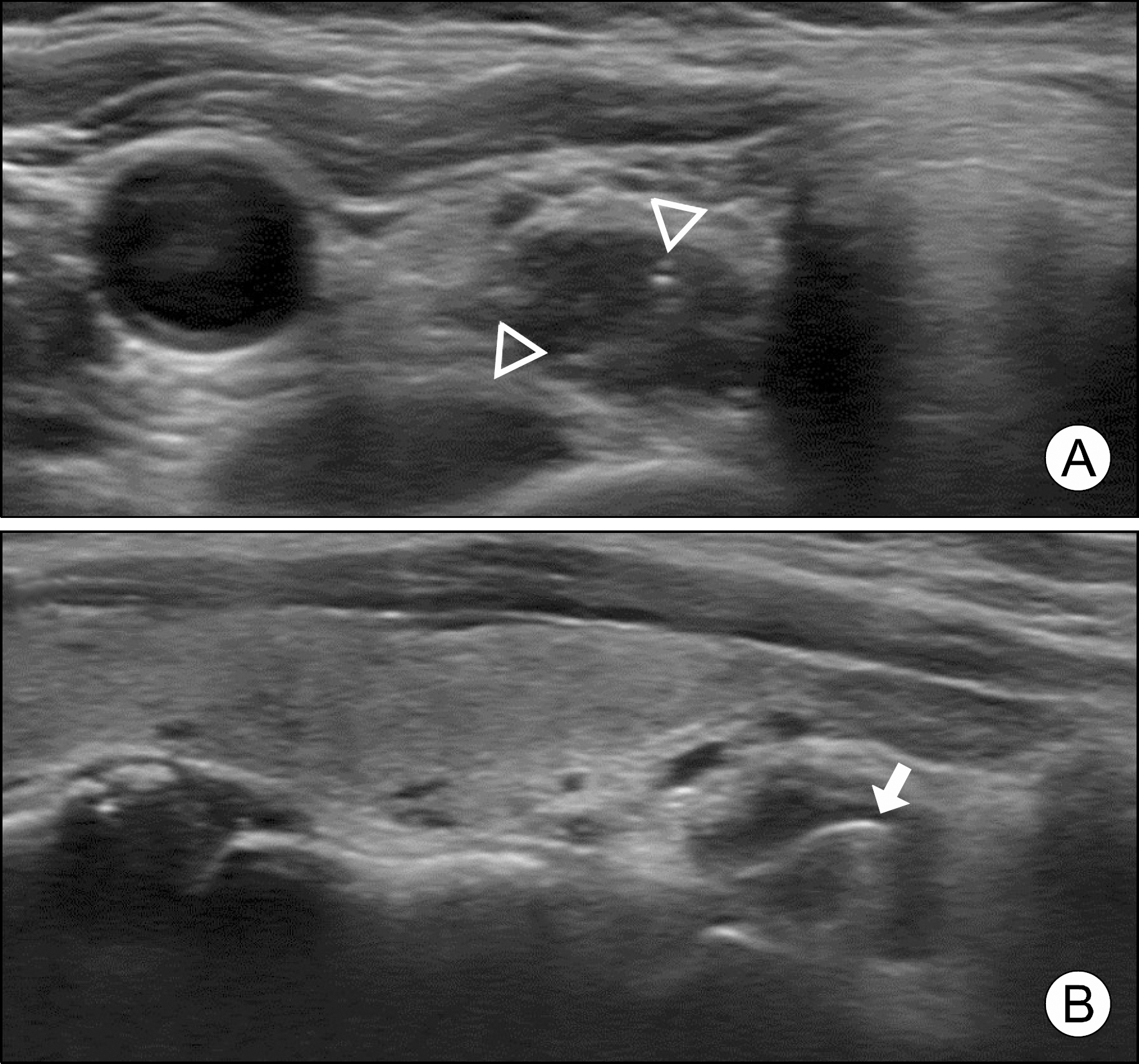 | Fig. 1.Ultrasonography (US) findings of the lesion. (A) A transverse US scan of the inferior pole of the right thyroid lobe shows a 0.9×0.4×1.1-cm-sized hypoechoic mass with internal hyperechoic dots (arrowheads), just lateral to the trachea. (B) On longitudinal scan, the lesion showed a linear hyperechoic focus with ring-down artifact (arrow), suggesting the presence of air. A hypoechoic boundary zone typically present in esophageal diverticula is absent. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download