초록
Viral infections are known to be a predisposing factor for subacute (De Quervain's) thyroiditis. In this report, we document a novel case of thyroiditis, with an atypical presentation, following an influenza B infection. A 13-year-old previously healthy female visited the outpatient clinic complaining of right neck pain. She had been diagnosed with an influenza B infection at a local clinic 3 weeks earlier. All laboratory tests were normal. A thyroid ultrasound showed an ill-defined hypoechoic mass (1.0×0.5×1.5 cm) in the right lower thyroid, and scintigraphy of the thyroid with Technetium-99m (99m-Tc) demonstrated the normal uptake of the radiotracer. Fine-needle aspiration from the nodule showed the presence of a few neutrophils. To the best of our knowledge, this is the first case of atypical thyroiditis associated with an influenza B infection described in the literature. Influenza B infection should be considered as a possible cause of atypical thyroiditis.
REFERENCES
1). Prummel MF, Strieder T, Wiersinga WM. The environment and autoimmune thyroid diseases. Eur J Endocrinol. 2004; 150(5):605–18.

2). Dimos G, Pappas G, Akritidis N. Subacute thyroiditis in the course of novel H1N1 influenza infection. Endocrine. 2010; 37(3):440–1.

3). Cunha BA, Berbari N. Subacute thyroiditis (de Quervain's) due to influenza A: presenting as fever of unknown origin (FUO). Heart Lung. 2013; 42(1):77–8.

4). Michas G, Alevetsovitis G, Andrikou I, Tsimiklis S, Vryonis E. De Quervain thyroiditis in the course of H1N1 influenza infection. Hippokratia. 2014; 18(1):86–7.
5). Altay FA, Guz G, Altay M. Subacute thyroiditis following seasonal influenza vaccination. Hum Vaccin Immunother. 2016; 12(4):1033–4.

7). Sari O, Erbas B, Erbas T. Subacute thyroiditis in a single lobe. Clin Nucl Med. 2001; 26(5):400–1.
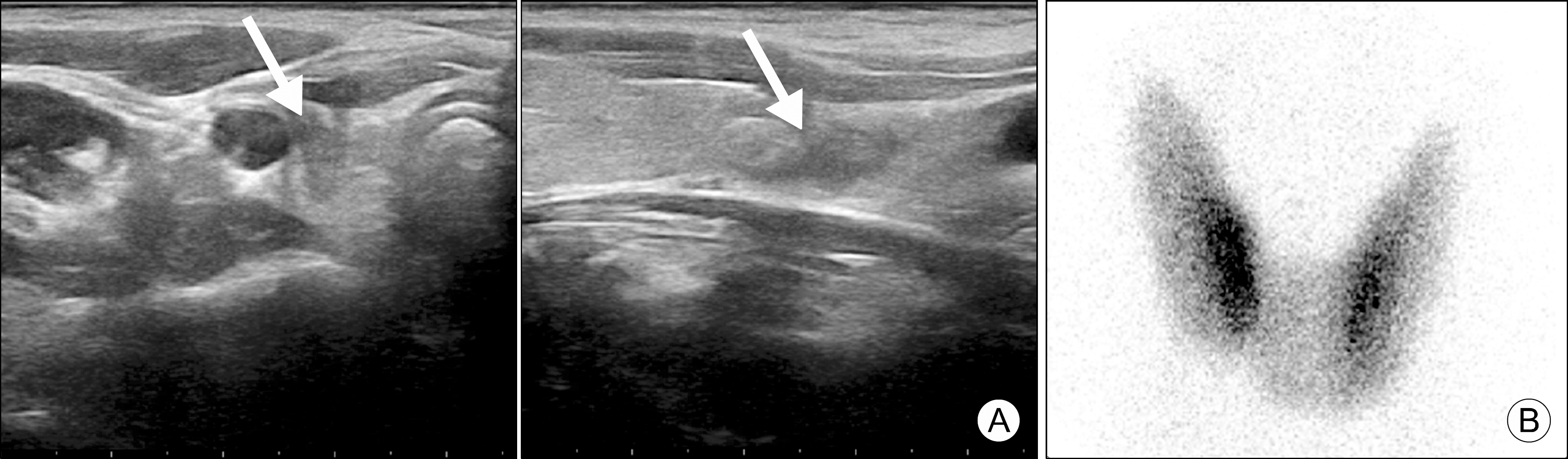
Fig. 1.
Initial thyroid ultrasonography and 99m-Technetium scintiscan. (A) Thyroid ultrasonography showed an ill-defined hypoechoic nodule (1.0×0.5×1.5 cm) in the right lobe of the thyroid gland (indicated by white arrows). (B) Thyroid scintigraphy with 99m-Tc revealed normal radiotracer uptake in the thyroid gland.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download