Abstract
A pseudoaneurysm is a collection of blood that locates between the two outer layers of an artery, the muscularis propria and the adventitia. It is resulted from disruption of a portion of the arterial wall. A pseudoaneurysm can be caused by trauma, blood vessel intervention, intravenous drug use, vasculitis, infectious aneurysm, and postoperative anastomotic leakage. The pseudoaneurysm of superior thyroid artery after core needle biopsy is rare. We report a case of pseudoaneurysm caused by thyroid core needle biopsy and treated by surgical treatment.
Figures and Tables
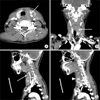 | Fig. 1The radiologic finding of the pseudoaneurysm (computed tomography). (A, B) The neck computed tomography of the left thyroid gland shows 2×2×3.2 cm sized large hematoma with abnormal vascular pooling in the left thyroid gland (arrows) (axial and coronal view). (C, D) Pseudoaneurysm (arrowhead) arises from the superior thyroidal artery (arrow) (sagittal view). |
 | Fig. 2The radiologic finding of the pseudoaneurysm (ultrasonography). (A) Ultrasonographic finding demonstrates heterogeneous echogenic swirling mass (2.3×1.9 cm) in the left thyroid gland. (B) Color Doppler identifies that the vascular flow in the pseudoaneurysm is originated from the superior thyroid artery (arrow) through the pseudoaneurysm neck (between the arrowheads). (C) Pseudoaneurysm with typical ‘to-and-fro’ color Doppler flow signal in the left lobe of thyroid gland. |
References
1. Kim HK. Diagnosis and treatment of iatrogenic pseudoaneurysm. J Surg Ultrasound. 2015; 2:69–73.
2. Na DG, Baek JH, Jung SL, Kim JH, Sung JY, Kim KS, et al. Core needle biopsy of the thyroid: 2016 consensus statement and recommendations from Korean Society of Thyroid Radiology. Korean J Radiol. 2017; 18(1):217–237.

3. Varetto G, Benintende E, Pagliasso E, Suita R, Garneri P, Castagno C, et al. Iatrogenic pseudoaneurysm of the superior thyroid artery. Vasa. 2013; 42(5):379–381.

4. Ha EJ, Baek JH, Lee JH, Kim JK, Choi YJ, Sung TY, et al. Complications following US-guided core-needle biopsy for thyroid lesions: a retrospective study of 6,169 consecutive patients with 6,687 thyroid nodules. Eur Radiol. 2017; 27(3):1186–1194.

5. Suh CH, Baek JH, Lee JH, Choi YJ, Kim KW, Lee J, et al. The role of core-needle biopsy in the diagnosis of thyroid malignancy in 4580 patients with 4746 thyroid nodules: a systematic review and meta-analysis. Endocrine. 2016; 54(2):315–328.

6. Noordzij JP, Goto MM. Airway compromise caused by hematoma after thyroid fine-needle aspiration. Am J Otolaryngol. 2005; 26(6):398–399.

7. Boey J, Hsu C, Collins RJ, Wong J. A prospective controlled study of fine-needle aspiration and Tru-cut needle biopsy of dominant thyroid nodules. World J Surg. 1984; 8(4):458–465.

8. Tsang K, Duggan MA. Vascular proliferation of the thyroid. A complication of fine-needle aspiration. Arch Pathol Lab Med. 1992; 116(10):1040–1042.
9. Jun YK, Jung SL, Byun HK, Baek JH, Sung JY, Sim JS. Radiofrequency ablation for iatrogenic thyroid artery pseudoaneurysm: initial experience. J Vasc Interv Radiol. 2016; 27(10):1613–1617.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download