Abstract
Purpose
We aimed to evaluate and compare the clinical and functional outcomes of dynamic hip screw (DHS) and proximal femoral nail antirotation (PFNA) treatment of AO type 1 intertrochanteric fractures in elderly patients.
Materials and Methods
We retrospectively reviewed 194 consecutive patients with type A1 intertrochanteric femoral fractures who were treated with DHS (n=113) or PFNA (n=81). We evaluated operation time, intraoperative blood loss, and functional outcomes, walking ability, and the Barthel activities index. Fracture union, sliding of hip screw, proximal femur shortening, and presence of complications were assessed radiologically at relevant follow-up intervals.
Results
The mean operation time and blood loss were significantly lower for the PFNA group, but walking ability and Barthel index decreased to a similar extent for both groups. However, patients in the DHS group complained of significantly more pain (P=0.049). Although there were no significant differences between the two groups with respect to the time until fracture union was achieved, patients in the DHS group exhibited a higher extent of proximal femoral shortening and sliding of the hip screw. Differences about hip screw sliding and proximal femur shortening within each subgroup were not significant.
Conclusion
Compared to DHS treatment, PFNA treatment of type A1 intertrochanteric fractures is associated with reduced blood loss, shorter operation time, and less severe pain after surgery. Additionally, sliding of the hip screw and proximal femur shortening are expected to occur more frequently after DHS.
Intertrochanteric femoral fractures occur mostly in the elderly and are associated with high mortality rates. Systemic or localized complications can occur during long-term bed rest. Early rehabilitation through stable reduction and firm internal fixation can be viewed as the most important treatment goal1). Although the type of orthopedic implant used for surgical treatment of intertrochanteric femoral fracture should be selected based on the pattern of fracture and the patient’s condition, the experience and preference of the surgeon performing the procedure often play the most important role in this selection process. For long time, dynamic hip screws (DHS) were the main treatment option2), but proximal femoral nails have recently gained wide popularity3). Many researchers have reported on the outcomes of DHS and proximal femoral nails in the treatment of unstable trochanteric fractures4); however, there have been few studies regarding the treatment outcomes for stable trochanteric fractures, as such fractures can be easily overlooked. The surgical treatment of stable trochanteric fractures is uncontroversial, and good results regarding fracture union and a reduced need for revision surgery can be expected with various implants5). However, caution should be taken in cases involving elderly patients with osteoporosis, since postoperative reduction loss is not all that rare in such patients, even for stable fractures. In particular, most previous studies involving patients with stable trochanteric fractures have focused on evaluating different surgical methods and implants, with the primary aim to reduce the rate of fracture complication and reoperation6). Besides this key task, it is equally important to evaluate the outcome from the patients’ perspective, that is, postoperative hip function and health-related quality of life. The present study aimed to address this need, and included elderly patients with stable intertrochanteric femoral fracture, treated using DHS (Synthes, Zuchwil, Switzerland) or proximal femoral nail antirotation (PFNA) implants (Synthes); the ultimate objective was to compare the clinical and radiological outcomes of the two treatment approaches in elderly patients.
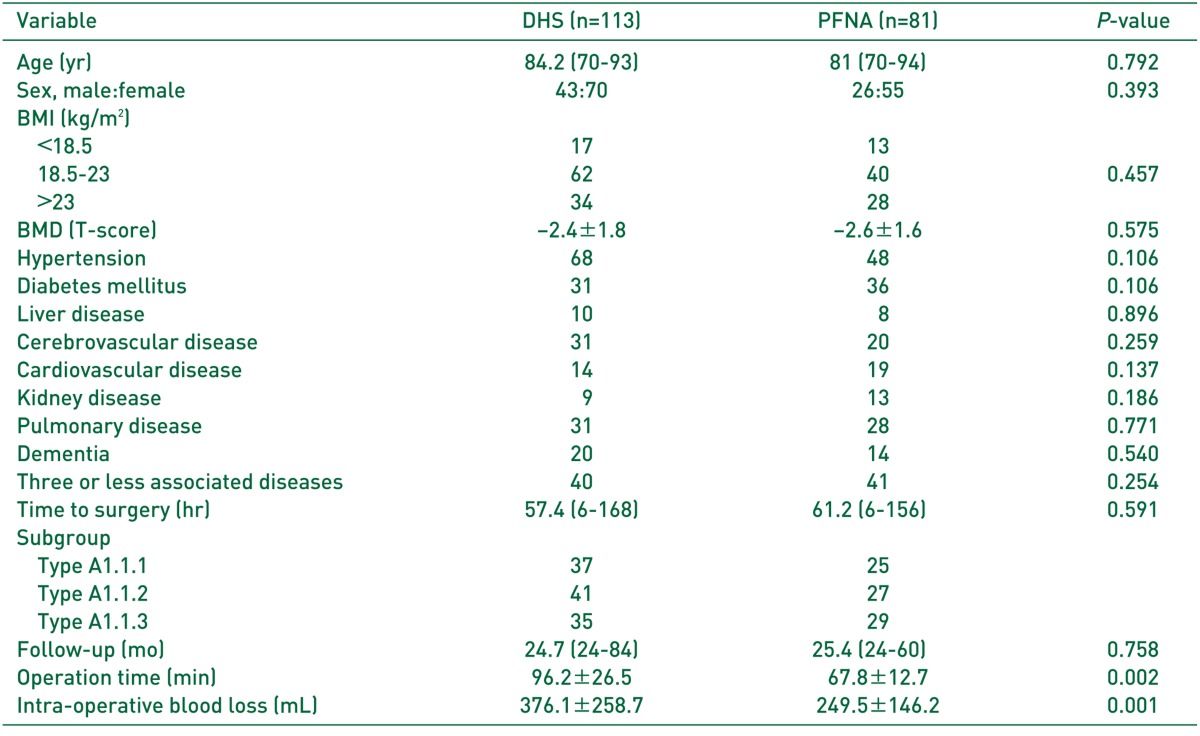
Out of 812 patients (867 hip joints) who were admitted and treated for intertrochanteric femoral fracture between January 2004 and December 2014, those younger than 70 years, with AO fracture classification of type 2 or higher7), with bilateral fracture, and who were not functionally ambulant were excluded, while those who were followed up for one year or longer were included. As a result, 113 cases treated with DHS (DHS group), and 81 cases treated with PFNA (PFNA group) were included in the study. Regarding the DHS and PFNA groups, respectively: mean patient age, 84.2 (70-93) years and 81.0 (70-94) years; male to female ratio, 43:70 and 26:55; mean follow-up period, 24.7 (12-84) months and 25.4 (14-60) months (Table 1). The AO/OTA classification system7) was used to classify trochanteric fractures as types 1, 2, and 3 fractures, and patients selected for the present study were all patients with type A1 fracture. The cases were classified into three subgroups (DHS subgroup, 37/41/35; PFNA subgroup, 25/27/29) according to AO/OTA classification and and were compared the clinical and radiological results (Table 1).
A three surgeon performed all surgical procedures and, surgery was performed within an average of 2.5 days from the injury. In cases accompanied by other diseases, surgery was performed after sufficient examination and evaluation. In all cases, surgery was performed under general or spinal anesthesia, with the patient placed on a fracture table, and after closed reduction under fluoroscopy. As this was a retrospective study, there was no special indication for choosing between DHS and PFNA. However, DHS was when the diameter of the bone marrow was insufficient to hold the smallest diameter nail used for PFNA. On the other hand, PFNA was available when the proximal femur presented with a deformation that made it difficult to use the DHS plate, which has a straight shape. The DHS group received a 135°-angled plate, and, for achieving contact between the plate and the fracture area, an image intensifier was used for the medial cortex based on the anteroposterior radiographs, while image intensifier was used for the anterior cortex based on the lateral radiographs. In cases with severe displacement, valgus reduction and over-correction of the proximal fragments were attempted. There were no cases in which open reduction was attempted, and for positioning the hip screws, central and inferior or posteroinferior positions were preferred, while efforts were also taken to ensure that the tip-apex distance did not exceed 20 mm. The reduction method used for the PFNA group was similar to that used for DHS group. After reaming the lateral cortex, a helical blade was inserted, followed by the insertion of distal locking screws. The size of the nail was determined based on the preoperative radiographs, and, for all patients, the neck-shaft angle was 130°, with a length of 170 mm (49 cases) or 200 mm (32 cases). Active range of motion exercise was initiated, on average, two days after postoperative acute pain had subsided, and partial weight-bearing gait was initiated using crutches or a walker, depending on the patient’s overall condition.
Retrospective analysis was performed, and information regarding operating time, amount of bleeding, postoperative complications, and additional treatments were obtained from the patients’ medical records. The operation time was evaluated from the start to the end of anesthesia. The total amount of blood lost during the surgery was measured as the sum of the volume of the blood collected through the suction bottle and the volume of the bloodsoaked gauze. The degree of osteoporosis was assessed based on the bone mineral density (T-score) in the contralateral hip area, which did not differ significantly between the DHS and PFNA groups (−2.4±1.8 points vs. −2.6±1.6 points; P=0.575). The two groups were also compared in terms of underlying diseases (especially dementia or ≥3 associated diseases) that may affect the functional recovery of performance in activities of daily living (Table 1).
The results from the postoperative clinical and radiological studies were assessed by two orthopedic residents who did not participate in the surgery. The radiological evaluations were performed by comparing the anteroposterior and lateral radiographs taken immediately after the surgery, with the patient’s latest radiographs. Kappa coefficient tests were applied for intra-rater (K1) and inter-rater (K2) reliability, and both categories were found to be at a reliable level (K1=0.88, K2=0.81).
Pain, walking ability, and performance in activities of daily living were clinically evaluated pre- and postoperatively. Pain was evaluated by using a scale (slight, moderate, and severe) according to the criteria reported by Hardy et al.3), while walking ability was evaluated as reported by Koval et al8). Meanwhile, performance in activities of daily living was evaluated by using the Barthel index9).
Radiological determination of fracture healing was made based on: absence of false motion or tenderness in the fracture; observation of 3 or 4 cortical bridge on anteroposterior and lateral radiographs; progressive loss of fracture line. The sliding distance of the hip screws, and the shortening in the fracture site were evaluated by comparing the preoperative and final postoperative anteroposterior radiographs. In order to normalize the radiographs for different magnification, the ratios between the entire screw lengths as observed in the radiographs taken immediately following surgery and the ones taken during the final postoperative follow-up were used as adjusting factors. Postoperative degree of sliding was divided by the adjusting factor, and the difference relative to the preoperative degree of sliding was calculated accordingly. Evaluation regarding shortening of the fracture site was made by measuring the distance between a line passing through the center of the femoral head and the most distal screw fixed on the femoral shaft. The position of the lag screw within the femoral head was assessed and fixation failure was defined when we observed: varus deformity with a change of ≥10° in the angle between the shaft and the head of the femur; femoral head cut-out caused by the lag screw; or excessive sliding (≥15 mm)10).
All statistical processing was performed by using the SPSS Statistical package (ver. 17.0; SPSS Inc., Chicago, IL, USA). Student t-test, chi-square test, oneway ANOVA analysis were used to statistically analyze. A P-value of less than 0.05 was considered statistically significant. The design and protocol of this retrospective study were approved by the institutional review board of our hospital (GJVH-IRB No. 2015-13-1).
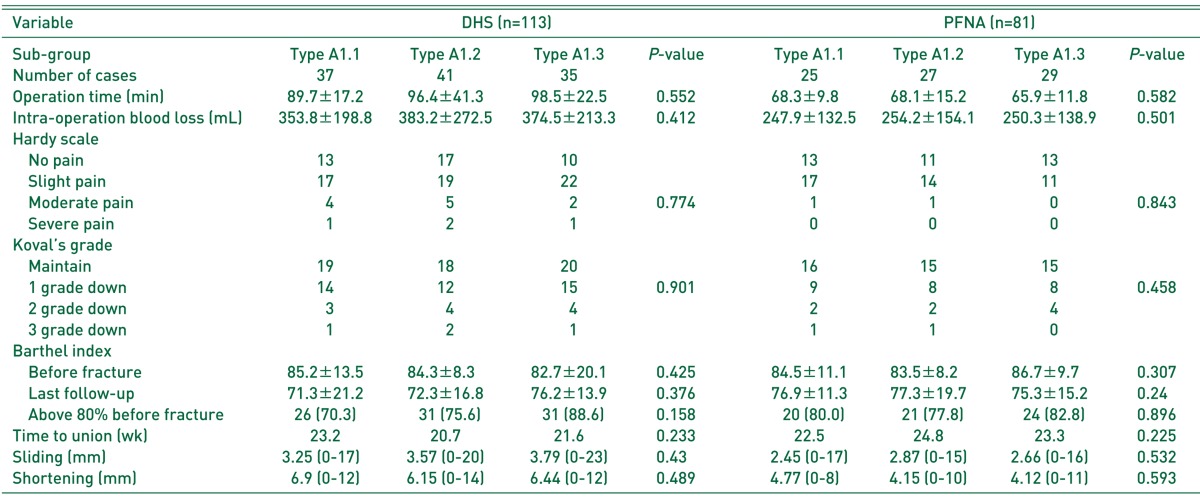
When compared to the DHS group, the PFNA group exhibited shorter mean operating times (respectively, 96.2±26.5 minutes and 67.8±12.7 minutes; P=0.002), counted from the start until the termination of anesthesia; and less bleeding (respectively, 376.1±258.7 mL and 249.5±146.2 mL; P=0.001) (Table 1). However, Differences in bleeding amout (P=0.552, 0.582) and operation times (P=0.412, 0.501) within each subgroup (DHS subgroup and PFNA subgroup) were not significant (Table 2).
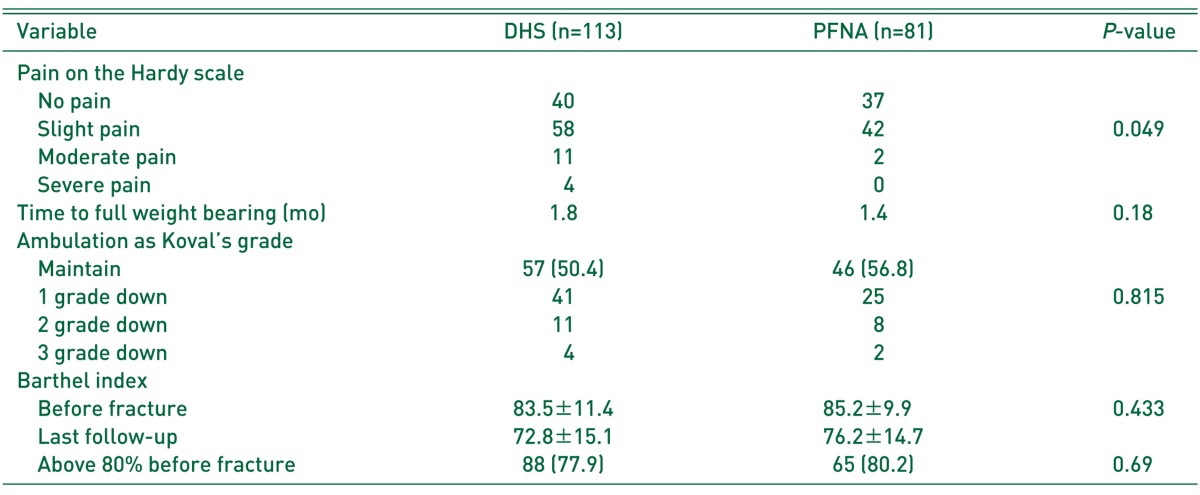
Pain during the final follow-up was assessed according to the criteria reported by Hardy et al3). The results regarding pain for the DHS and PFNA groups were, respectively: no pain, 40 and 37; slight pain, 58 and 42; moderate pain, 11 and 2; severe pain, 4 and 0. None of the PFNA groups exhibited any case of severe pain (P=0.049) (Table 3). The pain showed no significant difference within each subgroup (DHS subgroup and PFNA subgroup) (P=0.774, 0.843) (Table 2). The difference in the mobility score, as reported by Koval et al.8) was not statistically significant between prior to injury and the final follow-up (P=0.88), with a similar clinical decline in both groups. The number of cases in which the walking ability was recovered to pre-injury state was, for the DHS and PFNA groups, respectively: 57 (50.4%) and 46 (56.8%). The mean duration for which full-weight-bearing walking was performed was 1.8 months for the DHS group and 1.4 months for the PFNA group (P=0.18) (Table 3). And differences about walking ability within each subgroup (DHS subgroup and PFNA subgroup) were not significant (P=0.901, 0.458) (Table 2). With respect to performance in activities of daily living, measured according to the Barthel index (mean±standard deviation)9), the DHS group exhibited a preoperative score of 83.5±11.4 and a final follow-up score of 72.8±15.1, while the PFNA group exhibited a preoperative score of 85.2±9.9 and a final follow-up score of 76.2±14.7; no statistically significant difference between the two groups was observed (P=0.433). Eighty-eight patients (77.9%) from the DHS group and 65 (80.2%) from the PFNA group exhibited ≥80% recovery regarding performance in activities of daily living (Table 3). Patients who exhibited over the 80% of the Barthel index (performance in activities of daily living) recovery in final follow-up within each subgroup (DHS subgroup and PFNA subgroup) showed no significant difference (P=0.158, 0.896) (Table 2).
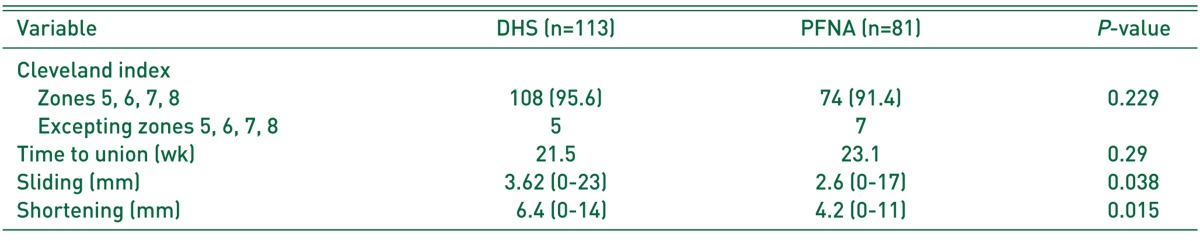
Using the index reported by Cleveland et al.11), 108 cases (95.6%) in the DHS group and 74 cases (91.4%) in the PFNA group were found to be in zones 5-8, which are zones associated with low complications rates. The mean fracture union time was 21.5 weeks for the DHS group and 23.1 weeks for the PFNA group, and the difference was not statistically significant (P=0.29) (Table 4). Differences in fracture union time within each subgroup (DHS subgroup and PFNA subgroup) were not significant (P=0.233, 0.225) (Table 2).
The mean hip screw sliding was 3.62 (0-23) mm for the DHS group and 2.6 (0-17) mm for 79 cases of the PFNA group, from which 2 cases, in which screw cut-through into the femoral head was observed, were excluded; therefore, hip screw sliding was significantly greater in the DHS group (P=0.038). Differences about hip screw sliding among subgroup within each group (DHS subgroup within DHS group and PFNA subgroup within PFNA group) were not significant (P=0.430, 0.532) (Table 2).
The mean proximal femur shortening was 6.4 (0-14) mm for the DHS group and 4.2 (0-11) mm for the PFNA group; therefore, proximal femur shortening was significantly greater in DHS group (P=0.015) (Table 4). The proximal femur shortening showed no significant difference among subgrup within each group (DHS subgroup within DHS group and PFNA subgroup within PFNA group) (P=0.489, 0.593) (Table 2). Fixation failure occurred in four cases (3.5%) for the DHS group (subgroup A1.1, two cases; A1.2, one case; A1.3, one case) and 2 cases (2.5%) for the PFNA group (subgroup A1.1, one cases; A1.2, one case). The treatment for the four cases of fixation failure that occurred in the DHS group was as follows: one case of switching to artificial hip replacement due to hip screw cut out; one case of mal-union without any additional treatments despite early reduction loss due to intraoperative fracture caused by lateral wall reaming (Fig. 1); two cases of switching to artificial hip replacement due to non-union. The treatment for the two cases of fixation failure that occurred in the PFNA group was as follows: one case of achieving union through intramedullary nail replacement and lateral cortical notching due to non-union accompanied by nail breakage; one case of artificial hip replacement being performed due to cut-through by the helical blade (Fig. 2, Table 5). Helical blade cut-through into the femoral head was suspected in one patient from the PFNA group; however, no revision surgery or additional treatment was performed, because union occurred without head penetration. Therefore, this case was not included when calculating fixation failure rates.
In DHS group, one case of superficial infection was treated with antibiotic therapy and debridement, while one case of deep infection was treated with antibiotic bead insertion, debridement, and lavage. The inserted bead was not removed because the patient and guardian refused an additional surgical procedure. In the PFNA group, there were no cases of infection.
Successful treatment of proximal femur fractures depends not only on the type of internal fixture used, but on various other factors as well, including bone quality, fracture type, degree of reduction, patient’s age, and comorbidities 12). There is an ongoing debate regarding the most suitable internal fixtures for the treatment of intertrochanteric fracture. Traditionally, extramedullary devices (DHS) are considered the gold standard for treating stable intertrochanteric fractures, because such devices lead to reproducible, reliable results. While plates and sliding screws offer mechanical advantages13), their use is sometimes associated with complications, the most common of them being progressive collapse in varus through the femoral head, with proximal migration and possibly screw cut-out in the head1415). In addition, the rate of fixation failure has been reported at 10-23%, associated with various factors as follows: long operation time; high blood loss; increase in femur lever arm, due to the fact that the DHS plate is located on the lateral side of the mechanical axis of the femur; femur head perforation by the hip screw, caused by excessive sliding and increased bending forces in trochanteric fractures complicated with osteoporosis; and lateral displacement of the greater trochanter, and shortening of the low exterimity16). In our present study, we found no significant difference between the patients treated with DHS and those treated with PFNA with respect to fixture failure rate (Table 4), even though operation time, blood loss, and hip screw sliding were higher for patients treated with DHS (Table 1). For PFNA patients, the lack of complications associated with postoperative infection is likely explained by the significantly shorter operation time and reduced blood loss. In our study, sliding was 3.6±2.9 mm in the DHS group, and 2.6±1.4 mm in the PFNA group, and this difference was statistically significant (P=0.038). Reduced sliding of the PFNA helical blade is likely explained by the fact that, when the helical blade is inserted into the cancellous bone and locked, a certain amount of pressure is applied to the fracture site during locking, allowing for greater rotational stability than in the case of a conventional hip screw. In the case of DHS treatment, excessive sliding occurred when there was deficiency in the cancellous bone of the distal fragment; it was shown that even when stability of the posteromedial cortex is achieved during surgery, excessive sliding can still occur if cancellous bone deficiency exists. Other potential causes include: preexisting cortical fracture difficult to note on plain radiographs; collapse of cortical bone contact during bone union and weight bearing processes; movement of proximal fragment towards the area with bone deficiency; comminuted fracture difficult to note on plain radiographs; and additional bone damage incurred during surgery. In the present study, the intramedullary fixture of choice was a PFNA implant containing a helical blade instead of hip screw. Brunner et al.17) reported three cases where the PFNA blade penetrated the femoral head without causing varus or rotational deformity at the fracture site, as verified by radiography at six months postoperative. In one case, penetration occurred following a fall, and in another case the suspected cause was a clinically unconfirmed infection; however, no specific cause was identified in the remaining case. In the present study, proximal migration of the helical blade was found in two patients, without blockage of the distal end of helical blade by the lateral femoral cortex or callus formation on the lateral wall, suggesting that the problem may have been related to the PFNA implant itself. As such, caution and careful monitoring are deemed necessary in elderly patients suspected of having lower femoral bone density.
Kaufer18) described five variables that may affect the resistance of the combination of implant and fracture fragment, namely: bone quality, fragment geometry, fracture reduction, implant model, and implant choice. Among these, the latter three are under the control of the surgeon. The present study compared the outcomes of applying DHS, a typical extramedullary fixture, and those of applying PNFA, an increasingly popular intramedullary fixture, to treat type A1 intertrochanteric fracture, which is a representative form of stable fracture. The outcomes were assessed based on radiological findings and functional recovery indices, while ruling out factors which can affect the treatment outcome as a result of choices made by the surgeon. In a prospective study regarding quality of life in patients with stable intertrochanteric femoral fracture, Ekström et al.19) reported 55% recovery of pre-injury walking ability and 66% recovery of pre-injury performance of daily activities. Meanwhile, Setiobudi et al.20) reported that pre-injury walking ability was achieved at one year postoperatively in 47.35% of patients. These results are similar to those obtained in our present study. Specifically, patients in both groups showed 50% recovery of preinjury walking ability, and >75% of the patients showed ≥80% recovery of the performance of daily activities. However, there was no difference between the groups in terms of functional recovery. On the other hand, at the final follow-up, the patients in the DHS group complained of severe pain, which may be related to the protrusion of the screw or the shortening and varus of the proximal femur due to excessive sliding of the compression hip screw. In elderly patients with severe osteoporosis, even stable intertrochanteric fractures require more attention at the time of surgery.
In the present study, we found that bone union was achieved in 97.3% (110 out of 113) of patients treated with DHS, and in 98.8% (80 out of 81) patients treated by PFNA groups. These results suggest that reduced recovery of walking ability despite favorable radiological outcomes is related to persistent pain from the fracture itself, or pain caused by the surgery, especially in elderly patients, who typically exhibit incomplete recovery of muscle strength, limited walking ability, as well as low motivation for rehabilitation. Another study21) reported a higher rate of recovery of pre-injury walking ability (74%), but this study involved relatively younger patients. Moreover, trochanteric fractures often occur in elderly patients with osteoporosis when they have poor health or gait conditions; in such patients, a decrease in walking ability and diminished performance of daily activities can cause significant socioeconomic burden throughout the patient’s remaining life. Therefore, careful choice of surgical approach and postoperative rehabilitation is essential, even for stable trochanteric fractures.
The main strength of our study is that we reviewed a significant number of patients with stable fractures. Furthermore, by reporting the failure of the stable intertrochanteric fracture, we hope to increase the awareness of certain key aspects that should be considered by the chief surgeons, who typically expect good outcomes in the management of such fractures. PFNA may be more advantageous in the treatment of stable intertrochanteric fracture for patients with osteoporosis, when the following aspects are considered: intraoperative blood loss, operation time, loss of quality of life associated with sliding of the compression hip screw and the deformation of the proximal femur (e.g., varus or shortening).
Limitations of the present study include the retrospective study design, and the short follow-up period. Therefore, to verify the conclusions of our investigation, a prospective, large-scale clinical study and a cadaveric biomechanical experiment are warranted. Additionally, we expect that some of pain after surgery, sliding of the compression hip screw, and deformation of the proximal femur we noted in our study population might be related to the fact that most of the patients live in a culture where many activities are performed while sitting on the floor (sitting in a squatting position, lying on the floor, etc.). This aspect should be investigated in future studies. In cases involving type A1 intertrochanteric fractures, which are expected to have good treatment outcomes due to the fracture type being relatively stable, fixation failure occurred in approximately 3.5% and 2.5% of patients treated with DHS and PFNA, respectively. Since osteoporotic hip fracture occurring in elderly individuals is a significant event regardless of its severity, careful attention is needed during the reduction and surgery.
To summarize, when it comes to the surgical treatment of type A1 intertrochanteric fracture, which is a relatively stable type of fracture, we found no differences between the groups of patients treated with DHS and PFNA in terms of fracture union, union time, recovery of walking ability, or recovery of performance of activities of daily living. However PFNA was associated with reduced blood loss, reduced duration of surgery, less postoperative pain, less frequent sliding of hip screws, and reduced occurrence of proximal femur shortening.
References
1. Siegmeth AW, Gurusamy K, Parker MJ. Delay to surgery prolongs hospital stay in patients with fractures of the proximal femur. J Bone Joint Surg Br. 2005; 87:1123–1126. PMID: 16049251.

2. Rao JP, Banzon MT, Weiss AB, Rayhack J. Treatment of unstable intertrochanteric fractures with anatomic reduction and compression hip screw fixation. Clin Orthop Relat Res. 1983; (175):65–71.

3. Hardy DC, Descamps PY, Krallis P, et al. Use of an intramedullary hip-screw compared with a compression hip-screw with a plate for intertrochanteric femoral fractures. A prospective, randomized study of one hundred patients. J Bone Joint Surg Am. 1998; 80:618–630. PMID: 9611022.

4. Kumar R, Singh RN, Singh BN. Comparative prospective study of proximal femoral nail and dynamic hip screw in treatment of intertrochanteric fracture femur. J Clin Orthop Trauma. 2012; 3:28–36. PMID: 25983453.

5. Kaplan K, Miyamoto R, Levine BR, Egol KA, Zuckerman JD. Surgical management of hip fractures: an evidence-based review of the literature. II: intertrochanteric fractures. J Am Acad Orthop Surg. 2008; 16:665–673. PMID: 18978289.

6. Parker MJ, Handoll HH. Gamma and other cephalocondylic intramedullary nails versus extramedullary implants for extracapsular hip fractures in adults. Cochrane Database Syst Rev. 2005; (4):CD000093. PMID: 16235272.

7. Kregor PJ, Obremskey WT, Kreder HJ, Swiontkowski MF. Evidence-Based Orthopaedic Trauma Working Group. Unstable pertrochanteric femoral fractures. J Orthop Trauma. 2005; 19:63–66. PMID: 15668589.
8. Koval KJ, Aharonoff GB, Rosenberg AD, Bernstein RL, Zuckerman JD. Functional outcome after hip fracture. Effect of general versus regional anesthesia. Clin Orthop Relat Res. 1998; (348):37–41. PMID: 9553531.
9. Mahoney FI, Barthel DW. Functional evaluation: the Barthel index. Md State Med J. 1965; 14:61–65.
10. Madsen JE, Naess L, Aune AK, Alho A, Ekeland A, Strømsøe K. Dynamic hip screw with trochanteric stabilizing plate in the treatment of unstable proximal femoral fractures: a comparative study with the Gamma nail and compression hip screw. J Orthop Trauma. 1998; 12:241–248. PMID: 9619458.

11. Cleveland M, Bosworth DM, Thompson FR, Wilson HJ Jr, Ishizuka T. A ten-year analysis of intertrochanteric fractures of the femur. J Bone Joint Surg Am. 1959; 41-A:1399–1408. PMID: 13849408.

12. Lorich DG, Geller DS, Nielson JH. Osteoporotic pertrochanteric hip fractures: management and current controversies. Instr Course Lect. 2004; 53:441–454. PMID: 15116633.
13. Verhofstad MH, van der Werken C. DHS osteosynthesis for stable pertrochanteric femur fractures with a two-hole side plate. Injury. 2004; 35:999–1002. PMID: 15351666.

14. Kim WY, Han CH, Park JI, Kim JY. Failure of intertrochanteric fracture fixation with a dynamic hip screw in relation to pre-operative fracture stability and osteoporosis. Int Orthop. 2001; 25:360–362. PMID: 11820441.

15. Baumgaertner MR, Solberg BD. Awareness of tip-apex distance reduces failure of fixation of trochanteric fractures of the hip. J Bone Joint Surg Br. 1997; 79:969–971. PMID: 9393914.

16. Babst R, Renner N, Biedermann M, et al. Clinical results using the trochanter stabilizing plate (TSP): the modular extension of the dynamic hip screw (DHS) for internal fixation of selected unstable intertrochanteric fractures. J Orthop Trauma. 1998; 12:392–399. PMID: 9715446.

17. Brunner A, Jöckel JA, Babst R. The PFNA proximal femur nail in treatment of unstable proximal femur fractures--3 cases of postoperative perforation of the helical blade into the hip joint. J Orthop Trauma. 2008; 22:731–736. PMID: 18978550.

18. Kaufer H. Mechanics of the treatment of hip injuries. Clin Orthop Relat Res. 1980; (146):53–61. PMID: 7371269.

19. Ekström W, Miedel R, Ponzer S, Hedström M, Samnegård E, Tidermark J. Quality of life after a stable trochanteric fracture--a prospective cohort study on 148 patients. J Orthop Trauma. 2009; 23:39–44. PMID: 19104302.

20. Setiobudi T, Ng YH, Lim CT, Liang S, Lee K, Das De S. Clinical outcome following treatment of stable and unstable intertrochanteric fractures with dynamic hip screw. Ann Acad Med Singapore. 2011; 40:482–487. PMID: 22206063.
21. Liu Y, Tao R, Liu F, Wang Y, Zhou Z, Cao Y, Wang H. Mid-term outcomes after intramedullary fixation of peritrochanteric femoral fractures using the new proximal femoral nail antirotation (PFNA). Injury. 2010; 41:810–817. PMID: 20472234.

Fig. 1
Radiographs of a 77-year-old woman with left-sided type A1 intertrochanteric fracture treated with dynamic hip screws (DHS). (A) Preoperative anteroposterior radiographs suggesting type A1 intertrochanteric fracture. (B) Immediate postoperative radiographs showing reduction of fracture with DHS, and circular wiring fixation for the lateral wall fracture. (C) Proximal migration of greater trochanteric fragment at three months postoperatively. (D) Excessive sliding and shortening of proximal fracture fragment at 5 months postoperatively. (E) Antero-posterior radiographs showing complete union at 12 months postoperatively.
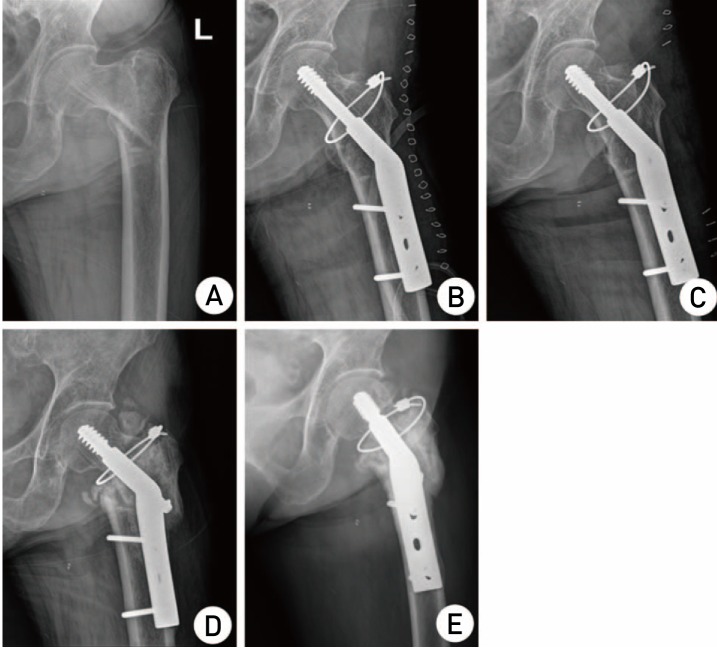
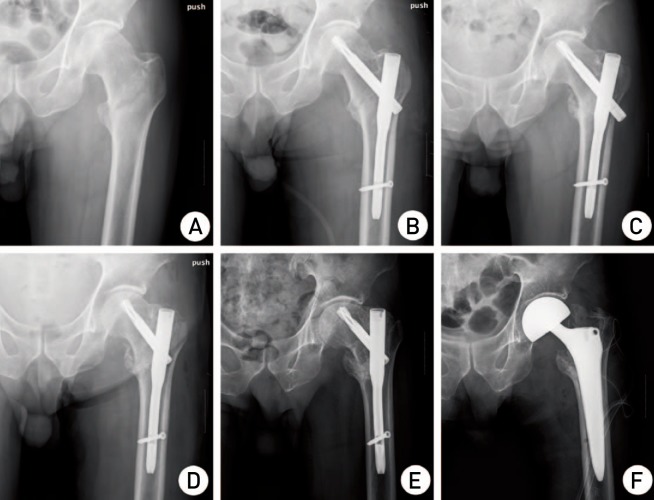
Fig. 2
Radiographs of a 77-year-old man with left-sided type A1 intertrochanteric fracture treated with proximal femoral nail antirotation (PFNA) implant. (A) Preoperative anteroposterior radiographs suggesting type A1 intertrochanteric fracture. (B) Immediate postoperative radiographs showing suitable reduction of fracture with PFNA. (C) Cut-through of helical blade at four months postoperatively, mandating reoperation. (D) Immediate postoperative radiographs showing replacement of helical blade with an autogenous bone graft. (E) Cut-through of helical blade at three months after reoperation. (F) Bipolar hemiarthroplasty was performed.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download