Abstract
Gastrointestinal stromal tumors (GISTs) are rare tumors of the gastrointestinal system and comprise only 1% to 3% of all gastrointestinal tract tumors, with the majority of them arising in the stomach. In this report, we present the unique findings of a case of gastroduodenal intussusception caused by an underlying gastric GIST and complicated with severe acute pancreatitis.
Gastrointestinal intussusception in adults is a rare condition and represents only 5% of all intussusceptions.1 Ileo-ileal and colo-colic intussusceptions are the most common types of gastrointestinal intussusceptions in adults. Gastroduodenal intussusceptions are rare, and frequently result from the prolapse of an underlying pedunculated gastric wall lesion into the duodenum. Various pathologies like adenoma, leiomyoma, lipoma, hamartoma inflammatory fibroid polyp, adenocarcinoma, and leiomyosarcoma can cause this pathology.234 Gastrointestinal stromal tumors (GISTs) comprise only 1% to 3% of all gastrointestinal tract tumors, with 60% of them arising in the stomach. They are reported to cause gastric gastrointestinal intussusceptions infrequently.56 In this report, we aimed to present radiologic and clinical findings of a unique case with gastroduodenal intussusception induced by an underlying gastric GIST and complicated with acute pancreatitis.
An 85-year-old woman complaining of abdominal and epigastric discomfort, nausea, and weight loss during the last 6 months was referred to a gastrointestinal clinic for further evaluation. Her body mass index was 27 kg/m2. Laboratory tests including complete blood count and biochemistry panel were within the normal range. A 6 by 5 cm epigastric mass was found by abdominal ultrasonography using an Aplio XG scanner equipped with a 5-MHz convex transducer (Toshiba Medical Systems, Tokyo, Japan). An intravenous (IV) contrast-enhanced computed tomography (CT) demonstrated a diffusely enhancing luminal mass at the gastric fundus (Fig. 1). There was no sign of extraluminal invasion or metastasis. The patient did not provide consent for gastric endoscopy and was discharged from the hospital upon her demand. One month after the initial presentation, the patient presented at the emergency department with severe acute abdominal pain radiating to the back, accompanied with nausea and vomiting. Laboratory findings were suggestive of an acute inflammatory response (white blood cell 21.66×109/L, C-reactive protein 0.9 mg/L, serum albumin 2.6 g/dl, serum glucose 185 mg/dl, and serum chlorine 110 mmol/L). Amylase and lipase values were elevated (1,974 IU/L and 1,503 IU/L, respectively), whereas liver enzymes and bilirubin values were within the normal range. A control IV contrast-enhanced CT study showed a gastric mass protruding toward the duodenum and obliterating the gastric exit and duodenal lumen. Gastric wall thickening and gastroduodenal intussusception were evident. The common biliary duct was compressed by the mass and resulted in dilation of the proximal biliary system. Pancreatic swelling, edema, and irregular peripancreatic mesenteric fat stranding were suggestive of acute pancreatitis (Fig. 2). Abdominal laparotomy revealed gastroduodenal intussusception due to a gastric mass arising from the superior part of the corpus. The obstruction of the ampulla vateri and consequent edema and necrosis in the pancreas were also visible during surgery after exploration of the retrocolic region. Because of the location, size, and extent of the mass, wedge resection was opted out as a surgical option. The patient underwent subtotal gastrectomy and Roux and Y anastomosis (Fig. 2). Histopathologic evaluation of the tumor specimen was most compatible with benign gastric GIST demonstrating proliferation of spindle cells with long oval nuclei.
In this report, we present the findings of a case of gastroduodenal intussusception caused by an underlying gastric GIST complicated with acute pancreatitis. According to our literature review, this is the first reported case of gastric GIST presenting with gastroduodenal intussusception accompanied with acute pancreatitis.
GISTs are rare tumors of the gastrointestinal system and account for 5% to 6% of all sarcomas. They comprise only 1% to 3% of all gastrointestinal tract tumors, with 60% of them arising in the stomach.6 The usual symptom is abdominal discomfort, but they may cause gastrointestinal obstruction in 10% to 30% of cases. Bleeding of the GISTs may present clinically with melena, hematemesis, or iron deficiency anemia.7 Abdominal pain usually occurs around the epigastric region, and has a sudden onset and intermittent character with possible accompanying vomiting. GISTs may be detected with gastric endoscopy as an endophytic mass with a smooth bright surface. Endoscopic ultrasound may be helpful in further evaluation of the mass, particularly in assessing the level of gastric wall involvement. Contrast-enhanced CT scan is currently the imaging modality of choice. Unlike endoscopy, it provides details beyond the gastric lumen and is critical in preoperative assessment. Magnetic resonance imaging is also helpful in the assessment of large exophytic masses. Surgical excision is the treatment of choice if the tumor is determined to be resectable. Care must be taken during resection as most gastric GISTs have a pseudocapsule formation and rupture may result in tumor spillage.8
Gastroduodenal intussusception induced by gastric GISTs is a very rare cause of gastroduodenal obstruction.9 Surgery may be needed for definitive diagnosis.10 Another rare complication of gastric GISTs is acute pancreatitis caused by duodenal obstruction. A few studies have also reported acute pancreatitis induced by a gastric hyperplastic polyp prolapsing into the duodenum.1112 In most reports of gastric mass-induced acute pancreatitis, the masses tended to arise in the distal part of stomach, mainly the antrum.11 According to our review, there are three case reports in the English literature presenting acute pancreatitis secondary to prolapsed gastric GISTs.131415 In one of these cases, the mass originated from the gastric antrum, whereas the masses originated from the gastric fundus in the other two cases. In all three cases, the masses were prolapsed into the duodenum and induced acute pancreatitis. No intussusception was reported in all three cases.
In conclusion, we report the unique case of acute pancreatitis induced by gastroduodenal intussusception in a patient with a previously known gastric GIST arising from the corpus and causing duodenal obstruction.
The study was retrospective and complied with ethical standards for retrospective research. No human or animal subjects were involved. Informed consent was provided for publication of the case reported here.
Figures and Tables
Fig. 1
Heterogenously enhancing endoluminal mass (arrows) arising from gastric fundus is seen on axial (A) and coronal (B) computed tomography images obtained after intravenous contrast administration at initial admission of the patient.

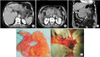
Fig. 2
(A) Gastroduedonal intussusception. (B, C) The mass protruding to the duedonum and causing obstruction (arrows). Also visible are stranding of the peripancreatic fat and fluid accumulation around heterogenously ehancing pancreas, a sign of early necrosis. (D) Macroscopic view of the mass arising from gastric corpus (arrow). (E) Perioperative view of pancreas. Please note relatively dark portion of the pankreas corresponding to pancreatic necrosis.
References
1. Stubenbord WT, Thorbjarnarson B. Intussusception in adults. Ann Surg. 1970; 172:306–310.
2. Vinces FY, Ciacci J, Sperling DC, Epstein S. Gastroduodenal intussusception secondary to a gastric lipoma. Can J Gastroenterol. 2005; 19:107–108.
3. Asai S, Kijima H, Yamamoto S, Shiraishi S, Suzuki T, Maeda Y, et al. Gastroduodenal intussusception secondary to pedunculated gastric carcinoma. J Ultrasound Med. 2008; 27:673–676.
4. Kim DJ, Lee JH, Kim W. Gastroduodenal intussusception resulting from large hyperplastic polyp. J Gastric Cancer. 2012; 12:201–204.
5. Rittenhouse DW, Lim PW, Shirley LA, Chojnacki KA. Gastroduodenal intussusception of a gastrointestinal stromal tumor (GIST): case report and review of the literature. Surg Laparosc Endosc Percutan Tech. 2013; 23:e70–e73.
6. Rossi CR, Mocellin S, Mencarelli R, Foletto M, Pilati P, Nitti D, et al. Gastrointestinal stromal tumors: from a surgical to a molecular approach. Int J Cancer. 2003; 107:171–176.
7. Laurini JA, Carter JE. Gastrointestinal stromal tumors: a review of the literature. Arch Pathol Lab Med. 2010; 134:134–141.
8. Galateros G, Simatos G, Lakiotis G, Stathaki M, Volteas S, Kafiri G, et al. Stromal tumors of the stomach: a clinicopathological study of 15 cases and review of the literature. Tumori. 2008; 94:459–463.
9. Crowther KS, Wyld L, Yamani Q, Jacob G. Case report: gastroduodenal intussusception of a gastrointestinal stromal tumour. Br J Radiol. 2002; 75:987–989.
10. Patil DT, Rubin BP. Gastrointestinal stromal tumor: advances in diagnosis and management. Arch Pathol Lab Med. 2011; 135:1298–1310.
11. Galeano-Cassaz C, Bonnet S, Chereau N, Dousset B, Lamarque D, Douard R. Gastric polyp prolapsed into the duodenum as a rare cause of acute pancreatitis. Ann R Coll Surg Engl. 2010; [In print].
12. de la Cruz RA, Albillos JC, Oliver JM, Dhimes P, Hernandez T, Trapero MA. Prolapsed hyperplastic gastric polyp causing pancreatitis: case report. Abdom Imaging. 2001; 26:584–586.
13. Jones O, Monk D, Balling T, Wright A. Acute pancreatitis secondary to a prolapsed gastric fundal GIST. Int J Surg Case Rep. 2012; 3:82–85.
14. Senadhi V, Arora D, Jani N. Gastrointestinal stromal tumor (GIST) presenting with acute pancreatitis. Endoscopy. 2011; 43:Suppl 2 UCTN. E76.
15. Sun J, Shen X, Li Z, Zhu J. A rare case of acute pancreatitis induced by a gastrointestinal stromal tumor arising from the gastric fundus. Endoscopy. 2012; 44:Suppl 2 UCTN. E426–E427.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download