Abstract
Purpose
To evaluate the prevalence of esophageal reflux-induced symptoms after gastrectomy owing to gastric cancer and assess the relationship between esophageal reflux-induced symptoms and quality of life.
Materials and Methods
From January 2012 to May 2012, 332 patients were enrolled in this cross-sectional study. The patients had a history of curative resection for gastric cancer at least 6 months previously without recurrence, other malignancy, or ongoing chemotherapy. Esophageal reflux-induced symptoms were evaluated with the GerdQ questionnaire. The quality of life was evaluated with the European Organization for Research and Treatment QLQ-C30 and STO22 questionnaires.
Results
Of the 332 patients, 275 had undergone subtotal gastrectomy and 57 had undergone total gastrectomy. The number of GerdQ(+) patients was 58 (21.1%) after subtotal gastrectomy, and 7 (12.3%) after total gastrectomy (P=0.127). GerdQ(+) patients showed significantly worse scores compared to those for GerdQ(-) patients in nearly all functional and symptom QLQ-C30 scales, with the difference in the mean score of global health status/quality of life and diarrhea symptoms being higher than in the minimal important difference. Additionally, in the QLQ STO22, GerdQ(+) patients had significantly worse scores in every symptom scale. The GerdQ score was negatively correlated with the global quality of life score (r=-0.170, P=0.002).
Conclusions
Esophageal reflux-induced symptoms may develop at a similar rate or more frequently after subtotal gastrectomy compared to that after total gastrectomy, and decrease quality of life in gastric cancer patients. To improve quality of life after gastrectomy, new strategies are required to prevent or reduce esophageal reflux.
Gastric cancer is still prevalent throughout the world, and long-term survival has increased owing to early detection, improved surgical techniques, and combined therapy.1 After gastrectomy, anatomical changes and loss of function induce various symptoms that may affect a patient's quality of life (QoL) after surgery. Therefore, postoperative QoL has received considerable attention, in addition to oncological outcomes, as there are many factors affecting QoL after curative gastric resection for gastric cancer.2 In the general population, symptomatic gastroesophageal reflux disease (GERD) negatively affects patients' QoL.3,4 Healthy individuals have anatomical features in the esophagogastric junction, which prevent esophageal reflux. These anatomical features may be disrupted after gastric surgery, resulting in esophageal reflux. Taken together, we can assume that a fair number of gastric cancer patients may suffer from reflux-related symptoms after gastrectomy, which may negatively affect their QoL. The prevalence and severity of reflux-related symptoms differ according to the extent of resection and/or reconstruction methods.5,6,7 Some studies have evaluated the reflux itself, assessed by scintigraphic methods, bilimetry, intraesophageal pH monitoring, or endoscopic changes of the esophageal mucosa.8,9,10 However, these studies did not evaluate the impact of reflux-related symptoms on QoL after gastrectomy.
We were interested in the esophageal reflux-related symptoms and their correlation with QoL. A recent study in our institute investigated GERD using the GerdQ questionnaire.11 The GerdQ is a self-administered, patient-oriented questionnaire developed by combining 6 questions from 3 different validated tools (the Reflux Disease Questionnaire, Gastrointestinal Symptom Rating Scale, and GERD Impact Scale),12,13,14 which are considered to have a high accuracy for symptom-based diagnosis of GERD in the general population.15,16,17 Therefore, the GerdQ questionnaire was used to evaluate esophageal reflux symptoms in this study.
Furthermore, the European Organization for Research and Treatment (EORTC) QLQ-C30 and QLQ-STO22 questionnaires were used for evaluating the QoL in this study. Since its release in 1993, the EORTC QLQ-C30 has become one of the most widely used 'core' instruments for the study of the health-related QoL of cancer patients, having been translated into several languages and used in hundreds of studies. The 14 single-item and multi-item scales in the EORTC QLC-C30 questionnaire assess physical and psychosocial functioning, key symptoms, and overall health-related QoL. The QLQ-C30 and its QLQ-STO22 disease-specific questionnaire module for patients with gastric cancer are used in combination, and these questionnaires are usually selected because they are fully validated, translated into many languages, and adequate for multicultural comparisons.2,18
In this study, we evaluated reflux-related symptoms using the GerdQ questionnaire and analyzed the prevalence of reflux-related symptoms and their impact on QoL after gastrectomy in gastric cancer patients.
This study was cross-sectional in design and was carried out at the Gastric Cancer Hospital, Gangnam Severance Hospital (Seoul, Korea). Eligible patients had a history of curative resection for gastric cancer >6 months previously and the ability to understand the nature of the study and communicate with the study personnel. Patients with evidence of recurrence of gastric cancer or any other malignancy, and those receiving chemotherapy were excluded from the study. Patients were recruited when they visited outpatient clinics in Gangnam Severance Hospital for follow-up or investigation of gastrointestinal symptoms from January 2012 to May 2012. The study was approved by the institutional review board at the Gangnam Severance Hospital (IRB #3-2012-0054). Demographic data on gender and age, and clinical data were collected from patient interviews and medical records.
A total of 346 patients visited our clinic during the study period and completed the questionnaires. We excluded 1 patient with recurrent gastric cancer, 1 patient with liver metastasis, and 12 patients who did not complete the GerdQ correctly. As a result, the data from a total of 332 patients were analyzed.
Postoperative symptoms related to esophageal reflux were assessed using the GerdQ questionnaire (Korean translation). The GerdQ questionnaire is composed of 4 positive predictors of GERD (heartburn, regurgitation, sleep disturbance due to reflux symptoms, and the use of over-the-counter medication; questions 1, 2, 5, and 6, respectively), and 2 negative correlates with GERD (epigastric pain and nausea; questions 3 and 4, respectively).14,19 The GerdQ scores were based on the frequency of 6 items during the past 7 days ranging from 0 to 3 for the positive predictors, and from 3 to 0 (in reversed order, with 3 representing 'none') for negative predictors. The total GerdQ score is calculated as the sum of these scores, ranging from 0 to 18. Patients without any symptoms will have a GerdQ score of 6, and GERD patients will have a GerdQ score of >8.15 In our study, patients with a total GerdQ score of >8 were assigned to the GerdQ (+) group, whereas patients with a total GerdQ score of 0 to 7 were assigned to the GerdQ (-) group.15
The QoL was assessed using the Korean version of the EORTC Core 30 (QLQ-C30) and a gastric cancer-specific module, the EORTC QLQ-STO22.20,21,22,23 The EORTC QLQ-C30 is a 30-item questionnaire, with both multi-item scales and single-item measures, including 5 functional scales (physical, role, cognitive, emotional, and social), 3 symptom scales (fatigue, nausea and vomiting, and pain), a global health status/QoL scale, and 6 single items (dyspnea, insomnia, appetite loss, constipation, diarrhea, and financial difficulties). The EORTC QLQ-STO22 consists of 22 items and includes 5 multi-item scales and 4 single-item measures.
All QLQ-C30 and QLQ-STO22 responses were scored using 4-point Likert scales and were linearly transformed to a 0 to 100 score according to the scoring manual provided by the EORTC. A high score for the global health status/QoL represents high QoL, and a high score for the multi-item functional scales represents a high/healthy level of functioning. Conversely, in symptom scales/single-items and all questions of the STO22, a high score reflects more symptoms or problems.24
Statistical analyses were completed using SPSS 19.0 (IBM Co., Armonk, NY, USA). The t-test and chi-square test were used to compare differences in clinicopathologic characteristics between the 2 groups, (t-test, for continuous variables; chi-square test, for nominal variables). QoL after gastrectomy in patients with gastric cancer was compared between the GerdQ (+) and GerdQ (-) groups.
For each domain of the QLQ-C30 and QLQ-STO22 questionnaires, we calculated the minimal important difference (MID), defined as the smallest change that patients would identify as important. We followed the EORTC published guidelines for the interpretation of clinically relevant differences in QLQ-C30 scores.25 However, similar guidelines are not available for the interpretation of QLQ-STO22 scores. We therefore defined the MID for the domains of QLQ-STO22 as an effect size >0.5, which empirically yields nearly identical values to the clinical interpretation of a 'moderate difference'.26,27 The effect size was calculated as the difference between the means in the 2 groups divided by the pooled standard deviation.28
The correlation between the GerdQ score and the global health status/QoL scale was analyzed. A P-value of <0.05 was considered statistically significant.
Three hundred and thirty-two patients were surveyed, including 215 men and 117 women (male : female=1.85 : 1) with a mean age of 59.8±11.6 years. The number of subjects in the GerdQ (+) and GerdQ (-) groups was 65 and 267, respectively. The mean postoperative follow-up duration was 49.7±81.1 months.
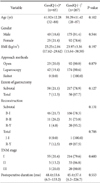
There were no significant differences in age, gender, or preoperative body mass index between the GerdQ (+) and GerdQ (-) groups. In addition, there were no significant differences in operation time, operative approach methods, TNM stage, or postoperative follow-up duration between the 2 groups (Table 1). Interestingly, only 12.3% of patients undergoing total gastrectomy suffered from reflux symptoms, whereas 21.1% of patients undergoing subtotal gastrectomy suffered from reflux symptoms. Although the prevalence of reflux symptoms was higher in patients after subtotal gastrectomy than after total gastrectomy, the difference was not statistically significant (P=0.127).
With regard to the MID, the difference between the means and MIDs was greater in the domains of the global health status/QoL, which means that the global health status/QoL in the GerdQ (+) group was worse than that in the GerdQ (-) group (Fig. 1). On the functional scales based on physical, role, emotional, cognitive, and social functioning, the score in the GerdQ (+) group was significantly lower than that in the GerdQ (-) group. However, the difference of the means was not greater than that of the MIDs. The EORTC QLQ-C30 guidelines did not provide the MID value for the emotional function domain.25 Therefore, we could not compare the difference of means and MIDs in that domain. The scores based on the symptom scales in the EORTC QLQ-C30 questionnaire are shown in Fig. 2. The scores in the GerdQ (+) group were significantly inferior to those in the GerdQ (-) group on most of the symptom scales. However, the difference of the means was greater than that of the MIDs only for diarrhea (Fig. 2).
Fig. 3 shows the effect sizes of the QLQ-STO22 domains. As expected, the effect size was >0.5 in the reflux domains, suggesting that the GerdQ (+) group had worse reflux symptoms compared to those in the GerdQ (-) group based on the EORTC QLQ-STO22 scores. Additionally, the effect size was >0.5 in the domains of eating restriction and body image.
The bivariate correlation analysis revealed that the GerdQ score was negatively correlated to the global health status/QoL scales (r=-0.170, P=0.002). Furthermore, the bivariate analysis performed in patients with a GerdQ score >6, revealed a negative correlation (r=-0.305, P<0.001) (Fig. 4).
GERD in the general population is one of the most common diseases in Western countries, while in Asia the incidence of GERD is relatively low.29 GERD consists of 2 types: reflux esophagitis (RE), diagnosed by endoscopic observation, and non-erosive reflux disease (NERD), mainly diagnosed on the basis of upper gastrointestinal symptoms. NERD patients make up more than half of all GERD patients.30 In addition, symptomatic GERD is associated with a substantial burden in affected individuals and society.3,4
Reflux and other duodenal contents in the esophagus following total gastrectomy is considered to be a serious complication and a Roux-en-Y reconstruction has been used for diversion of the duodenal juices.31 Furthermore, reflux following proximal gastrectomy might be worse than reflux after total gastrectomy.32,33 However, it is difficult to fully understand the incidence of esophageal reflux after gastrectomy, because some reports have evaluated the reflux itself, while other reports have evaluated the endoscopic findings of the esophageal mucosa. A few studies have evaluated the symptoms related to esophagitis using different survey methods.34,35 After gastrectomy, some patients showing symptoms suggestive of esophageal reflux such as heartburn and regurgitation did not demonstrate objective endoscopic findings.36 In this study, we evaluated the symptoms related to RE using the GerdQ questionnaire. Surprisingly, over 20% of the patients with subtotal gastrectomy suffered from significant reflux symptoms, while only 12.3% of the patients with total gastrectomy suffered from GERD symptoms. Although the ratios of patients with GERD symptoms were not statistically significant between subtotal gastrectomy patients and total gastrectomy patients, GERD may develop at a similar rate or more frequently after subtotal gastrectomy than after total gastrectomy. To our knowledge, this appears to be the first report of such a finding. The causes of GERD after subtotal gastrectomy include a change in lower esophageal sphincter pressure, development of hiatal hernia, and blunting of the angle of His caused by pericardial lymph node dissection.37,38,39,40 However, the published literature on GERD patients after subtotal gastrectomy is not sufficient to clarify the pathogenesis of post-operative GERD, as researchers have been less concerned with GERD after subtotal gastrectomy than after total gastrectomy. However, the incidence of GERD after subtotal gastrectomy is not negligible, but rather similar or higher than that after total gastrectomy. A previous report found that heartburn symptoms were a complaint in 16 of 61 (26.2%) patients who underwent partial gastrectomy, which is consistent with the findings in our study.41
Healthy individuals have anatomical features at the esophagogastric junction preventing esophageal reflux, which might be disrupted by gastric surgery. As described above, symptomatic GERD in the general population is closely associated with QoL.3,4 The prevalence and severity of reflux-related symptoms differ according to the extent of resection and/or reconstruction methods. Some studies evaluated the reflux itself, assessed by scintigraphic methods, bilimetry, intra-esophageal pH monitoring, or the endoscopic changes of the esophageal mucosa.8,9,10 However, these studies did not evaluate the impact of reflux-related symptoms on QoL after gastrectomy. The present study evaluated the impact of reflux-related symptoms on QoL after gastrectomy in gastric cancer patients. Furthermore, we used the concept of MID to interpret the data. Many studies on the QoL in gastrectomized patients with gastric cancer reported that the statistically significant differences were clinically relevant. However, the statistical significance of small differences does not necessarily imply clinical importance. The MID proposes a threshold above which the outcome is experienced as clinically relevant by the patients.25,26 Reflux-related symptoms were significantly correlated with the global health status/QoL scales. Interestingly, diarrhea in EORTC QLQ-C30 symptom scales was clinically relevant in association with reflux-related symptoms. Future studies need to investigate the correlation between diarrhea and reflux-related symptoms after gastrectomy, as we were unable to provide an explanation based on our study findings. In this study, we also demonstrated that reflux was clinically relevant to eating problems and body image, which are considered important factors by gastrectomized patients. Furthermore, the correlation analysis between the GerdQ score and global health status/QoL scales showed that the GerdQ score is useful in the determination of QoL. Initially, subjects with no positive or negative reflux symptoms have a GerdQ score of 6, which increases if the subject has reflux symptoms. On the other hand, the GerdQ score decreases if the subject has negative reflux-related symptoms. Therefore, a GerdQ score of <6 indicates the presence of negative reflux-related symptoms that could affect patients' QoL. For this reason, we analyzed the correlations again in a subpopulation with GerdQ scores of >6. As expected, a considerably higher correlation was observed between the GerdQ score and global health status/QoL scales (Fig. 4).
This study has some limitations. Esophageal reflux after total or subtotal gastrectomy could be different from GERD experienced in the general population, because the refluxate after gastrectomy has low or no acidity and patients do not have a pylorus. Therefore, the accuracy of the GerdQ score describing reflux symptoms in gastrectomized patients remains undetermined. In addition, the Korean version of the GerdQ questionnaire used in this study has not been officially validated. However, the GerdQ questionnaire covers all significant esophageal reflux related symptoms and there might be no other symptoms related to esophageal reflux in gastrectomized patients. Furthermore, the Korean version of the GerdQ questionnaire was successfully used in evaluation of GERD patients in a previous report.11
Although the refluxate after total gastrectomy is alkaline, its acidity is variable after subtotal gastrectomy. Truncal vagotomy reduces acid secretion of the remnant stomach in the early periods of gastrectomy, but it is restored with time.42 Patients with decreased esophageal sphincter function after subtotal gastrectomy eventually suffer from mixed acid and bile reflux. As the present study did not evaluate the composition of the refluxates, we did not confirm whether the acidity is correlated with the degree of the symptoms. Furthermore, the reconstruction methods after gastrectomy are important factors associated with reflux. A previous report suggested the use of semifundoplication for prevention of GERD after subtotal gastrectomy.43 Additionally, a limited number of studies have demonstrated that Roux-en Y gastrojejunostomy is superior to Billroth I or Billroth II anastomosis for prevention of GERD after subtotal gastrectomy.5,44 In this study, we did not analyze the effects of the reconstruction methods owing to subgroup discrepancies.
RE has been considered as a typical aftereffect following total gastrectomy. However, esophageal reflux symptoms may develop at a similar frequency or more frequently after subtotal gastrectomy than after total gastrectomy. Esophageal reflux symptoms significantly decrease the QoL of gastric cancer patients. Therefore, strategies are required to prevent or reduce esophageal reflux symptoms in subtotal gastrectomy.
Figures and Tables
Fig. 1
Functional scales and global health status/quality of life (QoL) of the European Organization for Research and Treatment QLQ-C30. P-values were calculated by t-test. GerdQ (+) = GerdQ score ≥8; GerdQ (-) = GerdQ score <8; PF = physical function; RF = role function; EF = emotional function; CF = cognitive function; SF = social function; GQ = global QoL; DoM = difference of means; MID = minimal important difference. *Mark represents the domain with a difference greater than or equal to the MID. MIDs were from the article and the MID in the domain of the emotional function could not be determined from the article [25].

Fig. 2
Symptom scales of the European Organization for Research and Treatment QLQ-C30. P-values were calculated by t-test. GerdQ (+) = GerdQ score ≥8; GerdQ (-) = GerdQ score <8; FA = fatigue; NV = nausea & vomiting; PA = pain; DN = dyspnea; IN = insomnia; AL = appetite loss; CO = constipation; DI = diarrhea; FD = financial difficulties; DoM = difference of means; MID = minimal important difference. *Mark represents the domain with a difference greater than or equal to the MID. MIDs were from the article [25].

Fig. 3
Symptom scales of the European Organization for Research and Treatment QLQ-STO22. P-values were calculated by t-test. GerdQ (+) = GerdQ score ≥8; GerdQ (-) = GerdQ score <8; DP = dysphagia; PA = pain; RE = reflux; ER = eating restriction; AN = anxiety; DM = dry mouth; TA = taste; BI = body image; HL = hair loss. *Mark represents the domains with differences greater than or equal to the minimal important difference.

Fig. 4
Correlation analysis between the GerdQ score and Global health status/quality of life (QoL) scale. The solid line is the regression analysis line among all patients (r=-0.170, P=0.002). The dotted line is the regression line of the subgroup analysis in patients with a GerdQ score >6 (r=-0.305, P<0.001).

Acknowledgments
These study findings were presented at the 10th International Gastric Cancer Congress, Verona, Italy, 2013.
References
1. Guggenheim DE, Shah MA. Gastric cancer epidemiology and risk factors. J Surg Oncol. 2013; 107:230–236.

2. Conroy T, Marchal F, Blazeby JM. Quality of life in patients with oesophageal and gastric cancer: an overview. Oncology. 2006; 70:391–402.

3. Gisbert JP, Cooper A, Karagiannis D, Hatlebakk J, Agréus L, Jablonowski H, et al. Impact of gastroesophageal reflux disease on patients' daily lives: a European observational study in the primary care setting. Health Qual Life Outcomes. 2009; 7:60.

4. Toghanian S, Wahlqvist P, Johnson DA, Bolge SC, Liljas B. The burden of disrupting gastro-oesophageal reflux disease: a database study in US and European cohorts. Clin Drug Investig. 2010; 30:167–178.
5. Inokuchi M, Kojima K, Yamada H, Kato K, Hayashi M, Motoyama K, et al. Long-term outcomes of Roux-en-Y and Billroth-I reconstruction after laparoscopic distal gastrectomy. Gastric Cancer. 2013; 16:67–73.

6. Nunobe S, Okaro A, Sasako M, Saka M, Fukagawa T, Katai H, et al. Billroth 1 versus Roux-en-Y reconstructions: a quality-of-life survey at 5 years. Int J Clin Oncol. 2007; 12:433–439.

7. Lee MS, Ahn SH, Lee JH, Park do J, Lee HJ, Kim HH, et al. What is the best reconstruction method after distal gastrectomy for gastric cancer? Surg Endosc. 2012; 26:1539–1547.

8. Matei D, Dadu R, Prundus R, Danci I, Ciobanu L, Mocan T, et al. Alkaline reflux esophagitis in patients with total gastrectomy and Roux en Y esojejunostomy. J Gastrointestin Liver Dis. 2010; 19:247–252.
9. Kim JW, Yoon H, Kong SH, Kim JS, Paeng JC, Lee HJ, et al. Analysis of esophageal reflux after proximal gastrectomy measured by wireless ambulatory 24-hr esophageal pH monitoring and TC-99m diisopropyliminodiacetic acid (DISIDA) scan. J Surg Oncol. 2010; 101:626–633.

10. Enjoji M, Yamada H, Kojima K, Inokuchi M, Kato K, Kawano T, et al. Scoring system for evaluating functional disorders following laparoscopy-assisted distal gastrectomy. J Surg Res. 2010; 164:e229–e233.

11. Kim JH, Park H, Lee YC. MIGHT study group. Is minimal change esophagitis really part of the spectrum of endoscopic findings of gastroesophageal reflux disease? A prospective, multicenter study. Endoscopy. 2011; 43:190–195.

12. Shaw MJ, Talley NJ, Beebe TJ, Rockwood T, Carlsson R, Adlis S, et al. Initial validation of a diagnostic questionnaire for gastroesophageal reflux disease. Am J Gastroenterol. 2001; 96:52–57.

13. Jones R, Coyne K, Wiklund I. The gastro-oesophageal reflux disease impact scale: a patient management tool for primary care. Aliment Pharmacol Ther. 2007; 25:1451–1459.

14. Revicki DA, Wood M, Wiklund I, Crawley J. Reliability and validity of the Gastrointestinal Symptom Rating Scale in patients with gastroesophageal reflux disease. Qual Life Res. 1998; 7:75–83.
15. Jones R, Junghard O, Dent J, Vakil N, Halling K, Wernersson B, et al. Development of the GerdQ, a tool for the diagnosis and management of gastro-oesophageal reflux disease in primary care. Aliment Pharmacol Ther. 2009; 30:1030–1038.

16. Ponce J, Garrigues V, Agréus L, Tabaglio E, Gschwantler M, Guallar E, et al. Structured management strategy based on the Gastro-oesophageal Reflux Disease (GERD) Questionnaire (GerdQ) vs. usual primary care for GERD: pooled analysis of five cluster-randomised European studies. Int J Clin Pract. 2012; 66:897–905.

17. Dent J, Vakil N, Jones R, Bytzer P, Schöning U, Halling K, et al. Accuracy of the diagnosis of GORD by questionnaire, physicians and a trial of proton pump inhibitor treatment: the Diamond Study. Gut. 2010; 59:714–721.

18. Huang CC, Lien HH, Sung YC, Liu HT, Chie WC. Quality of life of patients with gastric cancer in Taiwan: validation and clinical application of the Taiwan Chinese version of the EORTC QLQ-C30 and EORTC QLQ-STO22. Psychooncology. 2007; 16:945–949.

19. Shaw M, Dent J, Beebe T, Junghard O, Wiklund I, Lind T, et al. The Reflux Disease Questionnaire: a measure for assessment of treatment response in clinical trials. Health Qual Life Outcomes. 2008; 6:31.

20. Blazeby JM, Conroy T, Bottomley A, Vickery C, Arraras J, Sezer O, et al. European Organisation for Research and Treatment of Cancer Gastrointestinal and Quality of Life Groups. Clinical and psychometric validation of a questionnaire module, the EORTC QLQ-STO 22, to assess quality of life in patients with gastric cancer. Eur J Cancer. 2004; 40:2260–2268.

21. Blazeby JM, Currie E, Zee BC, Chie WC, Poon RT, Garden OJ. EORTC Quality of Life Group. Development of a questionnaire module to supplement the EORTC QLQ-C30 to assess quality of life in patients with hepatocellular carcinoma, the EORTC QLQ-HCC18. Eur J Cancer. 2004; 40:2439–2444.

22. Yun YH, Park YS, Lee ES, Bang SM, Heo DS, Park SY, et al. Validation of the Korean version of the EORTC QLQ-C30. Qual Life Res. 2004; 13:863–868.

23. Kong H, Kwon OK, Yu W. Changes of quality of life after gastric cancer surgery. J Gastric Cancer. 2012; 12:194–200.

24. Fayer PM, Aaronson NK, Bjordal K, Groenvold M, Curran D, Bottomley A, et al. EORTC QLQ-C30 scoring manual. 3rd ed. Brussels: European Organisation for Research and Treatment of Cancer;2001.
25. Cocks K, King MT, Velikova G, Martyn St-James M, Fayers PM, Brown JM. Evidence-based guidelines for determination of sample size and interpretation of the European Organisation for the Research and Treatment of Cancer Quality of Life Questionnaire Core 30. J Clin Oncol. 2011; 29:89–96.

26. King MT. A point of minimal important difference (MID): a critique of terminology and methods. Expert Rev Pharmacoecon Outcomes Res. 2011; 11:171–184.

27. Cohen J. Statistical power analysis for the behavioral sciences. New York: Academic Press;1977.
28. Copay AG, Subach BR, Glassman SD, Polly DW Jr, Schuler TC. Understanding the minimum clinically important difference: a review of concepts and methods. Spine J. 2007; 7:541–546.

29. Dent J, El-Serag HB, Wallander MA, Johansson S. Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2005; 54:710–717.

31. Lehnert T, Buhl K. Techniques of reconstruction after total gastrectomy for cancer. Br J Surg. 2004; 91:528–539.

32. Katsoulis IE, Robotis JF, Kouraklis G, Yannopoulos PA. What is the difference between proximal and total gastrectomy regarding postoperative bile reflux into the oesophagus? Dig Surg. 2006; 23:325–330.

33. Hsu CP, Chen CY, Hsieh YH, Hsia JY, Shai SE, Kao CH. Esophageal reflux after total or proximal gastrectomy in patients with adenocarcinoma of the gastric cardia. Am J Gastroenterol. 1997; 92:1347–1350.
34. Tokunaga M, Hiki N, Ohyama S, Nunobe S, Miki A, Fukunaga T, et al. Effects of reconstruction methods on a patient's quality of life after a proximal gastrectomy: subjective symptoms evaluation using questionnaire survey. Langenbecks Arch Surg. 2009; 394:637–641.

35. Ichikawa D, Komatsu S, Okamoto K, Shiozaki A, Fujiwara H, Otsuji E. Evaluation of symptoms related to reflux esophagitis in patients with esophagogastrostomy after proximal gastrectomy. Langenbecks Arch Surg. 2013; 398:697–701.

36. Johnson DA, Fennerty MB. Heartburn severity underestimates erosive esophagitis severity in elderly patients with gastroesophageal reflux disease. Gastroenterology. 2004; 126:660–664.

37. Iida F, Ishizaka K, Sugenoya A. Lower esophageal sphincter pressure after subtotal gastrectomy and postoperative reflux esophagitis. Hepatogastroenterology. 1994; 41:581–584.
38. Fujiwara Y, Nakao K, Inoue T, Koishi K, Nishio Y, Yagyu R, et al. Clinical significance of hiatal hernia in the development of gastroesophageal reflux after distal gastrectomy for cancer of the stomach. J Gastroenterol Hepatol. 2006; 21:1103–1107.

39. Crookes PF. Gastroesophageal reflux after partial gastrectomy. Am J Gastroenterol. 1998; 93:3–4.

40. Fujiwara Y, Nakagawa K, Kusunoki M, Tanaka T, Yamamura T, Utsunomiya J. Gastroesophageal reflux after distal gastrectomy: possible significance of the angle of His. Am J Gastroenterol. 1998; 93:11–15.

42. Gutschow C, Collard JM, Romagnoli R, Salizzoni M, Hölscher A. Denervated stomach as an esophageal substitute recovers intraluminal acidity with time. Ann Surg. 2001; 233:509–514.

43. Shibata Y. Effect of semifundoplication with subtotal gastrectomy for prevention of postoperative gastroesophageal reflux. J Am Coll Surg. 2004; 198:212–217.

44. Montesani C, D'Amato A, Santella S, Pronio A, Giovannini C, Cristaldi M, et al. Billroth I versus Billroth II versus Roux-en-Y after subtotal gastrectomy. Prospective [correction of prespective] randomized study. Hepatogastroenterology. 2002; 49:1469–1473.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download