Introduction
Intussusception is a rare cause of postoperative intestinal obstruction in adults.1 Various kinds of symptoms have been expressed such as epigastric pain, nausea/vomiting, and hematemesis. Intussusception can be diagnosed by performing upper gastrointestinal series, endoscopy, ultrasonography, or a computed tomography scan.2 We report our experience with a patient who developed early postoperative retrograde jejunojejunal intussusception after total gastrectomy.
Case Report
A 77-year-old woman visited Chonbuk National University Hospital because of gastric adenocarcinoma detected at a periodic examination. She had no history of abdominal surgery. Radical total gastrectomy with Roux-en-Y esophagojejunostomy was performed. After radical total gastrectomy, the jejunum was resected 20 cm below from the Treitz ligament. Distal part of resected jejunum was pulled up through the transverse mesocolon, and esophagojejunostomy was constructed in end-to-side anastomosis by using an EEA stapler (25 mm; Covidien, Mansfield, MA, USA). Fifty centimeters below the esophagojejunostomy site, a jejunojejunostomy was constructed by performing end-to-side hand-sewn anastomosis. A nasojejunal feeding tube (NJFT) was inserted into the distal part of the efferent loop of the jejunostomy for early postoperative enteral nutrition. A closed drain tube was placed at the esophagojejunostomy through the abdominal wall.
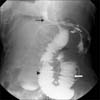
On the fifth postoperative day, the patient complained of abdominal pain, and bile-colored fluid was seen in the closed drain tube. A water-soluble contrast swallowing imaging study indicated leakage at the esophagojejunostomy site and dilatation of the Roux limb and the afferent loop of the jejunojejunostomy, which indicated intestinal obstruction (Fig. 1). Emergency surgery was performed.
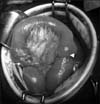
During surgery, retrograde jejunojejunal intussusception accompanied with NJFT was found at the efferent loop of the jejunojejunostomy. The intussusception was approximately 7 cm in length from the NJFT tip portion to the jejunojejunostomy and showed mild edematous changes without necrosis (Fig. 2). Manual reduction without bowel resection and primary repair of esophagojejunostomy was performed, and the NJFT was removed. Feeding Jejunostomy for enteral nutrition was constructed at the distal part of the efferent loop of the jejunojejunostomy. On the ninth repostoperativeday, a follow-up soluble contrast swallowing imaging study showed no leakage. She was discharged without complications on the 23rd re-postoperativeday.
Discussion
Intussusception after abdominal surgery is a comparatively rare disorder and occurs in only 0.07% to 2.1% of individuals who undergo gastrectomy.3 However, the majority of intussusceptions following abdominal surgery occur after gastrectomy; many are associated with the Billroth II method or Roux-en-Y anastomosis.4,5
In adults, the exact mechanism is unknown; however, postoperative intussusceptions are likely to be caused by altered peristalsis after prolonged and excessive manipulation with drying and bruising of the bowel, extensive preperitoneal dissection, abdominal serum electrolyte level, local hypoxia, anesthetic agents, and postoperatively administered drugs.6 In general, the majority of small intestinal intussusceptions are caused by benign lesions such as benign neoplasm, inflammatory lesion, Meckel's diverticuli, appendix, adhesion, intestinal tubes, whereas the majority of large intestinal intussusception have a malignant etiology.7 In general, retrograde intussusceptions arise late in the postoperative period, whereas the antegrade cases occur during the early period following gastrectomy.8
The first case of retrograde jejunojejunal intussusception after total gastrectomy was reported in 1954.9 Yoneda et al.3 analyzed 20 cases of retrograde jejunojejunal intussusception after total gastrectomy. There were only 3 cases that occurred in the early postoperative period (i.e., within 30 days postoperatively), whereas 17 cases occurred variously from 1 year to 21 years later. All cases except one underwent surgical treatment (6 cases with manual reduction and the other cases with enterectomy).
In our case, intestinal obstruction occurred because of retrograde jejunojejunal intussusception after total gastrectomy in the early postoperative period. This led to increased intraluminal pressure and resulted in esophagojejunostomy leakage.
The use of long cantor tubes caused both antegrade and retrograde small bowel intussusceptions in adults. Antegrade intussusception in this situation occurs through telescoping of the bowel over the tube, especially when it is fixed in place with tape at the nose. Retrograde intussusception occurs during or after the tube is removed, especially if it is removed quickly and with force.10
However, our patient did not eliminate the NJFT, and we could not find any palpable mass in the small bowel. Additionally, the postoperative adhesion was not severe because reoperation was performed in the early postoperative period. Therefore, we suggest that the NJFT acts as a trigger for intussusception. The tip of the NJFT irritates the jejunal lumen, so it alters normal peristaltic activity and causes an invagination of the distal jejunum.10 However, the etiology and mechanism remain unclear.
Retrograde jejunojejunal intussusception after total gastrectomy commonly occurs with Roux-en-Y anastomosis and Braun's anastomosis. Jejunojejunal intussusception needs immediate operative management. A delayed diagnosis may lead to an unsatisfactory result. In our case, it progressed to dilatation of the distal portion of esophagojejunostomy and leakage of the esophagojejunostomy site. No definite symptoms indicate intussusception. Therefore, early detection should be required.
We experienced rare early postoperative retrograde jejunojejunal intussusceptions after total gastrectomy with esophagojejunostomy and report our results with a brief review of the literature.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download