Abstract
Purpose
The purpose of this study was to provide basic data about agitation in patients with dementia by surveying the literature.
Method
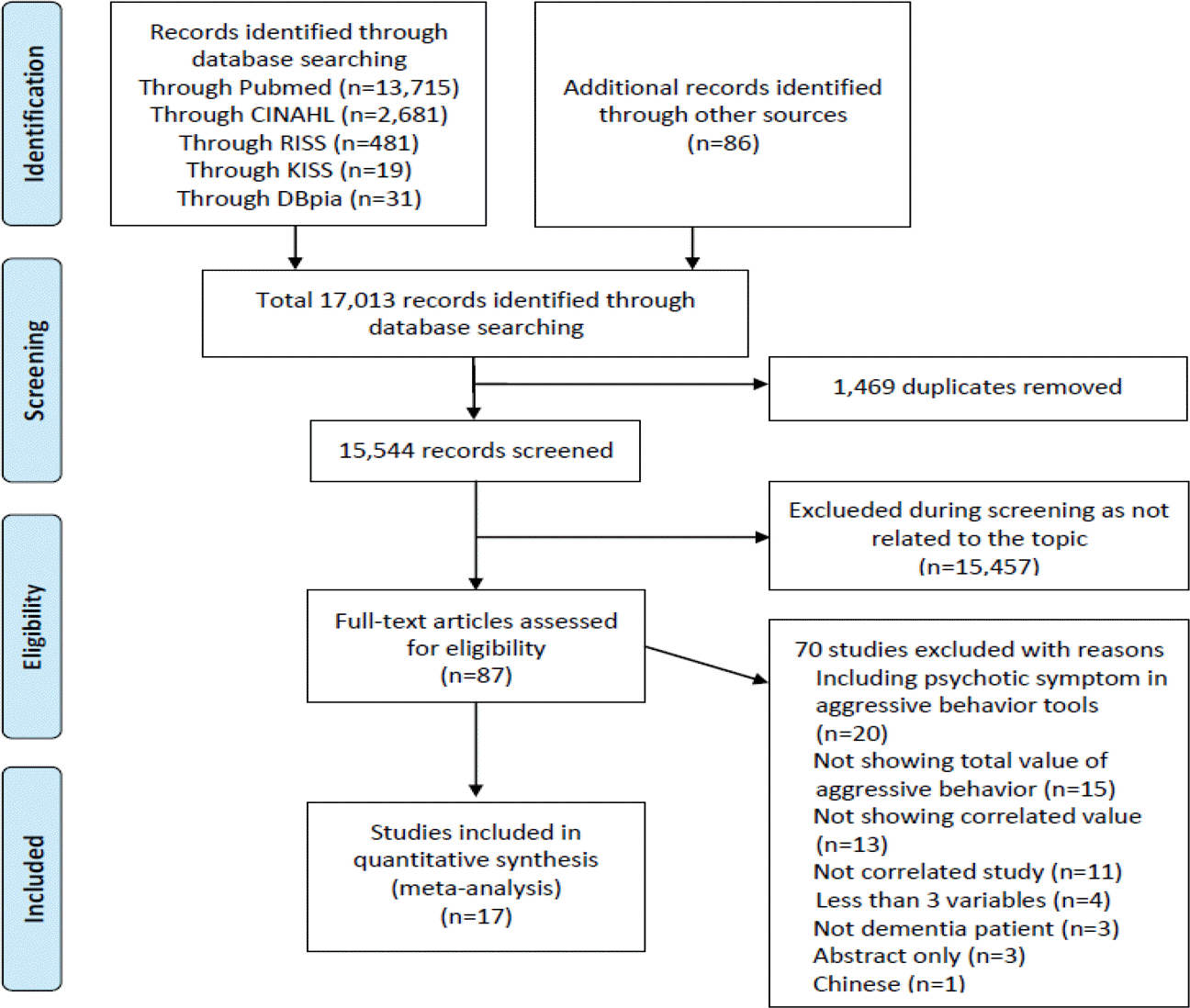
Key words used for search through hand-search and electronic database (CINHAL, Pubmed, Google scholar, Riss, Kiss, DBpia) included 'dementia', 'Alzheimer disease', ‘agitation’, ‘aggression or aggressive behavior’, ‘problem or disruptive behavior’, and ‘abnormal behavior.’ Seventeen studies met the inclusion criteria for the Meta-analysis and ‘R’ version 3.2.2 was used to analyze the correlated effect size.
Results
Study results showed that variables related to agitation were identified as the demographic (age, gender), dementia-related (cognition, medication uses), physical (Activity of Daily Living [ADL], pain), psychological (depression, psychotic symptom, caregiver burden) and environmental (psychosocial environment) factors. The effect size between the correlated variables and agitation were low to moderate (caregiver burden .36; ADL -.24; psychotic symptom and depression .21; pain .19; cognition -.15; medication uses .12; and psychosocial environment -.12).
REFERENCES
1.Korea Ministry of Health & Welfare. 3rd National dementia management plan [Internet]. Seoul: Korea Ministry of Health & Welfare;2015. [cited 2016 January 19]. Available from:. http://www.mohw.go.kr/front_new/al/sal0301vw.jsp?PAR_MENU_ID=04&MENU_ID=0403&page=7&CONT_SEQ=329062.
2.Oh BH. Diagnosis and treatment for behavioral and psychological symptoms of dementia. Journal of the Korean Medical Association. 2009. 52(11):1048–54.

3.Cohen-Mansfield J., Billig N. Agitated behaviors in the elderly: I. a conceptual review. Journal of the American Geriatrics Society. 1986. 34(10):711–21. http://dx.doi.org/10.1111/j.1532-5415.1986.tb04302.x.

4.Cerejeira J., Lagarto L., Mukaetova-Ladinska EB. Behavioral and psychological symptoms of dementia. Frontiers in Neurology. 2012. 3(73):1–21. http://dx.doi.org/10.3389/fneur.2012.00073.

5.Kunik ME., Snow AL., Davila JA., McNeese T., Steele AB., Bala-subramanyam V, et al. Consequences of aggressive behavior in patients with dementia. The Journal of Neuropsychiatry and Clinical Neurosciences. 2010. 22(1):40–7. http://dx.doi.org/10.1176/jnp.2010.22.1.40.

6.Brodaty H., Draper B., Low LF. Nursing home staff attitudes towards residents with dementia: strain and satisfaction with work. Journal of Advanced Nursing. 2003. 44(6):583–90. http://dx.doi.org/10.1046/j.0309-2402.2003.02848.x.

7.Pitkala KH., Laurila JV., Strandberg TE., Tilvis RS. Behavioral symptoms and the administration of psychotropic drugs to aged patients with dementia in nursing homes and in acute geriatric wards. International Psychogeriatrics. 2004. 16(01):61–74. http://dx.doi.org/10.1017/s1041610204000079.

8.Gitlin LN., Kales HC., Lyketsos CG. Nonpharmacologic management of behavioral symptoms in dementia. The Journal of the American Medical Association. 2012. 308(19):2020–9. http://dx.doi.org/10.1001/jama.2012.36918.

9.Cohen-Mansfield J., Marx MS., Lipson S., Werner P. Predictors of mortality in nursing home residents. Journal of Clinical Epidemiology. 1999. 52(4):273–80. http://dx.doi.org/10.1016/s0895-4356(98)00156-5.

10.Algase DL., Beck C., Kolanowski A., Whall A., Berent S., Richards K, et al. Need-driven dementia-compromised behavior: an alternative view of disruptive behavior. American Journal of Alzheimer's Disease and Other Dementias. 1996. 11(6):10–9. http://dx.doi.org/10.1177/153331759601100603.

11.Zuidema SU., de Jonghe JF., Verhey FR., Koopmans RT. Predictors of neuropsychiatric symptoms in nursing home patients: influence of gender and dementia severity. International Journal of Geriatric Psychiatry. 2009. 24(10):1079–86. http://dx.doi.org/10.1002/gps.2225.

12.Estabrooks CA., Floyd JA., Scott Findlay S., O'Leary KA., Gushta M. Individual determinants of research utilization: a systematic review. Journal of advanced nursing. 2003. 43(5):506–20. http://dx.doi.org/10.1046/j.1365-2648.2003.02748.x.

13.Cicolini G., Comparcini D., Simonetti V. Workplace empowerment and nurses' job satisfaction: a systematic literature review. Journal of Nursing Management. 2014. 22(7):855–71. http://dx.doi.org/10.1111/jonm.12028.

14.Giovannucci E. Meta-analysis of coffee consumption and risk of colorectal cancer. American Journal of Epidemiology. 1998. 147(11):1043–52. http://dx.doi.org/10.1093/oxfordjournals.aje.a009398.

15.Higgins J., Green S. Cochrane handbook for systematic reviews of interventions version 5.1.0 [Internet]. London, UK. The Cochrane Collaboration;2011. [cited 2015 October 15]. Available from:. http://handbook.cochrane.org/.
16.Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed.Hillsdale, NJ: Lawrence Erlbaum Associates;1988.
17.Salzman C., Jeste D., Meyer RE., Cohen-Mansfield J., Cummings J., Grossberg G, et al. Elderly patients with dementia-related symptoms of severe agitation and aggression: consensus statement on treatment options, clinical trials methodology, and policy. The Journal of Clinical Psychiatry. 2008. 69(6):889–98. http://dx.doi.org/10.4088/jcp.v69n0602.
18.Jung JH. Stress and psychological status between the demented and the nondemented elderly person's caregivers. Journal of Special Education & Rehabilitation Science. 2013. 52(4):51–65.
19.Sink KM., Covinsky KE., Barnes DE., Newcomer RJ., Yaffe K. Caregiver characteristics are associated with neuropsychiatric symptoms of dementia. Journal of the American Geriatrics Society. 2006. 54(5):796–803. http://dx.doi.org/10.1111/j.1532-5415.2006.00697.x.

20.Lee HJ., Lee OS., Jung SH., Park MS., Lim SC. Evaluation of pharmacotherapy for the patients with depression in alzheimer's disease, parkinson's disease or vascular dementia. Korean Journal of Clinical Pharmacy. 2013. 23(1):33–41.
21.Korea Institute for Health and Social Affairs. 2014 A survey of the elderly [Internet]. Seoul: Korea Institute for Health and Social Affairs;2014. [cited 2016 January 20]. Available from:. http://www.mohw.go.kr/front_new/jb/sjb030301vw.jsp?PAR_MENU_ID=03&MENU_ID=0328&CONT_SEQ=318518&page=1.
22.Enache D., Winblad B., Aarsland D. Depression in dementia: epidemiology, mechanisms, and treatment. Current Opinion in Psychiatry. 2011. 24(6):461–72. http://dx.doi.org/10.1097/yco.0b013e32834bb9d4.
Figure 2.
Forest plots of the effects size of variables related to agitation in patients with dementia.
Table 1.
Characteristics of Studies Included in Meta-Analysis
ADL=activity of daily living; BPC=behavioral problems checklist; DBS=disruptive behavior scale; CMAI=cohen-mansfield agitation inventory; RMBPC=revised memory and behavior problem checklist; BEHAVE-AD=behavioral pathology in Alzheimer's disease scale; NPI=neuropsychiatric inventory; PGDRS=psychogeriatric dependency rating scale; BSRS=behavior symptom rating scale; NPI-NH=neuropsychiatric inventory nursing home version; MDS=minimum data set.
Table 2.
Subgroup Analysis of Moderator Variables in Cognition
| Variables | Categories | k | ES | -95% CI | +95% CI | I2 (%) | Qb (p) | R2 (%) |
|---|---|---|---|---|---|---|---|---|
| Setting | Community & outpatient clinic | 7 | -.17 | -.22 | -.11 | 0.0 | 0.07 | |
| Nursing home & long-term facility | 8 | -.15 | -.24 | -.07 | 61.4 | (.789) | ||
| Severity of dementia | Below & moderate | 8 | -.14 | -.20 | -.09 | 5.4 | 0.19 | |
| Severe | 7 | -.16 | -.25 | -.07 | 68.6 | (.662) | ||
| Cognition measurement | Type of score | 13 | -.17 | -.22 | -.12 | 18.3 | 11.10 | 80.7 |
| Type of grade | 2 | -.05 | -.10 | -.01 | 0.0 | (<.001) | ||
| Agitation measurement | CMAI | 6 | -.20 | -.25 | -.14 | 0.0 | 2.39 | |
| Others | 9 | -.13 | -.19 | -.06 | 52.6 | (.122) |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download