Abstract
Objectives
Nodular fasciitis is a non-neoplastic soft-tissue lesion located in the deep subcutaneous region; it may be misdiagnosed as a malignant tumor due to its rapid growth and microscopic characteristics. We introduce an unusual case of nodular fasciitis which presented as a posterior neck mass.
Summary of Literature Review
Nodular fasciitis is an unusual benign lesion. Becaue it sometimes shows aggressive microscopic characteristics, (being hypercellular and polymorphic), the condition has the potential to be misdiagnosed as sarcoma.
Materials and Methods
A 20-year-old woman presented with a 1-month history of a progressively enlarging mass on her posterior neck. Computed tomography (CT) scans of the neck showed a markedly enhanced, well-defined, ovoid soft tissue mass at the posterior of the spinous process of C2. The patient underwent marginal excision. There was a 2 cm, well–capsulated, pinkish-gray mass.
Results
She recovered without any complications. Histopathologic examination showed a spindle cell proliferation, increased cellularity, and nuclear atypia with mitosis. The immunohistochemistry stain showed negative findings. The mass was diagnosed as nodular fasciitis.
Conclusions
A diagnosis of nodular fasciitis, not just malignant tumor, should be considered for a rapidly growing posterior neck mass showing aggressive microscopic appearance, Nodular fasciitis is a self-limiting lesion readily treated by marginal excision. However, followups should be increased to watch for recurrence.
REFERENCES
1. Shin J, Lee H, Cho K-J, et al. Nodular fasciitis of the head and neck: radiographic findings. Clin Imaging. 2003; 27:31–7.
2. Harrison HC, Motbey J, Kan AE, de Silva M. Nodular fasciitis of the nose in a child. Int J Pediatr Otorhinolaryngol. 1995; 33:257–64.

3. Powers CN, Berardo MD, Frable WJ. Fine-needle aspiration biopsy: pitfalls in the diagnosis of spindle-cell lesions. Diagn Cytopathol. 1994; 10:232–40.

4. Montgomery EA, Meis JM. Nodular fasciitis. Its morpho-logic spectrum and immunohistochemical profile. Am J Surg Pathol. 1991; 15:942–8.
6. Plaza J, Mayerson J, Wakely P. Nodular fasciitis of the hand: a potential diagnostic pitfall in fine-needle aspiration cytopathology. Am J Clin Pathol. 2005; 123:388–93.
7. Koenigsberg RA, Faro S, Chen X, Marlowe F. Nodular fasciitis as a vascular neck mass. AJNR, Am J Neuroradiol. 1996; 17:567–9.
8. Oshiro Y, Fukuda T, Tsuneyoshi M. Fibrosarcoma versus fibromatoses and cellular nodular fasciitis. A comparative study of their proliferative activity using proliferating cell nuclear antigen, DNA flow cytometry, and p53. Am J Surg Pathol. 1994; 18:712–9.
9. Kim S, Kim H-J, Park S-W, et al. Nodular fasciitis in the head and neck: CT and MR imaging findings. AJNR, Am J Neuroradiol. 2005; 26:2617–23.
10. Dahl I, Jarlstedt J. Nodular fasciitis in the head and neck. A clinicopathological study of 18 cases. Act otolaryngol. 1980; 90:152–9.

11. Batsakis JG, el Naggar AK. Pseudosarcomatous proliferative lesions of soft tissues. The Annals of otology, rhinology & laryngology. Ann Otol Rhinol Laryngol. 1994; 103:578–82.
12. DiNardo LJ, Wetmore RF, Potsic WP. Nodular fasciitis of the head and neck in children. A deceptive lesion. Arch Otolaryngol Head Neck Surg. 1991; 117:1001–2.

13. Wong N, Di F. Pseudosarcomatous fasciitis and myositis: diagnosis by fine-needle aspiration cytology. Am J Clin Pathol. 2009; 132:857–65.
Figures and Tables%
FigI 1.
(A) A CT scan of the soft tissuted tomography reveals a 1.2 cm sized oval shaped well-defed mass. (B) A CT scan of the soft tissuted tomography with enhancement reveals a strongly enhancing soft tissue mass between the superficial and deep muscle layers of the posteor neck. (C) A CT scan of the soft tissuted tomography with sagittal reconstruction shows that the mass is located posterior to the spinous procesof C2.
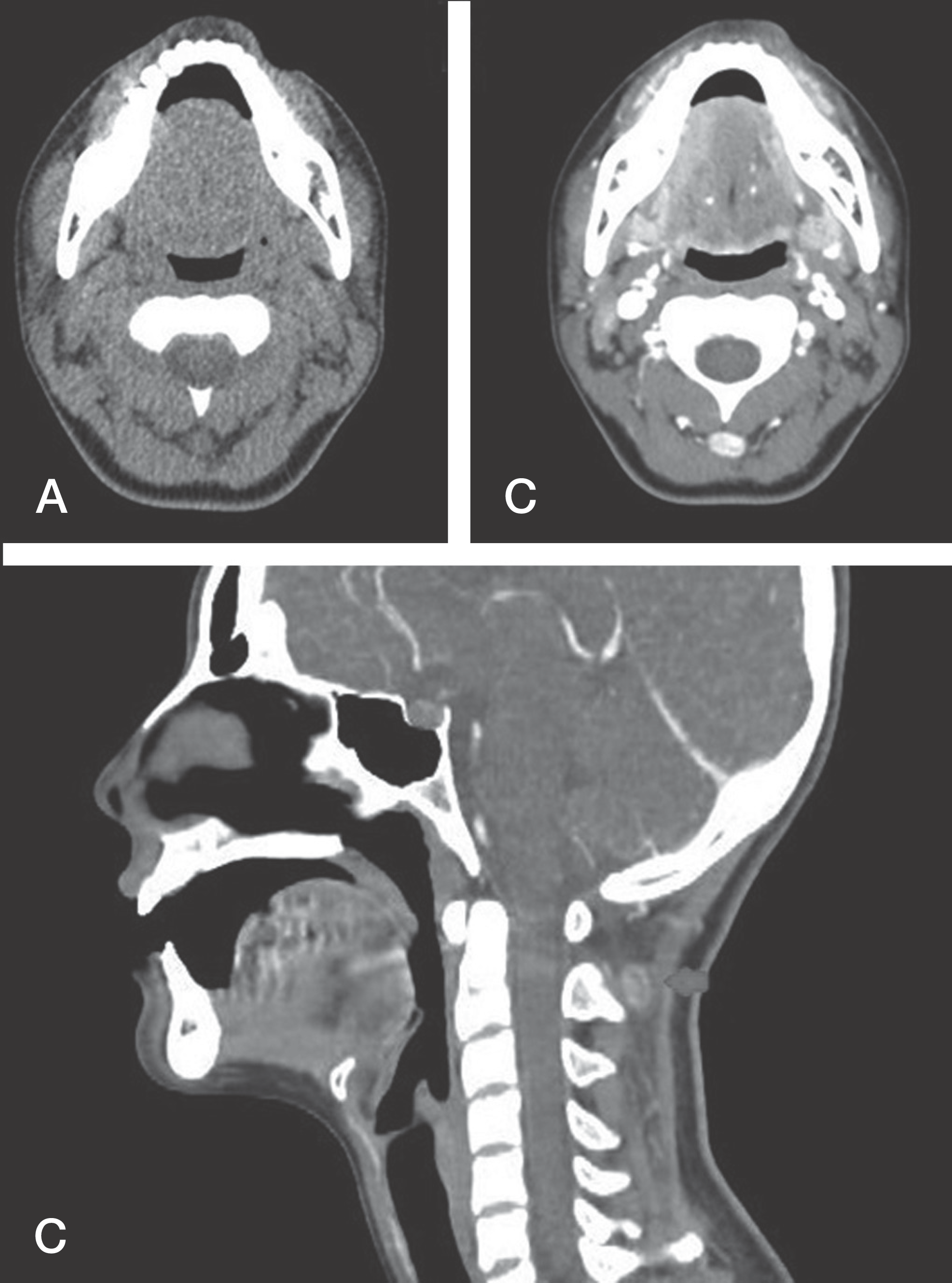
Fig 2.
A Llongitudinal section of nodular fasciitis (x1.25 magnifations). (B) Histopathologic findings under the hematoxylin-eosin stain. The lesion is composed of interlacing fascicles of plump spindle-shaped fibroblasts/myofibroblasts lacking nuclear pleomorphism. The prominentculatures, and intralesional extravasated erythrocytes, and mixed chronic inflammat cells werear seen (H& x200). (C) Mitoses were present in 6/10 high power fields but no atypicforms were are idenified (H&E, x400).

Table 1.
Pathologic Differences Between Nodular Fasciitis and Malignant Sarcomas




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download