Abstract
Objectives
To compare the efficacy of lidocaine and bupivacaine for the ultrasound-guided lumbar medial branch block in chronic low back pain.
Summary of Literature Review
There is no study for comparison of the efficacy between lidocaine and bupivacaine for the medial branch block.
Materials and Methods
From August 2011 to May 2013, 186 patients were assigned 0.5% lidocaine(n=136) or 0.25% bupivacaine(n=45) for the ultrasound-guided lumbar medial branch block. All procedures have been performed by the same operator, and 23G, 10 cm needle was placed and drug was injected under ultrasound guide. To target medial branches from lumbar spinal nerve, the groove at the root of transverse process and the base of superior articular process has been identified on transverse scan. Patients were evaluated by pre- and post-interventional(1 hour) Visual Analog Scale and analyzed statistically.
Results
Reduction of VAS score in bupivacaine group is significantly greater than that in lidocaine group and post-interventional VAS score in bupivacaine group is significantly lower than that in lidocaine group through analysis of covariance test with adjusted pre-interventional VAS score. In multivariate analysis, while age, sex and treatment level were not significant factors, pre-interventional VAS score and the kind of drug were significant factors. Severe pain before treatment and bupivacaine was indicator of better result. Bupivacaine group reduced pain score in the VAS 2.285 more than lidocaine group with adjustment with other factors.
REFERENCES
1. Uematsu S, Udvarhelyi GB, Benson DW, Siebens AA. Percutaneous radiofrequency rhizotomy. Surg Neurol. 1974; 2:319–25.
2. Shealy CN. Percutaneous radiofrequency denervation of spinal facets. Treatment for chronic back pain and sciatica. J Neurosurg. 1975; 43:448–51.
3. Moon SH, Lee S, Kim KH, Rho JH, Kim JH, Jung WS. Effect of ultrasound-guided lumbar medial branch block in chronic low back pain. J of Korean Orthopaedic Research Society. 2012; 15:54–61.
4. Cohen SP, Strassels SA, Kurihara C, et al. Randomized study assessing the accuracy of cervical facet joint nerve (medial branch) blocks using different injectate volumes. Anesthesiology. 2010; 112:144–52.

5. Thorburn J, Moir DD. Bupivacaine toxicity in association with extradural analgesia for caesarean section. Br J Anaesth. 1984; 56:551–3.

6. Gould DB, Aldrete JA. Bupivacaine cardiotoxicity in a patient with renal failure. Acta Anaesthesiol Scand. 1983; 27:18–21.
7. Buffington CW. The magnitude and duration of direct myocardial depression following intracoronary local anesthetics: a comparison of lidocaine and bupivacaine. Anesthesiology. 1989; 70:280–7.
8. Strichartz GR, Sanchez V, Arthur GR, Chafetz R, Martin D. Fundamental properties of local anesthetics. II. Mea-sured octanol: buffer partition coefficients and pKa values of clinically used drugs. Anesth Analg. 1990; 71:158–70.
9. Wildsmith JA, Brown DT, Paul D, Johnson S. Structure-activity relationships in differential nerve block at high and low frequency stimulation. Br J Anaesth. 1989; 63:444–52.

10. Scholz A. Mechanisms of (local) anaesthetics on voltage-gated sodium and other ion channels. Br J Anaesth. 2002; 89:52–61.

11. Ibusuki S, Katsuki H, Takasaki M. The effects of extracellular pH with and without bicarbonate on intracel-lular procaine concentrations and anesthetic effects in crayfish giant axons. Anesthesiology. 1998; 88:1549–57.

12. Cohen SP, Raja SN. Pathogenesis, diagnosis, and treatment of lumbar zygapophysial (facet) joint pain. Anesthesiology. 2007; 106:591–614.

13. Manchikanti L, Singh V, Falco FJ, et al. Evaluation of lumbar facet joint nerve blocks in managing chronic low back pain: a randomized, double-blind, controlled trial with a 2-year followup. Int J Med Sci. 2010; 7:124–35.

14. Alhelail M, Al-Salamah M, Al-Mulhim M, Al-Ha-mid S. Comparison of bupivaaine and lidocaine with epinephrine for digital nerve blocks. Emerg Med J. 2009; 26:347–50.
15. Chu CR, Izzo NJ, Papas NE, Fu FH. In vitro exposure to 0.5% bupivacaine is cytotoxic to bovine articular chon-drocytes. Arthroscopy. 2006; 22:693–9.

16. Gomoll AH, Yanke AB, Kang RW, et al. Longterm effects of bupivacaine on cartilage in a rabbit shoulder model. Am J Sports Med. 2009; 37:72–7.

17. Lehner C, Gehwolf R, Hirzinger C, et al. Bupivacaine induces short-term alterations and impairment in rat tendons. Am J Sports Med. 2013; 41:1411–8.

Figures and Tables%
Fig. 1.
The photograph shows sterile draping and preparation for ultra-sound-guided medial branch block.
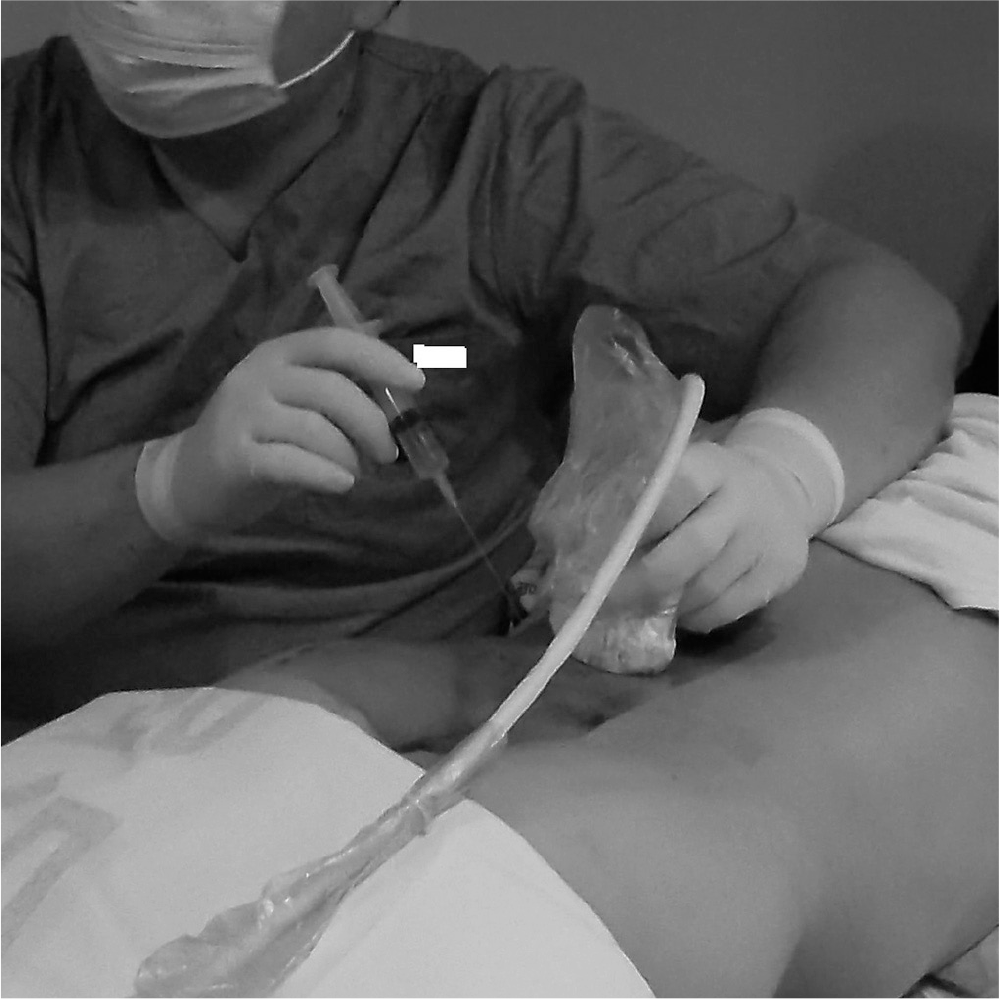
Fig. 2.
Ultrasonography on longitudinal scan at midline of lumbar area shows cephalad part of spinous process in sacrum as landmark from which other lumbar spinous processes can be counted upwards. S1; spinous process (median sacral crest) of sacrum, L5; spinous process of 5th lumbar vertebra, L4; spinous process of 4th lumbar vertebra.
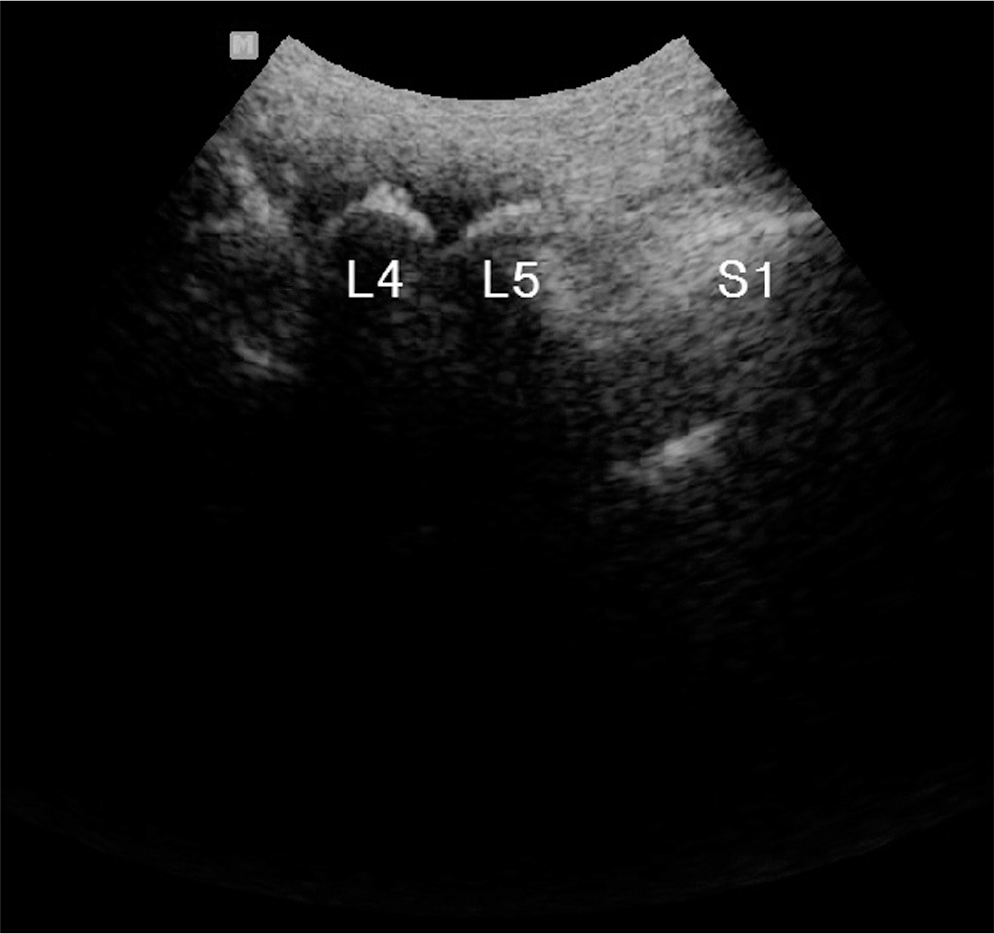
Fig. 3.
Target facet segment can be counted by longitudinal paravertebral sonogram corresponding with previously checked spinous process. L5S1; facet joint between sacrum and 5th lumbar vertebra, L45; facet joint between 4th and 5th lumbar vertebra, L34; facet joint between 3rd and 4th lumbar vertebra.
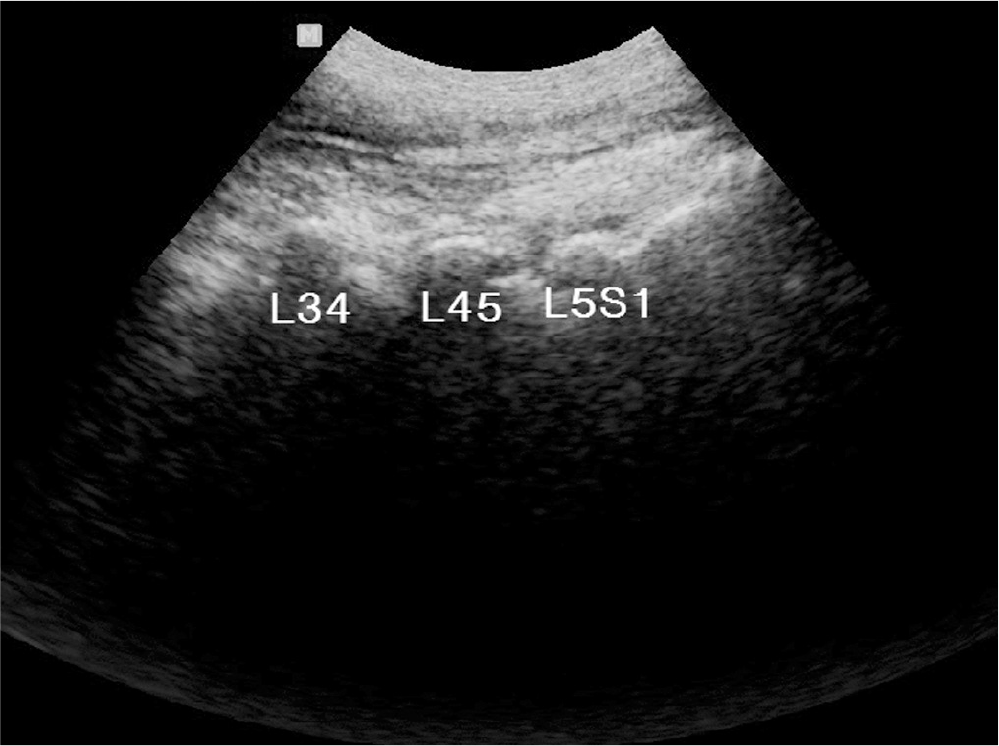
Fig. 5.
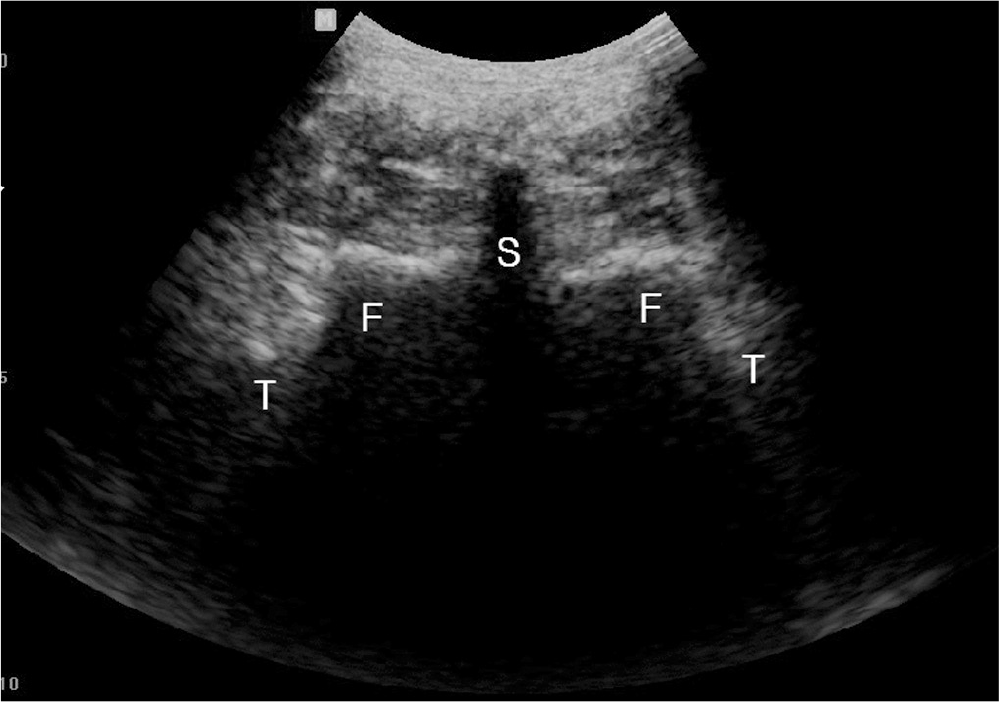
Move ultrasound probe laterally until transverse process and superior articular process can be located at center of image.
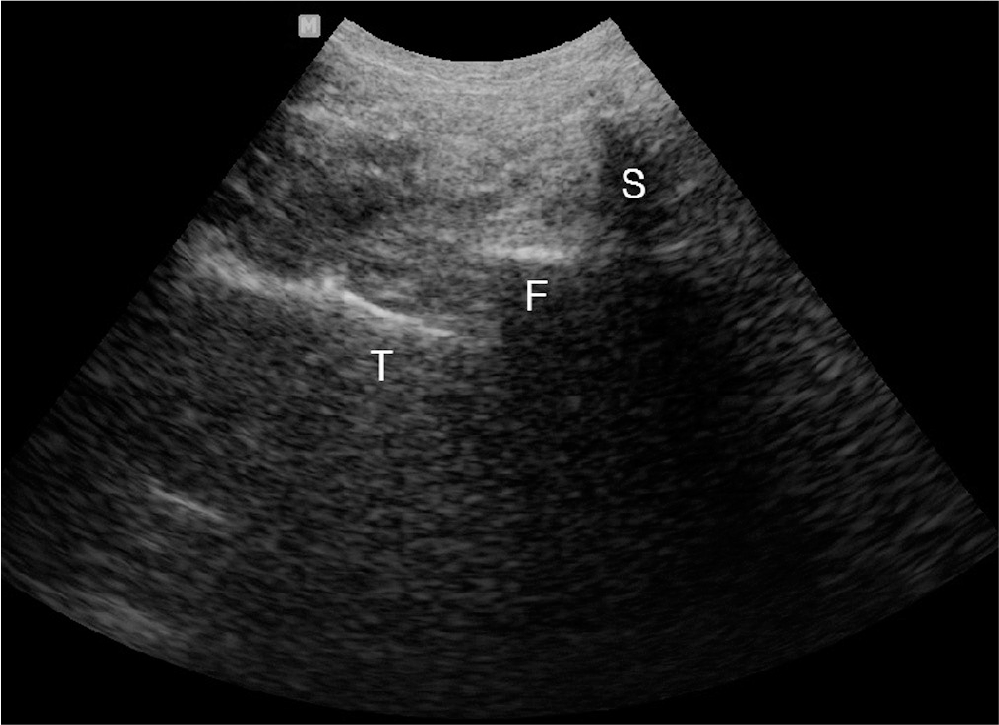
Fig. 6.
(A) Doppler scan shows multiple red spots which indicate vascularity around posterior muscular structure. (B) Imaginary pathway(white arrow) for needle avoiding vessles.
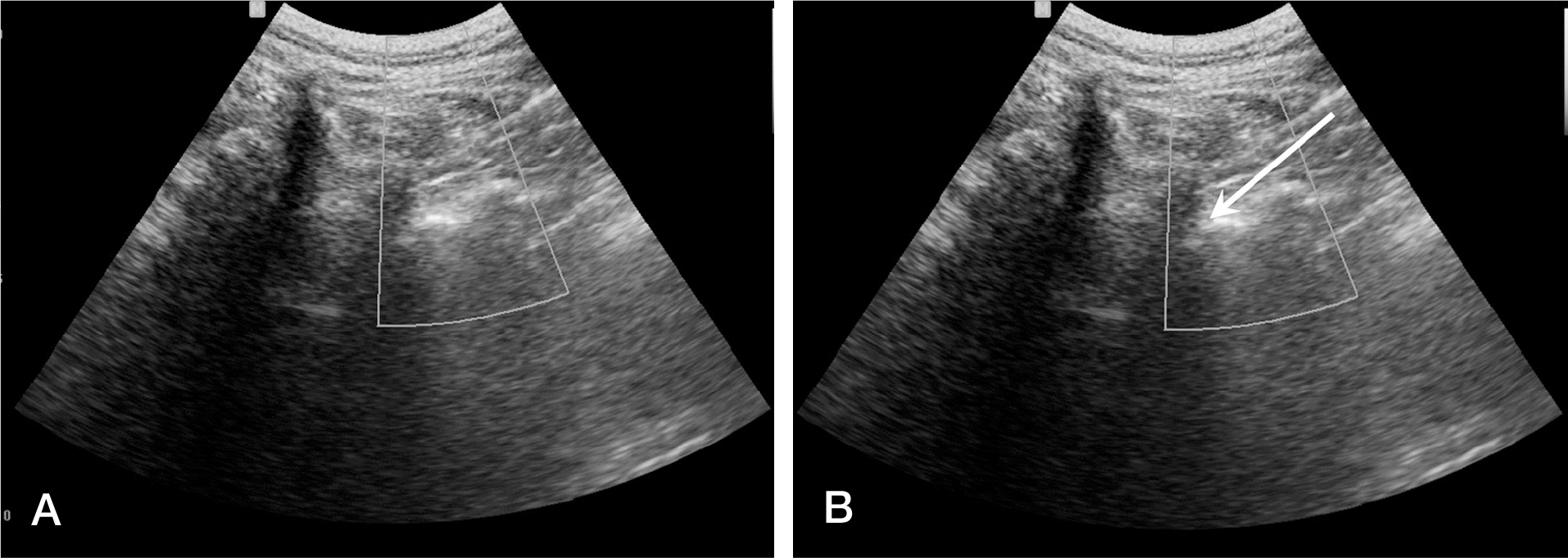
Fig. 7.
23G, 10cm needle (arrowheads) is introduced by use of real-time in-plane ultrasound guidance to target point, which is groove at root of transverse process and base of superior articular process.
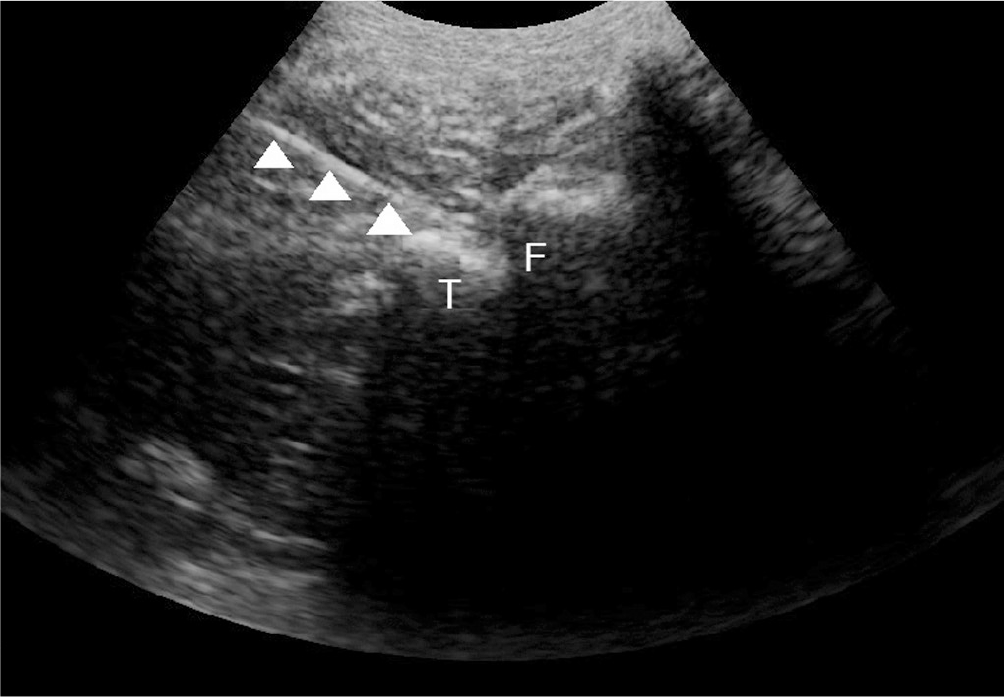
Table 1.
Baseline characteristic and demography of patients
Table 2.
postMBB VAS and improved VAS adjusted with preMBB VAS
| Lidocaine (N=136) | Bupivacaine (N=45) | Significance | |
|---|---|---|---|
| Improved VAS (mean±standard deviation) | 4.691±1.852 | 7.7±1.698 | 0.000* |
| PostMBB VAS (mean±standard deviation) | 2.412±2.203 | 0.622±0.936 | 0.000* |
Table 3.
Multi variable analysis with multiple regression
| Variables | Coefficient | 95% Confidence Interval of Coefficient | Significance |
|---|---|---|---|
| Age | 0.007 | 0.4398 | |
| Sex (male vs female) | -0.158 | 0.5553 | |
| Level | |||
| 1 level | 1 | ||
| 2 level | -0.091 | 0.7456 | |
| 3 level | 0.897 | 0.1370 | |
| 4 level | 0.773 | 0.5362 | |
| Preop. VAS | 0.369 | (0.02079, 0.05296) | 0.0000* |
| Bupivacaine vslidocaine | 2.285 | (1.6620, 2.9079) | 0.0000* |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download