Abstract
Objectives
The aim of the study was to investigate the usefulness of a handheld digital pulse oximetry in the detection of lower extremity arterial disease.
Summary of Literature Review
Pulse oximetry is a well-established method for noninvasive evaluation of arterial oxygenation.
Materials and Methods
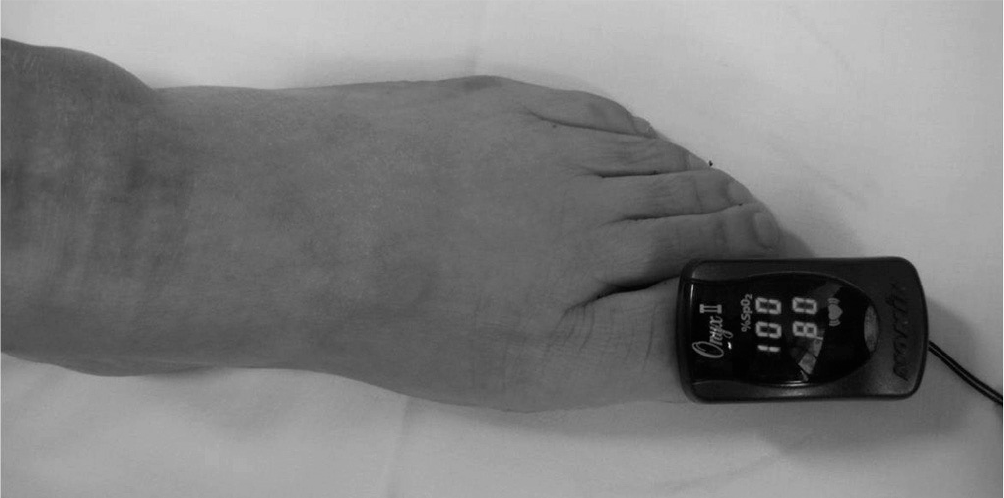
A Retrospective study was performed in 45 patients with lower extremity arterial disease. We compared the accuracy of a handheld digital pulse oximetry and the ankle brachial index (ABI). Digital pulse oximetry was conducted for 42 patients with 84 limbs to measure the SaO2 of their index fingers and big toes in supine position. The ABI was defined as abnormal if it was less than 0.9. Pulse oximetry of big toes was defined as abnormal if the SPO2 was less than 96% or it was more than 2% lower than that of the index finger.
Results
Digital pulse oximetry had a sensitivity of 47%(95% CI, 34-60%) and specificity of 86%(95% CI, 64-96%). ABI had a sensitivity of 49%(95% CI, 34-64%) and specificity of 95%(95% CI, 72-99%). Positive predictive values were 91%(95% CI, 74-98%) for digital pulse oximetry and 96%(95% CI, 77-99%) for ABI. Negative predictive values were 37%(95% CI, 24-51%) for digitial pulse oximetry and 43%(95% CI, 25-72%) for ABI. In 22 cases with acute ischemicwere the sensitivity 73%, the specifity 100%, the positive predictive value 100% and the negative predictive value 79%.
REFERENCES
1. Chae IJ. Lumbar spinal stenosis. J Korean Soc Spine Surg. 1999; 6:220–7.
2. Lee HM. Pathophysiology of Lumbar Spinal stenosis. JKorean Soc Spine Surg. 2000; 7:100–5.
3. Brearley S, Shearman CP, Simms MH. Peripheral pulse pal-pation: an unreliable physical sign. Ann R Coll Surg Engl. 1992; 74:169–71.
4. Barnhorst DA, Barner HB. Prevalence of congenitally absent pedal pulses. N Engl J Med. 1968; 278:264–5.

5. Criqui MH, Fronek A, Klauber MR, Barrett-Connor E, Gabriel S. The sensitivity, specificity, and predictive value of traditional clinical evaluation of peripheral arterial disease: results from noninvasive testing in a defined population. Circulation. 1985; 71:516–22.

6. Joyce WP, Walsh K, Gough DB, Gorey TF, Fitzpatrick JM. Pulse oximetry: a new non-invasive assessment of peripheral arterial occlusive disease. Br J Surg. 1990; 77:1115–7.

7. Feigelson HS, Criqui MH, Fronek A, Langer RD, Molgaard CA. Screening for peripheral arterial disease: the sensitivity, specificity, and predictive value of noninvasive tests in a defined population. Am J Epidemiol. 1994; 140:526–34.

8. Jawahar D, Rachamalla HR, Rafalowski A, Ilkhani R, Bharathan T, Anandarao N. Pulse oximetry in the evaluation of peripheral vascular disease. Angiol-ogy. 1997; 48:721–4.

9. Johansson KE, Marklund BR, Fowelin JH. Evaluation of a new screening method for detecting peripheral arterial disease in a primary health care population of patients with diabetes mellitus. Diabet Med. 2002; 19:307–10.

10. Ouriel K, McDonnell AE, Metz CE, Zarins CK. Criti-cal evaluation of stress testing in the diagnosis of peripheral vascular disease. Surgery. 1982; 91:686–93.
11. Hauser CJ, Klein SR, Mehringer CM, Appel P, Shoemaker WC. Assessment of perfusion in the diabetic foot by regional transcutaneous oximetry. Diabetes. 1984; 33:527–31.

Figures and Tables%
Fig 2.
Receiver operating characteristic (ROC) curve for the pulse oximetry test and the ankle brachilaindex(ABI). (A) ROC curve for pulse oximetry test, Area under the curve was 0.321 (95% confidence interval:0.205-0.438,p<0.014). (B) ROC curve for ABI, Area under the curve was 0.375 (95% confidence interval:0.246-0.505,p<0.114).
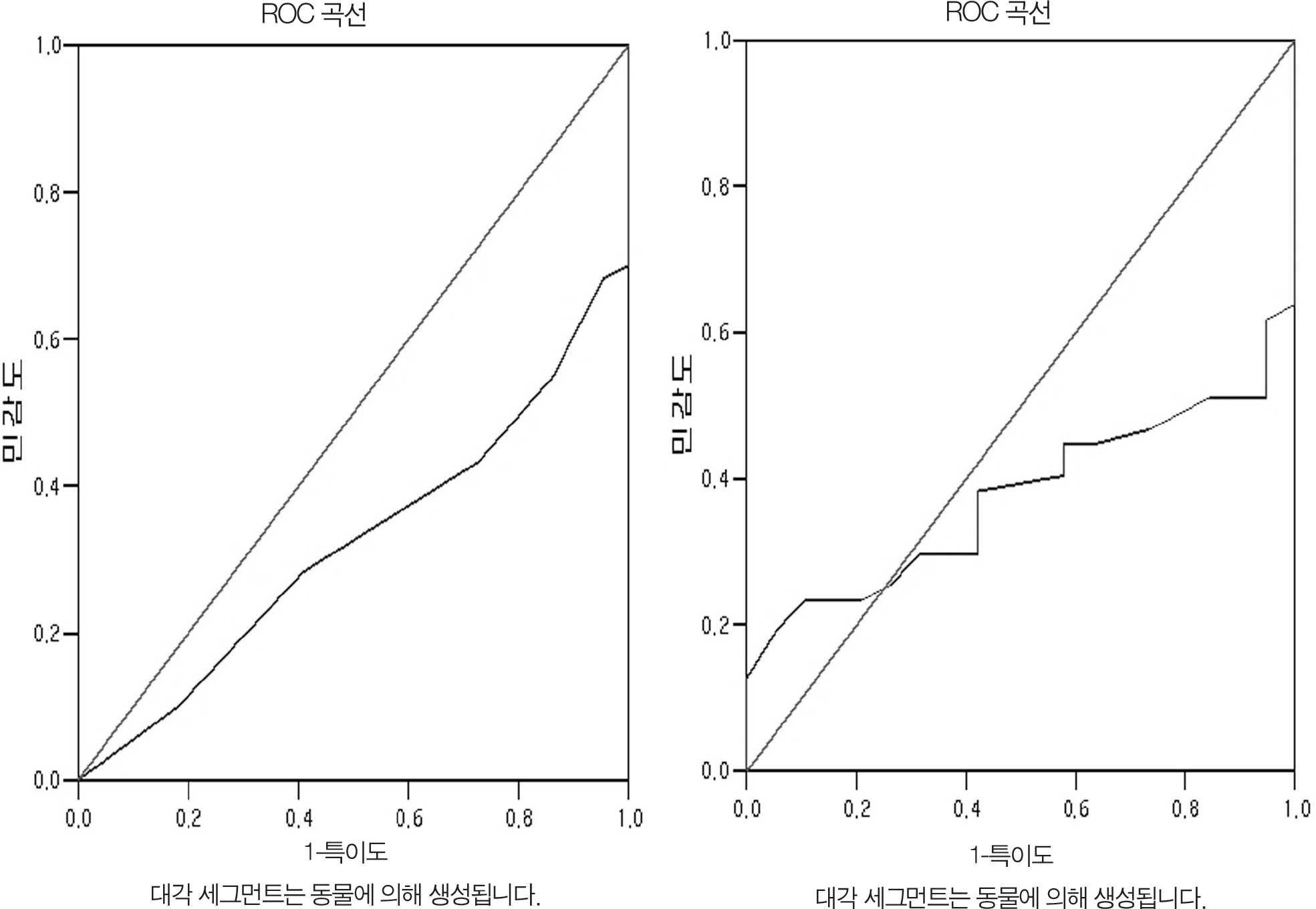
Table 1.
Demography of patients.
| Number of Patients(limbs) | 45 (90 limbs) |
|---|---|
| Average Age (yr) | 66.9(40-92) |
| DM,n (%) | 31(69%) |
| Hypertension,n(%) | 32(71%) |
| Known heart disease,n(%) | 11(24%) |
| Treatment option Surgery | 28(62%) |
| Conservative | 17(38%) |
Table 2.
Results for Pulse oximetry test, Ankle brachial index.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download