Pleomorphic adenoma (PA), also known as a mixed tumor of the salivary glands, is a benign neoplasm, histologically characterized by a biphasic proliferation of polygonal epithelial cells and spindled myoepithelial cells, immersed in a variable amount of background stroma, mucoid, myxoid, cartilaginous or hyaline in appearance.1 Rarely, it can undergo malignant transformation (carcinoma ex-PA) or metastasize without apparent malignant transformation (metastasizing PA).2 It is the most frequent salivary gland tumor and the most common neoplasm of the parotid gland.1 It derives its name from the typical morphological pleomorphism, due to the arrangement in duct-like structures, sheets, clumps and/or interlacing strands.1 The nodule is usually solitary, it can be surrounded by a fibrous pseudo-capsule of variable thickness, and only occasional minor nodular outgrowths occur at initial presentation.1 However, in case of recurrence, a classical myxoid multinodular aspect is observable, configuring the histological picture of the so-called “recurrent pleomorphic adenoma” (RPA).3 In 2015, Jayaram and colleagues described the presence of perineural invasion in the case of benign PA of the minor salivary gland.4 In a similar case, we were recently able to detect the same phenomenon in a benignant RPA (Fig. 1), that arose in the right parotid gland of a 30-year-old female patient, 4 years from the initial diagnosis. To the best of our knowledge, this is the first report in literature of benign RPA of the salivary glands with perineural space invasion. The immunohistochemical investigations have highlighted both epithelial and myoepithelial cells and have disclosed a very low cytoproliferative index (MIB1 labeling index), allowing the exclusion of the possibility of a polymorphous low-grade adenocarcinoma, initially misdiagnosed.5 Our diagnostic experience leads us to emphasize the possible rare finding of perineural space invasion in either benign PA or RPA of the salivary glands. In the final diagnostic report, we have recommended a follow-up period, because the tumor is also present in the surgical margin.
Figures and Tables
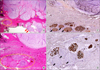
FIG. 1
Recurrent pleomorphic adenoma of the parotid gland: the tumor recurs inside the salivary tissue (A, yellow asterisks), it shows a typical myxoid appearance and a plurinodular growth pattern on panoramic histological view, and it involves the surgical margin (A, red arrows), highlighted by ink marking. Some neoplastic nests (A, yellow circle) spread along the perineural spaces (A, hematoxylin & eosin, 1.25×). At higher magnification, this phenomenon (B, yellow circle) is best appreciated (B, hematoxylin & eosin, 10×). Both neoplastic nests and nerves (C, black arrows) are brown-stained by immunohistochemistry for S100 protein (C, polyclonal, 10×); however, nerves (D, black arrows) are not reactive for pancytokeratins, which reveal in brown only the neoplastic nests (D, clone MNF116, 20×).
ACKNOWLEDGEMENT
This study was supported by the Italian Research Program of Emilia Romagna Region for the University of Modena and Reggio Emilia (CUP E35E09000880002).
References
1. Mendenhall WM, Mendenhall CM, Werning JW, Malyapa RS, Mendenhall NP. Salivary gland pleomorphic adenoma. Am J Clin Oncol. 2008; 31:95–99.

2. Knight J, Ratnasingham K. Metastasising pleomorphic adenoma: systematic review. Int J Surg. 2015; 19:137–145.

3. Witt RL, Eisele DW, Morton RP, Nicolai P, Poorten VV, Zbären P. Etiology and management of recurrent parotid pleomorphic adenoma. Laryngoscope. 2015; 125:888–893.

4. Jayaram R, Patel D, Santhanam V. Benign pleomorphic adenoma of minor salivary gland showing perineural invasion: a rare entity. Br J Oral Maxillofac Surg. 2015; 53:81–82.

5. Zaib N, Mushtaq S, Mamoon N, Akhter N, Ayaz B. Immunohistochemical pattern of pleomorphic adenoma, polymorphous low grade adenocarcinoma and adenoid cystic carcinoma in minor salivary glands. J Dent (Tehran). 2014; 11:38–46.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download