Abstract
This retrospective study was undertaken to compare the outcomes of staged bilateral total hip arthroplasty (THA) by the conventional approach with those of two-incision minimally invasive (MIS-2) THA in terms of clinical and radiological results, complications, and patient preferences. Twenty-two patients aged 30 to 80 years underwent staged bilateral THA. The conventional posterolateral approach was used on the first hips treated and a modified MIS-2 approach on the second hips. The mean time between the first and second procedures was 73.8 months, and the patients were followed up for at least 12 months after both procedures. At the last follow-up visits, THA via the MIS-2 approach was found to provide significantly earlier partial-weight-bearing ambulation, better postoperative Harris hip scores, and better ability to sit cross-legged and was found to be more preferred by patients than conventional THA. There were no significant differences in the complication rates for the two approaches. The present results show that MIS-2 THA is as safe as the conventional posterolateral approach in experienced hands and presents no additional complication risks.
Total hip arthroplasty (THA) using a smaller incision has generated substantial interest among orthopedic surgeons and patients during the past decade. In the early era of minimally invasive (MIS) THA, single-incision approaches were usually performed by decreasing the incision length of either a posterior or an anterior approach to less than 10 cm. The two-incision minimally invasive (MIS-2) technique constitutes a novel theoretical approach to hip replacement. This technique enables access to the hip joint because it uses intermuscular and internervous planes while minimizing damage to the muscles and tendons around the hip joint.1 By reducing the extent of tissue disruption, this technique may reduce intraoperative bleeding, reduce postoperative pain, and lead to more rapid functional recovery.2 However, the use of intraoperative fluoroscopy for accurate reaming and prosthesis placement during MIS-2 is essential owing to the limited direct visualization.
Despite these potential advantages, several reports have claimed that the MIS-2 approach has higher complication rates than does the conventional approach.3 These include the risk of proximal femoral fracture4 and injury to the femoral and lateral femoral cutaneous nerves.3,5 In a cadaveric study by Mardones et al.6 in which degrees of muscle damage following THA performed by using the two-incision and the mini-posterior techniques were compared, it was concluded that although both approaches resulted in some degree of muscle damage, two-incision hip replacement results in more damage to the gluteus medius and gluteus minimus muscles and external rotators. Understandably, this technically demanding approach has an associated learning curve.7
After modifying the Mears technique, we achieved good results and lower complication rates in short-term follow up.8 This modification involves placing the patient in a lateral decubitus position, in contrast with the method of Mears et al. We utilized the Watson-Jones anterolateral approach to insert the acetabular component and made a posterior incision through the intermuscular interval between the gluteus medius and piriformis for femoral component insertion.
After our experiences of conventional and MIS-2 THA, we decided to compare the outcomes of patients who underwent staged bilateral THA with these two approaches. We hypothesized that the MIS-2 technique would give early postoperative benefits in patient function with an increase in complication rates and that patients would prefer the MIS-2 technique to the conventional posterolateral technique.
We included patients who underwent staged bilateral THA in which the conventional posterolateral approach (Fig. 1A) was used on the first hip and the MIS-2 approach (Fig. 1B) was used later on the second hip. We excluded patients with prior surgery at both hips before the index THA, neuromuscular disorders, or a leg length discrepancy of more than 2 cm. We retrospectively reviewed 22 patients who underwent bilateral THA from December 2003 to June 2006. The conventional posterolateral approach was performed either by the experienced surgeon or by other surgeons at other hospitals. All modified MIS-2 THAs were performed by the experienced orthopedic surgeon. Of the hips treated by the conventional posterolateral approach, 19 were treated with cementless stem fixation and 3 with cemented stem insertion; cementless cups were inserted in all 22 hips. Regarding articulation, 9 hips received ceramic-on-ceramic articulation, 7 hips metal-on-metal, and 6 hips metal-on-polyethylene. All MIS-2 THA hips were treated by cementless fixation, and 19 patients received ceramic-on-ceramic articulation and 3 patients metal-on-metal articulation.
Demographic data and pre- and postoperative 1-year and 2-year Harris hip scores9 (HHSs) and Western Ontario and McMaster Universities Arthritis Index (WOMAC) scores10 were recorded. Preoperative HHSs and WOMAC scores were also obtained for patients who underwent conventional surgery at other centers. Patients were also asked which side they preferred and the reasons for their preferences. Details of intra- and postoperative complications were noted. Postoperative radiographs of both hips were obtained at the final follow-up and were analyzed by a blinded orthopedic surgeon. Anteversion of the acetabular component, lateral opening angle, femoral component alignment within the femoral canal, radiological leg length discrepancy, percentage canal fill, and femoral component subsidence were included in the radiologic evaluation.
Statistical analysis was performed by using the Mann-Whitney U test in SPSS software version 19.0 (SPSS Inc, Chicago, IL, USA) on all numerical variables (length of hospitalization, time to partial weight bearing, HHS, WOMAC score). We used the Fisher's exact test for categorical variables (functional variables, such as squatting, sitting cross-legged, and preference). Statistical significance was accepted for p values of <0.05.
No patient was lost to follow-up and all 22 patients were available for review. There were 11 male and 11 female patients of an average age of 59.6 years (range, 30-80 years). The reasons for total hip replacement were avascular necrosis of the femoral heads in 15 patients, osteoarthritis of the hips in 6 patients, and bilateral hip fractures that occurred 6 years apart in 1 patient (Table 1). Average follow-up after MIS-2 THA was 43.7 months (range, 12-101 months) and that after conventional THA was 118.9 months (range, 14-267 months). The overall average follow-up was 81.3 months (range, 12-267 months).
In all patients, MIS-2 THA was performed as a second procedure. The average time between the two surgeries was 73.8 months (range, 4-240 months). All MIS-2 THA procedures and 8 of the 22 conventional THA procedures were performed by the senior author. The remaining 14 conventional THA procedures were performed in other institutions. The average duration of hospital admission for MIS-2 THA was 10 days (range, 6-27 days) and that for conventional THA was 13 days (range, 10-34 days); the average overall duration of admission was 15 days. Patients tolerated weight-bearing crutch walking following MIS-2 THA on the 3rd postoperative day (range, 1-6 days) and after conventional THA on the 6th day (range, 2-8 days) (Table 2).
The patients who experienced bilateral femoral neck fractures were excluded from the HHS and WOMAC score assessment because scoring before surgery could not be performed. The mean preoperative, 1-year postoperative, and 2-year postoperative HHSs of the MIS-2 THA hips were 47.7 (range, 25-63), 94.7 (range, 84-100), and 91.9 (range, 82-100), respectively, and the corresponding scores for the conventional THA hips were 46.1 (range, 30-60), 92.1 (range, 81-100), and 90.9 (range, 79-100), respectively. The mean preoperative, 1-year postoperative, and 2-year postoperative mean WOMAC scores for the MIS-2 THA hips were 74.7 (range, 56-97), 22.3 (range, 9-34), and 23.1 (range, 9-35), respectively, and the corresponding scores for the conventional THA hips were 77.7 (range, 59-110), 25.3 (range, 9-39), and 26.7 (range, 9-39), respectively.
Of the 22 patients, 8 underwent both surgeries by the senior author. In this group of patients, average preoperative, 1-year postoperative, and 2-year postoperative HHS scores for the MIS-2 hips were 45.9, 97.6, and 96.1, respectively, whereas the average values for the conventionally treated hips were 43.5, 96.8, and 95.6, respectively. The average preoperative, 1-year postoperative, and 2-year postoperative WOMAC scores for the MIS-2 hips were 73.3, 21.7, and 20.3, respectively, and the average WOMAC scores for the conventionally treated hips were 70.9, 24.1, and 22.6, respectively.
At the 1-year and 2-year postoperative visits, 12 patients had no difficulty running, but the other 10 could not. However, of these 10, nine patients admitted that this was probably because they had not tried to run. The other patient was not able to run owing to discomfort in the conventionally treated hip. Seventeen patients had no difficulty sitting cross-legged and five were not able to do so. Of these five, one had limitations in both hips, and in the other four the conventionally treated hip prevented cross-legged sitting. Seventeen patients were able to squat without difficulty. In two of the patients not able to squat, this inability was due to limitations in both hips. The remaining three patients felt that the conventionally treated hip prevented squatting. Eleven patients preferred the MIS-2 THA hip and cited faster rehabilitation (3 patients), less pain (3 patients), and less discomfort (5 patients) as reasons. Four patients preferred the conventionally treated hip and citing squeaking (1 patient), clicking (1 patient), and mild discomfort following exertion (2 patients) in the MIS-2 THA hip as reasons. However, the two patients who complained of squeaking or clicking were implanted with ceramic-on-ceramic articulation. Seven patients expressed no preference for one hip over the other.
The average lateral opening angle was 41.10 (range, 35.1-45.20) for conventional posterolateral THA and 40.80 (range, 35.8-45.30) for MIS-2 THA. The average angles of anteversion for conventional posterolateral THA and MIS-2 THA were 14.90 (range, 10.2-18.60) and 16.50 (range, 11.1-19.50), respectively. All the femoral components were implanted in neutral to 50 of valgus during MIS-2 THA. However, 1 stem was implanted in slight varus (1.90) during conventional THA. No patient had a limb length discrepancy of more than 5 mm postoperatively, and no femoral component showed subsidence of more than 3 mm in either group. Femoral canal filling by prosthesis was excellent in all cases.
No infection, dislocation, intraoperative fracture, or deep vein thrombosis was encountered in any patient. In one patient, the hip implanted conventionally at another institution was found to be in a varus position, but this hip remains asymptomatic. In another, abductor weakness was noted on the conventional side, which persisted at 5 years postoperatively. In addition, one patient developed a postoperative fever following MIS-2 THA, which was attributed to a urinary tract infection. The fever and infection were resolved by medication and did not adversely affect the outcome of hip surgery. Another patient complained of mild anterolateral thigh numbness in the MIS-2 THA side, and this persisted at 4 years postoperatively but did not interfere with daily activities.
The current definition of MIS THA involves any hip arthroplasty procedure in which the length of the wound and surgical dissection are modified to minimize the tissue damage associated with hip replacement.11 The reported benefits of MIS THA include reduced hospital stay, faster recovery, less blood loss, and better cosmetic results. Thus, it is no surprise that journals and popular media have devoted significant attention to this topic and that patients are demanding such surgery.12
Our study had several limitations. As in any retrospective review, some information was lacking, especially when multiple institutions were involved in patient care. In addition, patient numbers were small. However, our ability to compare results in the same patients reduced or eliminated variabilities introduced by weight, comorbidity, bone quality, activity level, and gender. On the other hand, although both procedures were performed in the same patients, in 14 patients, conventional posterolateral THA was performed by different surgeons. As a result, outcome comparisons are fraught by different surgical techniques, anaesthesia, pain and rehabilitation protocols, surgeons, prostheses, articulation, and institutions. These shortcomings are why we opted to focus on patient satisfaction levels, rather than on only clinical outcome measures. Furthermore, blood loss and operative times were not compared in the present study because some hips were treated conventionally at other centers, and intra- and perioperative details were not available for review.
In this study, patients were found to mobilize sooner and to require crutches for significantly less time after MIS-2 THA. Despite a lack of peer-reviewed literature on MIS THA, especially randomized trials,12,13 some data support a reduction in blood loss and faster recovery after MIS. In a study by Chimento and Sculco14 it was found that patients in the mini-incision group (an 8-cm long incision) lost significantly less blood than did patients in a standard incision group (15-cm incision) and more rapidly achieved a normal gait pattern. Wenz et al.15 compared 124 minimally invasive anterolateral THAs with 65 standard anterolateral THAs and found that the minimally invasive group had lower operative times and transfusion requirements and achieved earlier functional recovery without any increase in complications or component malposition. In this previous study, three times as many patients were able to ambulate on day 1 and 50% more patients met all discharge criteria by day 3 after MIS THA. Furthermore, patients in the minimally invasive group were able to sit up, stand, and transfer more rapidly than did the patients in the conventional group. This finding was supported by Berger et al.,16 who reported substantially faster recoveries. In fact, those authors reported being able to discharge all 100 patients within 23 hours postoperatively. In the present study, although MIS-2 patients had longer hospital stays than found in these previous studies,15,16 hospital stay was shorter than in the conventional group. Moreover, this difference in hospital stays is probably explained by the medical insurance reimbursement system in Korea, which allows hospital stay for up to 3 weeks postoperatively in uncomplicated cases. Thus, patients tend to opt to remain in the hospital to recuperate without incurring any extra cost.
In a study by Ogonda et al.,13 109 patients treated by use of a mini-incision technique were compared with 110 patients treated by use of a standard approach. In terms of early outcomes (follow-up at 6 weeks), no significant difference was found between the two patient groups for any outcome parameter measured. The authors concluded that the mini-incision technique is safe and reproducible, although this technique offers no significant benefit. Lawlor et al.17 in a prospective randomized blinded trial compared total hip replacement using a minimally invasive approach versus a standard incision approach in terms of early postoperative functional levels, and concluded that there was no difference between the two approaches in the ability of patients to mobilize and perform functional tasks necessary for safe discharge. Khan et al.18 reported that patients in their less invasive group showed significantly better WOMAC scores than did their standard group for up to 12 months. At 24 months, however, this difference failed to reach statistical significance. The findings of the present study concur. No intergroup difference in WOMAC score was observed at the final follow-up. However, the HHS was significantly better with MIS-2 THA.
In this series, complication rates were similar for the two approaches. In a previous study by Kim,19 a comparison of primary THA performed by using a modified posterolateral minimally invasive technique with a standard posterolateral approach in patients who underwent simultaneous bilateral THA showed no significant difference in postoperative outcomes, but a higher infection rate for MIS THA. In the present study, however, no infection developed in the MIS-2 THA arm.
Pagnano et al.20 reported in their series of 26 patients who underwent staged bilateral THA with MIS-2 on one hip and mini-posterior THA on the other that no early functional outcome differences were evident. In this previous study, 16 patients preferred mini-posterior THA and two patients had no preference, whereas in the present study, 11 patients preferred MIS-2 THA, 4 preferred conventional posterolateral THA, and 7 patients expressed no preference. In the present study, no significant difference was found between the functional abilities of the two study groups, which shows that the hips treated by MIS-2 THA function sooner, as well as if not better than the hips treated by conventional THA by use of the posterolateral approach.
Furthermore, in the present study, radiologic evaluations showed acceptable femoral and acetabular component placement and limb length restoration after MIS-2 THA, which refutes the argument that component positioning is compromised during minimally invasive procedures.21
In summary, we found THA via MIS-2 to be as safe as the conventional posterolateral approach in experienced hands and to not present any additional risk of complications. Furthermore, MIS-2 THA provided significantly earlier partial weight-bearing ambulation, better postoperative HHS, and better ability to sit cross-legged; was more preferred by patients than conventional THA; and achieved satisfactory clinical and radiological results.
Figures and Tables
References
2. Berger RA. Minimally invasive total hip arthroplasty with two incisions. Oper Tech Orthop. 2006; 16:102–111.

3. Bal BS, Haltom D, Aleto T, Barrett M. Early complications of primary total hip replacement performed with a two-incision minimally invasive technique. J Bone Joint Surg Am. 2005; 87:2432–2438.

4. Duwelius PJ, Berger RA, Hartzband MA, Mears DC. Two-incision minimally invasive total hip arthroplasty: Operative technique and early results from four centers. J Bone Joint Surg Am. 2003; 85:2240.
5. Berry DJ, Berger RA, Callaghan JJ, Dorr LD, Duwelius PJ, Hartzband MA, et al. Minimally invasive total hip arthroplasty. Development, early results, and a critical analysis. Presented at the Annual Meeting of the American Orthopaedic Association, Charleston, South Carolina, USA, June 14, 2003. J Bone Joint Surg Am. 2003; 85:2235–2246.
6. Mardones R, Pagnano MW, Nemanich JP, Trousdale RT. The Frank Stinchfield Award: muscle damage after total hip arthroplasty done with the two-incision and mini-posterior techniques. Clin Orthop Relat Res. 2005; 441:63–67.

7. Archibeck MJ, White RE Jr. Learning curve for the two-incision total hip replacement. Clin Orthop Relat Res. 2004; (429):232–238.

8. Yoon TR, Bae BH, Choi MS. A modified two-incision minimally invasive total hip arthroplasty: technique and short-term results. Hip Int. 2006; 16:Suppl 4. 28–34.

9. Harris WH. Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am. 1969; 51:737–755.

10. Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW. Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol. 1988; 15:1833–1840.
11. Jando VT, Duncan CP. Two-incision technique for minimally invasive total hip arthroplasty. Oper Tech Orthop. 2004; 14:102–110.

12. Bostrom MP, Demetrakopoulos D, Reinhart J, Sculco TP. Minimally invasive posterior approach to total hip replacement. Curr Opin Orthop. 2005; 16:2–4.

13. Ogonda L, Wilson R, Archbold P, Lawlor M, Humphreys P, O'Brien S, et al. A minimal-incision technique in total hip arthroplasty does not improve early postoperative outcomes. A prospective, randomized, controlled trial. J Bone Joint Surg Am. 2005; 87:701–710.

14. Chimento GF, Sculco TP. Minimally invasive total hip arthroplasty. Oper Tech Orthop. 2011; 11:270–273.

15. Wenz JF, Gurkan I, Jibodh SR. Mini-incision total hip arthroplasty: a comparative assessment of perioperative outcomes. Orthopedics. 2002; 25:1031–1043.

16. Berger RA, Jacobs JJ, Meneghini RM, Della Valle C, Paprosky W, Rosenberg AG. Rapid rehabilitation and recovery with minimally invasive total hip arthroplasty. Clin Orthop Relat Res. 2004; (429):239–247.

17. Lawlor M, Humphreys P, Morrow E, Ogonda L, Bennett D, Elliott D, et al. Comparison of early postoperative functional levels following total hip replacement using minimally invasive versus standard incisions. A prospective randomized blinded trial. Clin Rehabil. 2005; 19:465–474.

18. Khan RJ, Fick D, Khoo P, Yao F, Nivbrant B, Wood D. Less invasive total hip arthroplasty: description of a new technique. J Arthroplasty. 2006; 21:1038–1046.
19. Kim YH. Comparison of primary total hip arthroplasties performed with a minimally invasive technique or a standard technique: a prospective and randomized study. J Arthroplasty. 2006; 21:1092–1098.

20. Pagnano MW, Leone J, Lewallen DG, Hanssen AD. Two-incision THA had modest outcomes and some substantial complications. Clin Orthop Relat Res. 2005; 441:86–90.

21. Bhan S, Pankaj A, Malhotra R. One- or two-stage bilateral total hip arthroplasty: a prospective, randomised, controlled study in an Asian population. J Bone Joint Surg Br. 2006; 88:298–303.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


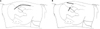


 XML Download
XML Download