Abstract
Hashimoto thyroiditis (HT) is an autoimmune thyroid disorder that usually presents as a diffuse, nontender goiter, whereas subacute thyroiditis (SAT) is an uncommon disease that is characterized by tender thyroid enlargement, transient thyrotoxicosis, and an elevated erythrocyte sedimentation rate (ESR). Very rarely, patients with HT can present with painful, tender goiter or fever, a mimic of SAT. We report a case of painful HT in a 68-year-old woman who presented with pain and tenderness in a chronic goiter. Her ESR was definitely elevated and her thyroid laboratory tests suggested subclinical hypothyroidism of autoimmune origin. 99mTc pertechnetate uptake was markedly decreased. Fine needle aspiration biopsy revealed reactive and polymorphous lymphoid cells and occasional epithelial cells with Hürthle cell changes. Her clinical symptoms showed a dramatic response to glucocorticoid treatment. She became hypothyroid finally and is now on levothyroxine therapy.
Hashimoto thyroiditis is an autoimmune thyroid disorder that is probably the most common cause of hypothyroidism. It predominantly affects middle-aged women and usually manifests as a painless, nontender, diffuse goiter.1 In contrast, subacute thyroiditis causes neck pain, thyroid tenderness, and systemic symptoms of inflammatory disease with or without thyrotoxicosis. These two disease entities seem to have quite different pathogenic mechanisms, specifically, autoimmune and probably various viral infections, respectively. However, in a very few cases of Hashimoto thyroiditis, symptoms and signs such as thyroid pain and tenderness, fever, and general malaise could be initial manifestations.2,3 In their cytopathologic study of 51 cases, Jayaram et al. reported the coexistence of Hashimoto thyroiditis with subacute thyroiditis in two cases.4 It was not clarified whether the coexistence was accidental or pathogenically interrelated, because only a few cases of an association between subacute thyroiditis and Hashimoto thyroiditis have been reported.5 Furthermore, Hashimoto thyroiditis itself can be a very rare cause of painful or tender thyroid.2 We describe here a case of a Hashimoto thyroiditis patient who had a chronic goiter for several months and subsequently presented with a painful, tender goiter, elevated erythrocyte sedimentation rate (ESR), and decreased thyroid Tc-99m pertechnetate uptake typical of subacute thyroiditis.
A 68-year-old woman, who had a chronic nontender goiter for several months, presented with pain on the anterior neck, otalgia, and sore throat. Her symptoms had been apparent for 5 days, and she reported a 2-week history of fatigue and malaise. No prior treatment or evaluation had been done during that time. She had been taking Imatinib mesylate (Gleevec®) since 2004 when she was diagnosed with chronic myeloid leukemia (CML). She recalled that she had been informed of mild thyroid dysfunction by a doctor in another hospital several months ago. However, she did not receive any treatment for the thyroid dysfunction. Physical examinations showed both thyroid lobes to be diffusely enlarged with a firm consistency with marked tenderness. No definitive nodule was palpable in either thyroid gland. She denied experiencing any change in her body weight; her height was 159 cm and she weighed 47.8 kg. Her vital signs were as usual: blood pressure 154/75 mmHg, pulse rate 98 per minute, respiration rate 14 per minute, and body temperature 36.5℃.
Her thyroid function tests revealed subclinical hypothyroidism on presentation; her serum TSH level was elevated to 7.70 uIU/ml, whereas free thyroxine (FT4) and total triiodothyronine (T3) were within the lower limits of their normal ranges. The anti-thyroglobulin (anti-Tg) antibody level was significantly elevated; on the other hand, the titers of anti-thyroperoxidase (anti-TPO) and anti-TSH receptor antibodies were not (Table 1). Tests for inflammatory markers were markedly elevated: ESR, 110 mm/h (normal range, 0-20 mm/h); C-reactive protein, 4.43 mg/dl (normal range, 0.00-0.30 mg/dl). Biochemistry, complete blood count, and liver and kidney function tests were not contributory. Thyroid ultrasonography revealed a diffusely enlarged thyroid gland with heterogeneously hypoechoic changes involving the entire area of both thyroid glands. Color Doppler ultrasonography showed nearly no vascular flow in the hypoechoic lesion. No cervical lymphadenopathy was detected (Fig. 1). 99mTc pertechnetate uptake in both thyroid lobes was markedly decreased (Fig. 2). Fine needle aspiration biopsy was performed and cytology revealed reactive and polymorphous lymphoid cells. They were composed of a mixed cell population of lymphocytes, centroblasts, plasma cells, and macrophages. Occasionally, epithelial cells with Hürthle cell changes were observed. Few multinucleate histiocytes were seen (Fig. 3). Oral prednisone 30 mg/d as the starting dose was prescribed and her clinical signs and symptoms improved dramatically. Steroid therapy was tapered and stopped in 10 days. On her follow-up visit in 2 weeks, she complained of neck pain and malaise again. Physical examinations revealed moderate tenderness of the thyroid. On thyroid function tests, her serum TSH level was increased to 24.68 uIU/ml, whereas both T3 and FT4 levels were decreased (Table 1). The patient showed a good response to glucocorticoid therapy again. However, overt hypothyroidism was persistent. She is now on maintenance therapy with levothyroxine (0.1 mg daily).
Hashimoto thyroiditis is common and usually presents as a diffuse painless goiter.1 However, it has been reported that Hashimoto thyroiditis can present very rarely as pain and tenderness on a preexisting goiter. Also, the pain may be chronic, persistent, or recurrent and not responsive to medical treatment.2,3,6
If there is pain in a goiter or thyroid tenderness, painful thyroiditis should be considered. It may be difficult to differentiate painful Hashimoto thyroiditis from subacute thyroiditis, the most common cause of painful thyroiditis. Other causes include invasive fibrous thyroiditis, radiation thyroiditis, primary or metastatic thyroid malignancy, and other infectious causes of thyroiditis.2 In our case, cytologic study revealed reactive lymphoid cell infiltrations with occasional Hürthle cell changes and a few multinucleate histiocytes. Multinucleate histiocytes may be seen in Hashimoto thyroiditis. In subacute thyroiditis, however, numerous multinucleate histiocytes are usually seen and Hürthle cell changes are not.7 Thus, painful Hashimoto thyroiditis was considered first in our case. However, patients with painful Hashimoto thyroiditis usually have a normal ESR level and variable uptake of isotope in a thyroid scan according to the stage of disease. Also, the pain and tenderness in patients with painful thyroiditis are usually long-lasting with variable response to thyroxine, aspirin, or glucocorticoid, sometimes requiring total thyroidectomy.2,3 Subacute thyroiditis complicating Hashimoto thyroiditis can also be a differential diagnosis. However, Shigemasa et al. reported 8 Japanese patients with painful Hashimoto's thyroiditis confirmed by needle biopsy.6 Their initial clinical presentation was characteristic of subacute thyroiditis. All patients presented with fever and painful tender goiter with markedly elevated ESR. Six patients had transient thyrotoxicosis associated with a markedly depressed radioactive iodine uptake (RAIU; 0.8-3%). More patients were responsive to steroid therapy. Taken together, these findings suggest that painful Hashimoto thyroiditis may have variable clinical courses and therapeutic responses according to patient background. Compared with patients with subacute thyroiditis, nearly all patients with painful Hashimoto thyroiditis have prior goiter, the duration of goiter ranging from months to years.6,7
Our patient also had a prior goiter, elevated thyroid autoantibody titer, profuse lymphocyte infiltration with occasional Hürthle cell changes and few giant cells on cytologic examination, and became hypothyroid finally, which suggests that the patient can be diagnosed with painful Hashimoto thyroiditis, rather than subacute thyroiditis.
The histopathologic pattern of subacute thyroiditis is intrafollicular cellular infiltration with loss of colloid and disruption of their lining epithelium. These follicular changes tend to eventually lead to the multiple formation of granuloma-like structures.8 Follicles containing numerous giant cells are a characteristic feature of the disease. The published false-negative rate of thyroid fine needle aspiration varies between 1% and 10%.9 We performed fine needle aspiration in both thyroid lobes and checked a great enough number of cell blocks, precluding false negativity for giant cells. Her clinical course and cytologic findings also excluded the possibility of CML involvement of the thyroid gland as a cause of thyroid pain.
The reason for pain and tenderness on the thyroid in patients with Hashimoto thyroiditis remains to be clarified. Thyroid capsule distension from rapid goiter growth may be an explanation. However, some patients respond to thyroxine therapy, whereas other patients do not show a relief of pain even after a decrease in goiter. There is no difference in histologic findings between patients presenting with pain and patients presenting without pain.3 The various clinical presentation of Hashimoto thyroiditis may reflect an interaction between the thyroid gland and a variety of ill-understood cellular immune determinants as well as humoral factors that are active locally in the thyroid gland.4 One or more of these factors may be associated with pain and the other features according to the patient's background.
Although our patient responded to two series of glucocorticoid treatments, if pain is persistent and does not respond to medical treatment, total thyroidectomy should be considered. The surgery requires an experienced surgeon because the thyroid gland may be fibrosed and pain can be persistent if remnant thyroiditis remains. If remnant thyroiditis causes pain, radioiodine ablation may be used.3 The first case of painful Hashimoto thyroiditis that required total thyroidectomy in the Korean literature was reported in 2008.10 To our knowledge, this is the second case report of painful Hashimoto thyroiditis treated with corticosteroid therapy in the Korean literature. In conclusion, painful Hashimoto thyroiditis can rarely be a cause of painful, tender goiter and can have very similar clinical characteristics to subacute thyroiditis, requiring careful clinical approaches to differentiate the two diseases.
Figures and Tables
FIG. 1
Ultrasonography scan shows heterogeneously hypoechoic changes involving both thyroid lobes (glands). Both thyroid lobes (glands) were diffusely enlarged (A). A color Doppler image shows that blood flow is markedly decreased in the hypoechoic areas (B).
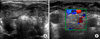
FIG. 2
Thyroid scintigraphy using 99mTc pertechnetate. Markedly decreased uptake of the radiotracer was seen in both lobes of the thyroid gland.
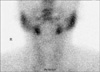
FIG. 3
The cytopathology of the thyroid gland. (A) The cytopathology of the thyroid gland revealed reactive and polymorphous lymphoid cell infiltrations (Papanicolaou's stain, ×100). (B) Occasional epithelial cells with Hürthle cell changes were mixed with lymphocytes, centroblasts, plasma cells, and macrophages (Papanicolaou's stain, ×200).

References
1. Li Y, Nishihara E, Kakudo K. Hashimoto's thyroiditis: old concepts and new insights. Curr Opin Rheumatol. 2011. 23:102–107.

2. Zimmerman RS, Brennan MD, McConahey WM, Goellner JR, Gharib H. Hashimoto's thyroiditis. An uncommon cause of painful thyroid unresponsive to corticosteroid therapy. Ann Intern Med. 1986. 104:355–357.
3. Kon YC, DeGroot LJ. Painful Hashimoto's thyroiditis as an indication for thyroidectomy: clinical characteristics and outcome in seven patients. J Clin Endocrinol Metab. 2003. 88:2667–2672.

4. Jayaram G, Marwaha RK, Gupta RK, Sharma SK. Cytomorphologic aspects of thyroiditis. A study of 51 cases with functional, immunologic and ultrasonographic data. Acta Cytol. 1987. 31:687–693.
5. Minciullo PL, Ruggeri RM, Vita G, Benvenga S, Gangemi S. Development of Hashimoto's thyroiditis after subacute thyroiditis: an unusual patient. Thyroid. 2009. 19:73–74.

6. Shigemasa C, Ueta Y, Mitani Y, Taniguchi S, Urabe K, Tanaka T, et al. Chronic thyroiditis with painful tender thyroid enlargement and transient thyrotoxicosis. J Clin Endocrinol Metab. 1990. 70:385–390.

8. Ishihara T, Mori T, Waseda N, Ikekubo K, Akamizu T, Imura H. Histological, clinical and laboratory findings of acute exacerbation of Hashimoto's thyroiditis--comparison with those of subacute granulomatous thyroiditis. Endocrinol Jpn. 1987. 34:831–841.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download